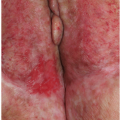
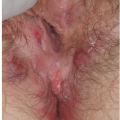
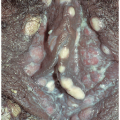
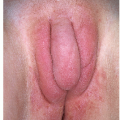
Principles of Genital Diagnosis and Therapy
Peter J. Lynch
GENERAL PRINCIPLES OF DIAGNOSIS
Correct diagnosis is the sine qua non for the care of any patient with any disorder. If you don’t know the diagnosis you can’t establish the cause, provide the prognosis, or institute appropriate therapy. For patients with mucocutaneous disease a working diagnosis is almost always first established on the basis of clinical symptoms and signs. If necessary, this clinical diagnosis can subsequently be confirmed through procedures such as biopsy, cytology, and microbial culture (see Chapter 3).
There are two major approaches to using clinical symptoms and signs to establish a working diagnosis: the use of visual memory and the use of a morphologically determined diagnostic algorithm. Dermatologists by virtue of repeated exposure to patients with both common and uncommon diseases almost always depend on visual memory. And, because it works for them, they consistently use that same approach when teaching medical students and other clinicians. Thus, in the classroom or at continuing medical education courses, they bombard their audience with clinical photo after clinical photo, leaving the participants with a jumbled mass of impossible to remember images of skin disease.
The use of visual memory works for the dermatologist because of sufficient, repetitive exposure to these diseases. But other clinicians, encountering fewer patients with mucocutaneous disorders, lack the opportunity for sufficient visual reinforcement to dependably recognize uncommon and rare diseases. By analogy, they are put in the position of someone attending a large gathering where they know few of the guests. In spite of many introductions, the names of those they have met quickly disappear from memory. At best, on subsequent encounter, one might remember the face as vaguely familiar but find it impossible to identify the person by name. The same problem occurs for the nondermatologist in a clinical setting. In this situation, when faced with an unrecognized mucocutaneous disorder, one might futilely turn to a standard dermatology textbook but find that the diseases in it are organized on the basis of etiology or pathophysiology. This is, of course, of no help, as one must know the diagnosis first before it is possible to make use of the material contained in such a book. As a last resort one might then end up paging through an atlas hoping to stumble on a disease that matches what was just found on examination of the patient. At best this offers a hit or miss approach and even when it is helpful, it is an inefficient and mostly inaccurate approach to diagnosis.
A better diagnostic approach for the nondermatologist is the use of a diagnostic algorithm in which the diseases are organized on the basis of clinical morphology. This type of diagnostic algorithm directs the clinician to a cluster of diseases that share similarities in appearance. Once having arrived at the correct group of diseases, reading a small amount of text describing the characteristic diagnostic features together with perusal of the associated clinical photos for each disease within that group allows one to arrive at a likely diagnosis that then can be confirmed by a biopsy or other diagnostic test. Importantly, this approach even allows a clinician to make a correct diagnosis of a disorder that he or she has never previously encountered.
Of course, to use a morphologic approach like this, one must be able to describe in dermatologic terms the features that one has seen on examination. This is not very difficult because, as is true for most “foreign” languages, a relatively small number of words can serve one’s basic needs. The dermatologic words that are required for this approach together with the diagnostic algorithm that uses them (Table 2-1) are contained below.
As is true in all fields of medicine, history and physical examination represent the first two steps in diagnosis; they are covered in this chapter. A third step, that of utilizing diagnostic procedures to confirm a clinical diagnosis, is covered in the next chapter.
Initial Approach to the Patient: History and Physical Examination
There are at least two good approaches that can be used in obtaining the initial history. Some clinicians prefer using a questionnaire that can be completed by the patient either at home or in the office prior to first contact with the clinician. One of us (LE) utilizes this approach and she has made her questionnaire available at her online site, www.libbyedwardsmd.com. This may be downloaded, modified, and subsequently used by any clinician. This approach allows the patient to express what he or she feels is important and minimizes any discomfort a patient may have about beginning a discussion
about genital and/or sexual problems. Alternatively, one of us (PJL) takes the initial history after the patient is placed in the examination room but, importantly, before the patient is asked to disrobe. With either alternative a more directed history is then taken during or after the examination.
about genital and/or sexual problems. Alternatively, one of us (PJL) takes the initial history after the patient is placed in the examination room but, importantly, before the patient is asked to disrobe. With either alternative a more directed history is then taken during or after the examination.
TABLE 2.1 Algorithm for the diagnosis of genital disorders | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
The two key points in examination of patients with genital problems are exposure and illumination. First, in a misguided attempt to protect patient modesty, some clinicians erroneously allow the patient to determine the extent of clothing to be removed. This leads patients to believe that they can simply pull underwear partially down or to one side whereas, in fact, all clothing covering the anogenital area must be completely removed.
Second, nearly all examinations should take place with the patient lying supine on the examination table. Women can then be examined either in a “frog leg” position or with their feet in stirrups. The latter is preferred as it allows for good visualization of the anal area. Men are usually examined the “frog leg” position as they fairly strenuously resist being placed in stirrups. For men, the anal area can be examined either with the patient rolled to his side or with him standing but bending forward over the examination table. It cannot be emphasized strongly enough: the genital area in men cannot be adequately examined with the patient seated or standing.
Good lighting is required for all examinations. This requires use of a light separate from a fixed ceiling light: one that is adequately bright and that is flexible enough so that it can be moved to illuminate every aspect of the anogenital region. Needless to say, except in extraordinary circumstances examination of a patient of the sex opposite to that of the clinician should be carried out in the presence of a chaperone.
Definition of Dermatologic Terms
The definitions included here are very similar, though not necessarily identical, to those found in standard dermatology textbooks. The differences, where they occur, will not significantly interfere with the use of the diagnostic algorithm that follows.
Macule. A macule is a small (1.5 cm or less), nonelevated, nonpalpable area of color change. The surface of macules is usually smooth, though a small amount of powdery scale may be present.
Patch. A patch is a larger (greater than 1.5 cm), nonelevated, nonpalpable area of color change. It may be considered as a two-dimensional (length and width) increase in the size of a macule. Again, the surface is usually smooth but sometimes a small amount of powdery scale may be present.
Papule. A papule is a small (1.5 cm or less) palpable lesion. Usually, but not always, a papule is visibly elevated above the surface of the surrounding tissue. A palpable lesion contained within the skin is a papule whether or not it is visibly elevated. A papule may be considered as a onedimensional (lesional thickness) increase in the size of a macule. Papules may be either smooth or rough surfaced. Roughness on the surface of a papule is due to the presence of either scale or crust.
Plaque. A plaque is a large (greater than 1.5 cm) flattopped, palpable lesion. It may be considered as a two-dimensional (length and width) increase in the size of a papule. Plaques are usually, but not always, elevated above the surface of the surrounding tissue. As for papules, intracutaneous lesions that are palpable are termed plaques whether or not they are elevated. Likewise, plaques may be smooth or rough surfaced. Roughness on the surface of a plaque is due to the presence of scale or crust.
Nodule. A nodule is a large (greater than 1.5 cm) dome-shaped, palpable lesion. It may be considered as a three-dimensional (length, width, and depth) increase in the size of a papule. Nodules are usually smooth surfaced.
Vesicle. A vesicle is a small (1.0 cm or less) fluid-filled blister. It may be considered as a fluid-filled papule in which the fluid is loculated. Fluid-filled papules in which the fluid is nonloculated are known as wheals. Vesicles and wheals are differentiated clinically by the observation that when the surface of a blister is pierced, the fluid runs out and the blister collapses. When a wheal is pierced, a drop of fluid may appear on the surface but the papule remains
as it was before the piercing. When the surface of a vesicle has been removed or has disintegrated, an erosion is left.
as it was before the piercing. When the surface of a vesicle has been removed or has disintegrated, an erosion is left.
Pustule. A pustule is a vesicle that contains visibly purulent (pus-filled) fluid. That is, the lesion appears opaquely white, yellow, or yellow-white. This color occurs as a result of the presence of packed neutrophils and other white blood cells. Note that a vesicle may turn cloudy as it ages. This change does not make it a pustule. To be a pustule, a blister must have been purulent from the time of its inception.
Bulla (plural: bullae). A bulla is a large (greater than 1.0 cm) vesicle. Here too, the fluid is loculated. Usually the fluid is found in a single compartment occupying the whole of the lesion but, uncommonly, coalescence of closely set vesicles occurs to form a multiloculated bulla.
Erosion. An erosion is a shallow defect in the surface of the skin. In this context “shallow” means the epidermis is missing but the defect does not extend more deeply into the dermal component of the skin. The base of an erosion may be red and moist or the base may be covered with crust. In an erosion any crust that is present is yellow in color and is crumbly and easily removed. Erosions occur as the result of two mechanisms. They can develop subsequent to trauma, most often as a result of scratching. Erosions due to trauma are usually linear or angular in appearance. Alternatively, erosions may occur when the roof of a blister is removed or disintegrates. Such erosions are usually round and generally have a thin peripheral rim of scale. This is called “collarette” scale and it occurs as a result of fragments of the peripheral blister roof that remain intact at the edge of a previous blister.
Fissure. A fissure is a subtype of an erosion in which a thin (less than 1 mm wide), linear crack occurs into or through the epithelium. A fissure appears clinically as a thin red line and possibly may not be recognized as a true defect in the surface of the skin unless a magnifying lens is used. Fissures generally arise in the setting of an epithelial surface that is too dry. They are analogous to the cracked surface present in the bed of a dried pond or stream.
Ulcer. An ulcer is a deep defect in the surface of the skin. The defect is deeper than that of an erosion and extends into, or even through, the dermal connective tissue. Such a defect involves significant blood vessel damage and, as a result, the base of an ulcer may contain crust that includes heme pigment as well as plasma proteins. Such crust may be red, blue, or black. When considerable fibrin is present as well, the crust is very adherent to the base of the ulcer; such crust is known as “eschar.”
Scale and crust. Scale is due to excess keratin on the surface of a lesion. It generally occurs as a result of epithelial hyperproliferation. The presence of scale indicates that the epithelial surface is intact. Scale is usually visible as gray, white, or silver “flakes” on the surface of a lesion. However, sometimes, especially on moist surfaces, scale is not visible at all and is only recognized as being present when a slight sense of roughness is palpable on the surface of a lesion. Crust is due to the presence of plasma proteins left after the water component of plasma has evaporated. It occurs as a result of an epithelial defect (erosion or ulcer). Crust is always visible and is usually yellow but may be red, blue, or black if heme pigment is present.
Margination. Margination refers to the zone of transition between normal and lesional tissue as would be visualized in a cross-sectional view of the lesion. This transition can be very distinct (sharply marginated) or somewhat indistinct (poorly, or diffusely marginated). Margination can be helpful in distinguishing the papulosquamous diseases such as psoriasis from the eczematous diseases such as atopic dermatitis.
Configuration. Configuration refers to the shape of the lesions when viewed from above. Most often, this shape is round or slightly oval. Gyrate (serpiginous) margination occurs in urticaria whereas linear and angular shapes suggest a traumatic etiology, especially that due to scratching.
Eczema. In this book, “eczema” is used synonymously with “dermatitis.” Both refer to a pattern of disease characterized by the presence of red, scaling, poorly marginated papules and plaques displaying evidence of epithelial disruption. Epithelial disruption is identified by the presence of visible excoriations, fissures, weeping, crusting, and/or yellow-colored scale (see Chapter 4). Note that, although we disagree with this usage, some clinicians use the term “eczema” as a synonym for “atopic dermatitis.”
Lichenification. Lichenification refers to the presence of thickened, rough surfaced (scaling) skin with prominent skin markings. It occurs as a callus-like response due to chronic rubbing. Lichenification is characteristically seen in the two related conditions of atopic dermatitis and lichen simplex chronicus (see Chapter 4).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree