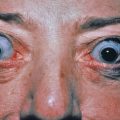
The body requires a certain amount of heat, but beyond definite limits, insufficient or excessive amounts are injurious. The local action of excessive heat causes burns or scalds; undue cold causes chilblains, frostbite, and congelation. Thresholds of tolerance exist in all body structures sensitive to electromagnetic wave radiation of varying frequencies, such as x-rays and ultraviolet (UV) rays. The skin, which is exposed to so many external physical forces, is more subject to injuries caused by this radiation than any other organ.
Heat Injuries
Thermal Burns
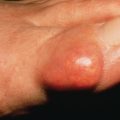
Injury of varying intensity may be caused by the action of excessive heat on the skin ( Fig. 3.1 ). If this heat is extreme, the skin and underlying tissue may be destroyed. The changes in the skin resulting from dry heat or scalding are classified in four degrees, as follows:
- •
First-degree burns of the skin result merely in an active congestion of the superficial blood vessels, causing erythema that may be followed by epidermal desquamation (peeling). Ordinary sunburn is the most common example of a first-degree burn. The pain and increased surface heat may be severe, and some constitutional reaction can occur if the involved area is large.
- •
Second-degree burns are subdivided into superficial and deep forms.
- •
In the superficial second-degree burn, there is a transudation of serum from the capillaries, which causes edema of the superficial tissues. Vesicles and bullae are formed by the serum gathering beneath the outer layers of the epidermis. Complete recovery without scarring is usual in patients with superficial burns.
- •
The deep second-degree burn is pale and anesthetic. Injury to the reticular dermis compromises blood flow and destroys appendages, so healing takes more than 1 month and results in scarring.
- •
- •
Third-degree burns involve loss of the full thickness of the dermis and often some of the subcutaneous tissues. Because the skin appendages are destroyed, there is no epithelium available for regeneration of the skin. An ulcerating wound is produced, which on healing leaves a scar.
- •
Fourth-degree burns involve the destruction of the entire skin, including the subcutaneous fat, and any underlying tendons.
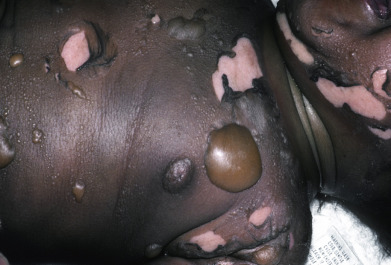
Both third-degree and fourth-degree burns require grafting for closure. All third- and fourth-degree burns are followed by constitutional symptoms of varying severity, depending on the size of the involved surface, the depth of the burn, and particularly the location of the burned surface. The more vascular the involved area, the more severe are the symptoms.
The prognosis is poor for any patient in whom a large area of skin surface is involved, particularly if more than two thirds of the body surface has been burned. Women, infants, and toddlers all have a greater risk of death from burns than men. Excessive scarring, with either keloid-like scars or flat scars with contractures, may produce deformities and dysfunction of the joints, as well as chronic ulcerations from impairment of local circulation. Delayed postburn blistering may occur in partial-thickness wounds and skin graft donor sites. It is most common on the lower extremities and is self-limited. Although burn scars may be the site of development of carcinoma, evidence supports only the possibility of a modest excess of squamous cell carcinomas in burn scars. With modern reconstructive surgery, this unfortunate end result can be minimized.
Treatment
Immediate first aid for minor thermal burns consists of prompt cold applications (ice water, or cold tap water if no ice is available), which are continued until pain does not return on stopping them.
The vesicles and bullae of second-degree burns should not be opened but should be protected from injury because they form a natural barrier against contamination by microorganisms. If they become tense and unduly painful, the fluid may be evacuated under strictly aseptic conditions by puncturing it with a sterile needle, allowing collapse onto the underlying wound. Excision of full-thickness and deep dermal wounds that will not reepithelialize within 3 weeks (as soon as hemodynamic stability is achieved, normally 2–3 days) reduces wound infections, shortens hospital stays, and improves survival. Additionally, contractures and functional impairment may be mitigated by such intervention. Skin grafting, or coverage with biologic dressings such as allograft or xenograft skin, cultured epidermal autografts, or skin substitutes also assist in healing. The role of early ablative laser treatments to prevent disabling scars and its use in improving fully formed scars is an area of active investigation. The most superficial wounds may be dressed with greasy gauze, whereas silver-containing dressings are used for their antibiotic properties in intermediate wounds.
Fluid resuscitation, treatment of inhalation injury and hypercatabolism, monitoring and early intervention of sepsis, pain control, environmental control, and nutritional support are key components of the critical care of burns. Intensive care management in a burn center is recommended for patients with partial-thickness wounds covering more than 10% of the body surface, if involving the face, hands, feet, genitalia, perineum, or joints; if secondary to electrical, chemical, or inhalation injury; in patients with special needs; and for any full-thickness burn.
Electrical Burns
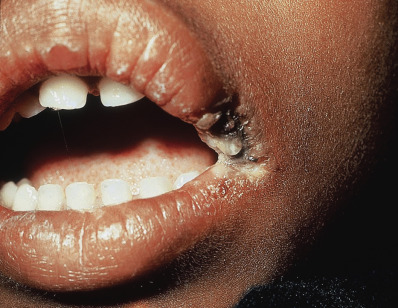
Electrical burns may occur from contact or as a flash exposure. A contact burn is small but deep, causing some necrosis of the underlying tissues. Low-voltage injuries usually occur in the home, are treated conservatively, and generally heal well. Oral commissure burns may require reconstructive procedures ( Fig. 3.2 ). High-voltage burns are often occupational; internal damage may be masked by minimal surface skin change and may be complicated by subtle and slowly developing sequelae. Early surgical intervention to improve circulation and repair vital tissues is helpful in limiting loss of the extremity.
Flash burns usually cover a large area and, being similar to any surface burn, are treated as such. Lightning may cause burns after a direct strike, where an entrance and an exit wound are visible. This is the most lethal type of strike, and cardiac arrest or other internal injuries may occur. Other types of lightning strike are indirect and result in the following burns:
- •
Linear burns in areas on which sweat was present
- •
Burns in a feathery or arborescent pattern, which is believed to be pathognomonic
- •
Punctate burns with multiple, deep, circular lesions
- •
Thermal burns from ignited clothing or heated metal, which may occur if the patient was speaking on a cell phone or listening to an iPod or similar device when struck
Hot Tar Burns
Polyoxyethylene sorbitan in bacitracin zinc–neomycin–polymyxin B (e.g., Neosporin) ointment, vitamin E ointment, and sunflower oil are excellent dispersing agents that facilitate the removal of hot tar from burns.
Alemayehu H, et al: Management of electrical and chemical burns in children. J Surg Res 2014; 190: 210.
Carta T, et al: Use of mineral oil Fleet enema for the removal of a large tar burn. Burns 2015; 41: e11.
Compton CC: The delayed postburn blister. Arch Dermatol 1992; 128: 24.
El-Zawahry BM, et al: Ablative CO2 fractional resurfacing in treatment of thermal burn scars. J Cosmet Dermatol 2015; 14: 324.
Esteban-Vives R, et al: Second-degree burns with six etiologies treated with autologous noncultured cell-spray grafting. Burns 2016; 42: e99.
Heffernan EJ, et al: Thunderstorms and iPods. N Engl J Med 2007; 357: 198.
Kalantar Motamedi MH, et al: Prevalence and pattern of facial burns. J Oral Maxillofac Surg 2015; 73: 676.
Russell KW, et al: Lightning burns. J Burn Care Res 2014; 35: e436.
Saracoglu A, et al: Prognostic factors in electrical burns. Burns 2014; 40: 702.
Sheridan RL, Greenhalgh D: Special problems in burns. Surg Clin North Am 2014; 94: 781.
Sokhal AK, et al: Clinical spectrum of electrical burns. Burns 2017; 43: 182.
Wallingford SC, et al: Skin cancer arising in scars: a systematic review. Dermatol Surg 2011; 37: 1239.
Wang KA, et al: Epidemiology and outcome analysis of hand burns. Burns 2015; 41: 1550.
Miliaria
Miliaria, the retention of sweat as a result of occlusion of eccrine sweat ducts, produces an eruption that is common in hot, humid climates, such as in the tropics and during the hot summer months in temperate climates. Staphylococcus epidermidis, which produces an extracellular polysaccharide substance, induces miliaria in an experimental setting. This polysaccharide substance may obstruct the delivery of sweat to the skin surface. The occlusion prevents normal secretion from the sweat glands, and eventually pressure causes rupture of the sweat gland or duct at different levels. The escape of sweat into the adjacent tissue produces miliaria. Depending on the level of the injury to the sweat gland or duct, several different forms are recognized.
Miliaria Crystallina
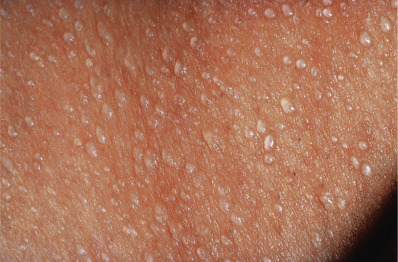
Miliaria crystallina is characterized by small, clear, superficial vesicles with no inflammatory reaction ( Fig. 3.3 ). It appears in bedridden patients whose fever produces increased perspiration or when clothing prevents dissipation of heat and moisture, as in bundled children. Hypernatremia without fever may induce it. The lesions are generally asymptomatic, and their duration is short-lived because they tend to rupture at the slightest trauma. Drugs such as isotretinoin, adrenergic/cholinergic drugs, and doxorubicin may induce it. The lesions are self-limited; no treatment is required.
Miliaria Rubra (Prickly Heat)
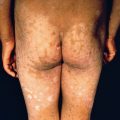
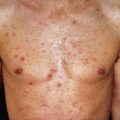
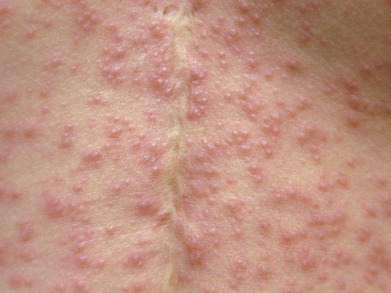
The lesions of miliaria rubra appear as discrete, extremely pruritic, erythematous papulovesicles ( Fig. 3.4 ) accompanied by a sensation of prickling, burning, or tingling. They later may become confluent on a bed of erythema. The sites most frequently affected are the antecubital and popliteal fossae, trunk, inframammary areas (especially under pendulous breasts), abdomen (especially at the waistline), and inguinal regions; these sites frequently become macerated because evaporation of moisture has been impeded. Exercise-induced itching or that of atopic dermatitis may also be caused by miliaria rubra. The site of injury and sweat escape is in the prickle cell layer, where spongiosis is produced.
Miliaria Pustulosa
Miliaria pustulosa is preceded by another dermatitis that has produced injury, destruction, or blocking of the sweat duct. The pustules are distinct, superficial, and independent of the hair follicle. The pruritic pustules occur most frequently on the intertriginous areas, flexural surfaces of the extremities, scrotum, and back of bedridden patients. Contact dermatitis, lichen simplex chronicus, and intertrigo are some of the associated diseases, although pustular miliaria may occur several weeks after these diseases have subsided. Recurrent episodes may be a sign of type I pseudohypoaldosteronism, because salt-losing crises may precipitate miliaria pustulosa or rubra, with resolution after stabilization.
Miliaria Profunda
Nonpruritic, flesh-colored, deep-seated, whitish papules characterize miliaria profunda. It is asymptomatic, usually lasts only 1 hour after overheating has ended, and is concentrated on the trunk and extremities. Except for the face, axillae, hands, and feet, where there may be compensatory hyperhidrosis, all the sweat glands are nonfunctional. The occlusion is in the upper dermis. Miliaria profunda is observed only in the tropics and usually follows a severe bout of miliaria rubra.
Postmiliarial Hypohidrosis
Postmiliarial hypohidrosis results from occlusion of sweat ducts and pores, and it may be severe enough to impair an individual’s ability to perform sustained work in a hot environment. Affected persons may show decreasing efficiency, irritability, anorexia, drowsiness, vertigo, and headache; they may wander in a daze.
It has been shown that hypohidrosis invariably follows miliaria, and that the duration and severity of the hypohidrosis are related to the severity of the miliaria. Sweating may be depressed to half the normal amount for as long as 3 weeks.
Tropical Anhidrotic Asthenia
Tropical anhidrotic asthenia is a rare form of miliaria with long-lasting poral occlusion, which produces anhidrosis and heat retention.
Treatment
The most effective treatment for miliaria is to place the patient in a cool environment. Even a single night in an air-conditioned room helps to alleviate the discomfort. Circulating air fans can also be used to cool the skin. Anhydrous lanolin resolves the occlusion of pores and may help to restore normal sweat secretions. Hydrophilic ointment also helps to dissolve keratinous plugs and facilitates the normal flow of sweat. Soothing, cooling baths containing colloidal oatmeal or cornstarch are beneficial if used in moderation. Patients with mild cases may respond to dusting powders, such as cornstarch or baby talcum powder.
Chao CT: Hypernatremia-related miliaria crystallina. Clin Esp Nephrol 2014; 18: 831.
Haque MS, et al: The oldest new finding in atopic dermatitis. JAMA Dermatol 2013; 149: 436.
Mowad CM, et al: The role of extracellular polysaccharide substance produced by Staphylococcus epidermidis in miliaria. J Am Acad Dermatol 1995; 20: 713.
Onal H, et al: Miliaria rubra and thrombocytosis in pseudohypoaldosteronism. Platelets 2012; 23: 645.
Erythema Ab Igne
Erythema ab igne is a persistent erythema—or the coarsely reticulated residual pigmentation resulting from it—that is usually produced by long exposure to excessive heat without the production of a burn ( Fig. 3.5 ). It begins as a mottling caused by local hemostasis and becomes a reticulated erythema, leaving pigmentation. Multiple colors are simultaneously present in an active patch, varying from pale pink to old rose or dark purplish brown. After the cause is removed, the affection tends to disappear gradually, but sometimes the pigmentation is permanent.
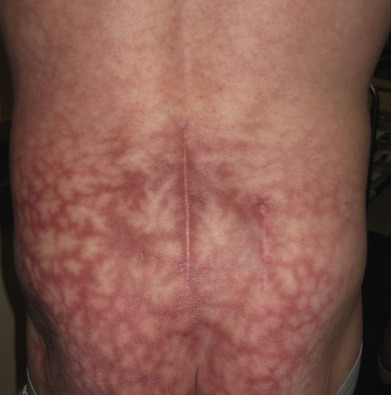
Histologically, an increased amount of elastic tissue in the dermis is noted. The changes in erythema ab igne are similar to those of actinic elastosis. Interface dermatitis and epithelial atypia may be noted.
Erythema ab igne on the legs results from habitually warming them in front of open fireplaces, space heaters, or car heaters. Similar changes may be produced on the lower back or at other sites of an electric heating pad application, on the upper thighs with laptop computers, or on the posterior thighs from heated car seats. The reason for chronically exposing the skin to heat may be pain from an underlying cancer, or from a condition which predisposes to a feeling of cold, such as anorexia nervosa. The condition occurs also in cooks, silversmiths, and others exposed over long periods to direct moderate heat.
Epithelial atypia, which may lead to Bowen disease and squamous cell carcinoma, has rarely been reported to occur overlying erythema ab igne. In remote areas of Kashmir, Kangri fire pots can induce erythema ab igne and cancer within the affected area. Treatment with 5-fluorouracil (5-FU), imiquimod, or photodynamic therapy may be effective in reversing this epidermal alteration.
The use of emollients containing α-hydroxy acids or a cream containing fluocinolone acetonide 0.01%, hydroquinone 4%, and tretinoin 0.05% may help reduce the unsightly pigmentation, as may treatment with the Q-switched neodymium-doped yttrium-aluminum-garnet (Nd:YAG) laser.
Brodell D, et al: Automobile seat heater-induced erythema ab igne. Arch Dermatol 2012; 148: 264.
Dessinoti C, et al: Erythema ab igne in three girls with anorexia nervosa. Pediatr Dermatol 2016; 333: e149.
Kim HW, et al: Erythema ab igne successfully treated with low fluenced 1,064-nm Q-switched neodymium-doped yttrium aluminum garnet laser. J Cosmet Laser Ther 2014; 16: 147.
Riahi RR, et al: Practical solutions to prevent laptop-induced erythema ab igne. Int J Dermatol 2014; 53: e395.
Wani I: Kangri cancer. Surgery 2010; 147: 586.
Wharton JB, et al: Squamous cell carcinoma in situ arising in the setting of erythema ab igne. J Drugs Dermatol 2008; 7: 488.
Cold Injuries
Exposure to cold damages the skin by at least three mechanisms:
- •
Reduced temperature directly damages the tissue, as in frostbite and cold immersion foot.
- •
Vasospasm of vessels perfusing the skin prevents adequate perfusion of the tissue and causes vascular injury and consequent tissue injury (pernio, acrocyanosis, and frostbite).
- •
In unusual circumstances, adipose tissue is predisposed to damage by cold temperatures because of fat composition or location (cold panniculitis; see Chapter 23 ).
Outdoor workers and recreationalists, military service members, alcoholic persons, and homeless people are particularly likely to sustain cold injuries. Maneuvers to treat orthopedic injuries or heatstroke and cooling devices for other therapeutic use may result in cold injuries ranging from acrocyanosis to frostbite. Holding ice coated with salt (salt and ice challenge) will induce cold-induced blistering.
Heil K, et al: Freezing and non-freezing cold weather injuries. Br Med Bull 2016; 117: 79.
Roussel LO, et al: Tweens feel the burn. Int J Adolesc Med Health 2016; 28: 217.
Acrocyanosis
Acrocyanosis is a persistent blue discoloration of the entire hand or foot worsened by cold exposure. The hands and feet may be hyperhidrotic ( Fig. 3.6 ). It occurs chiefly in young women. Cyanosis increases as the temperature decreases and changes to erythema with elevation of the dependent part. The cause is unknown. Smoking should be avoided. Acrocyanosis is distinguished from Raynaud syndrome by its persistent (rather than episodic) nature and lack of tissue damage (ulceration, distal fingertip resorption).
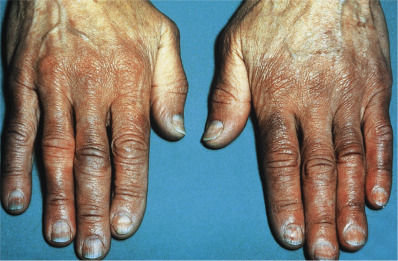
Acrocyanosis with swelling of the nose, ears, and dorsal hands may occur after inhalation of butyl nitrite. Interferon alpha-2a and beta may induce it. Repeated injection of the dorsal hand with narcotic drugs may produce lymphedema and an appearance similar to the edematous phase of scleroderma. This so-called puffy hand syndrome may include erythema or a bluish discoloration of the digits. Patients with anorexia nervosa frequently manifest acrocyanosis as well as perniosis, livedo reticularis, and acral coldness. It may improve with weight gain. Approximately one third of patients with skin findings of POEMS syndrome (polyneuropathy, organomegaly, endocrinopathy, M component, skin changes) have acrocyanosis. Also, in patients with a homozygous mutation in SAMDH1 and cerebrovascular occlusive disease, acrocyanosis was frequent.
Acral vascular syndromes, such as gangrene, Raynaud phenomenon, and acrocyanosis, may be a sign of malignancy. In 47% of 68 reported cases, the diagnosis of cancer coincided with the onset of the acral disease. If such changes appear or worsen in an elderly patient, especially a man, without exposure to vasoconstrictive drugs or prior autoimmune or vascular disorders, a paraneoplastic origin should be suspected.
Del Giudice P, et al: Hand edema and acrocyanosis. Arch Dermatol 2006; 142: 1084.
Dessinoti C, et al: Erythema ab igne in three girls with anorexia nervosa. Pediatr Dermatol 2016; 333: e149.
Kurklinsky AK, et al: Acrocyanosis. Vasc Med 2011; 16: 288.
Masuda H, et al: Bilateral foot acrocyanosis in an interferon-β-treated MS patient. Intern Med 2016; 55: 319.
Miest RY, et al: Cutaneous manifestations in patients with POEMS syndrome. Int J Dermatol 2013; 52: 1349.
Poszepczynska-Guigné E, et al: Paraneoplastic acral vascular syndrome. J Am Acad Dermatol 2002; 47: 47.
Xin B, et al: Homozygous mutation in SAMHD1 gene causes cerebral vasculopathy and early onset stroke. Proc Natl Acad Sci USA 2011; 108: 5372.
Pernio (Chilblains, Perniosis)
Pernio constitutes a localized erythema and swelling caused by exposure to cold. Blistering and ulcerations may develop in severe cases. In people predisposed by poor peripheral circulation, even moderate exposure to cold may produce chilblains. Cryoglobulins, cryofibrinogens, antiphospholipid antibodies, or cold agglutinins may be present and pathogenic. Chilblain-like lesions may occur in discoid and systemic lupus erythematosus (SLE; chilblain lupus), particularly the TREX1-associated familial type, as a presenting sign of leukemia cutis, or if occurring in infancy may herald the Nakajo-Nishimura syndrome or the Aicardi-Goutières and Singleton-Merten syndrome. The chronic use of crack cocaine and its attendant peripheral vasoconstriction will lead to perniosis with cold, numb hands and atrophy of the digital fat pads, especially of the thumbs and index fingers, as well as nail curvature.
Pernio occur chiefly on the feet, hands, ears, and face, chiefly in women; onset is enhanced by dampness ( Fig. 3.7 ). In surgery technicians, the hands are affected if an orthopedic cold therapy system is used; the skin under the device develops the lesions. The lateral thighs are involved in women equestrians who ride on cold, damp days and the hips in those wearing tight-fitting jeans with a low waistband. Wading across cold streams may produce similar lesions. Nondigital lesions of cold injury can be nodular.
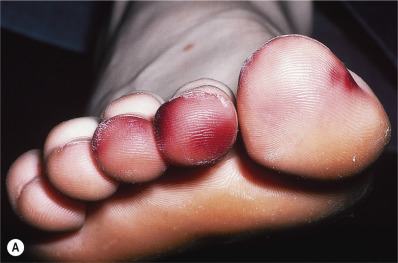
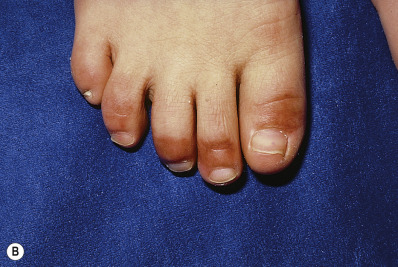
Patients with chilblains are often unaware of the cold injury when it is occurring, but later burning, itching, and redness call it to their attention. The affected areas are bluish red, with the color partially or totally disappearing on pressure, and are cool to the touch. Sometimes the extremities are clammy because of excessive sweating. As long as the dampness and cold exposure continues, new lesions will continue to appear. Investigation into an underlying cause should be undertaken in patients with pernio that is recurrent, chronic, extending into warm seasons, or poorly responsive to treatment.
Pernio histologically demonstrates a lymphocytic vasculitis. There is dermal edema, and a superficial and deep perivascular, tightly cuffed, lymphocytic infiltrate. The infiltrate involves the vessel walls and is accompanied by characteristic “fluffy” edema of the vessel walls.
Treatment
The affected parts should be protected against further exposure to cold or dampness. If the feet are involved, woolen socks should be worn at all times during the cold months. Because patients are often not conscious of the cold exposure that triggers the lesions, appropriate dress must be stressed, even if patients say they do not sense being cold. Because central cooling triggers peripheral vasoconstriction, keeping the whole body (not just the affected extremity) warm is critical. Heating pads may be used judiciously to warm the parts. Smoking is strongly discouraged.
Nifedipine, 20 mg three times a day, has been effective. Vasodilators such as nicotinamide, 500 mg three times a day, or dipyridamole, 25 mg three times a day, or the phosphodiesterase inhibitor sildenafil, 50 mg twice daily, may be used to improve circulation. Pentoxifylline and hydroxychloroquine may be effective. Spontaneous resolution occurs without treatment in 1–3 weeks. Systemic corticoid therapy is useful in chilblain lupus.
Al-Sudany NK: Treatment of primary perniosis with oral pentoxifylline (a double-blind placebo-controlled randomized therapeutic trial). Dermatol Ther 2016; 29: 263.
Baker JS, Miranpuri S: Perniosis a case report with literature review. J Am Podiatr Med Assoc 2016; 106: 138.
Ferrara G, Cerroni L: Cold-associated perniosis of the thighs (“equestrian-type” chilblain). Am J Dermatopathol 2016; 38: 726.
Günther C, et al: Familial chilblain lupus due to a novel mutation in the exonuclease III domain of 3′ repair exonuclease 1 (TREX1). JAMA Dermatol 2015; 151: 426.
Kanazawa N: Nakajo-Nishimura syndrome. Allergol Int 2012; 61: 197.
King JM, et al: Perniosis induced by a cold-therapy system. Arch Dermatol 2012; 148: 1101.
Mireku KA, et al: Tender macules and papules on the toes. JAMA Dermatol 2014; 150: 329.
Payne-James JJ, et al: Pseudosclerodermatous triad of perniosis, pulp atrophy and parrot-beaked clawing of the nails. J Forensic Leg Med 2007; 14: 65.
Tran C, et al: Chilblain-like leukaemia cutis. BMJ Case Rep 2016 Apr 19; 2016.
Weismann K, et al: Pernio of the hips in young girls wearing tight-fitting jeans with a low waistband. Acta Derm Venereol 2006; 86: 558.
Frostbite
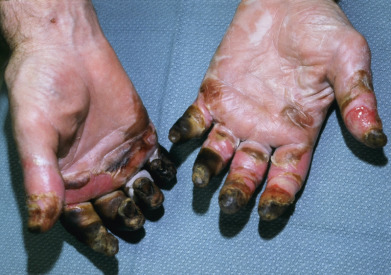
When soft tissue is frozen and locally deprived of blood supply, the damage is called frostbite. The ears, nose, cheeks, fingers, and toes are most often affected. The frozen part painlessly becomes pale and waxy. Various degrees of tissue destruction similar to that caused by burns are encountered. These are erythema and edema, vesicles and bullae, superficial gangrene, deep gangrene, and injury to muscles, tendons, periosteum, and nerves ( Fig. 3.8 ). The degree of injury is directly related to the temperature and duration of freezing. African Americans are at increased risk of frostbite. Arthritis of the small joints of the hands and feet may appear months to years later.
Treatment
Early treatment of frostbite before swelling develops should consist of covering the part with clothing or with a warm hand or other body surface to maintain a slightly warm temperature so that adequate blood circulation can be maintained. Rapid rewarming in a water bath between 37°C and 43°C (100°F and 110°F) is the treatment of choice for all forms of frostbite. Rewarming should be delayed until the patient has been removed to an area where there is no risk of refreezing. Slow thawing results in more extensive tissue damage. Analgesics should be administered because of the considerable pain experienced with rapid thawing. When the skin flushes and is pliable, thawing is complete. The use of tissue plasminogen activator to lyse thrombi decreases the need for amputation if given within 24 hours of injury. Infusion of the vasodilator iloprost may be used if available. Supportive measures such as bed rest, a high-protein/high-calorie diet, wound care, and avoidance of trauma are imperative. Any rubbing of the affected part should be avoided, but gentle massage of proximal portions of the extremity that are not numb may be helpful.
The use of anticoagulants to prevent thrombosis and gangrene during the recovery period has been advocated. Pentoxifylline, ibuprofen, and aspirin may be useful adjuncts. Antibiotics should be given as a prophylactic measure against infection, and tetanus immunization should be updated. Recovery may take many months. Injuries that affect the proximal phalanx or the carpal or tarsal area, especially when accompanied by a lack of radiotracer uptake on bone scan, have a high likelihood of requiring amputation. Whereas prior cold injury is a major risk factor for recurrent disease, sympathectomy may be preventive against repeated episodes. Arthritis may be a late complication.
Heil K, et al: Freezing and non-freezing cold weather injuries. Br Med Bull 2016; 117: 79.
Johnson-Arbor K: Digital frostbite. N Engl J Med 2014; 370: e3.
McIntosh SE, et al: Wilderness Medical Society practice guidelines for the prevention and treatment of frostbite. Wilderness Environ Med 2014; 25: S43.
Wang Y, et al: Frostbite arthritis. Am J Phys Med Rehabil 2016; 95: e28.
Immersion Foot Syndromes
Trench Foot
Trench foot results from prolonged exposure to cold, wet conditions without immersion or actual freezing. The term is derived from trench warfare in World War I, when soldiers stood, sometimes for hours, in trenches with a few inches of cold water in them. Fishermen, sailors, and shipwreck survivors may be seen with this condition. The lack of circulation produces edema, paresthesias, and damage to the blood vessels. Similar findings may complicate the overuse of ice, cold water, and fans by patients trying to relieve the pain associated with erythromelalgia. Gangrene may occur in severe cases. Treatment consists of removal from the causal environment, bed rest, and restoration of the circulation. Other measures, such as those used in the treatment of frostbite, should be employed.
Warm Water Immersion Foot
Exposure of the feet to warm, wet conditions for 48 hours or more may produce a syndrome characterized by maceration, blanching, and wrinkling of the soles and sides of the feet ( Fig. 3.9 ). Itching and burning with swelling may persist for a few days after removal of the cause, but disability is temporary. This condition was often seen in military service members in Vietnam but has also been seen in persons wearing insulated boots.
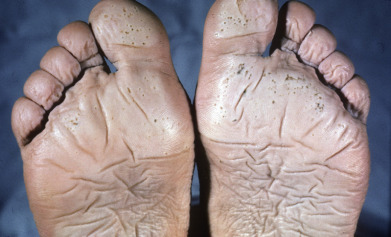
Warm water immersion foot should be differentiated from tropical immersion foot, seen after continuous immersion of the feet in water or mud at temperatures above 22°C (71.6°F) for 2–10 days. This was known as “paddy foot” in Vietnam. It involves erythema, edema, and pain of the dorsal feet, as well as fever and adenopathy ( Fig. 3.10 ). Resolution occurs 3–7 days after the feet have been dried.
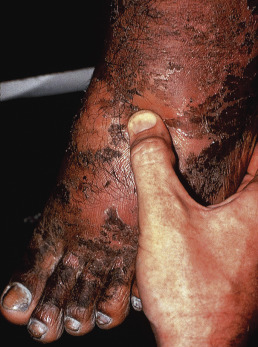
Warm water immersion foot can be prevented by allowing the feet to dry for a few hours in every 24 or by greasing the soles with a silicone grease once a day. Recovery is usually rapid if the feet are thoroughly dry for a few hours.
Adnot J, et al: Immersion foot syndromes. In: James WD (ed): Military Dermatology. Washington, DC: Office of the Surgeon General, 1994.
Davis MD: Immersion foot associated with the overuse of ice, cold water, and fans. J Am Acad Dermatol 2013; 69: 169.
Olson Z, Kman N: Immersion foot. J Emerg Med 2015; 49: e45.
Actinic Injury
Sunburn and Solar Erythema
The solar spectrum has been divided into different regions by wavelength. The parts of the solar spectrum important in photomedicine include UV radiation (below 400 nm), visible light (400–760 nm), and infrared radiation (beyond 760 nm). Visible light has limited biologic activity, except for stimulating the retina. Infrared radiation is experienced as radiant heat. Below 400 nm is the UV spectrum, divided into three bands: UVA, 320–400 nm; UVB, 280–320 nm; and UVC, 200–280 nm. UVA is divided into two subcategories: UVA I (340–400 nm) and UVA II (320–340 nm). Virtually no UVC reaches the Earth’s surface because it is absorbed by the ozone layer above the Earth.
The minimal amount of a particular wavelength of light capable of inducing erythema on an individual’s skin is called the minimal erythema dose (MED). Although the amount of UVA radiation is 100 times greater than UVB radiation during midday hours, UVB is up to 1000 times more erythemogenic than UVA, and so essentially all solar erythema is caused by UVB. The most biologically effective wavelength of radiation from the sun for sunburn is 308 nm. Although it does not play a significant role in solar erythema, UVA is of major importance in patients with drug-induced photosensitivity and also play a role in photoaging and cutaneous immunosuppression.
The amount of UV exposure increases at higher altitudes, is substantially larger in temperate climates in the summer months, and is greater in tropical regions. UVA may be reflected somewhat more than UVB from sand, snow, and ice. Whereas sand and snow reflect as much as 85% of the UVB, water allows 80% of the UV to penetrate up to 3 feet. Cloud cover, although blocking substantial amounts of visible light, is a poor UV absorber. During the middle 4–6 hours of the day, the intensity of UVB is 2–4 times greater than in the early morning and late afternoon.
Clinical Signs and Symptoms
Sunburn is the normal cutaneous reaction to sunlight in excess of an erythema dose. UVB erythema becomes evident at around 6 hours after exposure and peaks at 12–24 hours, but the onset is sooner and the severity greater with increased exposure. The erythema is followed by tenderness and in severe cases, blistering, which may become confluent ( Fig. 3.11 ). Discomfort may be severe; edema typically occurs in the extremities and face; chills, fever, nausea, tachycardia, and hypotension may be present. In severe cases, such symptoms may last for as long as a week. Desquamation is common about 1 week after sunburn, even in areas that have not blistered.
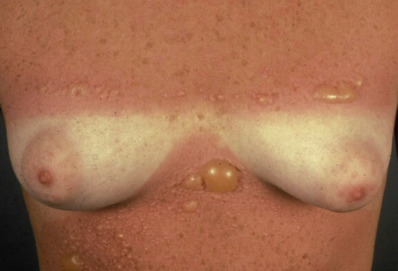
After UV exposure, skin pigment undergoes two changes: immediate pigment darkening (IPD, Meirowsky phenomenon) and delayed melanogenesis. IPD is maximal within hours after sun exposure and results from metabolic changes and redistribution of the melanin already in the skin. It occurs after exposure to long-wave UVB, UVA, and visible light. With large doses of UVA, the initial darkening is prolonged and may blend into the delayed melanogenesis. IPD is not photoprotective. Delayed tanning is induced by the same wavelengths of UVB that induce erythema, begins 2–3 days after exposure, and lasts 10–14 days. Delayed melanogenesis by UVB is mediated through the production of DNA damage and the formation of cyclobutane pyrimidine dimers (CPD). Therefore, although UVB-induced delayed tanning does provide some protection from further solar injury, it is at the expense of damage to the epidermis and dermis. Tanning is not recommended for sun protection. Commercial tanning bed–induced tanning, while increasing skin pigment, does not increase UVB MED and is therefore not protective for UVB damage. Such tanning devices have been shown to cause melanoma, and their use for tanning purposes should be banned. An individual’s inherent baseline pigmentation, ability to tan, and susceptibility to burns are described as the person’s “skin type.” Skin type is used to determine starting doses of phototherapy and sunscreen recommendations and reflects the risk of development of skin cancer and photoaging ( Table 3.1 ).
| Skin Type | Baseline Skin Color | Sunburn and Tanning History |
|---|---|---|
| I | White | Always burns, never tans |
| II | White | Always burns, tans minimally |
| III | White | Burns moderately, tans gradually |
| IV | Olive | Minimal burning, tans well |
| V | Brown | Rarely burns, tans darkly |
| VI | Dark brown | Never burns, tans darkly black |
Exposure to UVB and UVA causes an increase in the thickness of the epidermis, especially the stratum corneum. This increased epidermal thickness leads to increased tolerance to further solar radiation. Patients with vitiligo may increase their UV exposure without burning by this mechanism.
Treatment
Once redness and other symptoms are present, treatment of sunburn has limited efficacy. The damage is done, and the inflammatory cascades are triggered. Prostaglandins, especially of the E series, are important mediators. Aspirin (acetylsalicylic acid [ASA]) and nonsteroidal antiinflammatory drugs (NSAIDs), including indomethacin, have been studied, as well as topical and systemic steroids. Medium-potency (class II) topical steroids applied 6 hours after the exposure (when erythema first appears) provide a small reduction in signs and symptoms. Oral NSAIDs and systemic steroids have been tested primarily before or immediately after sun exposure, so there is insufficient evidence to recommend their routine use, except immediately after solar overexposure. Therefore treatment of sunburn should be supportive, with pain management (using acetaminophen, ASA, or NSAIDs), plus soothing topical emollients or corticosteroid lotions. In general, a sunburn victim experiences at least 1 or 2 days of discomfort and even pain before much relief occurs.
Prophylaxis
Sunburn is best prevented. Use of the UV index facilitates taking adequate precautions to prevent solar injury. Numerous educational programs have been developed to make the public aware of the hazards of sun exposure. Despite this, sunburn and excessive sun exposure continue to occur in the United States and Western Europe, especially in white persons under age 30, more than 50% of whom report at least one sunburn per year. Sun protection programs have the following four main messages:
- •
Avoid midday sun.
- •
Seek shade.
- •
Wear sun-protective clothing.
- •
Apply a sunscreen.
The period of highest UVB intensity, between 9 am and 3–4 pm , accounts for the vast majority of potentially hazardous UV exposure. This is the time when the angle of the sun is less than 45 degrees, or when a person’s shadow is shorter than his or her height. In temperate latitudes, it is almost impossible to burn if these hours of sun exposure are avoided. Trees and artificial shade provide substantial protection from UVB. Foliage in trees provides the equivalent of sun protection factor (SPF) 4–50, depending on the density of the greenery. Clothing can be rated by its ability to block UVB radiation. The scale of measure is the UV protection factor (UPF), analogous to SPF in sunscreens. Although it is an in vitro measurement, UPF correlates well with the actual protection the product provides in vivo. In general, denser weaves, washed older clothing, and loose-fitting clothes screen UVB more effectively. Wetting a fabric may substantially reduce its UPF. Laundering a fabric in a Tinosorb-containing material (SunGuard) will add substantially to the UPF of the fabric. Hats with at least a 4-inch brim all around are recommended.
A sunscreen’s efficacy in blocking the UVB (sunburn-inducing) radiation is expressed as an SPF. This is the ratio of the number of MEDs of radiation required to induce erythema through a film of sunscreen (2 mg/cm 2 ) compared with unprotected skin. Most persons apply sunscreens in too thin a film, so the actual “applied SPF” is about half that on the label. Sunscreen agents include UV-absorbing chemicals (chemical sunscreens) and UV-scattering or blocking agents (physical sunscreens). Available sunscreens, especially those of high SPFs (>30), usually contain both chemical sunscreens (e.g., p -aminobenzoic acid [PABA], PABA esters, cinnamates, salicylates, anthranilates, benzophenones, benzylidene camphors such as ecamsule [Mexoryl], dibenzoylmethanes [Parsol 1789, in some products present as multicompound technology Helioplex], and Tinosorb [S/M]) and physical agents (zinc oxide or titanium dioxide). Sunscreens are available in numerous formulations, including sprays, gels, emollient creams, and wax sticks. Sunscreens may be water resistant, with some maintaining their SPF after 40 minutes of water immersion and others maintaining their SPF after 80 minutes of water immersion.
For skin types I to III (see Table 3.1 ), daily application of a broad-spectrum sunscreen with an SPF of 30 in a facial moisturizer, foundation, or aftershave is recommended. For outdoor exposure, a sunscreen of SPF 30 or higher is recommended for regular use. In persons with severe photosensitivity and at times of high sun exposure, high-intensity sunscreens of SPF 30+ with inorganic blocking agents may be required. Application of the sunscreen at least 20 minutes before and 30 minutes after sun exposure has begun is recommended. This dual-application approach will reduce the amount of skin exposure by twofold to threefold over a single application. Sunscreen should be reapplied after swimming or vigorous activity or toweling. Sunscreen failure occurs mostly in men, from failure to apply it to all the sun-exposed skin or failure to reapply sunscreen after swimming. Sunscreens may be applied to babies (under 6 months) on limited areas. Vitamin D supplementation is recommended with the most stringent sun protection practices. The dose is 600 IU daily for those 70 and younger and 800 IU for older patients.
Photoaging and cutaneous immunosuppression are mediated by UVA as well as UVB. For this reason, sunscreens with improved UVA coverage have been developed. Those containing excellent protection for both UVB and UVA are identified on the label by the words “broad spectrum,” and these sunscreens should be sought by patients.
Aguilera J, et al: New advances in protection against solar ultraviolet radiation in textiles for summer clothing. Photochem Photobiol 2014; 90: 1199.
Almutawa F, Buabbas H: Photoprotection. Dermatol Clin 2014; 32: 439.
Cohen LE, Grant RT: Sun protection. Clin Plast Surg 2016; 43: 605.
Faurschaou A, et al: Topical corticosteroids in the treatment of acute sunburn. Arch Dermatol 2008; 144: 620.
Fisher DE, et al: Indoor tanning. N Engl J Med 2010; 363: 901.
Lim HW, et al: Adverse effects of ultraviolet radiation from the use of indoor tanning equipment. J Am Acad Dermatol 2011; 64: 893.
Mallett KA, et al: Rates of sunburn among dermatology patients. JAMA Dermatol 2015; 151: 231.
Polefka PG, et al: Effects of solar radiation on the skin. J Cosmet Dermatol 2012; 11: 134.
Thompson AE: Suntan and sunburn. JAMA 2015; 314: 638.
Ephelis (Freckle) and Lentigo
Freckles are small (<0.5 cm) brown macules that occur in profusion on the sun-exposed skin of the face, neck, shoulders, and backs of the hands. They become prominent during the summer when exposed to sunlight and subside, sometimes completely, during the winter when there is no exposure. Blonds and redheads with blue eyes and of Celtic origin (skin types I or II) are especially susceptible. Ephelides may be genetically determined and may recur in successive generations in similar locations and patterns. They usually appear at about age 5 years.
Ephelis must be differentiated from lentigo simplex. The lentigo is a benign, discrete hyperpigmented macule appearing at any age and on any part of the body, including the mucosa. The intensity of the color is not dependent on sun exposure. The solar lentigo appears at a later age, mostly in persons with long-term sun exposure. The backs of the hands and face (especially the forehead) are favored sites ( Fig. 3.12 ).
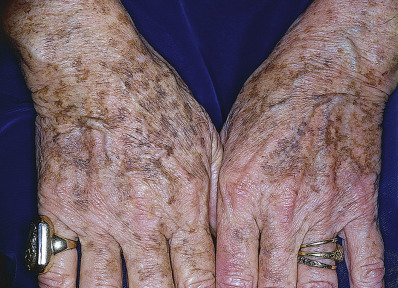
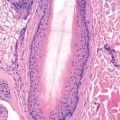
Histologically, the ephelis shows increased production of melanin pigment by a normal number of melanocytes. Otherwise, the epidermis is normal, whereas the lentigo has elongated rete ridges that appear to be club shaped.
Freckles and solar lentigines are best prevented by appropriate sun protection. Cryotherapy, topical retinoids, hydroquinone, intense pulse light, undecylenoyl phenylalanine, and lasers are effective in the treatment of solar lentigines.
Hafner C, et al: The absence of BRAF, FGFR3, and PIK3CA mutations differentiates lentigo simplex from melanocytic nevus and solar lentigo. J Invest Dermatol 2009; 129: 2730
Imhof L, et al: A prospective trial comparing Q-switched ruby laser and a triple combination skin-lightening cream in the treatment of solar lentigines. Dermatol Surg 2016; 42: 853.
Praetorius C, et al: Sun-induced freckling. Pigment Cell Melanoma Res 2014; 27: 339.
Photoaging (Dermatoheliosis)
The characteristic changes induced by chronic sun exposure are called photoaging or dermatoheliosis. An individual’s risk for developing these changes correlates with the person’s skin type (see Table 3.1 ). Risk for melanoma and nonmelanoma skin cancer is also related to skin type. The persons most susceptible to the deleterious effects of sunlight are those of skin type I: blue-eyed, fair-complexioned persons who do not tan. They are frequently of Irish or other Celtic or Anglo-Saxon descent. Individuals who develop photoaging have the genetic susceptibility and have had sufficient actinic damage to develop skin cancer, and they therefore require more frequent and careful cutaneous examinations.
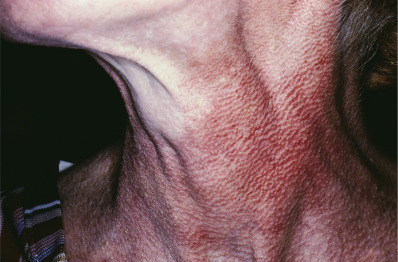
Chronic sun exposure and chronologic aging are additive. Cigarette smoking is also important in the development of wrinkles, resulting in the inability of observers to distinguish solar-induced from smoking-induced skin aging accurately. The areas primarily affected by photoaging are those regularly exposed to the sun: the V area of the neck and chest, back and sides of the neck, face, backs of the hands and extensor arms, and in women the skin between the knees and ankles. The skin becomes atrophic, scaly, wrinkled, inelastic, or leathery with a yellow hue (milian citrine skin). In some persons of Celtic ancestry, dermatoheliosis produces profound epidermal atrophy without wrinkling, resulting in an almost translucent appearance of the skin through which hyperplastic sebaceous glands and prominent telangiectasias are seen ( Fig. 3.13 ). These persons are at high risk for nonmelanoma skin cancer. Pigmentation is uneven, with a mixture of poorly demarcated, hyperpigmented and white atrophic macules observed. The photodamaged skin appears generally darker because of these irregularities of pigmentation; in addition, dermal hemosiderosis occurs from actinic purpura. Solar lentigines occur on the face and dorsa of the hands.
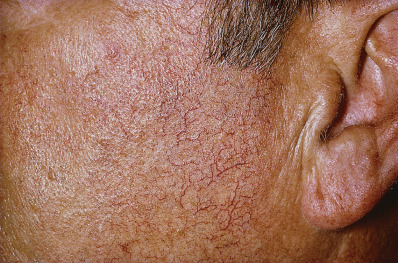
Many of the textural and tinctorial changes in sun-damaged skin are caused by alterations in the upper dermal elastic tissue and collagen. This process is called solar (actinic) elastosis, which imparts a yellow color to the skin. Many clinical variants of solar elastosis have been described, and an affected individual may simultaneously have many of these changes. Small yellowish papules and plaques may develop along the sides of the neck. They have been variably named “striated beaded lines” (the result of sebaceous hyperplasia) or “fibroelastolytic papulosis” of the neck, which is caused by solar elastosis. At times, usually on the face or chest, this elastosis may form a macroscopic, translucent papule with a pearly color that may closely resemble a basal cell carcinoma (actinic elastotic plaque). Similar plaques may occur on the helix or antihelix of the ear (elastotic nodules of the ear). Poikiloderma of Civatte refers to reticulate hyperpigmentation with telangiectasia, and slight atrophy of the sides of the neck, lower anterior neck, and V of the chest. The submental area, shaded by the chin, is spared ( Fig. 3.14 ). Poikiloderma of Civatte frequently presents in fair-skinned men and women in their mid to late thirties or early forties. Cutis rhomboidalis nuchae (sailor’s or farmer’s neck) is characteristic of long-term, chronic sun exposure ( Fig. 3.15 ). The skin on the back of the neck becomes thickened, tough, and leathery, and the normal skin markings are exaggerated. Nodular elastoidosis with cysts and comedones occurs on the inferior periorbital and malar skin (Favre-Racouchot syndrome) ( Fig. 3.16 ) on the forearms (actinic comedonal plaque) or helix of the ear. These lesions appear as thickened yellow plaques studded with comedones and keratinous cysts. The ears may exhibit one or more firm nodules on the helix, known as weathering nodules. Biopsy reveals fibrosis and cartilage metaplasia.