10 Management of the Massive-Weight-Loss Breast
Summary
The massive-weight-loss patient can present with severe deformities of the breast, including major deflation of skin, loss of upper pole fullness, medialization of the nipple areolar complex, loss of the lateral curvature of the breast with prominent lateral chest roll, and loose and inferiorly displaced inframammary fold. Deformities of the breast can be complicated by surrounding soft tissue laxity of adjacent aesthetic units such as the upper abdomen, arm, lateral chest, or back. The dermal suspension, parenchymal reshaping mastopexy is the authors’ method of choice for restoring the breast to a youthful shape and normalized breast position on the chest wall. This chapter includes a review of careful patient selection for the procedure, discussion of staging of breast reshaping procedures relative to other aesthetic units, advantages and disadvantages, relative contraindications, and results from outcomes studies utilizing the dermal suspension technique. A step-by-step approach to marking the dermal suspension, parenchymal reshaping mastopexy will be described along with surgical tips and pearls to optimize results and reduce complications. Other surgical options for the massive-weight-loss breast will be discussed.
10.1 Introduction
The most effective and durable method to treat morbid obesity is bariatric surgery. 1 The landscape of bariatric procedures has changed over the past several years. According to the American Society for Metabolic and Bariatric Surgery (ASMBS), the number of bariatric procedures continues to increase, from 158,000 in 2011 to 228,000 in 2017. Popularity of procedures has shifted from the Roux-en-Y gastric bypass to the sleeve gastrectomy, which accounted for 59.4% of procedures in 2018. 2 After massive weight loss (MWL) resulting from such measures, thousands of patients present for breast-contouring procedures every year: 15,360 procedures in 2018, according to the American Society of Plastic Surgeons (ASPS). 3
The MWL breast presents a distinct surgical challenge. The deformities observed in the MWL breast are severe, far beyond what plastic surgeons usually see in the regular cosmetic patient, and present a great technical challenge. The MWL breast is not just ptotic and deflated but has specific unique features 4 , 5 :
Poor tissue quality, with redundancy and loss of skin elasticity.
Severe volume loss, especially in the upper pole, which may be asymmetric, with an enormous skin excess relative to parenchymal volume.
Ptosis (usually third-degree) and medialization of the nipple-areola complex (NAC).
Loss of lateral curvature of the breast and, occasionally, prominent lateral chest wall excess that merges with the breast.
Low and loose inframammary fold (IMF), especially laterally.
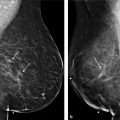
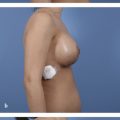
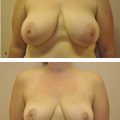
The breast deformities are often seen in concert with other upper body deformities after MWL, with surrounding aesthetic units of the lateral chest wall, arm, back, and upper abdomen also in need of concurrent evaluation (Fig. 10‑1).
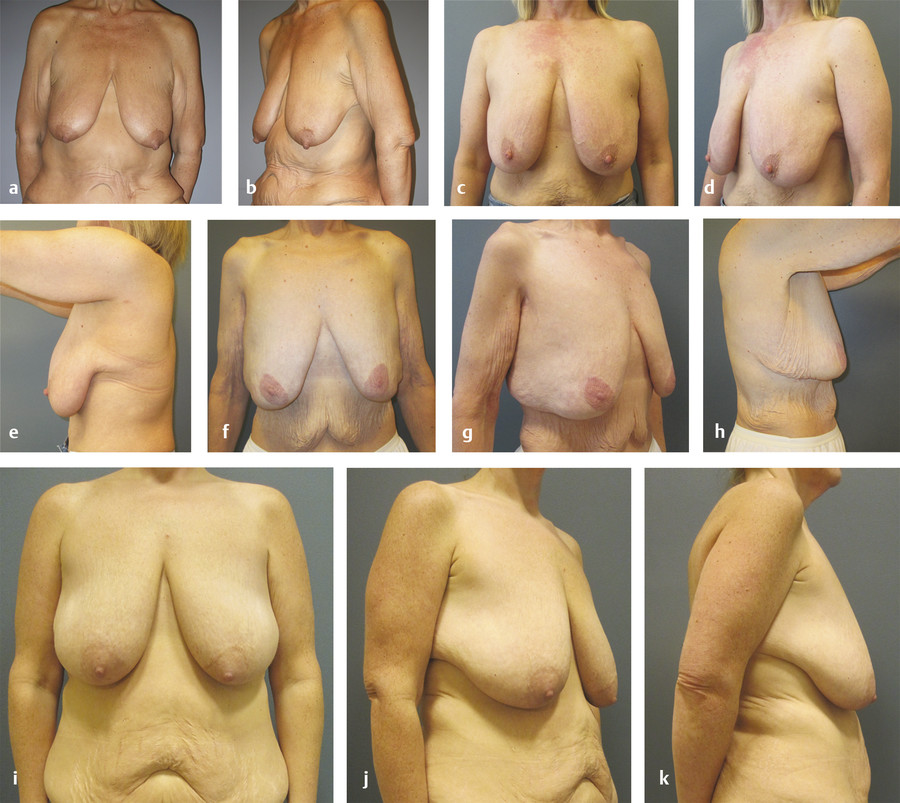
There are several goals of breast reshaping after MWL: to obtain a youthful, well-contoured breast; to restore volume, especially in the upper pole, with central projection; to position the nipple properly on the chest wall; to improve the lateral curvature of the breast; and, most importantly, to maintain the longevity of the result, which is especially relevant in patients after MWL because of their poor skin quality and tendency for recurrent skin laxity.
Most of the breast reduction and mastopexy techniques (with or without breast implants or added autologous tissue) fall short in addressing the deformities associated with the MWL breast because of progressive skin laxity with loss of projection, loss of upper pole fullness, bottoming-out and implant malposition. To choose the correct surgical procedure to achieve these goals, the surgeon must assess the volume, shape, degree of ptosis, laxity/excess tissues surrounding the breast, the patient’s desires, and what extent of scars she is willing to accept.
This chapter focuses mainly on the dermal suspension and parenchymal reshaping mastopexy pioneered by the senior author. 6 Several surgical procedures have been developed to aid in contouring the MWL breast, and these will be mentioned briefly.
10.2 Preoperative Assessment
10.2.1 Weight Stability
Patients after bariatric surgery lose most of their weight during the first and second year after the procedure. 7 Patients typically reach a nadir and then plateau at a slightly higher weight. Body contouring after weight loss typically is deferred until the patient is at least 12–18 months out from her weight loss surgery or start of self weight loss and has been stable for 3 months with only approximately 5 lb (2.25 kg) of weight fluctuation over that time. 8 , 9 Patients who are not yet weight stable or who have residual obesity are typically referred to weight loss specialists or their bariatric team, with a scheduled follow-up in 3 months for re-evaluation.
10.2.2 Nutrition
Certain bariatric procedures, such as the Roux-en-Y gastric bypass, have a malabsorptive component in addition to the restrictive nature of the surgery. Care must be taken to assess and correct nutritional deficiencies, as this is crucial for wound healing and minimizing the need for blood transfusion. All patients should have a thorough evaluation including albumin, prealbumin, iron, and vitamins A, D, E, K, and B12. Protein malnutrition may be present, especially for patients with malabsorptive procedures or fad diets. Patients are guided to increase their protein intake perioperatively with a goal of 75–100 grams per day.
10.2.3 Body Mass Index
Obesity is defined as body mass index (BMI) greater than 30 kg/m2. Several investigators have reported an increased risk for complications in patients undergoing body contouring procedures with a body mass index greater than 30 kg/m2. 10 , 11 , 12 , 13 , 14 A large cohort study of MWL patients undergoing multiple procedures demonstrated complications associated with maximal BMI prior to weight loss and change in BMI, or delta BMI. However, the exact etiology of this is not well understood, as many factors can contribute to complications. In addition, no strict BMI cutoff was determined to influence complications. 15 For this reason, the authors advocate for examining patients for breast contouring procedures on an individual basis, as a patient with a high BMI may have very deflated breasts but carry most of her excess weight in a pannus or thighs, which are not the patient’s priority or goal. Patients with lower BMI around the time of surgery typically obtain better cosmetic results, and patients with a BMI greater than 35 kg/m2 are not uncommonly referred for further weight loss prior to proceeding with surgery.
10.2.4 Preoperative Assessment and Comorbidities
At consultation, a complete medical and surgical history is obtained, including any personal or familial history of coagulopathies or thrombotic events; former problems with anesthesia; and history of breast cancer, breast disease, or prior breast surgery. Detailed medication history includes all prescription, over-the-counter, and herbal medications and specifically the use of aspirin, other nonsteroidal anti-inflammatory drugs (NSAIDs) or any other medication that might increase the risk of bleeding postoperatively. A history of substance abuse or need for chronic pain medication is obtained. Many of the comorbidities associated with obesity will resolve or improve with bariatric surgery, such as diabetes, sleep apnea, hypertension, heart disease, and gastroesophageal reflux disease (GERD) 16 , 17 , 18 ; however, depression and anxiety may not improve. Patients are often referred for consultation for various residual comorbidities, such as hematology evaluation for iron deficiency anemia, or to medical specialists for clearance for surgery (such as internal medicine, cardiology, or psychology).
Smoking increases the risk for surgical complications, and all patients should stop smoking for at least 4 weeks prior to and after surgery. 10 , 19 , 20 , 21 This is especially important for flap survival and prevention of distal flap necrosis. Urine cotinine prior to surgery is routinely measured in patients who state they have recently quit smoking.
Complete physical examination with a comprehensive breast exam and assessment of the position of the IMF, quality of skin, degree of ptosis and nipple position, amount of breast tissue, asymmetry, and adjacent tissue excess is mandatory.
Preoperative laboratory workup includes complete blood count with platelets, complete metabolic panel (including albumin), prothrombin, and activated partial prothrombin time within 30 days of surgery. Urine pregnancy testing is done in all reproductive-age women on the morning of surgery.
Chest radiograph and electrocardiograms are ordered as indicated by age and medical profile. All patients above 40 must obtain a mammogram prior to surgery.
Preoperative photography is obtained in standing position with anterior, lateral, and oblique views from the lower neck to the waist. Photographic documentation is important to analyze and plan the procedure properly as well as to document preoperative asymmetry and surrounding soft tissue deformities that may become more noticeable after the breasts are contoured.
During the consent process, it is important to make sure the patient has realistic goals and understands the limitations of plastic surgery, including possible asymmetry postoperatively and recurrent skin laxity despite how tight the tissues are in surgery. Managing expectations ahead of surgery can avoid significant patient and surgeon disappointment postoperatively.
10.2.5 Staging and Combination of Body-Contouring Procedures
Breast contouring after MWL is often done as a solo procedure; however, adjacent body areas may need contouring as well. Patients and the surgeon may opt to perform multiple procedures, depending on the patient’s desires, financial abilities, comorbidities, nutritional status, and ability to withstand a lengthy operation and recovery and on the surgeons’ experience and the available team.
When combining procedures, keep in mind the following: 22 , 23
Pulling in opposite vectors at the same time can limit results.
Patient safety comes first: if medical comorbidities preclude a lengthy operation, the surgical plan may need to be changed.
Consider the magnitude and stress of recovery when combining procedures.
Optimal staging and combination of procedures may not correspond with patient’s preferences.
Favorable procedure combinations including the breast are 10
Abdominoplasty + mastopexy: a common combination that gives the patient a powerful transformation.
Circumferential lower body lift + mastopexy.
Upper body lift + mastopexy: eliminating the upper body lift “dog-ears” while merging the incisions together.
Brachioplasty + mastopexy: curving the lateral chest incision into the axilla.
Vertical thigh lift + mastopexy.
Caveats for combining breast and other body contouring procedures:
Mastopexy may be safely combined with an abdominoplasty with excellent results. Since the IMF on the MWL breast is very loose and mobile, especially laterally, it may be displaced inferiorly upon completion of the abdominoplasty, requiring the surgeon to adjust the mastopexy markings. 10 , 22 Similarly, addition of a fleur-de-lis vertical extension to an abdominoplasty can mobilize the inframammary fold inferomedially. Hence, it is wise to complete the abdominoplasty before proceeding with the mastopexy. In cases where the IMF is completely nonadherent to the chest wall, it would better serve the patient to separate these two procedures completely.
Be careful of fresh triple point incisions, such as when combining an upper body lift + dermal suspension parenchymal-reshaping mastopexy + brachioplasty; these areas tend to break down and cause wound healing problems. 10 , 22 The mastopexy can be performed merging in the brachioplasty scar at the lateral chest, or merged into the upper body lift, delaying either the upper body lift or brachioplasty until a later time.
10.3 Dermal Suspension Parenchymal Reshaping Mastopexy
The dermal suspension and parenchymal reshaping mastopexy is based on an extended deepithelialized Wise pattern. The lateral and medial extensions, which would ordinarily be discarded in a breast reduction, are mobilized and incorporated into the breast mound as dermoglandular flaps for auto-augmentation. These help enhance the breast volume and improve shape while redefining the contour of the lateral chest wall. The dermoglandular flaps are suspended to the chest wall in multiple fixation points to ensure longevity of the result and secure the new nipple position, while plication of the broad dermal surface enables the surgeon to reshape the breast parenchyma and reposition the breast on the chest wall. This technique is very versatile in addressing and correcting the patient’s specific anatomy, as the surgeon can titrate the amount of breast tissue needed for the auto-augmentation by elongating the lateral extension or shortening it. The Wise pattern can be laterally extended beyond the borders of the T (lateral dermoglandular) flap to improve the contour of the lateral chest wall effectively, as needed.
This technique was developed based on previous publications discussing breast reconstruction, reduction, and mastopexy. In 1986, Holmström described breast reconstruction using a lateral thoracodorsal fasciocutaneous flap for auto-augmentation with or without an implant, based on redundant tissue of the lateral chest wall. 24 In 1999, Frey published his technique of a bralike dermal suspension method for breast reduction, which was secured to the deep fascia of the chest wall, with a B-formed incision, eliminating the medial inframammary scar. 25 Lockwood described superficial fascial system (SFS) suspension with nonabsorbable sutures to improve scarring and achieving long-lasting results. 26 Gulyás developed a periareolar dermal cloak, relying on dermis for glandular support. 27 In 2002, Graf and Biggs described creating an inferiorly based de-epithelialized flap, which was mobilized superiorly and held in place by a loop of pectoralis muscle, to maintain upper pole fullness with added support by suturing the dermal edges of the flap to pectoralis muscle fascia. 28 In 2003, Qiao et al published their technique for breast reduction with a crescent glandular resection excluding the inferior quadrant of the breast, with creation of a dermal bra, secured to the pectoralis muscle fascia. 29 Several other investigators have published reports on their experience with auto-augmentation of the MWL with local flaps. 30 , 31 , 32 , 33 , 34 , 35
Patients who would benefit most from this technique are MWL patients, with ptotic, deflated, and flattened breasts, an excess of inelastic skin, and prominent axillary folds, providing sufficient tissue for auto-augmentation.
Those patients with inadequate amounts of tissue for auto-augmentation may be candidates for an implant-based augmentation-mastopexy or other auto-augmentation methods. Patients with ptosis and significant excess parenchymal breast tissue would be better served with a formal breast reduction, as described in the algorithmic approach to the MWL breast by Colwell et al. 36
10.3.1 Advantages of This Technique
The method is safe with reliable, long-lasting, reproducible results and a low complication rate.
It uses all the available breast tissue and surrounding autologous tissue (as needed), avoiding the need to use breast implants with their associated morbidity and tendency to descend over time or develop ptosis of natural tissues over the implant.
It repositions the NAC on the chest wall, securing its position intraoperatively with ease, with less chance of bottoming out thanks to the secure suspension to the chest wall.
It enables the surgeon to shape the breast parenchyma, restoring upper pole fullness and mammary projection.
It enables the surgeon to reshape the skin envelope of the breast without relying on it for support of the breast tissue and NAC position.
It improves the lateral chest contour by eliminating the lateral skin roll and re-creating a discrete lateral curvature.
It may be combined with other body-contouring procedures safely.
10.3.2 Disadvantages of This Technique
It requires longer operation times because of extensive de-epithelialization and intraoperative tailoring (a two-team approach increases efficiency and decreases operative time).
It cannot be easily combined with an implant for further augmentation. The patient must have enough autologous tissue available for auto-augmentation. Should the patient desire additional volume, a subpectoral augmentation may be added in a separate future procedure.
10.3.3 Relative Contraindications
Active tobacco users are at risk of flap necrosis.
Patients with previous breast surgery are at risk of inadequate perfusion to undermined tissues.
In non-MWL breasts, tight parenchymal reshaping or skin closure can increase risk of parenchymal or skin necrosis.
10.3.4 Markings
The patient is marked in a standing position, based on an extended Wise pattern marking with a central pedicle.
Mark the sternal notch and midline.
Mark the breast meridian: at the midclavicle (approximately 6 cm from the sternal notch), a line is dropped toward the IMF. In many MWL patients, the breast meridian will not be in line with the nipple, as the nipple is often medialized.
Mark the new nipple position on the breast meridian: Pitanguy’s point is projected forward by placing a hand at the level of the IMF and projecting the point forward. In patients with very descended IMFs, this point may need to be elevated slightly, but care should be taken not to overelevate the IMF and thus the new nipple position. Check for symmetry.
Mark the extended Wise pattern:
The superior part of the keyhole (representing the new upper border of the areola) is placed 2 cm above the new nipple position.
7-cm vertical limbs are drawn from the new nipple position. The keyhole is then designed extending from the point 2 cm above the new nipple position to 2 cm down each vertical limb. This maintains a 5-cm vertical limb that represents the new inferior nipple-to-IMF distance. An 8-cm base (angle of divergence) is planned. If the patient has more dense breast parenchyma, the angle of divergence may be narrowed, reducing the amount of parenchyma internally for reshaping and increasing the amount of skin externally. In addition, the vertical limbs can be extended to increase the estimated length from the bottom of the nipple to the IMF (Fig. 10‑2).
Mark the medial point of the extended Wise pattern: typically, at the takeoff of the breast.
