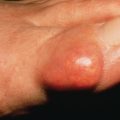
Seborrheic Dermatitis
Clinical Features
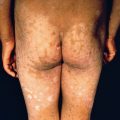
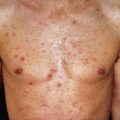
Seborrheic dermatitis is common, occurring in 2%–5% of the population. It is a chronic, superficial, inflammatory disease with a predilection for the scalp, eyebrows, eyelids, nasolabial creases, lips, ears ( Fig. 10.1 ), sternal area, axillae, submammary folds, umbilicus, groins, and gluteal crease. The disease is characterized by scaling on an erythematous base. The scale often has a yellow, greasy appearance. Itching may be severe. Dandruff (pityriasis sicca) represents a mild form of seborrheic dermatitis. An oily type, pityriasis steatoides, is accompanied by erythema and an accumulation of thick crusts.
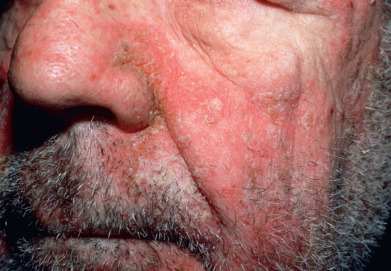
Other types of seborrheic dermatitis on the scalp include arcuate, polycyclic, or petaloid patches and psoriasiform, exudative, or crusted plaques. The disease frequently spreads beyond the hairy scalp to the forehead, ears, postauricular regions, and neck. On these areas, the patches have convex borders and are reddish yellow or yellowish. In dark-skinned individuals, arcuate and petaloid lesions typically involve the hairline. In extreme cases, the entire scalp is covered by a greasy, dirty crust with an offensive odor. In infants, yellow or brown scaling lesions on the scalp, with accumulated adherent epithelial debris, are called “cradle cap.”
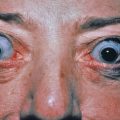
Erythema and scaling are often seen in the eyebrows. The lids may show fine, yellowish white scales and faint erythema. The edges of the lids may be erythematous and granular (marginal blepharitis), and the conjunctivae may be injected. If the glabella is involved, fissures in the wrinkles at the inner end of the eyebrow may accompany the fine scaling. In the nasolabial creases and on the alae nasi, there may be yellowish or reddish yellow scaling macules, sometimes with fissures. In men, folliculitis of the beard area is common.
In the ears, seborrheic dermatitis may be mistaken for an infectious otitis externa. There is scaling in the aural canals, around the auditory meatus, usually with marked pruritus. The postauricular region and skin under the lobe may be involved. In these areas, the skin often becomes red, fissured, and swollen. In the axillae, the eruption begins in the apices, bilaterally, and later progresses to neighboring skin. This pattern resembles that of allergic contact dermatitis to deodorant, but differs from that of clothing dermatitis (which involves periphery of axillae but spares the vault). The involvement may vary from simple erythema and scaling to more pronounced petaloid patches with fissures. The inframammary folds and the umbilicus may be involved. The presternal area is a favored site on the trunk.
Seborrheic dermatitis is common in the groin and gluteal crease, where its appearance may closely simulate tinea cruris or candidiasis. In these areas, the appearance often overlaps with that of inverse psoriasis. In fact, many of these patients have an overlap of the two conditions (sebopsoriasis or seborrhiasis) in the groin, as well as the scalp. The lesions may also become generalized and progress to an exfoliative erythroderma (erythroderma desquamativum), especially in infants. A minority of these infants will have evidence of immunosuppression. In adults, generalized eruptions may be accompanied by adenopathy and may simulate mycosis fungoides or psoriatic erythroderma.
Seborrheic dermatitis may be associated with several internal diseases. Parkinson disease is often accompanied by severe refractory seborrheic dermatitis involving the scalp and face, with waxy, profuse scaling. A unilateral injury to the innervation of the face, or a stroke, may lead to unilateral localized seborrheic dermatitis. Patients with acquired immunodeficiency syndrome (AIDS) have an increased incidence of seborrheic dermatitis. An increased incidence has also been noted in patients who are seropositive for human immunodeficiency virus (HIV) but have not developed other signs of clinical disease. Diabetes mellitus (especially in obese persons), sprue, malabsorption disorders, epilepsy, neuroleptic drugs (e.g., haloperidol), and reactions to arsenic and gold have all produced seborrheic dermatitis–like eruptions.
Etiology and Pathogenesis
The etiology of this common disorder is complex but may be related to the presence of the lipophilic yeast Malassezia ovalis (Pityrosporum ovale), which produces bioactive indoles, oleic acid, malssezin, and indole-3-carbaldehyde. The density of yeast has been correlated with the severity of the disease, and reduction of the yeast occurs with response to therapy. M. ovalis may also be abundant on the scalps of patients who have no clinical signs of the disease, and the yeast may only be pathogenic in predisposed individuals. Heavy colonization with Staphylococcus epidermidis has also been noted.
Patients with seborrheic dermatitis may show upregulation of interferon (IFN)–γ, expressed interleukin-6 (IL-6), expressed IL-1β, and IL-4. Expression of cytotoxicity-activating ligands and recruitment of natural killer (NK) cells have also been noted.
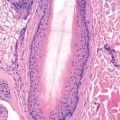
Histology
The epidermis demonstrates regular acanthosis with some thinning of the suprapapillary plates. Varying degrees of spongiosis and lymphocyte exocytosis are noted. A characteristic finding is the presence of a focal scale crust adjacent to the follicular ostia.
Differential Diagnosis
Some cases of seborrheic dermatitis bear a close clinical resemblance to psoriasis, and the two conditions may overlap. Patients with psoriasis tend to have more pronounced erythema and heavier silvery scales that peel in layers. Removal of scales in psoriasis may disclose bleeding points (Auspitz sign). This sign is common but lacks great specificity. Severe itching favors seborrheic dermatitis. Characteristic psoriasis elsewhere (nail pitting, balanitis) may resolve the question. Impetigo of the scalp, especially when associated with pediculosis, may cause difficulty in differentiation. Scalp impetigo can be an indolent crusted dermatosis associated with failure to thrive. Langerhans cell histiocytosis may also resemble seborrheic dermatitis, but typically demonstrates yellow-brown perifollicular papules and groin fissuring. Crusted scabies of the scalp can also be confused with seborrheic dermatitis, and Trichophyton tonsurans often produces a subtle seborrheic scale. In subtle cases of tinea, a moist gauze pad rubbed vigorously on the scalp will typically dislodge short, broken potassium hydroxide (KOH)–positive hairs. This can be the fastest way to make the diagnosis.
Treatment
Agents suitable for use on glabrous skin include corticosteroid creams, gels, sprays, and foams. Corticosteroids tend to produce a rapid effect with high clearance rates, but on the face, even medium-potency corticosteroids can produce steroid rosacea. For this reason, antifungal agents and topical calcineurin inhibitors (CNIs) are often used. Ketoconazole, ciclopirox, sertaconazole, tacrolimus, pimecrolimus, zinc pyrithione, and Quassia amara extract preparations are all effective alone and in combination. The antifungals are now available in a wide range of vehicles, including foams, gels, and liquids. Surfactant-based pronosomal formulations can improve drug delivery. Proniosomes are particles coated with a nonionic surfactant. Bifonazole shampoo has been effective in treating infants and small children. Topical CNIs may be associated with a burning sensation, especially on moist skin, and may produce flushing if patients consume alcohol. Patients generally tolerate these agents better after initial treatment with a corticosteroid. An open, randomized, prospective, comparative study of topical pimecrolimus 1% cream versus topical ketoconazole 2% cream found the two to be equally effective, but side effects were somewhat more common with pimecrolimus. Preliminary studies suggest oral itraconazole and oral terbinafine may show some efficacy. Oral fluconazole showed marginal benefit. Study results with topical metronidazole have been mixed.
When secondary bacterial infection is present, a topical or oral antibiotic may be required. In patients infected with HIV, lithium succinate ointment has been used for facial disease. Lithium gluconate 8% ointment has compared favorably with ketoconazole 2% emulsion in healthy adults and was more effective in terms of control of scaling and symptoms. Sodium sulfacetamide products, with or without sulfur, are effective in some refractory patients.
For scalp disease, selenium sulfide, ketoconazole, tar, zinc pyrithione, fluocinolone, and resorcin shampoos are effective. In many patients, these agents may be used two to three times a week, with a regular shampoo used in between as required. White patients often prefer antifungal foams and gels, as well as corticosteroid solutions, foams, gels, and sprays, whereas some black patients prefer ointment or oil preparations.
Itching of the external ear canal usually responds to a topical corticosteroid, CNIs, or antifungals (e.g., ketoconazole, ciclopirox). Some patients require the use of a class 1 corticosteroid on weekends to control refractory pruritus. Cortisporin otic suspension (neomycin, polymyxin B, hydrocortisone) can bring about prompt clearing, but contact dermatitis to neomycin may complicate the use of some Cortisporin products. Desonide otic lotion (0.05% desonide, 2% acetic acid) is also effective and may be better tolerated than Domeboro otic solution (aluminum acetate).
Sodium sulfacetamide drops or ointment may be effective for seborrheic blepharitis. Oral tetracyclines can also be effective and have been shown to decrease the density of microorganisms in the affected follicles. Steroid preparations are suitable for short-term use but may induce glaucoma and cataracts. Daily gentle cleansing with a cotton-tipped applicator and baby shampoo in water can reduce symptoms. In severe cases, oral antibiotics or oral antifungals may be combined with topical agents. Low-dose isotretinoin has also been shown to be effective in refractory disease.
An Q, et al: High Staphylococcus epidermidis colonization and impaired permeability barrier in facial seborrheic dermatitis. Chin Med J (Engl) 2017; 130: 1662.
Balighi K, et al: Hydrocortisone 1% cream and sertaconazole 2% cream to treat facial seborrheic dermatitis. Int J Womens Dermatol 2016; 3: 107.
de Souza Leão Kamamoto C, et al: Low-dose oral isotretinoin for moderate to severe seborrhea and seborrheic dermatitis. Int J Dermatol 2017; 56: 80.
Gupta AK, et al: Topical treatment of facial seborrheic dermatitis. Am J Clin Dermatol 2017; 18: 193.
Kastarinen H, et al: Topical anti-inflammatory agents for seborrhoeic dermatitis of the face or scalp. Cochrane Database Syst Rev 2014; 5: CD009446.
Psoriasis
Clinical Features
Psoriasis is a common, chronic, and recurrent inflammatory disease of the skin characterized by circumscribed, erythematous, dry, scaling plaques of various sizes, usually covered by silvery white lamellar scales. The lesions are usually symmetrically distributed and have a predilection for the scalp, nails, extensor surfaces of the limbs, umbilical region, and sacrum. It usually develops slowly but may be exanthematous, with the sudden onset of numerous guttate (droplike) lesions ( Fig. 10.2 ). Subjective symptoms, such as itching or burning, may be present and may cause extreme discomfort.
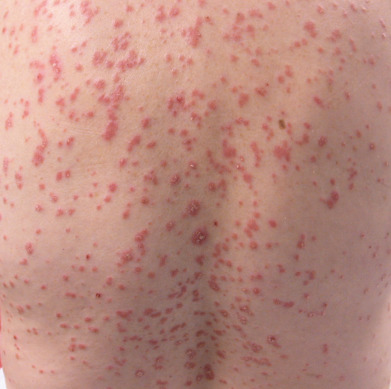
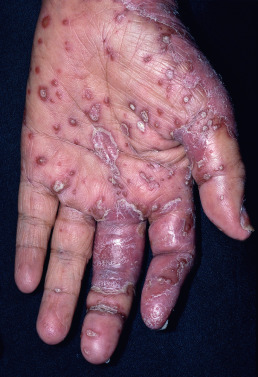
The early lesions are small, erythematous macules covered with dry, silvery scales from the onset. The lesions increase in size by peripheral extension and coalescence. The scales are micaceous, meaning they peel in layers, and are looser toward the periphery and adherent centrally. When removed, bleeding points appear (Auspitz sign). Although plaques typically predominate, lesions may be annular or polycyclic. Old patches may be thick and covered with tough lamellar scales like the outside of an oyster shell (psoriasis ostracea). Descriptive terms applied to the diverse appearance of the lesions include psoriasis guttata, in which the lesions are the size of water drops; psoriasis follicularis, in which tiny, scaly lesions are located at the orifices of hair follicles; psoriasis figurata, annulata, or gyrata, in which curved linear patterns are produced by central involution; psoriasis discoidea, in which central involution does not occur and solid patches persist; and psoriasis rupioides, in which crusted lesions occur, resembling syphilitic rupia. The term chronic plaque psoriasis is often applied to stable lesions of the trunk and extremities. Inverse psoriasis predominates in intertriginous areas ( Fig. 10.3 ). Pustular variants of psoriasis may be chronic on the palms and soles ( Fig. 10.4 ), or these may be eruptive and accompanied by severe toxicity and hypocalcemia.
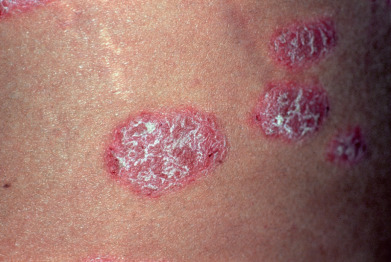
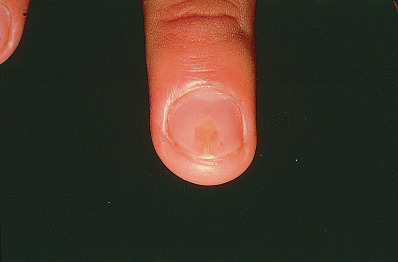
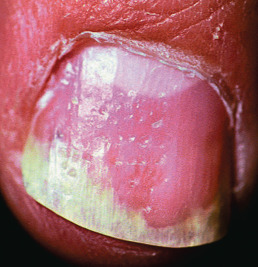
Involved nails can demonstrate distal onycholysis, random pitting caused by parakeratosis from the proximal matrix ( Fig. 10.5 ), oil spots (yellow areas of subungual parakeratosis from the distal matrix; Fig. 10.6 ), or salmon patches (nail bed psoriasis). Thick, subungual hyperkeratosis may resemble onychomycosis.
Types
Seborrheic-Like Psoriasis
Some cases of psoriasis overlap with seborrheic dermatitis. Seborrheic lesions may predominate on the face, under the breasts, and in the scalp, flexures, and axillae. Lesions in these areas are moist and erythematous, with yellow, greasy, soft scales, rather than dry and micaceous scales. Terms such as sebopsoriasis and seborrhiasis may be used to describe the condition of such patients.
Inverse Psoriasis
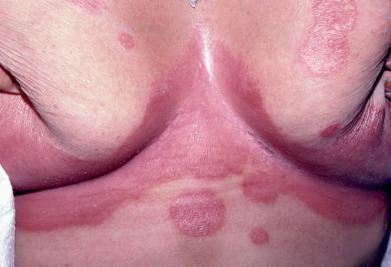
Inverse psoriasis selectively and often exclusively involves folds, recesses, and flexor surfaces, such as the ears, axillae, groin, inframammary folds ( Fig. 10.7 ), navel, intergluteal crease, penis, lips, and web spaces. Other areas, such as the scalp and nails, may be involved.
“Napkin” Psoriasis
Napkin psoriasis, or psoriasis in the diaper area, is characteristically seen in infants between 2 and 8 months of age. Lesions appear as brightly erythematous, sharply demarcated patches of skin involving much of the diaper area. The lesions typically clear with topical therapy, but psoriasis may reappear in adulthood.
Psoriatic Arthritis
Five clinical patterns of psoriatic arthritis occur, as follows:
- 1.
Asymmetric distal interphalangeal joint involvement with nail damage (16%)
- 2.
Arthritis mutilans with osteolysis of phalanges and metacarpals (5%) ( Fig. 10.8 )
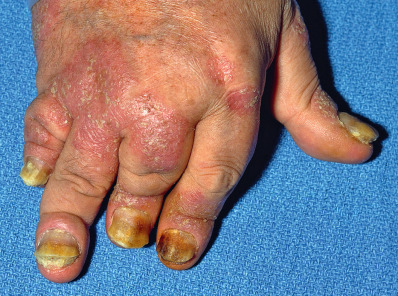
Fig. 10.8
Psoriatic arthritis.
- 3.
Symmetric polyarthritis-like rheumatoid arthritis (RA), with clawhand (15%)
- 4.
Oligoarthritis with swelling and tenosynovitis of one or a few hand joints (70%)
- 5.
Ankylosing spondylitis alone or with peripheral arthritis (5%)
Most radiographic findings resemble those in RA, but certain findings are highly suggestive of psoriasis. These include erosion of terminal phalangeal tufts (acrosteolysis), tapering or “whittling” of phalanges or metacarpals with “cupping” of proximal ends of phalanges (“pencil in a cup deformity”), bony ankylosis, osteolysis of metatarsals, predilection for distal interphalangeal and proximal interphalangeal joints, relative sparing of metacarpophalangeal and metatarsophalangeal joints, paravertebral ossification, asymmetric sacroiliitis, and rarity of “bamboo spine” when the spine is involved. Almost half the patients with psoriatic arthritis have type human leukocyte antigen (HLA)–B27.
Rest, splinting, passive motion, and nonsteroidal antiinflammatory drugs (NSAIDs) may provide symptomatic relief but do not prevent deformity. Methotrexate, cyclosporine, tacrolimus, anti-TNF, anti-IL-17 and anti-IL-12/23 agents are disease-modifying drugs that prevent deformity.
Guttate Psoriasis
In the distinctive guttate form of psoriasis, typical lesions are the size of water drops, 2–5 mm in diameter. Lesions typically occur as an abrupt eruption after acute infection, such as a streptococcal pharyngitis. Guttate psoriasis occurs mostly in patients under age 30. This type of psoriasis usually responds rapidly to broad-band ultraviolet B (UVB) at erythemogenic doses. Suberythemogenic doses often have little impact on the lesions. This is one of the few forms of psoriasis where broad-band UVB may have an advantage over narrow-band (NB) UVB. Minimal erythemogenic (erythema) dose (MED) testing is recommended to allow for appropriately aggressive treatment. Recurrent episodes may be related to pharyngeal carriage of the responsible streptococcus by the patient or a close contact. A course of a semisynthetic penicillin (e.g., dicloxacillin, 250 mg four times daily for 10 days) with rifampin (600 mg/day for adults) may be required to clear chronic streptococcal carriage.
Generalized Pustular Psoriasis (von Zumbusch Psoriasis)
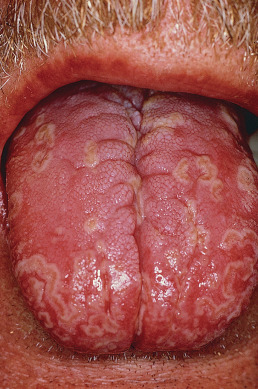
Typical patients with generalized pustular psoriasis have plaque psoriasis and often psoriatic arthritis. The onset is sudden, with formation of lakes of pus periungually, on the palms, and at the edge of psoriatic plaques. Erythema occurs in the flexures before the generalized eruption appears. This is followed by a generalized erythema and more pustules ( Fig. 10.9 ). Pruritus and intense burning are often present. Mucous membrane lesions are common. The lips may be red and scaly, and superficial ulcerations of the tongue and mouth occur. Geographic or fissured tongue frequently occurs ( Fig. 10.10 ).
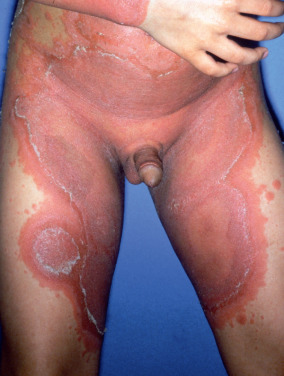
The patient is frequently ill with fever, erythroderma, hypocalcemia, and cachexia. A number of cases of acute respiratory distress syndrome associated with pustular and erythrodermic psoriasis have been reported. Other systemic complications include pneumonia, congestive heart failure, and hepatitis.
Episodes are often provoked by withdrawal of systemic corticosteroids. The authors have also observed generalized pustular psoriasis as the presenting sign of Cushing disease. Other implicated drugs include iodides, coal tar, terbinafine, minocycline, hydroxychloroquine, acetazolamide, and salicylates. There is usually a strong familial history of psoriasis. Generalized pustular psoriasis may occur in infants and children with no implicated drug. It may also occur as an episodic event punctuating the course of localized acral pustular psoriasis.
Acitretin is the drug of choice in this severe disease. The response is generally rapid. Isotretinoin is also effective. Cyclosporine, methotrexate, and biologic agents are alternatives. In some cases, dapsone is effective in doses of 50–100 mg/day.
Acrodermatitis Continua (of Hallopeau)
Typical patients develop acral erythematous plaques studded with pustules. The nail beds are heavily involved, and the fingernails float away on lakes of pus, resulting in anonychia. Hyperkeratosis often ensues, and the fingertips become increasingly painful, tapering to long, keratotic points. Occasionally, patients may develop generalized pustular flares. Acrodermatitis continua is discussed in more detail later (see Dermatitis Repens under Recalcitrant Palmoplantar Eruptions, later in this chapter).
Impetigo Herpetiformis
The term impetigo herpetiformis has been applied to pustular psoriasis of pregnancy. Flexural erythema, studded with pustules, often occurs initially, followed by a generalized pustular flare and increasing toxicity. These patients are pregnant, so systemic retinoids are not appropriate. Many patients only respond to delivery, and early delivery should be strongly considered as soon as it is safe for the infant. Alternatively, patients may respond to prednisone, 1 mg/kg/day. The corticosteroid can also contribute to neonatal lung maturity.
Keratoderma Blennorrhagicum (Reiter Syndrome)
Keratoderma blennorrhagicum resembles psoriasis both histologically and clinically, except for its tendency for thicker keratotic lesions. Patients are often positive for HLA-B27 and develop reactive arthritis and skin disease after a bout of urethritis or enteritis.
Erythrodermic Psoriasis
Patients with psoriasis may develop a generalized erythroderma ( Fig. 10.11 ). Erythrodermic psoriasis is covered in greater detail in Chapter 11 under Exfoliative Dermatitis.
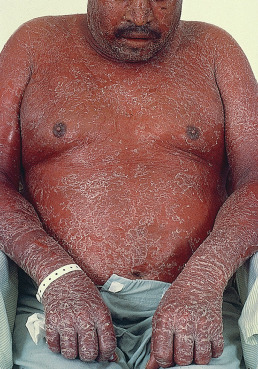
Course
The course of psoriasis is unpredictable. It usually begins on the scalp or elbows and may remain localized in the original region for years. Chronic disease may also be almost entirely limited to the fingernails. Involvement over the sacrum may easily be confused with candidiasis or tinea. Onset may also be sudden and widespread.
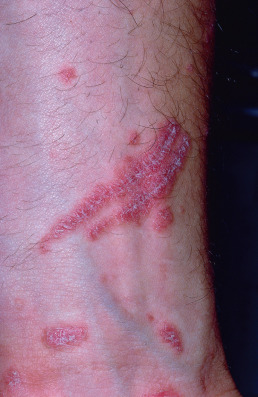
Two of the chief features of psoriasis are its tendency to recur and its persistence. The isomorphic response (Koebner phenomenon) is the appearance of typical lesions of psoriasis at sites of even trivial injury ( Fig. 10.12 ). Lesions may occur at sites of scratches, incisions, and burns. Lesions may first appear after viral exanthema or pityriasis rosea. The isomorphic response may occur if psoriatic lesions are severely burned during phototherapy. With a reduction in light dosage, the erythema and burning resolve, and the plaques begin to clear. Woronoff ring is concentric blanching of the erythematous skin at or near the periphery of a healing psoriatic plaque. It is often the first sign that the patient’s psoriasis is responding to phototherapy.
The palms and soles are sometimes exclusively affected, showing discrete, dry, erythematous scaling patches, circumscribed verrucous thickenings, or pustules on an erythematous base. The patches usually begin in the midportion of the palms or on the soles and gradually expand. Psoriasis of the palms and soles is typically chronic and extremely resistant to treatment.
Many studies report an association between hepatitis C and psoriasis, and hepatitis C virus (HCV) has also been implicated in psoriatic arthritis. If treatment of psoriasis is to include a potentially hepatotoxic drug, such as methotrexate, a full hepatitis panel should be obtained. Also, IFN treatment of the hepatitis can further exacerbate or induce psoriasis. Anti–tumor necrosis factor (TNF)–α therapy shows promise in the treatment of psoriasis, even in the setting of chronic HCV infection.
Inheritance
In a large study of psoriasis in monozygotic twins, heritability was high and environmental influence low. Patients with psoriasis often have relatives with the disease, and the incidence typically increases in successive generations. Multifactorial inheritance is likely. Analysis of population-specific HLA haplotypes has provided evidence that susceptibility to psoriasis is linked to major histocompatibility complex (MHC) classes I and II on human chromosome 6. A number of genetic loci are linked to psoriasis, including PSORS1 on chromosome 6 and within the MHC, and PSORS2 on chromosome 17q. Also, there are two subsets that differ in age of onset and frequency of HLA associations. Early onset is type I psoriasis and is associated mostly with Cw6, B57, and DR7. Late onset is type II and predominantly features Cw2. PSORS9 has also been confirmed as a susceptibility locus for psoriasis.
A variety of other HLA associations have been reported. It is believed that any individual who has B13 or B17 carries a fivefold risk of developing psoriasis. In pustular psoriasis, HLA-B27 may be seen, whereas B13 and B17 are increased in guttate and erythrodermic psoriasis. In palmoplantar pustulosis, there is an association with HLA-B8, Bw35, Cw7, and DR3. HLA typing is a research tool for population-based studies, but of limited value in assessing an individual patient.
Epidemiology
Psoriasis occurs with equal frequency in men and women. Between 1% and 2% of the U.S. population has psoriasis. It occurs less frequently in the tropics. It is less common in North American and West African black persons. Native (Indian) Americans and native Fijians rarely have psoriasis. The onset of psoriasis is at a mean age of 27 years, but the range is wide, from the neonatal period to the seventies. Severe emotional stress tends to aggravate psoriasis in almost half of those studied.
In pregnancy, there is a distinct tendency for improvement or even temporary disappearance of lesions in the majority of women studied. After childbirth, there is a tendency for exacerbation of lesions. Paradoxically, pregnancy is also the milieu for impetigo herpetiformis, and psoriasis may behave differently from one pregnancy to another in the same patient.
A high prevalence of celiac disease has been noted in patients with psoriasis. Lymphoma also has an increased incidence in these patients, and psoriasis has been linked to the metabolic syndrome and a higher risk of cardiovascular disease, although early age of onset does not appear to correlate with greater risk. Patients should be screened for comorbidities.
Pathogenesis
Psoriasis is a hyperproliferative disorder, but the proliferation is driven by a complex cascade of inflammatory mediators. Psoriasis appears to represent a mixed T-helper 1 (Th1) and Th17 inflammatory disease. Th17 cells appear to be more proximal in the inflammatory cascade. T cells and cytokines play pivotal roles in the pathophysiology of psoriasis. Overexpression of type 1 cytokines, such as IL-2, IL-6, IL-8, IL-12, IFN-γ, and TNF-α, has been demonstrated, and overexpression of IL-8 leads to the accumulation of neutrophils. The main signal for Th1 development is IL-12, which promotes intracellular IFN-γ production. In animal models, shifting from Th1 to Th2 responses improves psoriasis. IL-4 is capable of inducing Th2 responses and improving psoriasis. Reduced expression of the antiinflammatory cytokines IL-1RA and IL-10 has been found, and polymorphisms for IL-10 genes correlate with psoriasis. IL-10 is a type 2 cytokine with major influence on immunoregulation, inhibiting type 1 proinflammatory cytokine production. Patients receiving established traditional therapies show rising levels of IL-10 messenger RNA expression, suggesting that IL-10 may have antipsoriatic capacity.
IL-15 triggers inflammatory cell recruitment, angiogenesis, and production of inflammatory cytokines, including IFN-γ, TNF-α, and IL-17, all of which are upregulated in psoriatic lesions. The interplay is complex, but IL-17 appears to be proinflammatory, and IL-22 may serve to retard keratinocyte differentiation. IL-23 stimulates survival, as well as proliferation of Th17 cells. Circulating NK cells are reduced in psoriasis.
Streptococci
Streptococci play a role in some patients. Patients with psoriasis report sore throat more often than controls. β-Hemolytic streptococci of Lancefield groups A, C, and G can cause exacerbation of chronic plaque psoriasis. Th1 cells recognize cell wall extract isolated from group A streptococci. HLA variation has a significant effect on the immune response to group A streptococci.
Stress
Various studies have shown a positive correlation between stress and severity of disease. In almost half of patients studied, stress appears to play a significant role.
Drug-Induced Psoriasis
Psoriasis may be induced by β-blockers, lithium, antimalarials, terbinafine, calcium channel blockers, captopril, glyburide, granulocyte colony-stimulating factor, interleukins, interferons, and lipid-lowering drugs. Systemic steroids may cause rebound or pustular flares. Antimalarials are associated with erythrodermic flares, but patients traveling to malaria-endemic regions should take appropriate prophylaxis. Often, drugs such as doxycycline or mefloquine are appropriate for the geographic area, but when a quinine derivative offers the best protection, it is generally better to take the prophylactic doses of a quinine derivative than to risk disease and full-dose treatment.
Pathology
Histologically, all psoriasis is pustular. The microscopic pustules include spongiform intraepidermal pustules, and Munro microabscesses within the stratum corneum. In early guttate lesions, focal parakeratosis is noted within the stratum corneum. The parakeratotic focus typically has an outline resembling a seagull. Neutrophils are generally noted immediately above the focus of parakeratosis, but in some sections the neutrophils will not be visible as a result of sampling error. In plaque psoriasis, neutrophilic foci are so numerous that they are rarely missed. Neutrophilic microabscesses are generally present at multiple levels in the stratum corneum, usually on top of small foci of parakeratosis. These foci generally alternate with areas of orthokeratotic stratum corneum, suggesting that the underlying spongiform pustules arise in a rhythmic fashion. The granular layer is absent focally, corresponding to areas producing foci of parakeratosis. In well-developed plaques, there is regular epidermal acanthosis with long, bulbous rete ridges, thinning over the dermal papillae, and dilated capillaries within the dermal papillae. The last two findings correlate with the Auspitz sign. The stratum corneum may be entirely parakeratotic but still shows multiple small, neutrophilic microabscesses at varying levels. Spongiosis is typically scant, except in the area immediately surrounding collections of neutrophils.
In pustular psoriasis, geographic tongue, and Reiter syndrome, intraepidermal spongiform pustules tend to be much larger. Grossly pustular lesions often have little associated acanthosis. In Reiter syndrome, the stratum corneum is often massively thickened, with prominent foci of neutrophils above parakeratosis, alternating with orthokeratosis.
Acral lesions often demonstrate nondiagnostic features histologically. Spongiosis is typically prominent in these lesions and often leads to a differential diagnosis of psoriasis or chronic psoriasiform spongiotic dermatitis. Foci of neutrophils often contain serum and may be interpreted as impetiginized crusting.
On direct immunofluorescence testing, the stratum corneum demonstrates intense fluorescence with all antibodies, complement, and fibrin. This fluorescence is independent of the fluorescent label, as it has been noted in hematoxylin and eosin–stained sections and frozen unstained sections. The same phenomenon of stratum corneum autofluorescence has been noted in some cases of candidiasis that demonstrate a psoriasiform histology.
Psoriasis can generally be distinguished from dermatitis by the paucity of edema, relative absence of spongiosis, tortuosity of the capillary loops, and presence of neutrophils above foci of parakeratosis. Neutrophils in the stratum corneum are often seen in tinea, impetigo, candidiasis, and syphilis, but they rarely are found atop parakeratosis alternating with orthokeratosis rhythmically. In psoriasiform syphilis, the rete ridges are typically long and slender; a vacuolar interface dermatitis is usually present; dermal blood vessels appear to have no lumen because of endothelial swelling; and plasma cells are present in the dermal infiltrate. About one third of biopsies of syphilis lack plasma cells, but the remaining characteristics still suggest the correct diagnosis. Psoriasiform lesions of mycosis fungoides exhibit epidermotropism of large lymphocytes with little spongiosis. The lymphocytes are typically larger, darker, and more angulated than the lymphocytes in the dermis. There is associated papillary dermal fibrosis, and the superficial perivascular infiltrate is asymmetrically distributed around the postcapillary venules, favoring the epidermal side (“bare underbelly sign”).
Clinical Differential Diagnosis
Psoriasis must be differentiated from dermatomyositis (DM), lupus erythematosus (LE), seborrheic dermatitis, pityriasis rosea, lichen planus, eczema, and psoriasiform syphilid. The distribution in psoriasis is on the extensor surfaces, especially of the elbows and knees, and on the scalp; DM shares this distribution, whereas LE generally lacks involvement of the extensor surfaces. Patients with DM may exhibit a heliotrope sign, atrophy, poikiloderma, and nailfold changes. Advanced lesions of discoid LE often demonstrate follicular hyperkeratosis (carpet tack sign). Seborrheic dermatitis has a predilection for the eyebrows, nasolabial angle, ears, sternal region, and flexures. The scales in psoriasis are dry, white, and shiny, whereas those in seborrheic dermatitis are greasy and yellowish. On removal of the scales in psoriasis, blood oozes from the capillaries (Auspitz sign), whereas this does not occur in seborrheic dermatitis.
In pityriasis rosea, the eruption is located on the upper arms, trunk, and thighs, and the duration is over weeks. Lesions are typically oval and follow skin tension lines. Individual lesions show a crinkling of the epidermis and collarette scaling. A herald patch is frequently noted. Lichen planus chiefly affects the flexor surfaces of the wrists and ankles. Often the violaceous color is pronounced. In darker-skinned individuals, the lesions have a tendency to pronounced hyperpigmentation. The nails are not pitted as in psoriasis, but longitudinally ridged, rough, and thickened. Pterygium formation is characteristic of lichen planus.
Hand eczema may resemble psoriasis. In general, psoriatic lesions tend to be more sharply marginated, but at times the lesions are indistinguishable. Psoriasiform syphilid has infiltrated copper-colored papules, often arranged in a figurate pattern. Serologic tests for syphilis are generally positive, but prozone reactions may occur, and the serum may have to be diluted to obtain a positive test. Generalized lymphadenopathy and mucous patches may be present.
Treatment
Topical therapy, intralesional triamcinolone, excimer laser, light emitting diode (LED), and other forms of focused light may be suitable for limited plaques. Phototherapy remains highly cost-effective for widespread psoriasis. Cyclosporine has a rapid onset of action but is generally not suitable for sustained therapy. Methotrexate remains the systemic agent against which others are compared. Biologic agents can produce dramatic responses at dramatic expense.
Topical Treatment
Corticosteroids.
Topical application of corticosteroids in creams, ointments, lotions, foams, and sprays is the most frequently prescribed therapy for localized psoriasis. Class I steroids are suitable for 2-week courses of therapy on most body areas. Therapy can be continued with pulse applications on weekends to reduce the incidence of local adverse effects. On the scalp, corticosteroids in propylene glycol, gel, foam, and spray bases are preferred by most white patients. Black patients may find them drying and may prefer oil and ointment preparations. Low- to medium-strength creams are preferred in the intertriginous areas and on the face. To augment effectiveness of topical corticosteroids in areas with thick keratotic scale, the area should be hydrated before application and covered with an occlusive dressing of polyethylene film (plastic wrap) or a sauna suit. Side effects include epidermal atrophy, steroid acne, miliaria, and pyoderma.
Intralesional injections of triamcinolone are helpful for refractory plaques. Triamcinolone acetonide (Kenalog) suspension, 10 mg/mL, may be diluted with sterile saline to make a concentration of 2.5–5 mg/mL. Good results are also obtained in the treatment of psoriatic nails by injecting triamcinolone into the region of the matrix and the lateral nailfold. A digital block can be performed before injection to provide anesthesia. Injections are given once a month until the desired effect is achieved.
Tars.
Crude coal tar and tar extracts such as liquor carbonis detergens (LCD) can be compounded into agents for topical use. Tar bath oils and shampoos are readily available. Oil of cade (pine tar) or birch tar in concentrations of 5%–10% may also be incorporated into ointments. The odor of all tars may be offensive, and relapse is more rapid than with topical agents such as calcipotriene.
Anthralin.
Anthralin is effective but is irritating and stains skin, clothing, and bedding. To avoid these drawbacks, short-contact anthralin treatment (SCAT) can be helpful, with anthralin washed off after 15–30 minutes. Anthralin exerts a direct effect on keratinocytes and leukocytes by suppressing neutrophil superoxide generation and inhibiting monocyte-derived IL-6, IL-8, and TNF-α.
Tazarotene.
Tazarotene is a nonisomerizable retinoic acid receptor–specific retinoid. It appears to treat psoriasis by modulating keratinocyte differentiation and hyperproliferation, as well as by suppressing inflammation. Combining its use with a topical corticosteroid and weekend pulse therapy can decrease irritation.
Calcipotriene.
Vitamin D 3 affects keratinocyte differentiation partly through its regulation of epidermal responsiveness to calcium. Treatment with the vitamin D analog calcipotriene (Dovonex) in ointment, cream, or solution form has been effective in the treatment of plaque-type and scalp psoriasis. Combination therapy with calcipotriene and high-potency steroids may provide greater response rates, fewer side effects, and steroid sparing. Calcipotriene is unstable in the presence of many other topical agents and degrades in the presence of UV light. Monitoring of serum calcium levels in adults is not required. Calcipotriene plus betamethasone dipropionate is more effective than either agent alone.
Macrolactams (Calcineurin Inhibitors).
Topical macrolactams such as tacrolimus and pimecrolimus are especially helpful for thin lesions in areas prone to atrophy or steroid acne. The burning associated with these agents can be problematic but may be avoided by prior corticosteroid treatment and application to dry skin rather than after bathing.
Salicylic Acid.
Salicylic acid is used as a keratolytic agent in shampoos, creams, and gels. It can promote the absorption of other topical agents. Widespread application may lead to salicylate toxicity, manifesting with tinnitus, acute confusion, and refractory hypoglycemia, especially in patients with diabetes and those with compromised renal function.
Ultraviolet Light.
Phototherapy is a cost-effective and underused modality for psoriasis. In most cases, sunlight improves psoriasis. However, severe burning of the skin may cause the Koebner phenomenon and an exacerbation. Artificial UVB light is produced by fluorescent bulbs in broad-band or NB spectrum. Maximal effect is usually achieved at MEDs. Although suberythemogenic doses can be effective, the response is slower than with erythemogenic regimens. With treatment, a tanning response occurs, and the dose must be increased to maintain efficacy. Maintenance UVB phototherapy after clearing contributes to the duration of remission and is justified for many patients.
Using a monochromator, it has been shown that wavelengths of 254, 280, and 290 nm are ineffective; at 296, 300, 304, and 313 nm, however, there is clearing. NB UVB (peak emission about 311 nm) is now widely available.
Goeckerman Technique.
Goeckerman therapy remains an effective and cost-effective method of treatment even in patients with poor responses to biologic agents. In its modern form, a 2%–5% tar preparation is applied to the skin, and a tar bath is taken at least once a day. The excess tar is removed with mineral or vegetable oil, and UV light is given. In psoriasis day care centers, patients clear in an average of 18 days, and 75% remain free of disease for extended periods. The addition of a topical corticosteroid to the Goeckerman regimen shortens the time required for remission. Phototoxic reactions (tar smarts) may result from UVA generated by the predominantly UVB bulbs.
Ingram Technique.
Ingram therapy consists of a daily coal tar bath in a solution such as 120 mL LCD to 80 L of warm water. This is followed by daily exposure to UV light for increasing periods. An anthralin paste is then applied to each psoriatic plaque. Talcum powder is sprinkled over the lesions, and stockinette dressings are applied. Modern versions of the technique employ SCAT.
PUVA Therapy.
High-intensity longwave UV radiation (UVA) given 2 hours after ingestion of 8-methoxypsoralen (Oxsoralen-Ultra), twice a week, is highly effective, even in severe psoriasis. Most patients clear in 20–25 treatments, but maintenance treatment is needed.
Although PUVA therapy is highly effective, in patients with less than 50% of the skin surface affected, UVB may be as effective. Polyethylene sheet bath PUVA is another therapeutic alternative to oral psoralen–UVA. The patient is immersed in a psoralen solution contained in plastic sheeting that conforms to the patient’s body.
Oral psoralen can produce cataracts, and protective eyewear must be used. PUVA therapy is a risk factor for skin cancer, including squamous cell carcinoma (SCC) and melanoma. Arsenic exposure is a more significant cofactor than prior exposure to methotrexate, UVB, or concomitant use of topical tar. Men treated without genital protection are at an increased risk of developing SCC of the penis and scrotum. Although the risk of cancer is dose related, there is no definitive threshold dose of cumulative PUVA exposure above which carcinogenicity can be predicted.
Surgical Treatment
In patients with pharyngeal colonization by streptococci, an excellent response has been reported after tonsillectomy. More effective antibiotic regimens, such as a 10-day course of dicloxacillin combined with rifampin (600 mg/day for adult), have largely replaced tonsillectomy.
Hyperthermia
Local hyperthermia can clear psoriatic plaques, but relapse is usually rapid. Microwave hyperthermia may produce significant complications, such as pain over bony prominences and tissue destruction.
Occlusive Treatment
Occlusion with surgical tape or dressings can be effective as monotherapy or when combined with topical drugs.
Systemic Treatment
Corticosteroids.
The hazards of the injudicious use of systemic corticosteroids must be emphasized. There is great risk of “rebound” or induction of pustular psoriasis when therapy is stopped. Corticosteroid use is generally restricted to unique circumstances, such as impetigo herpetiformis when expeditious delivery is not possible.
Methotrexate.
This folic acid antagonist remains the standard against which other systemic treatments are measured. Methotrexate has a greater affinity for dihydrofolic acid reductase than does folic acid. The indications for methotrexate include psoriatic erythroderma, psoriatic arthritis, acute pustular psoriasis (von Zumbusch type), or widespread body surface area (BSA) involvement. Localized pustular psoriasis or palmoplantar psoriasis that impairs normal function and employment may also require systemic treatment.
It is important to ensure the patient has no history of liver or kidney disease. Methotrexate can be toxic to the liver, and decreased renal clearance can enhance toxicity. Other important factors to consider are alcohol abuse, cryptogenic cirrhosis, severe illness, debility, pregnancy, leukopenia, thrombocytopenia, active infectious disease, immunodeficiency, anemia, colitis, and ability to comply with directions. Hepatic enzymes, bilirubin, serum albumin, creatinine, alkaline phosphatase, complete blood count, platelet count, hepatitis serology (B and C), HIV antibody, a test for tuberculosis, and urinalysis should all be evaluated before starting treatment. Patients with hypoalbuminemia have a higher risk of developing pulmonary complications.
The need for liver biopsy remains controversial. Biopsy is not without risks and is not usually performed in the setting of methotrexate therapy for rheumatic disease. However, patients with psoriasis have a greater risk of liver disease than other patient populations. Weekly blood counts and monthly liver enzyme assessment are recommended at the onset of therapy or when the dosage is changed, but hepatitis fibrosis can occur without elevations in liver enzymes. Monitoring of aminoterminal procollagen III peptide may reduce or eliminate the need for liver biopsy.
Numerous treatment schedules have evolved, and the liquid for injection may be dosed orally in orange juice as a less expensive alternative to pills. The authors recommend either three divided oral doses (12 hours apart) weekly, weekly single doses orally, or single weekly subcutaneous injections. The weekly dose varies from 5 mg to more than 50 mg, with most patients requiring 15–30 mg a week. Once a single dose exceeds 25 mg, oral absorption is unpredictable, and subcutaneous injections are recommended. Midweek doses can result in severe toxicity and must be avoided. Oral or cutaneous ulceration may be a sign that the patient has taken a midweek dose. Oral folic acid has been reported to decrease side effects, especially nausea, and doses of 1–4 mg/day are used. Oral folic acid is not adequate for the treatment of overdosage, and leukovorin must be used in such cases.
Cyclosporine.
The therapeutic benefit of cyclosporine in psoriatic disease may be related to downmodulation of proinflammatory epidermal cytokines. The microemulsion formulation Neoral has greater bioavailability and is now standard. Doses of 2–5 mg/kg/day generally produce rapid clearing of psoriasis, with both efficacy and risk being dose related. Unfortunately, the lesions recur rapidly as well, and transition to another form of therapy is required. Treatment durations of up to 6 months are associated with a low incidence of renal complications, but blood pressure and serum creatinine must be monitored and doses adjusted accordingly. Usually, the dose is reduced if the baseline creatinine increases by one third. Some data support the feasibility of pulse dosing for a few days each week for both the induction and the maintenance of response in psoriasis patients.
Diet.
The antiinflammatory effects of fish oils rich in n-3 polyunsaturated fatty acids (PUFAs) have been demonstrated in RA, inflammatory bowel disease, psoriasis, and asthma. The n-3 and n-6 PUFAs affect a variety of cytokines, including IL-1, IL-6, and TNF. Herbal remedies have also been used with variable effects. Many of these products are unpalatable, and their efficacy does not compare favorably to pharmacologic agents.
Oral Antimicrobial Therapy.
The association of streptococcal pharyngitis with guttate psoriasis is well established. Staphylococcus aureus and streptococci secrete exotoxins that act as superantigens, producing massive T-cell activation, and pharyngeal colonization should be addressed as previously noted. Oral bile acid supplementation has been shown to improve psoriasis, presumably by affecting the microflora and endotoxins in the gut. Oral ketoconazole, itraconazole, and other antibiotics have shown efficacy in a limited number of patients with psoriasis.
Retinoids.
Oral treatment with the aromatic retinoid ethylester etretinate has been effective in many patients with psoriasis, especially in pustular disease. Because of its long half-life, etretinate has been replaced by acitretin. Alcohol ingestion can convert acitretin to etretinate and is discouraged. 13- Cis -retinoic acid can also produce good results in some patients with pustular psoriasis. All these drugs are potent teratogens, and elevated triglyceride levels may complicate therapy. Combinations of retinoic acids with photochemotherapy can be effective in chronic plaque psoriasis, resulting in lowered cumulative doses of light.
Dapsone.
Dapsone use is limited largely to palmoplantar pustulosis or other variants of pustular psoriasis. Even in this setting, it is a second- or third-line agent with limited efficacy.
Biologic Agents
A number of biologic agents are available that can produce dramatic responses in some patients with psoriasis; all are expensive. Retrospective analysis using BSA multiplied by physician’s global assessment as an endpoint suggests that outcomes with biologic agents are superior to those with other systemic agents, despite the patients taking biologics having a higher baseline severity and a greater number of previous treatments.
Several agents block TNF-α. Infliximab is a chimeric monoclonal antibody (mAb) to TNF-α and requires intravenous infusion; etanercept is a fusion protein of human TNF type II receptor and the Fc region of immunoglobulin (Ig)G1; and adalimumab is a recombinant, fully human IgG1 mAb to TNF-α. Alefacept is a fusion protein of the external domain of LFA-3 and the Fc region of IgG1; it blocks T-cell activation and triggers apoptosis of pathogenic T cells, but was withdrawn from the market in the United States. Golimumab is an anti-TNF agent with less frequent dosing used in patients with psoriatic arthritis, and certolizumab has also demonstrated efficacy. Ustekinumab, a human mAb against IL-12 and IL-23, blocks the inflammatory pathway at a more proximal point than anti-TNF agents. Guselkumab is an IL-23 receptor monoclonal antibody. Ixekizumab and secukinumab are IL-17A antagonists. Brodalumab is a human, anti–IL-17RA monoclonal antibody.
Percentage of Patients Clearing With Each Drug.
Published data allow for some comparisons of biologic agents, but the endpoints of some trials differ. Newer anti–IL-17 and anti-IL-23 agents can achieve PASI 100 in some patients, a dramatic improvement over previous biologic agents. The anti–IL-17 agents include secukinumab, ixekizumab, and brodalumab. A meta-analysis of published trials of the older biologics suggested that of the agents studied at the end of the induction phase (week 24), ustekinumab had the greatest probability of achieving at least 75% improvement from baseline in the psoriasis area and severity index (PASI 75), followed by infliximab, adalimumab, and etanercept. The percentage of patients reaching PASI 75 at week 10 is about 70% with infliximab at 3 mg/kg and 90% at 5 mg/kg, compared with 6% for placebo. About 35% of patients receiving etanercept, 25 mg subcutaneously twice weekly, achieve PASI 75 at 12 weeks and 45% at 24 weeks. With the 50-mg induction dose administered twice a week, about 46% of patients achieve PASI 75 at 12 weeks and 50% at 24 weeks. The data available suggest that about 53% of patients taking 40 mg of adalimumab every other week achieve PASI 75 by week 12, and about 80% of those taking 40 mg a week achieve PASI 75.
Risks.
Anti-TNF agents are contraindicated with demyelinating disease and anti-IL-17 agents are contraindicated with inflammatory bowel disease. The anti-TNF agents may induce flares of psoriasis through upregulation of plasmacytoid dendritic cells. This may be a class effect. The biologic agents all suppress the normal immune response. Infliximab has been associated with reactivation of tuberculosis, demyelinating disease, and serious systemic opportunistic infection. Infliximab may also lose its effect because of neutralizing antibodies. Methotrexate or azathioprine may be needed as concomitant therapy to reduce the incidence of neutralizing antibodies and infusion reactions. Even though adalimumab is a fully human antibody, it may also induce an antibody response. Serious infections have been reported in RA patients treated with this agent. Etanercept has been associated with infection, onset, or exacerbation of multiple sclerosis, vasculitis, and LE-like manifestations. All these effects are rare and may not be statistically increased from the general population. Many of the reported complications, such as lymphoma, demyelinating disease, progressive multifocal leukoencephalopathy and infection, are not unique to any one immunosuppressive agent.
The National Psoriasis Foundation has endorsed a recommendation that all patients be screened for latent tuberculosis infection before any immunologic therapy. The Foundation recommends delaying immunologic therapy until prophylaxis for latent tuberculosis infection is completed, although noting that patients with severe disease may be treated after 1–2 months of prophylaxis. IFN-γ assays have greater specificity than tuberculin skin tests and are being used along with imaging studies to confirm tuberculosis in patients with positive skin tests.
Phosphodiesterase Inhibitors
Apremilast, a small molecule specific inhibitor of phosphodiesterase 4, has demonstrated efficacy in recalcitrant plaque psoriasis. It is also indicated for psoriatic arthritis. Diarrhea is the most common adverse effect. Other adverse reactions include nausea, depression, upper respiratory tract infection, and headache.
Janus Kinase Inhibitors
Janus kinase (JAK) inhibitors such as tofacitinib have demonstrated efficacy in the treatment of psoriasis, including nail psoriasis. The side-effect profile of tofacitinib includes dose-dependent decreases in red blood cell counts, along with transient or reversible dose-dependent decreases in neutrophil counts. Tofacitinib has also demonstrated transient increases in lymphocyte counts, primarily attributable to increases in B-cell counts.
Combination Therapy
In more severe forms of psoriasis, a combination of treatment modalities may be employed. In treating patients with methotrexate, for example, concomitant topical agents may be used to minimize the dose. Methotrexate has been combined with infliximab to reduce the incidence of neutralizing antibodies, and also has been used with acitretin in managing patients with severe, generalized pustular psoriasis. Recent evidence suggests that neutralizing antibodies correlated with loss of response to biologics other than infliximab, suggesting a broader role for combination therapy. The use of PUVA and retinoids is called Re-PUVA and has been studied extensively. Acitretin has been combined with biologic agents to treat refractory psoriasis. Combination systemic therapy has the potential to reduce overall toxicity if the toxicities of each agent are different. However, new regimens should be used with caution because of the potential for cumulative toxicity or drug interaction.
Evolving Therapies
Alternative therapies for psoriasis include mycophenolate mofetil, sulfasalazine, paclitaxel, azathioprine, fumaric acid esters, climatotherapy, and grenz ray therapy. A3 adenosine receptor agonists are also being developed. Nail disease can respond to systemic agents, topical retinoids, local triamcinolone injections, and topical 5-fluorouracil. The latter agent can cause onycholysis if applied to the free edge of the nail.
Colombo MD, et al: Cyclosporine regimens in plaque psoriasis. Scientific World Journal 2013; 2013: 805705.
Elman SA, Weinblatt M, Merola JF. Targeted therapies for psoriatic arthritis: an update for the dermatologist. Semin Cutan Med Surg. 2018 Sep;37(3):173-181. doi: 10.12788/j.sder.2018.045. PubMed PMID: 30215635.
Fitzmaurice S, et al: Goeckerman regimen for management of psoriasis refractory to biologic therapy. J Am Acad Dermatol 2013; 69: 648.
Gladman DD, et al: Treating psoriasis and psoriatic arthritis. J Rheumatol 2017; 44: 519.
Hawkes JE, Yan BY, Chan TC, Krueger JG. Discovery of the IL-23/IL-17 Signaling Pathway and the Treatment of Psoriasis. J Immunol. 2018 Sep 15;201(6):1605-1613. doi: 10.4049/jimmunol.1800013. Review. PubMed PMID: 30181299; PubMed Central PMCID: PMC6129988.
Ho D, et al: A systematic review of light emitting diode (LED) phototherapy for treatment of psoriasis. J Drugs Dermatol 2017; 16: 482.
Kim BR, et al: Methotrexate in a real-world psoriasis treatment. Ann Dermatol 2017; 29: 346.
Langley RG, et al: Efficacy and safety of guselkumab in patients with psoriasis who have an inadequate response to ustekinumab. Br J Dermatol 2018; 178: 114.
Merola JF, et al: Efficacy of tofacitinib for the treatment of nail psoriasis. J Am Acad Dermatol 2017; 77: 79.
Millsop JW, et al: Diet and psoriasis, part III. J Am Acad Dermatol 2014; 71: 561.
Mota F, et al: Importance of immunogenicity testing for cost-effective management of psoriasis patients treated with adalimumab. Acta Dermatovenerol Alp Pannonica Adriat 2017; 26: 33.
Murage MJ, Tongbram V, Feldman SR, Malatestinic WN, Larmore CJ, Muram TM, Burge RT, Bay C, Johnson N, Clifford S, Araujo AB. Medication adherence and persistence in patients with rheumatoid arthritis, psoriasis, and psoriatic arthritis: a systematic literature review. Patient Prefer Adherence. 2018 Aug 21;12:1483-1503. doi: 10.2147/PPA.S167508. eCollection 2018. Review. PubMed PMID: 30174415; PubMed Central PMCID: PMC6110273.
Pereira R, et al: Infection and malignancy risk in patients treated with TNF inhibitors for immune-mediated inflammatory diseases. Curr Drug Saf 2017; 12: 162.
Prasad V, et al: Performance evaluation of non-ionic surfactant based tazarotene encapsulated proniosomal gel for the treatment of psoriasis. Mater Sci Eng C Mater Biol Appl 2017; 79: 168.
Saleem MD, et al: Comorbidities in patients with psoriasis. J Am Acad Dermatol 2017; 77: 191.
Spadaccini M, et al: PDE4 Inhibition and inflammatory bowel disease. Int J Mol Sci 2017; 18: E1276.
van de Kerkhof PC: Biologics for psoriasis. J Dermatolog Treat 2017; 28: 281.
Yiu ZZ, Warren RB. Ustekinumab for the treatment of psoriasis: an evidence update. Semin Cutan Med Surg. 2018 Sep;37(3):143-147. doi: 10.12788/j.sder.2018.040. PubMed PMID: 30215630.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree