8 Mastopexy Techniques—Basic Principles
Summary
Numerous techniques have been described to perform a mastopexy. This chapter reviews key concepts in understanding the footprint and how to get good, consistent, predictable results. Assessment of ptosis is re-evaluated to make surgical planning easier. The concept of parenchymal rearrangement is emphasized versus the failure of the skin as a brassiere. Different methods are reviewed, and emphasis is placed on the inferior flap of Ribeiro as being the most effective.
8.1 Introduction
The most common complication after mastopexy is recurrent ptosis. This problem results from a lack of understanding of the principles of aesthetic breast surgery. Most patients who are candidates for mastopexy have already proven that their skin has functioned poorly as a brassiere. Trying to tighten up the skin envelope and then expecting the skin to hold the shape against gravity is doomed to failure.
The key to achieving good consistent results in mastopexy surgery is first to understand the role of the breast footprint. The surgeon then needs to understand the difference between nipple ptosis and glandular ptosis and then to plan accordingly. Correcting nipple ptosis is the easy part. Correcting glandular ptosis entails an understanding of what true ptosis is and how important parenchymal reshaping is to the final outcome.
We have been taught over the years that the inframammary fold (IMF) is the best landmark for determining ptosis. 1 Unfortunately, this classification is misleading because it relates only to nipple ptosis and does not take into account glandular ptosis. The upper breast border is a better landmark than the IMF for planning a mastopexy.
8.2 Key Concepts
8.2.1 Breast Footprint
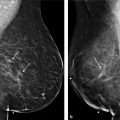
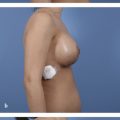
The actual attachment of the breast to the chest wall (footprint or base 2 , 3 ) varies significantly from patient to patient, and the breast borders can be only minimally changed with surgery. Some patients are “high-breasted” and some patients are “low-breasted.” It is important to understand that the breast borders can be altered only by adding or removing volume. The upper breast border can be elevated only with an implant (or fat injections), and the lower breast border (IMF) can be elevated when weight is removed, but it descends when weight is added. The medial and lateral breast borders are adjusted by adding volume (implant) or removing volume (liposuction). It is less about the skin than it is about the volume and weight (Fig. 8‑1, Fig. 8‑2). 4 , 5 , 6 , 7 , 8
8.2.2 Nipple Ptosis
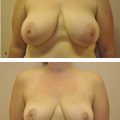
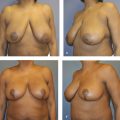