Mark the IMF: a “cheat” may be marked at the middle part of the central pedicle (along the breast meridian) to further reduce tension at the T point junction further. If not needed, it can be de-epithelialized prior to incision closure.
Mark the lateral point of the Wise pattern: this will determine how much of the axillary roll will be de-epithelialized and incorporated into the breast for auto-augmentation. Tissue is routinely taken and consistently reliable to the mid-axillary line. Excision may be extended to the posterior axillary line and farther to improve contour of the lateral chest wall.
Connect the lateral point to the vertical limb of the Wise pattern in a curvilinear line: this conserves more tissue medially and creates a larger takeout laterally.
Mark the second and third ribs bilaterally.
Mark the superior footprint of the breast by pushing up on the breast to simulate the upper boundary of the breast.
Check for symmetry in the markings between the breasts (Fig. 10‑3).
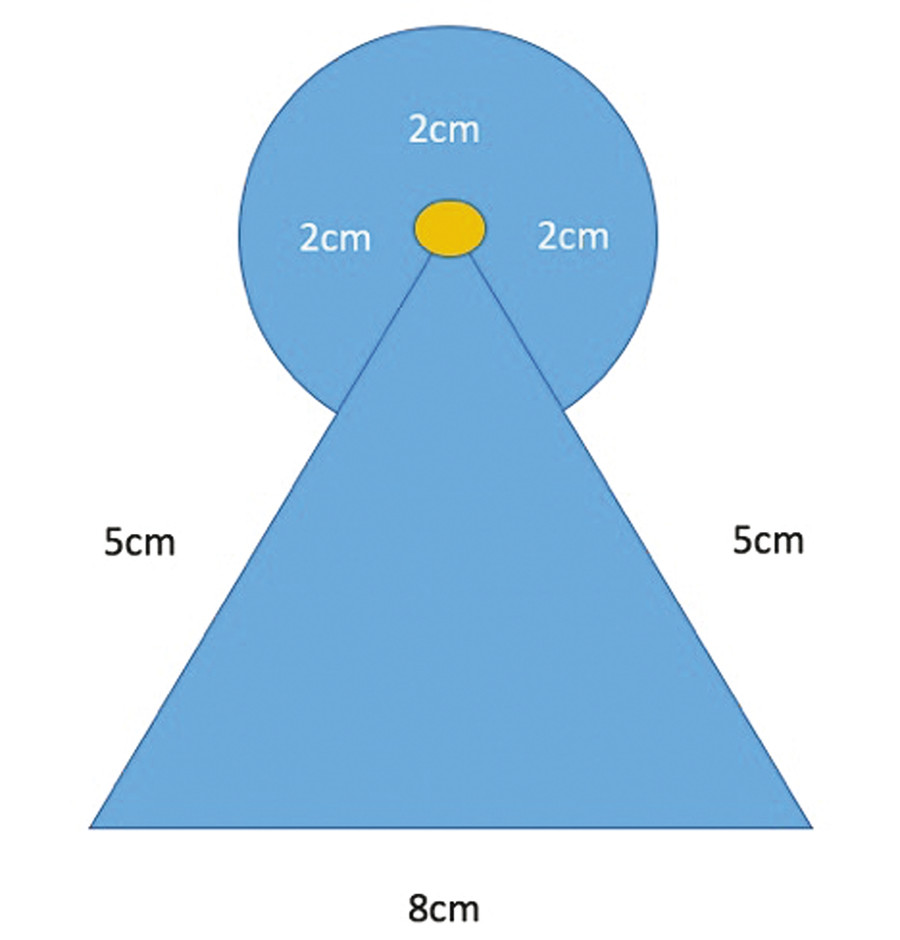
Fig. 10.2 Keyhole for the extended Wise pattern. 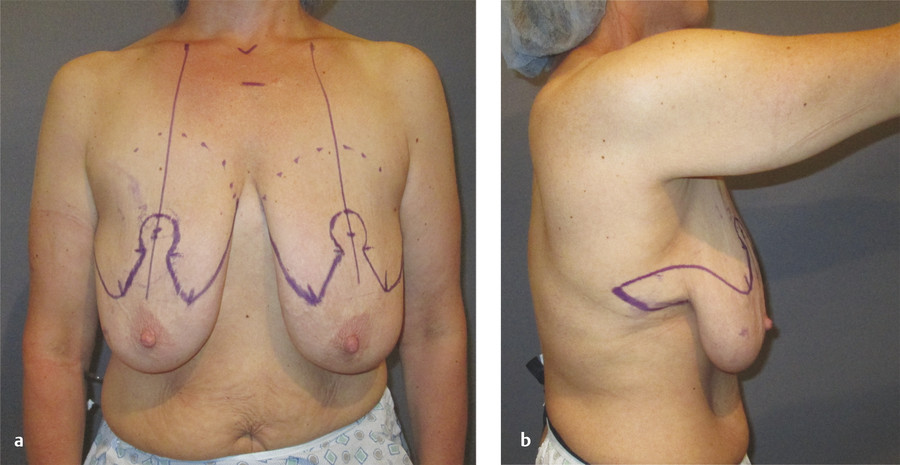
Fig. 10.3 Markings for dermal suspension parenchymal rearrangement mastopexy. (a) Anterior. (b) Lateral.
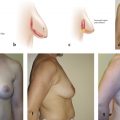
Preoperative asymmetry in nipple position is taken into consideration during the markings to avoid asymmetric nipple placement during the dermal suspension. To correct for the asymmetry, the keyhole markings are the same bilaterally, but less tissue is de-epithelialized on the side of the lower nipple to account for the discrepancy. The excess skin above this new point is excised (Fig. 10‑4).
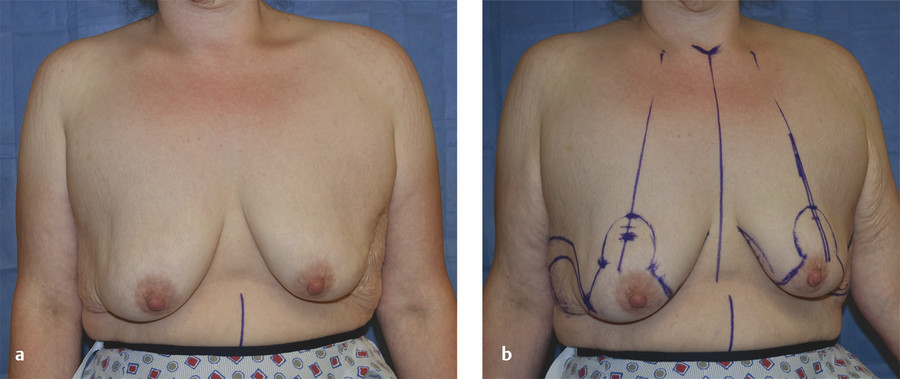
10.3.5 Surgical Technique
The patient is placed in the supine position, arms abducted to 90°. Care is taken to secure the arms to padded arm boards, as the patient will be in a near-sitting position for a large part of the surgery.
Mark the areola with a 42-mm nipple washer or cookie cutter.
Superficially inject a local anesthetic solution (epinephrine 1:100,000) to areas of de-epithelialization (the entire region within the Wise pattern, excluding the NAC).
De-epithelialize the entire extended Wise pattern with its extensions medially and laterally.
Mark a 10-cm-wide central pedicle at the base of the breast starting 7 cm from the most medial point of the extended Wise pattern (Fig. 10‑5).
Use electrocautery to score all around the Wise pattern markings to reach breast parenchyma, excluding the 10-cm base of the central pedicle inferiorly (Fig. 10‑6).
The upper breast flap is then raised with a 1- to 1.5-cm thickness until the chest wall is reached. Undermining along the breast meridian continues until the second rib is clearly palpable. A subcutaneous pocket is created, into which the breast tissue—which is now isolated on a central mound as a dermoglandular flap (with robust blood supply)—will be transposed as it is being shaped. Care should be taken not to overdissect medially, as this can result in a symmastia appearance of the breasts. Similarly, the lateral attachments of the upper flap should be released only as needed to accommodate the newly constructed breast mound (Fig. 10‑7).
The lateral and medial dermoglandular flaps are then elevated off the chest wall at the level of the fascia over the chest muscles, preserving as many significant perforating vessels as possible near the flap base. Care is taken to check routinely that the 10-cm central pedicle thickness is preserved, as it can easily be undermined unconsciously in a much-deflated breast. The authors typically limit the lateral extent of the dermoglandular flap to the mid- or posterior axillary line, since incorporating tissue distal to that point carries the potential risk of fat necrosis. Trim the lateral flap as needed for auto-augmentation, discarding distal tissue removed for contour purposes (Fig. 10‑8).
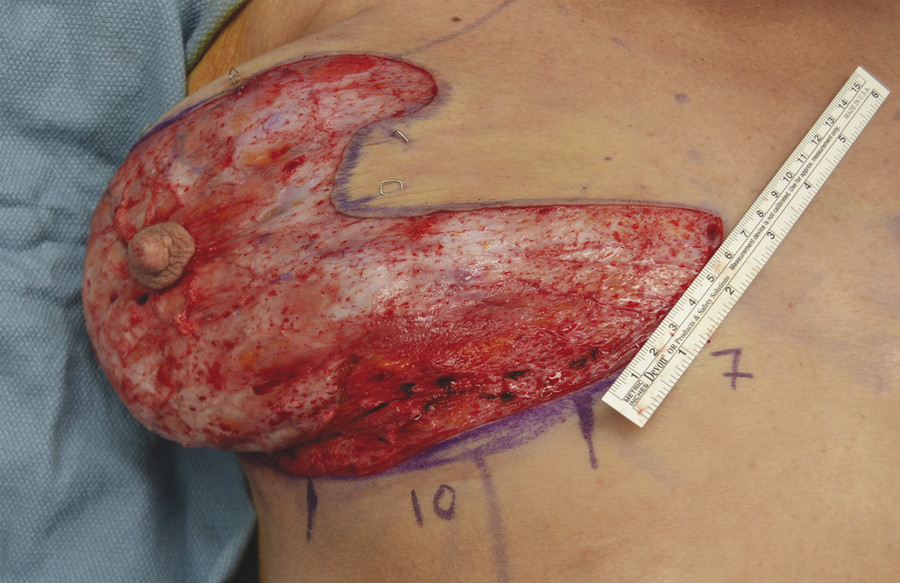
Fig. 10.5 Marking a 10 cm wide central pedicle: Determine the location of the central pedicle, approximately 7 cm from the most medial point of the extended Wise pattern. These measurements can be altered based on breast size or chest width. 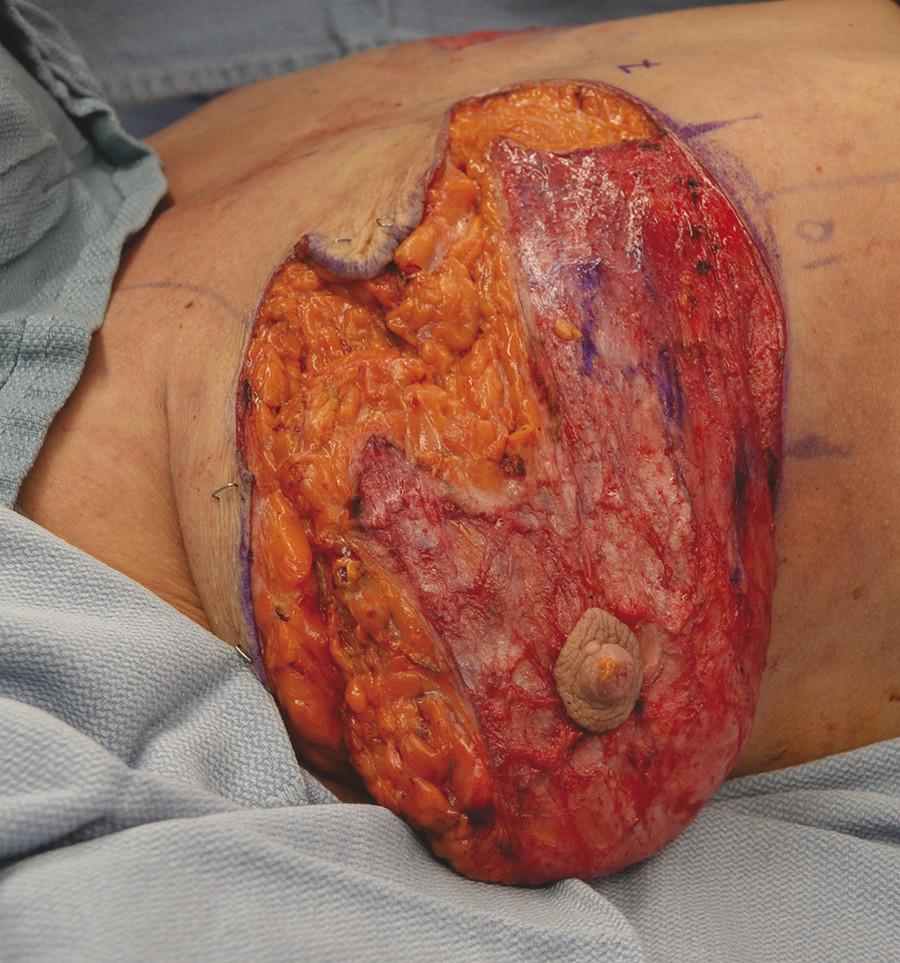
Fig. 10.6 Scoring all around the extended Wise pattern, excluding the central pedicle 10-cm base. 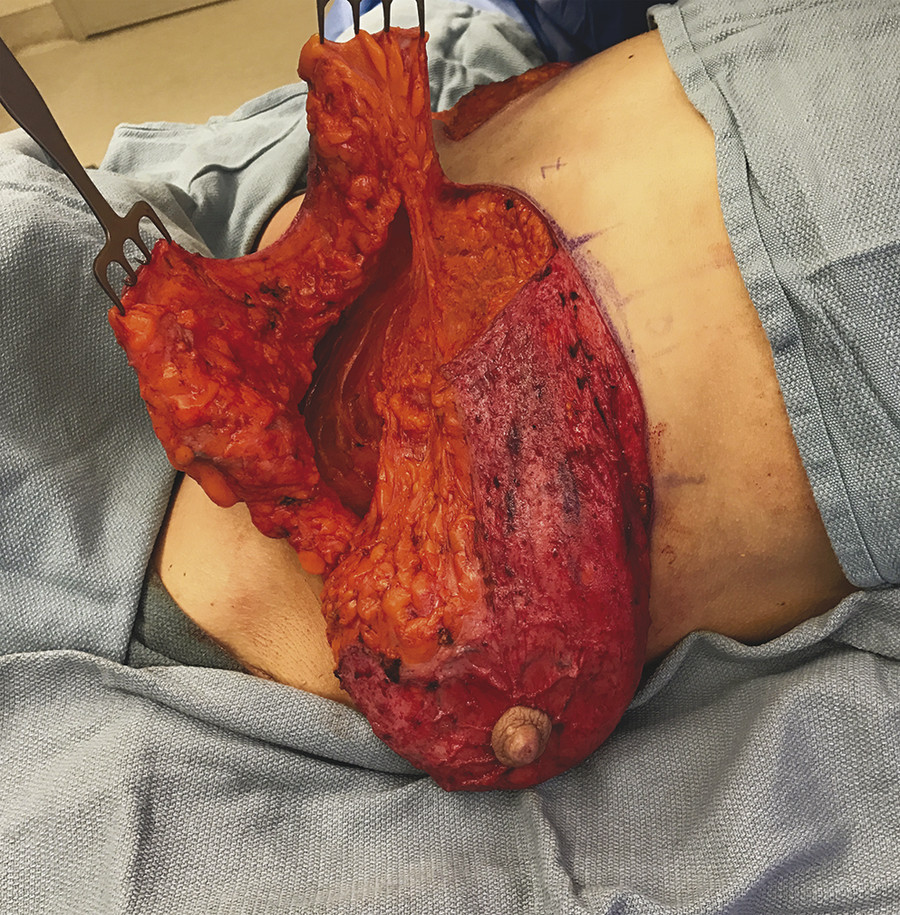
Fig. 10.7 Elevation of the upper breast flap, keeping it 1–1.5 cm thick, and additional pocket creation along the breast meridian, taking care not to overdissect medially and laterally, up to the level of the clavicle. 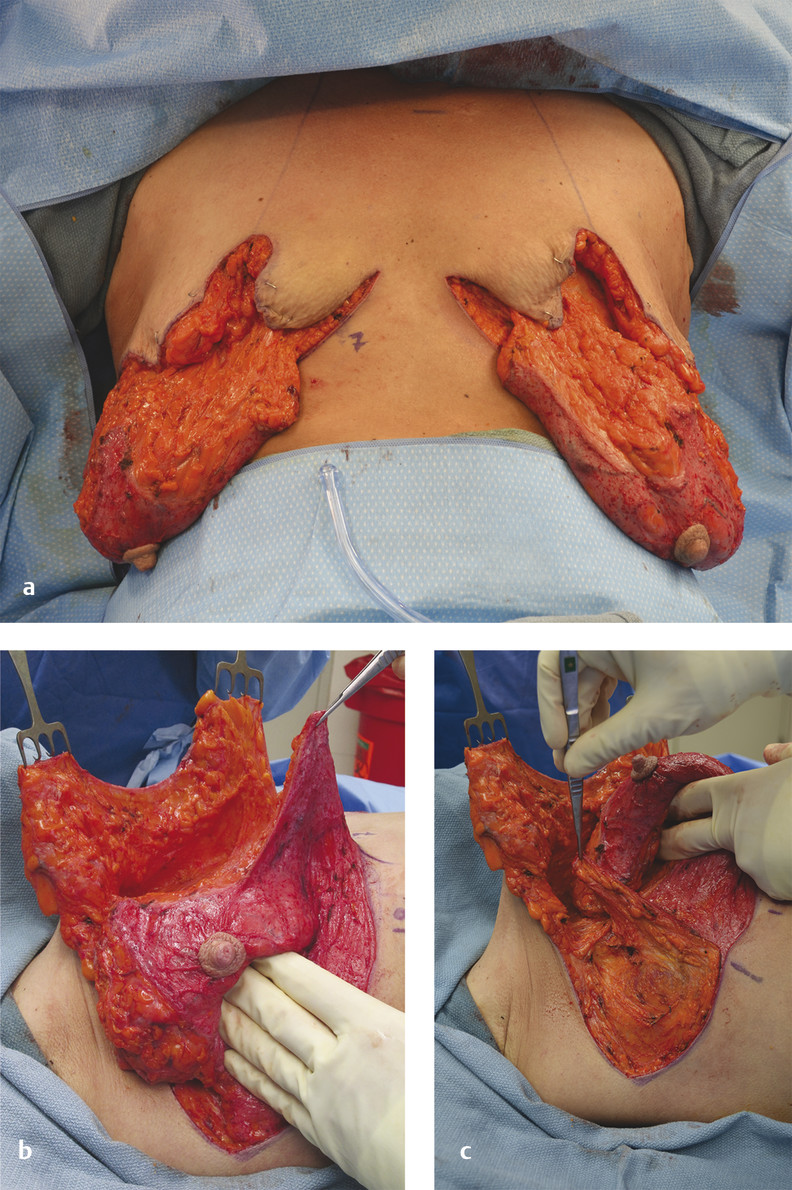
Fig. 10.8 (a) After elevation of the central, medial, and lateral dermoglandular flaps. (b) The medial flap. (c) The lateral flap.
Dermal Suspension
Reposition the patient in a near-sitting position. The upper flaps are elevated with Deaver retractors. The desired height of suspension is determined intraoperatively, usually the second rib. In a very ptotic breast, reaching the second rib is usually simple. However, if the NAC was relatively well positioned on the breast mound preoperatively, it is suggested to move the central mound down to the third rib to avoid a difficult nipple inset at the end of the case.
Suspend the superior dermal edge of the keyhole on the central pedicle to rib periosteum (usually the second rib) using a permanent 0 braided nylon suture in a mattress fashion along the breast meridian. Reinforce with a second similar suture, next to the first one. This sets the axis of the breast on the chest wall. To perform safely, place your fingers in the intercostal spaces and feel the rib between your fingers, passing the needle between them, making sure to take a good bite including rib periosteum.
Redrape and check nipple height. If it is too high because of a short distance on the keyhole pattern, drop the suspension suture down to the third rib. If the NAC is very ptotic at the second-rib position, you may plicate the dermis superior to the NAC to help elevate nipple position more (Fig. 10‑9).
Suspend the distal edge of the lateral flap one rib below the central flap (usually the third rib), and directly underneath it (essentially positioning it behind the central flap) along the breast meridian. This avoids a breast shape that is too wide (Fig. 10‑10).
The medial flap is often not very robust in size. It is typically suspended to the fourth rib periosteum to provide medial fullness once the breast flaps are redraped (Fig. 10‑11, Fig. 10‑12).
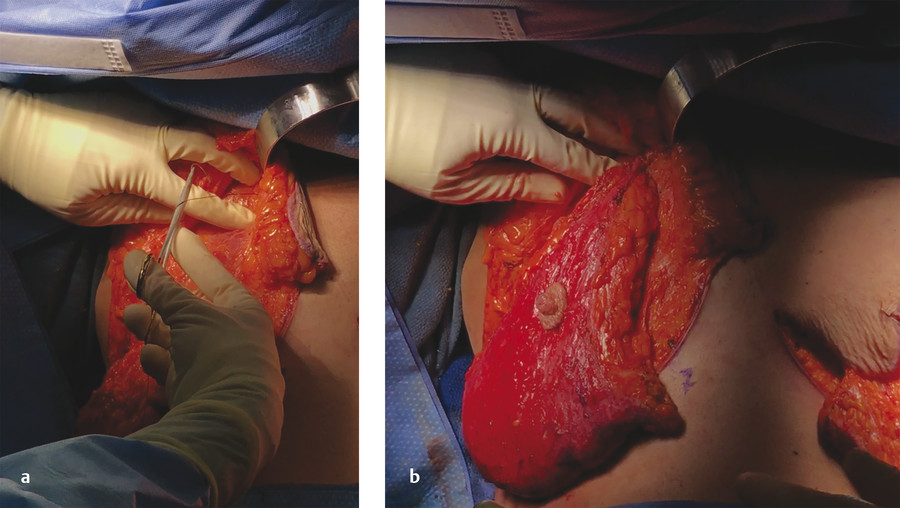
Fig. 10.9 (a) Suspension of the central flap (and the nipple areola complex) to the second-rib periosteum along the breast meridian using a permanent 0 braided nylon horizontal mattress suture. It is important to support the breast while tying the suture. Patient is in a near sitting position. (b) After suspension of the central flap. 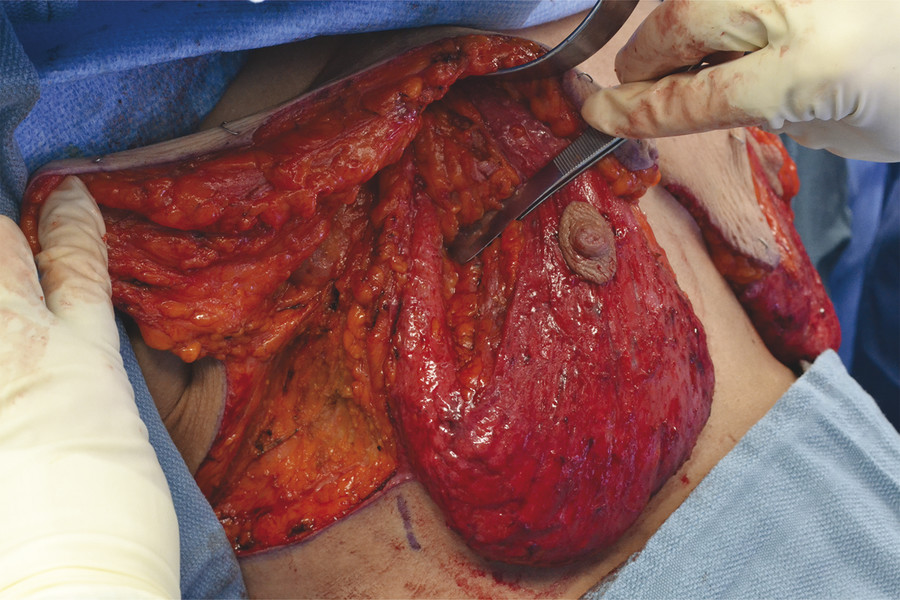
Fig. 10.10 Suspension of the lateral flap one rib below the central flap, exactly underneath the central pedicle suspension suture, using a permanent 0 braided nylon suture. 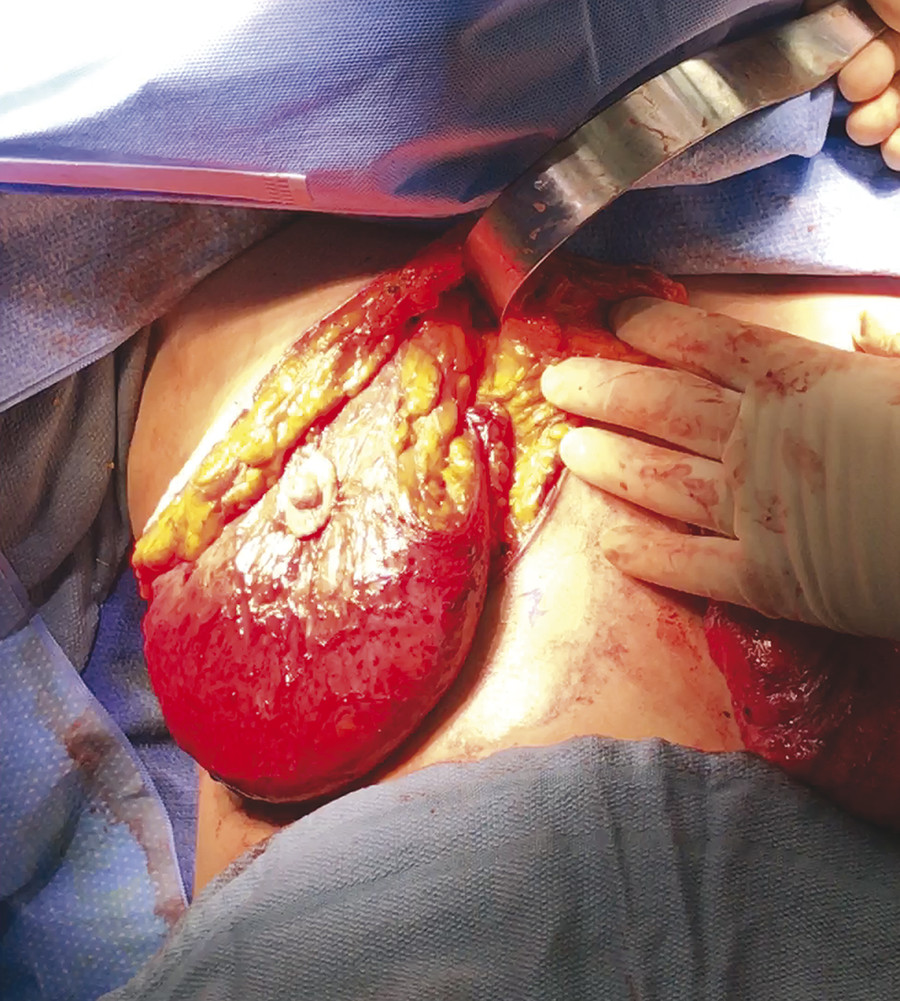
Fig. 10.11 Suspension of the medial flap, usually to the fourth rib, using a permanent 0 braided nylon suture. 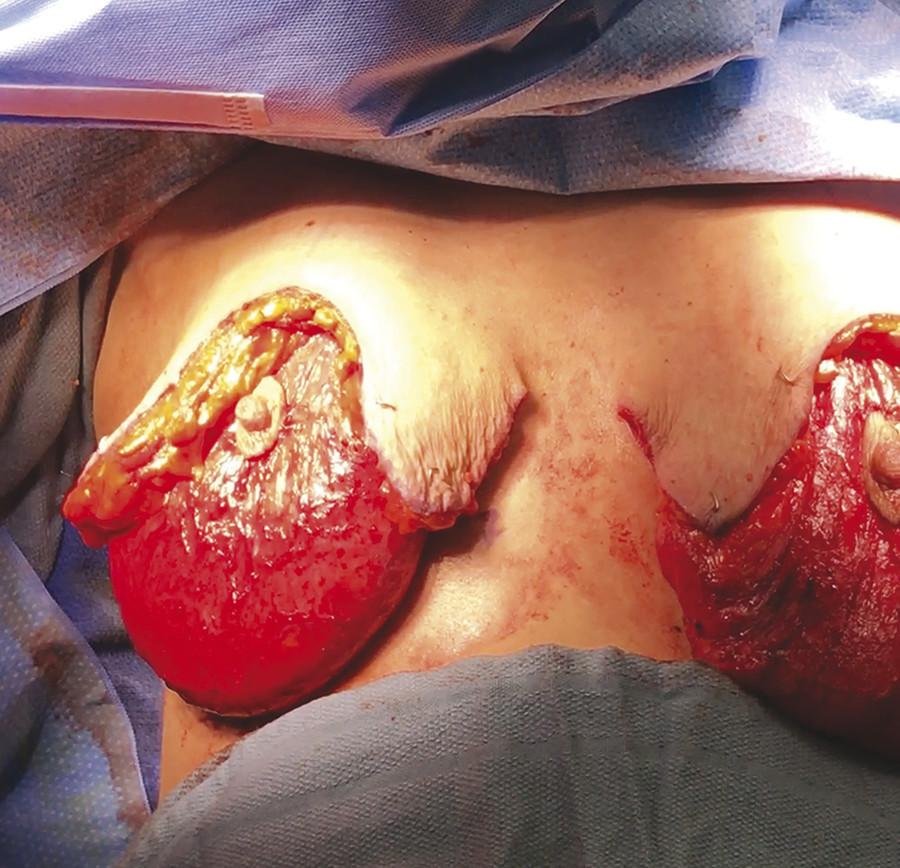
Fig. 10.12 After completing suspension of the central, lateral and medial flaps, redrape the skin to check for obvious asymmetries and discrepancy in volume so that the excess parenchyma can be resected before reshaping if needed.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree