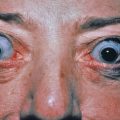
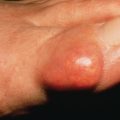
Cutaneous laser surgery is a continually evolving area of dermatology. Development of new lasers, as well as improvements in existing lasers, continues to advance the field. As a result of this progress, laser surgery has become an extremely effective therapeutic modality for a multitude of dermatologic conditions.
Laser Principles
Laser is an acronym for light amplification by stimulated emission of radiation. The first laser was a ruby laser operated in 1960 by Theodore Maiman. Medical applications were quickly recognized, and Leon Goldman pioneered their dermatologic use.
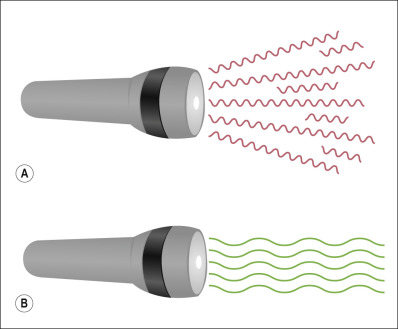
Although technology has advanced through the years, several distinctive characteristics have remained in all lasers. Compared with other light sources, laser light is defined as monochromatic (i.e., a single wavelength), collimated (i.e., nondivergent), coherent (i.e., in phase, with peaks and troughs of the light all aligned), and having high intensity that can travel over long distances ( Fig. 38.1 ). Laser energy is measured in joules (J). Fluence is defined as the amount of energy delivered per unit area (J/cm 2 ). Power is the rate at which energy is delivered and is measured in watts (1 watt is defined as 1 J/second).
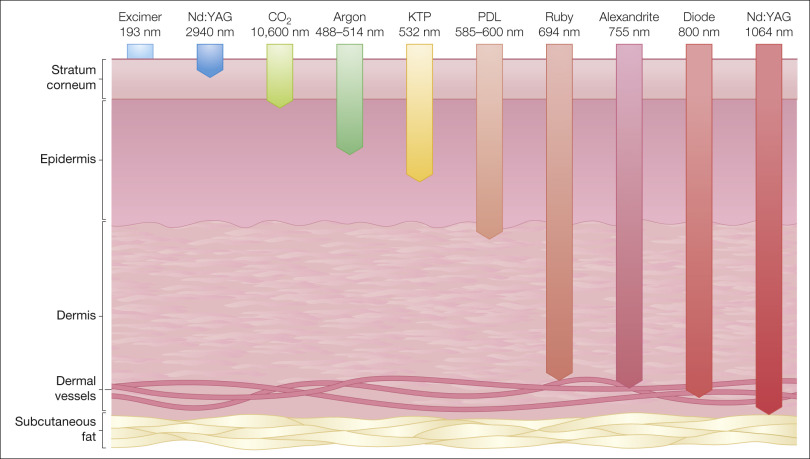
The wavelength is determined by the active medium of each particular laser. Active medium can consist of a gas (e.g., argon, CO 2 ), liquid (e.g., dye), or solid (e.g., ruby, yttrium-aluminum-garnet crystal) ( Table 38.1 ). The choice of wavelength is determined by the target tissue and depth of penetration required ( Fig. 38.2 ).
| Laser/System | Wavelength (nm) | Color | Applications |
|---|---|---|---|
| Argon | 488–514 | Blue-green | Vascular lesions |
| Intense pulsed light (IPL) | 515–1200 | Green-red and infrared | Vascular lesions, pigmented lesions, epilation, photodamage |
| Potassium titanyl phosphate (KTP) | 532 | Green | Vascular lesions, pigmented lesions |
| QS Nd:YAG (frequency doubled) | 532 | Green | Vascular lesions, pigmented lesions; tattoo—red |
| Copper vapor | 578/511 | Yellow-green | Vascular lesions, pigmented lesions |
| Flashlamp-pumped pulsed dye (PDL) | 585–600 | Yellow | Vascular lesions |
| QS ruby | 694 | Red | Deep and superficial pigmented lesions; tattoo—black, blue, green |
| Long-pulsed ruby | 694 | Red | Epilation |
| QS alexandrite | 755 | Infrared | Tattoo—blue, black, green |
| Long-pulsed alexandrite | 755 | Infrared | Epilation |
| Diode | 810 | Infrared | Epilation |
| QS Nd:YAG | 1064 | Infrared | Deep and superficial dermal pigment; tattoo—black, blue |
| Long-pulsed Nd:YAG | 1064 | Infrared | Epilation, vascular lesion |
| Er:YAG | 2940 | Infrared | Superficial skin resurfacing; destruction of superficial growths |
| Carbon dioxide | 10 ,600 | Infrared | Skin resurfacing; destruction of warts, keloids, superficial cancers, and benign growths |
Continuous-wave lasers emit a beam of light whose output power is constant over time, resulting in a long, continuous exposure. Quasi–continuous-wave lasers shutter the continuous beam into short segments, producing interrupted emissions of constant laser emission. Pulsed lasers produce short, high-energy pulses of light. Q-switched (quality-switched) lasers are able to generate extremely high-energy pulses over very short pulse durations (nanoseconds or picoseconds) and are used primarily for treating pigmented lesions.
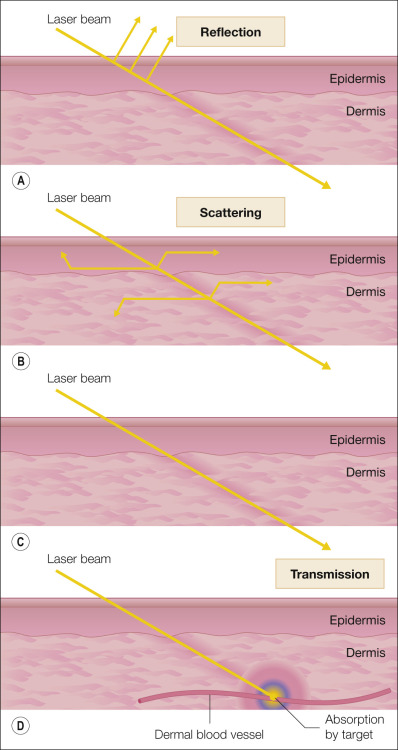
Light can interact with incident targets in one of several ways: reflected, transmitted, scattered, or absorbed ( Fig. 38.3 ). Approximately 5% of laser light is reflected from the epidermis and not absorbed. Transmitted light passes unaltered through the tissue. Light is scattered by the various skin structures, molecules, and cells, thus limiting its depth of penetration and effect on tissue. When reflected, transmitted, or scattered, the light has no effect on the target tissue. When absorbed, however, the light energy is transformed into heat. In most cases of laser therapy, it is the heat generated by absorption that produces the desired therapeutic effect.
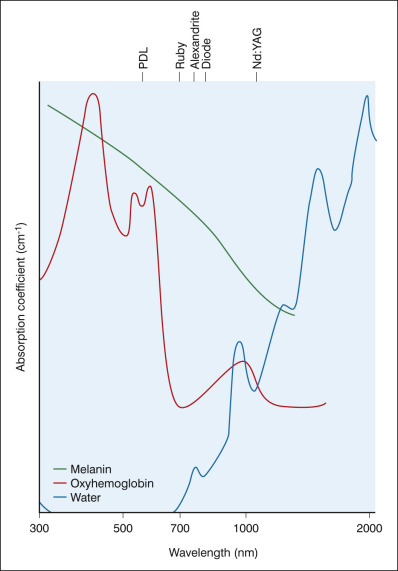
The concept of selective photothermolysis, originally promoted by Parish and Anderson, is the basis for all laser-tissue interactions. Lasers in cutaneous surgery are selected by matching their particular wavelength with the absorption spectrum of a desired target. The target structures that absorb laser light are defined as chromophores, with the most common in the skin being water, hemoglobin, and melanin ( Fig. 38.4 ). The goal is to deliver a wavelength that is specifically absorbed by the chromophore, inducing heat buildup and the resultant destruction of that target. In an ideal situation, this wavelength would have little or no absorption by surrounding structures. By controlling the laser’s exposure times and energy delivered, the amount of heat buildup can be confined to the desired target with minimal or no collateral damage to surrounding structures from heat dissipation. A target’s thermal relaxation time (TRT) is defined as the time required for the heated target tissue to dissipate half the absorbed heat from the laser. TRT is related to the size and shape of the target structure. Selective photothermolysis is achieved by ensuring that the laser pulse duration is equal to or less than the TRT of the target tissue. Thus larger structures (e.g., hair follicles) have a longer TRT and are best treated with longer pulse widths. Smaller structures (e.g., melanosomes) have a shorter TRT and can be treated with much shorter pulse durations ( Table 38.2 ).
| Chromophore | Diameter | TRT | Typical Laser Pulse Duration |
|---|---|---|---|
| Tattoo ink particle | 0.1 µm | 10 ns | 10 ns |
| Melanosome | 0.5 µm | 250 ns | 10–100 ns |
| Port wine stain vessels | 30–100 µm | 1–10 ms | 0.4–20 ms |
| Terminal hair follicle | 300 µm | 100 ms | 3–100 ms |
| Leg vein | 1 mm | 1 second | 0.1 second |
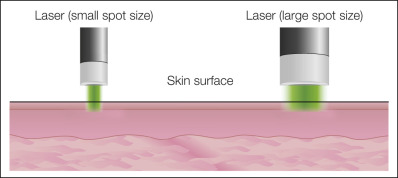
The beam diameter of the laser, or spot size, is a factor in depth of laser penetration. Small spot sizes produce significantly more scatter of the laser outside the effective beam, thus resulting in smaller effective treatment areas. In contrast, larger spot sizes produce more photons that remain within the beam diameter, resulting in higher fluences at a given depth. Therefore with any given wavelength, a larger beam diameter results in a deeper level of penetration ( Fig. 38.5 ).
Epidermal melanin and heat transfer from dermal structures can result in inadvertent epidermal heating and injury. By selectively cooling the overlying skin, while still maintaining sufficient dermal heat to damage the target, the laser surgeon can reduce the chances of epidermal injury. Precooling, parallel cooling, and postcooling have all been used to protect the skin. Dynamic cooling devices use a cryogen spray to cool the skin before and after laser exposure. Contact cooling with a chilled sapphire tip can be used throughout the treatment and is especially useful for parallel cooling. Contact cooling can also be achieved with a chilled metal plate to achieve precooling and postcooling. However, when using this kind of device, the operator must be especially careful to ensure adequate cooling is achieved, as it requires coordinated movement of the handpiece before and after firing the laser. Forced cooled air provides less effective cooling than other methods but can be useful in reducing pain associated with laser treatment. Direct application of ice can also be used for postcooling.
The laser is a technologically advanced instrument that has been used effectively and safely for a wide variety of dermatologic conditions. However, as with any surgery or therapeutic intervention, side effects and complications can occur. Short-term side effects include purpura, edema, and crusting. More concerning, long-term adverse events include scarring (both atrophic and hypertrophic), dyspigmentation, infection, and persistent erythema. Although not a complication, lasers sometimes show a lack of efficacy even when used properly in appropriate clinical settings. Detailed informed consent is critical before performing any laser treatment. Appropriate instruction and supervision in the use of lasers must be obtained by dermatologic surgeons to ensure optimum safety and surgical outcome. Adverse outcomes in laser-treated patients have a significant medicolegal impact, with nonphysician operators accounting for a significant proportion of these cases. Caution is required for any physician who is supervising these providers when performing laser treatment.
Anderson RR, Parrish JA: Selective photothermolysis. Science 1983; 220: 524.
Carroll L, Humphreys TR: Laser-tissue interactions. Clin Dermatol 2006; 24: 2.
Das A, et al: Cooling devices in laser therapy. J Cutan Aesthet Surg 2016; 9: 215.
Dawson E, et al: Adverse events associated with nonablative cutaneous laser, radiofrequency, and light-based devices. Semin Cutan Med Surg 2007; 26: 15.
Jalian HR, et al: Common causes of injury and legal action in laser surgery. JAMA Dermatol 2013; 149: 188.
Tanzi EL, et al: Lasers in dermatology. J Am Acad Dermatol 2003; 49: 1.
Vanaman M, et al: Complications in the cosmetic dermatology patient. Dermatol Surg 2016; 42: 12.
Laser Treatment of Vascular Lesions
A number of congenital and acquired vascular lesions can be effectively treated with laser. Given the variety of choices available, the laser surgeon must have a complete understanding of the inherent differences in wavelengths, pulse durations, and the vessel size of the particular lesion being targeted. Over the years, lasers have become more selective and the treatment of vascular lesions more effective.
Pulsed Dye Laser
The pulsed dye laser (PDL) was the first laser developed specifically to take advantage of selective photothermolysis. The laser medium is a rhodamine dye, which initially was developed to deliver a wavelength of 577 nm, coinciding with a specific hemoglobin absorption peak. Older lasers used a wavelength of 585 nm, but for various technical and clinical reasons, the wavelength has evolved in the current generation of PDL to be 595 nm. Initial pulse durations were about 500 microsecond (µs)/pulse. This was based on calculations that the target, hemoglobin, had a TRT of 1 ms or less. These parameters resulted in immediate postoperative purpura lasting up to 2 weeks.
Newer configurations of the laser allow for pulse durations from 0.45 to 40 ms, based on newer understandings of TRTs in the context of the size of the target (e.g., capillaries vs. larger vessels) and clinical effects (purpuric vs. nonpurpuric treatment). By using longer pulse durations, gentler and more uniform heating results in reduced or absent posttreatment purpura (more acceptable to patients) than the earlier PDL configurations, while still maintaining clinical efficacy.
The PDL is an extremely useful instrument for the treatment of vascular lesions. These lasers have traditionally been used for port wine stains, telangiectasias, erythematotelangiectatic rosacea, and hemangiomas. The risk of scarring and pigment change is very low with this technology. PDL is used in a wide range of patients, including newborns. The newer, long-pulsed and longer-wavelength lasers allow for treatment of larger and deeper vessels. By combining these treatments with surface-cooling devices, the epidermis can be protected, which allows for the delivery of greater energy in a safer and less painful manner.
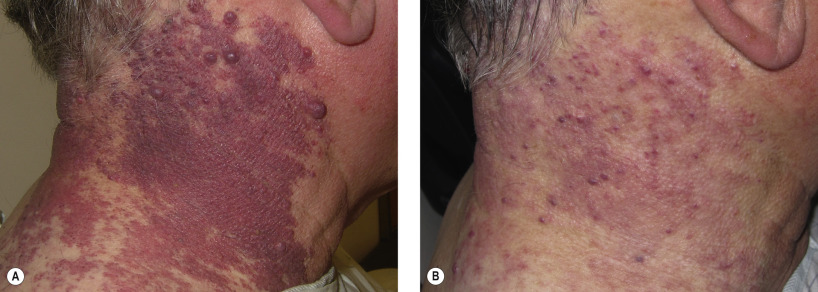
The PDL is the treatment of choice for port wine stains. A series of treatments every 4–6 weeks is required for maximum benefit, with gradual improvement after each session. Although most patients will show improvement, total clearance of lesions is extremely rare ( Fig. 38.6 ). Rate of improvement is related to anatomic location, with lesions on the extremity having a less robust response than facial lesions. Size also plays a role in the response rate of port wine stains, with smaller lesions having a greater rate of improvement than larger lesions. Treatments are typically performed with short pulse durations (i.e., 0.45 or 1.5 ms), with resulting purpura lasting for 10–14 days. When the treatment is performed with proper cooling and appropriate technique, the risk of atrophic scarring and pigmentary alterations is extremely low. Redarkening of treated port wine stains after treatment with PDL can occur over time and may necessitate repeat treatments years later.
Ulcerated hemangiomas have been successfully treated by PDL. In addition, after spontaneous resolution of infantile hemangiomas, PDL can be used for any persistent telangiectasias. PDL has a limited depth of penetration, however, and thus is not effective in the treatment of deeper components of hemangiomas, which are likely to continue to proliferate despite laser therapy. The use of PDL for superficial hemangiomas in the proliferative phase remains controversial. Some studies have demonstrated that early treatment with PDL results in improved clearing. However, other authors have advocated that the natural course of hemangiomas is of regression, and that potential risk of ulceration and atrophy from PDL treatment is not warranted for uncomplicated lesions.
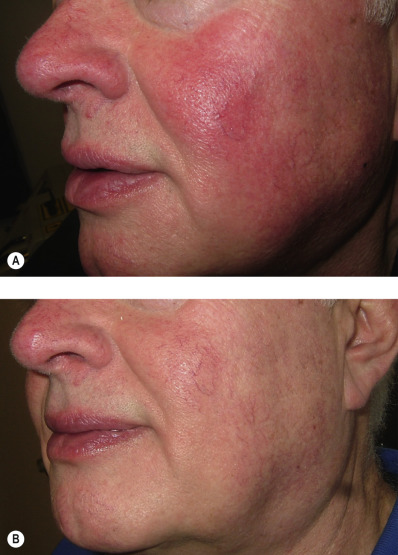
Erythematotelangiectatic rosacea is a common condition characterized by persistent facial erythema, telangiectasias, and flushing. PDL has been shown to be an effective and safe treatment option ( Fig. 38.7 ). The long-pulsed PDL has the advantage of purpura-free treatment, which is better tolerated by patients desiring cosmetic improvement.