The nipple needs to be “centralized” on the breast mound. The surgeon needs to understand not only the footprint but what can and cannot be achieved with manipulating the breast mound in order to determine the ideal nipple position. On an average “C-cup” breast on an average woman, the ideal nipple position is about 8–10 cm below the upper breast border and about 8–10 cm from the chest midline (drawn as a straight line, not curved around the breast). 9 Although some surgeons state that breasts look best with the nipple at 55% up from the bottom of the breast just above the horizontal meridian, 10 this could lead to patient dissatisfaction. Over time, breasts tend to bottom out, and high nipples are very difficult for patients to hide in clothing and bathing suits without suffering “nipple slip.” The high nipple might look good in magazines with the back arched and the arms elevated to reduce glandular ptosis, but the high nipple can be a problem in clothing (Fig. 8‑3).
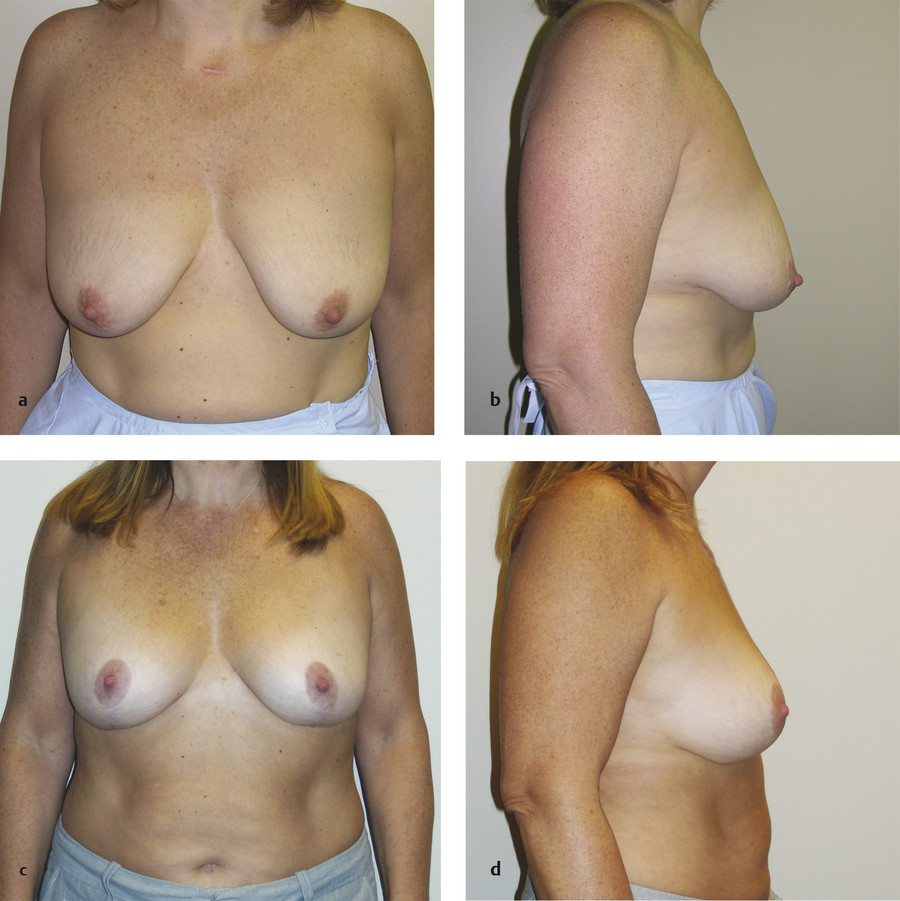
8.2.3 Glandular Ptosis
The surgeon needs to determine how much of the gland is sagging, or ptotic, and correct it. Ptotic gland tissue can be either removed (breast reduction) or moved (mastopexy). Although nipple ptosis can be easily corrected by repositioning, the breast mound needs to be corrected with parenchymal reshaping. Adjusting the skin brassiere will not correct glandular ptosis. The location of the IMF is less important than the actual amount of ptotic gland (Fig. 8‑4).
It is clear from the above that the Regnault 1 classification of breast ptosis (nipple position in relation to the IMF) can be misleading. What is important is an assessment of the breast mound—both the amount of glandular ptosis and the degree of nipple ptosis. The position of the IMF can be misleading in planning. It is important, however, for the surgeon to understand that the upper portion of the footprint will not change. The upper breast border is a better landmark for decision making (Spear S; personal communication).
8.2.4 Skin Brassiere versus Parenchymal Reshaping
Gravity wins. Skin is not a particularly good brassiere, especially when it has already shown that it is not good at holding the breast up, as occurs with most patients presenting for a mastopexy (Fig. 8‑5).
8.2.5 The Wise Pattern
The Wise pattern (not just the keyhole opening) is important for the surgeon to use as a template for the parenchyma (and not the skin)—for what should be left behind. Dr Robert Wise developed the pattern from a deconstructed brassiere. 11 Note that when the pattern is closed, it results in a nice coned breast shape. He used it for a skin pattern, but it is better used for the parenchymal pattern (Fig. 8‑6a,b).
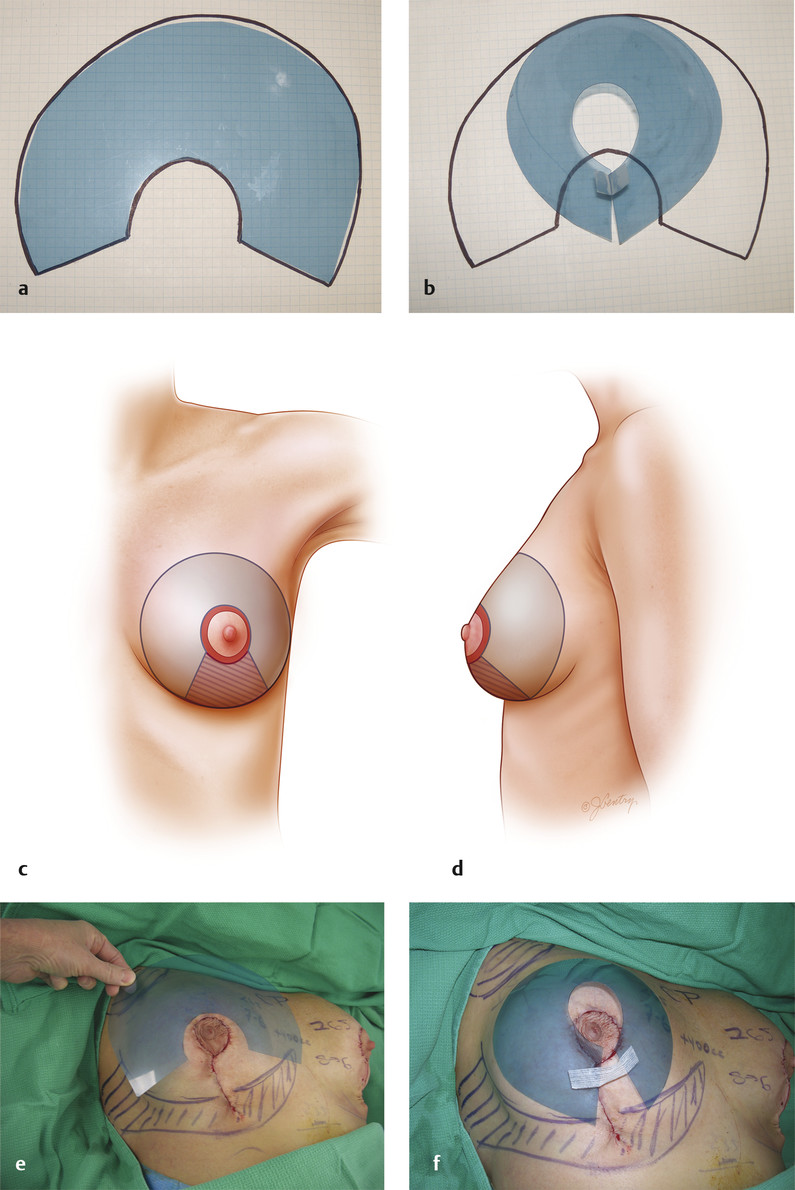
All tissue beyond the Wise pattern is removed in a breast reduction. 12 A vertical wedge of breast tissue and skin is removed inferiorly, and then any excess tissue beyond the limits of the Wise pattern is removed by direct excision, followed by tailoring out by peripheral liposuction. The pillars are brought together (without tension), giving good projection to the remaining breast. Note that lower pole tissue is recruited by this maneuver, while the inframammary fold rises. In a mastopexy, this inferior tissue is “moved” rather than “removed” (Fig. 8‑6c–f).
We have come to learn as plastic surgeons that we are much better at pulling excess tissue downward (abdominoplasty) than we are at pulling excess upward (facelifting). The key to successful breast surgery is to realize that we cannot “lift” the breast on the chest wall, and our most long-lasting results occur when we “remove” or “move” the heavy inferior pole and cone the remaining upper pole. Skin can act as a good brassiere when it is young and retains good elasticity, but we are often presented with patients with poor skin quality. We are well aware that our best clothing is made with good-quality fabric, but often in surgery we are forced to compromise with poor-quality material (skin). We must instead work against gravity, which means that we should address the lower pole tissue and not try to raise or lift or push tissue upward.
8.3 Anatomy
The breast is a subcutaneous fourth-intercostal-space structure that is attached to the skin at the level of the nipple. Posteriorly the breast has only loose attachments to the pectoralis fascia (which is why we used to sweep a subglandular pocket easily with our fingers for insertion of a breast implant).
The breast is only very loosely attached to the chest wall; it is instead held in place by skin–fascial attachments at the IMF and over the sternum (much like the gluteal fold and the sacrum for the buttocks; Fig. 8‑7). When a woman lies on her side, the upper breast folds over the sternum and the lower breast slides out laterally. When a woman stands on her head, the breast slides toward her chin. There are no significant lateral or superior skin–fascial attachments. The zones of adherence are medial and inferior, and they are not attachments from the breast but separate skin–fascial attachments. 9 , 12
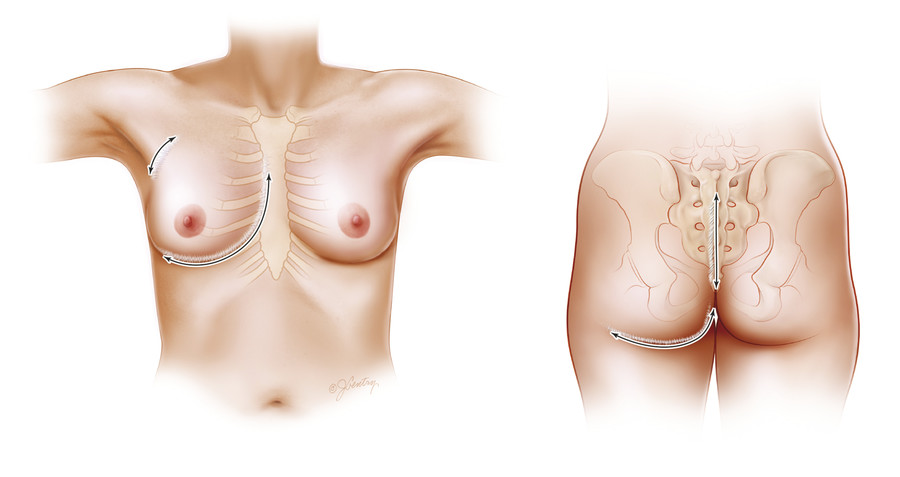
Attempts to suture the breast tissue to the pectoralis fascia are unlikely to succeed. Any actual adherence to the fascia results in scar contracture and retraction of the breast tissue with muscle movement. McKissock stated that the concept of suturing up breast tissue to the chest wall is so seductive that it is doomed to be tried (and fail) repeatedly. 13 On the other hand, removal of weight inferiorly will allow the IMF to rise with aggressive resection above the fold with a breast reduction or re-reduction. 14
The main blood supply consists of an artery and vein from the fourth intercostal space (from the internal mammary system) that enter the posterior surface of the breast just above the fifth rib just medial to the breast meridian. The rest of the blood supply is in the subcutaneous tissue superficial to the breast parenchyma, and it is pushed outward as the breast develops. The veins travel separately and drain mainly superomedially. The lateral aspect of the breast is supplied by the superficial branch of the lateral thoracic system, but the major blood supply is from the internal mammary vessels (Fig. 8‑8). 15 , 16
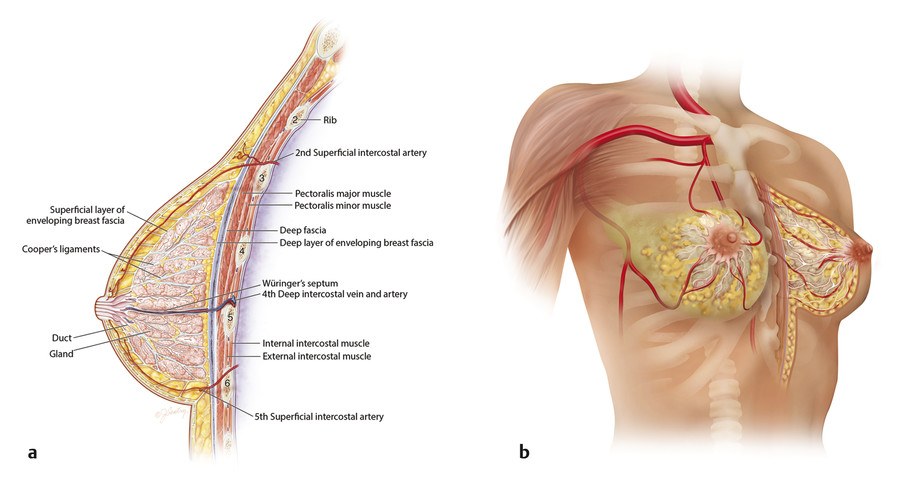
Innervation to the nipple is not just from the lateral fourth intercostal nerve (both deep and superficial) but also from the medial intercostal nerves as well. 17 In analyzing patient-reported sensation after vertical breast reduction, it was clear that the sensation from a medially based pedicle was about equal to that from an inferior pedicle (85% return of normal to near-normal sensation) but superior to both a lateral pedicle (76%) and a superior pedicle (67%). 8
Breast reduction and mastopexy cut through the ducts, but many of them reconnect. Cruz-Korchin has carefully studied breastfeeding after a medial-pedicle vertical breast reduction and found that the results were the same as in patients with large breasts and no surgery: about 60% were able to breastfeed, and 25% of those patients needed to supplement with formula. 18
8.4 Mastopexy Design
Knowledge of the anatomy will allow us to design methods to “move” that ptotic gland. Usually, the nipple needs to be moved, and knowledge of the various blood supplies to the pedicle is important. Most mastopexies, as described in this chapter, involve a superior or superomedial pedicle to move the nipple and an inferior flap to move or rearrange the ptotic gland.
There are various designs available to move the redundant gland, but the most effective is the inferior flap of Ribeiro described in Section 8.4.4. 4 , 5 A medial pedicle extension flap can be effective, but it does not allow much movement of the inferior parenchyma. A superior pedicle extension flap is turned up under the superior pedicle, but the breast can be difficult to close, and there is very little upward advancement of the parenchyma. None of these methods work as well as the inferior flap. 19 , 20
8.4.1 Medial Pedicle Extension Flap
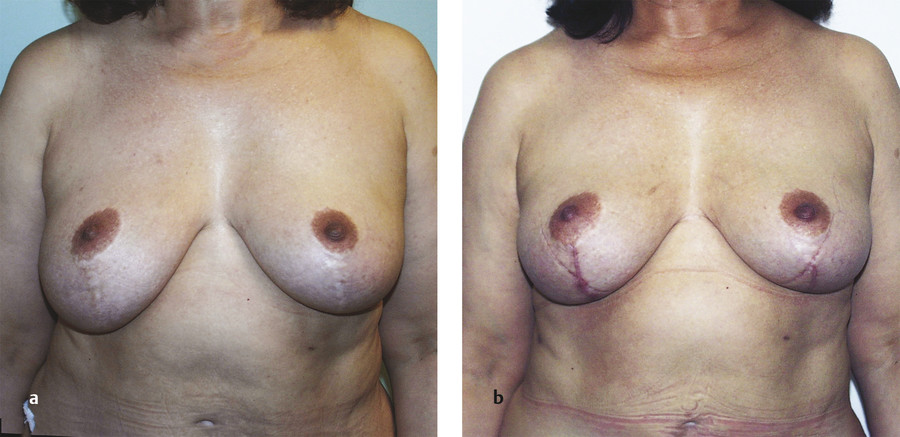
The design and execution of a medial pedicle extension flap are shown in Fig. 8‑9. Note that it is somewhat difficult to inset, thereby achieving only minimal glandular ptosis correction. For this patient, the result shows that the extension flaps did not make much, if any, difference.
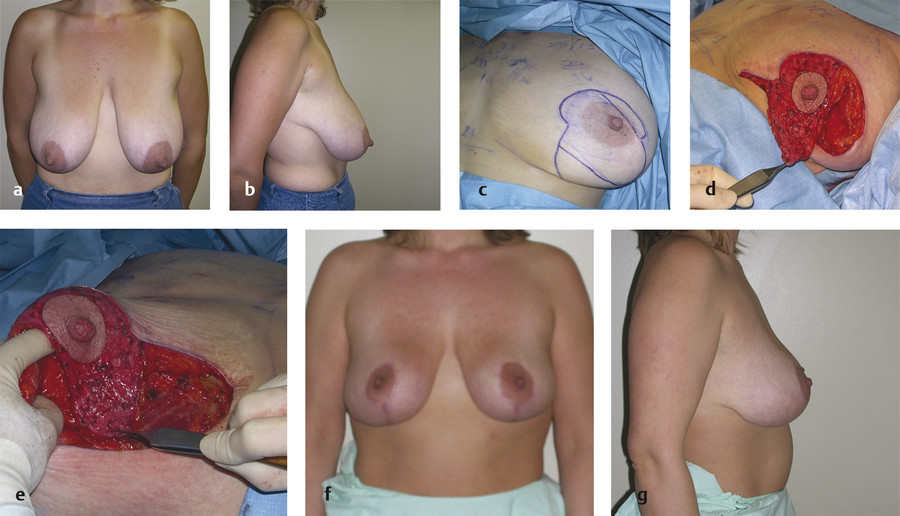
8.4.2 Superior Pedicle Extension Flap
The superior pedicle has an excellent blood supply, and the extension can be created from the inferior wedge that would be removed in a breast reduction. It can then be turned up under the areola to give the breast more fullness. Unfortunately it is difficult to inset without pulling the areola under with it, as shown in Fig. 8‑10. There is also tension on the flap, and it can give way. The patient shown felt both breasts “drop” at 3 months postoperatively.
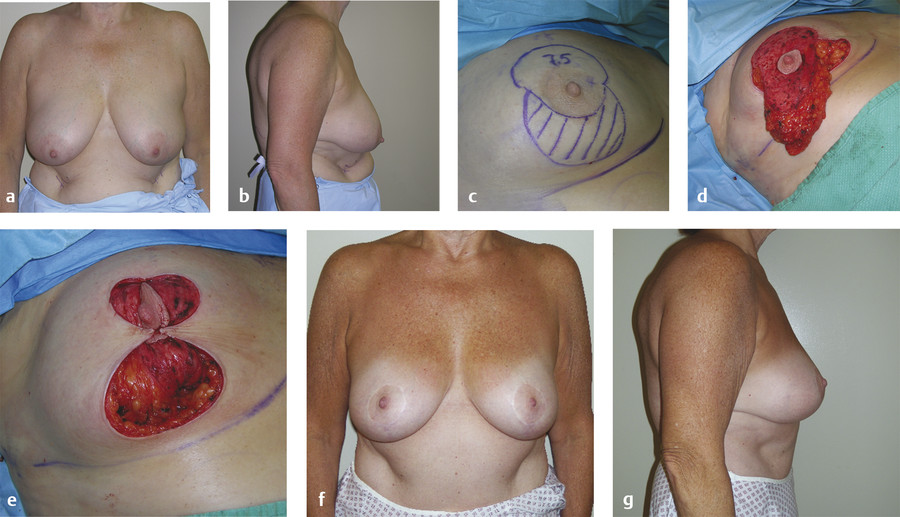
8.4.3 Other Rearrangement Flaps
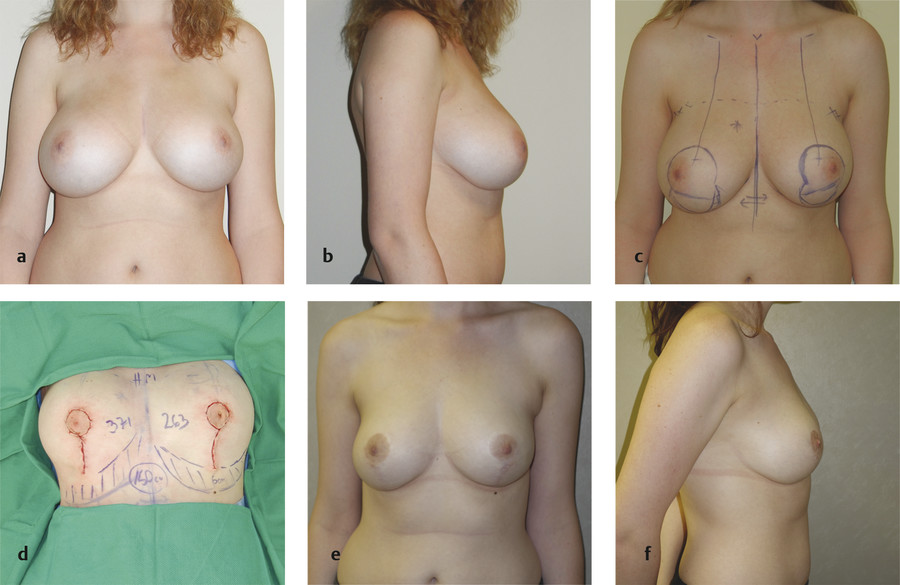
After realizing that the skin brassiere (including dermal flaps) was not effective at correcting glandular ptosis, the author tried multiple different methods of rearranging the breast parenchyma before finding that the inferior flap, discussed in the next section, was the most reliable. The patient in Fig. 8‑11 underwent a lateral pedicle along with two medial flaps (one above the pedicle into the upper pole and one below the pedicle to the midpoint of the breast) to rearrange the breast tissue.
8.4.4 Inferior Chest Wall–Based Flap (Ribeiro)
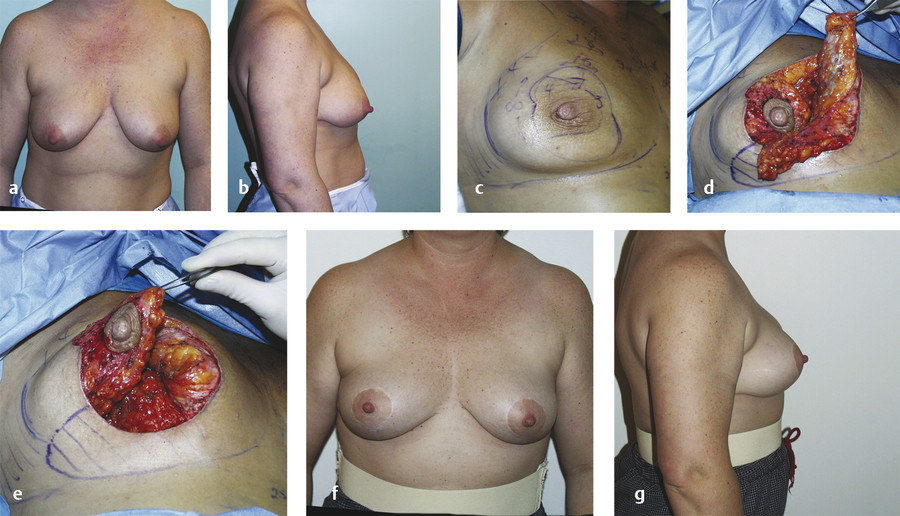
The inferior flap, as described by Liacyr Ribeiro, 5 has proven to be the most effective method of rearranging breast tissue for a mastopexy. The flap can be mobilized better than the other flaps described. This is the tissue that would be “removed” in a breast reduction and can be “moved” in a mastopexy. The flap can be better mobilized than any of the other flaps described in the preceding sections, and the breast and the flap move together. The flap does not heal to pectoralis fascia; rather, the anterior surface of the flap heals to the posterior surface of the pedicle. Later, if the patient decides to have an implant, there is still a good plane between the pectoralis fascia and the inferior flap. Unfortunately Ribeiro’s article was entitled “inferior pedicle,” so it was missed in the English literature, but in fact he used a superior pedicle with an inferior flap.
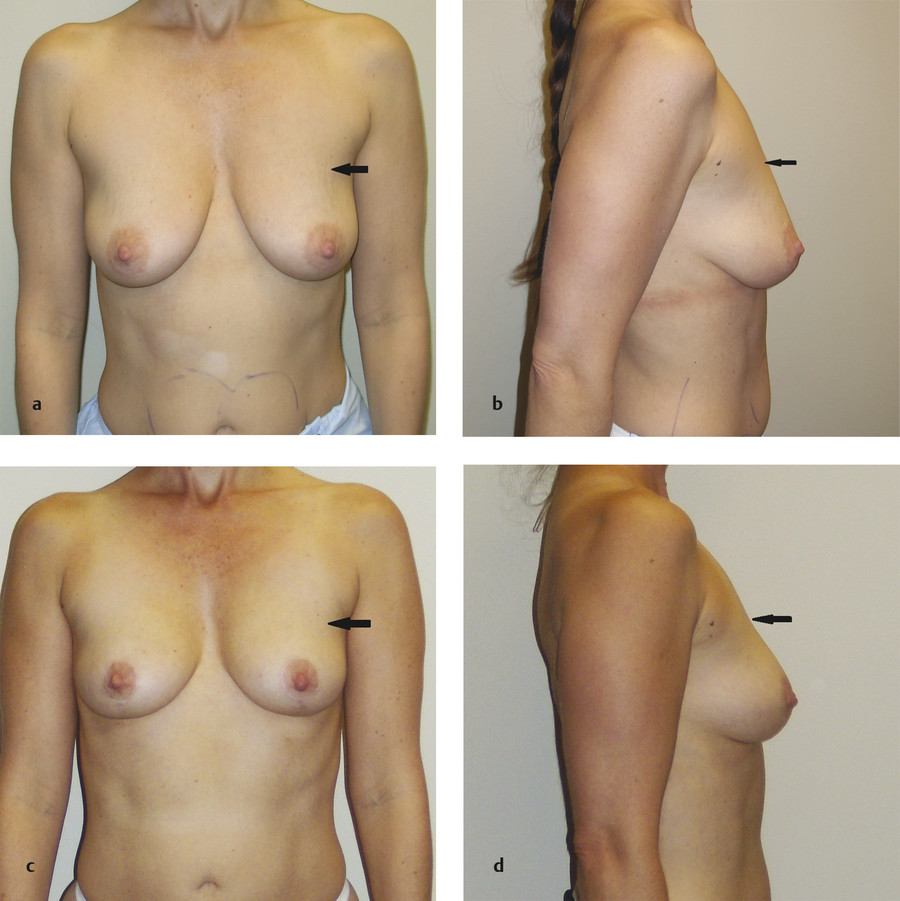
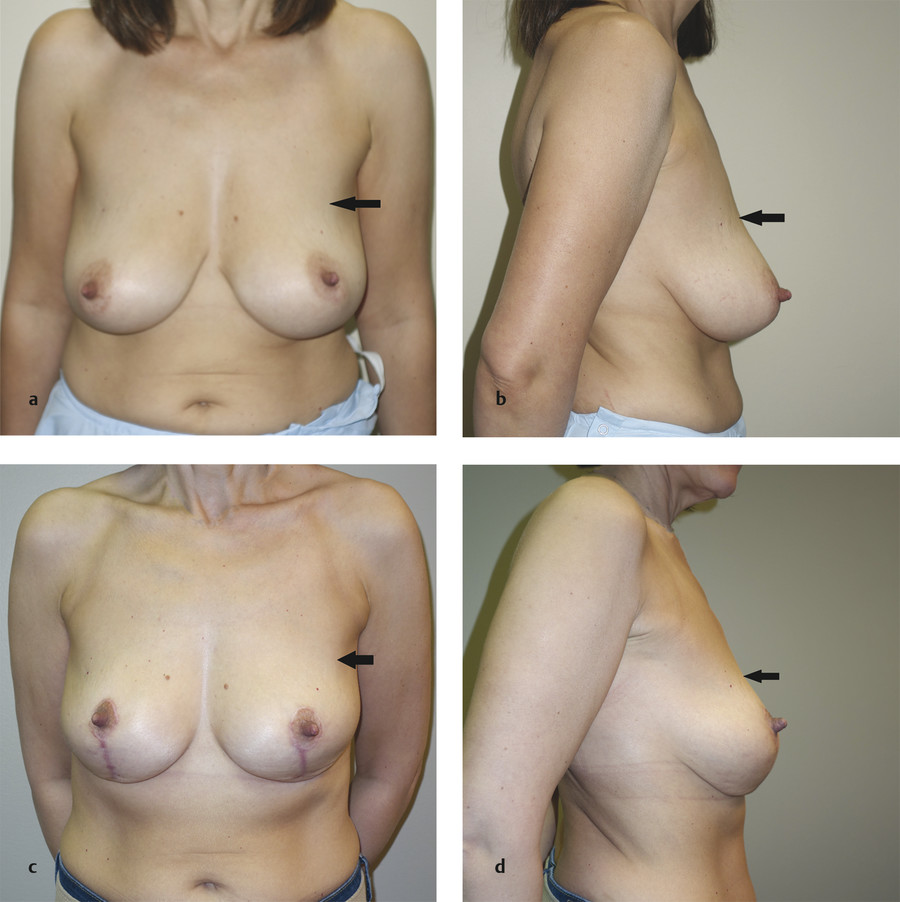
This is the type of flap used in the patients shown in Fig. 8‑1 and Fig. 8‑3; Fig. 8‑12 shows the interoperative photos from the latter. Both patients did have an inferior flap held up with a pectoralis sling, as described by Daniel and Graf, 6 , 7 but the pectoralis strip is not necessary. The author no longer uses the sling because sometimes the breast tissue descends around the flap, especially in a massive-weight-loss patient, leaving an unsightly bump. The original description provided by Ribeiro is the method that gives the author the best result. 4 , 5 It is best if both the breast and the flap settle together.
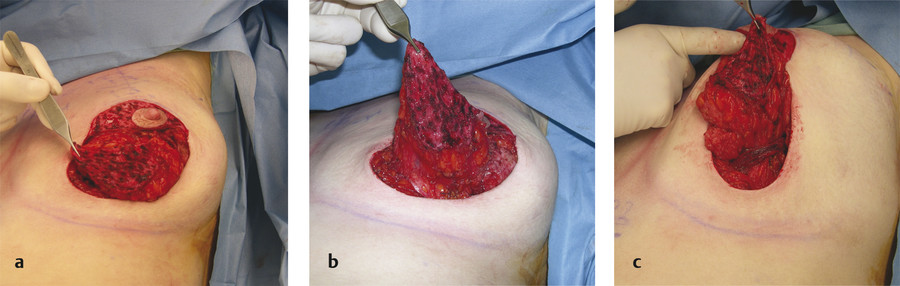
8.5 Operative Technique
There have been numerous descriptions of inverted T and vertical mastopexy techniques, and all have their merits. 21 , 22 , 23 , 24 , 25 , 26 , 27 , 28 , 29 , 30 , 31 , 32 , 33 , 34 , 35 , 36 , 37 , 38 The best mastopexy for a surgeon to perform is the mastopexy that individual surgeon performs the best. All of the long-lasting results involve rearrangement of the breast parenchyma. The following approach describes the technique that has worked the best in the author’s hands. 5 The author believes that it is important to move the excess breast tissue where it is in excess (inferior and lateral). It is important in a breast reduction to “remove” the glandular ptosis, and in a mastopexy it is important to “move” the glandular ptosis. 8
8.5.1 Markings
Upper Breast Border
The upper breast border is a better landmark for determining new nipple position than the IMF, as Scott Spear also maintained (Spear S, personal communication). The upper breast border will not change after surgery from its preoperative position with either a breast reduction or a mastopexy. The IMF, on the other hand, is quite variable from patient to patient (Fig. 8‑1). Some patients have a long vertical breast footprint, and other patients have a very narrow vertical footprint. Although the upper breast border remains the same after a breast reduction or a mastopexy, the IMF can be adjusted.
The upper breast border (small vertical arrows in Fig. 8‑13a) is the junction between the chest wall and the takeoff of the breast. It starts at the junction of the preaxillary fullness (large horizontal arrows) and the outward curvature of the breast. If it is not obvious, the breast can be folded up (not just pushed up), as shown in Fig. 8‑13b, and the line of demarcation will become more clear (smaller vertical arrows).
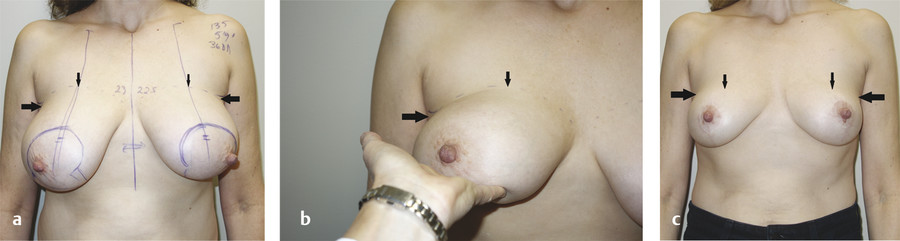
The patient in Fig. 8‑13 shows that the surgeon needs to evaluate not only glandular ptosis but also nipple position in all directions, not just elevation. Note that in the postoperative (18 months) photo (Fig. 8‑13c), the upper breast border has not changed from its original position.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree