7 Preoperative Evaluation of Patients with Macromastia and Ptosis
Summary
The preoperative evaluation of patients with macromastia and ptosis is a complex topic, as the definition of macromastia is not always clear. It is generally accepted that reduction mammaplasty can be a therapeutic rather than purely cosmetic procedure. However, regardless of whether the breast reduction surgery is motivated by cosmetic or therapeutic goals, the essence of the procedure remains the same. The goals of surgery are to reduce breast weight and volume, improve shape and asymmetry, remove excess skin, and reposition the nipple areola complex (NAC). The realization of these goals results in the regaining of a more youthful appearance. A thorough history and physical exam are an essential part of the preoperative assessment and enable the physician to recognize modifiable risk factors. However, surgeons should not limit patient access to this therapeutic procedure based on isolated comorbidities. It has been widely published that reduction mammaplasty surgery has one of the highest satisfaction rates of all plastic surgical procedures, and postoperative outcomes have repeatedly been shown to improve quality of life and provide positive emotional and aesthetic results that are long-lasting.
7.1 Introduction
Breast reduction surgery is one of the most common plastic surgical procedures, with over 60,000 operations performed annually. 1 , 2 It is generally accepted that reduction mammaplasty can be a therapeutic rather than purely cosmetic procedure. However, regardless of whether the breast reduction surgery is motivated by cosmetic or therapeutic goals, the essence of the procedure remains the same. The goals of surgery are to reduce breast weight and volume, improve shape and asymmetry, remove excess skin, and reposition the nipple areola complex (NAC). 3 The realization of these goals results in the regaining of a more youthful appearance. It has been widely published that reduction mammaplasty surgery has one of the highest satisfaction rates of all plastic surgical procedures. 4 In cases where patients present with symptomatic macromastia, more than 90% report improvement or resolution in symptoms after surgical intervention. 5 , 6 Postoperative outcomes have repeatedly been shown to improve quality of life and provide positive emotional and aesthetic results that are long-lasting. 5 , 7
7.1.1 Definition of Macromastia
The definition of macromastia is not always clear, and therefore, the preoperative management of patients with breast hypertrophy is a complex topic. However, there are a few minimum criteria that must be met in order to classify a patient as having symptomatic macromastia. History and physical examination are an essential part of the preoperative evaluation, and certain topics, as described in the following sections, must be addressed to support the diagnosis adequately. It has been argued that symptomatic macromastia is better defined by a complex combination of physical and emotional complaints than simply by breast volume and the amount of tissue to be removed. 8
7.2 Preoperative Consultation
The goals for the initial preoperative consultation are to understand the patient’s current complaints; to establish whether the patient’s goals for surgery are cosmetic, therapeutic, or both; and to determine the risks and benefits of surgical intervention. Documentation is one of the simplest things a physician can do preoperatively to ensure that the elective breast surgery is successful. At a minimum, photographs illustrating severe breast hypertrophy are necessary, but other reports of associated symptoms can also be useful, especially if the patient is seeking insurance coverage for the surgery. The components of a thorough preoperative evaluation are discussed in detail in this and the following sections.
7.2.1 Presenting Symptoms
If it is established that the motivation for surgery is therapeutic rather than cosmetic, most insurance companies require patients to obtain preauthorization for surgical procedures. It is essential that the physician be aware of the required information and documentation at the preoperative appointment, since preauthorization is based heavily on subjective information and symptom duration that may not surface unless the appropriate questions are asked (Box 7.1 , Box 7.2). 6
Box 7.1 Key Elements of History to Assess for Risk of Breast Reduction Complications
Patient symptoms and expectations
Comorbidities (including diabetes, hypertension, coagulopathy, connective tissue disorders, obesity)
Previous hypertrophic scarring
Smoking habits
Obstetric history
Medications
Mammogram status
Box 7.2 Key Elements of Physical Examination to Assess for Risk of Breast Reduction Complications
Shape
Symmetry
Contours
Scar location
Skin quality and elasticity
Nipple areola complex (NAC) shape
NAC position relative to inframammary fold (IMF)
NAC position relative to the volume of the breast
Volume distribution of both skin and parenchyma
Specific measurements (suprasternal notch–to-nipple distance, breast base width, nipple-to-IMF distance, nipple-to-midline distance)
Estimated volume of resection
A subjective history of neck pain, shoulder pain, lower back pain, and mastodynia is the most common combination of presenting symptoms of patients with macromastia. 5 These symptoms must be causing significant pain for greater than 1 year in order for the condition to be acknowledged by insurers. 3 , 9 , 10 Typically, the natural history involves the onset of pain during late adolescence with slow progression of symptoms as the breasts fully develop over time. Breast hypertrophy may eventually cause a change in posture resulting in progressive kyphosis, which could possibly be a subconscious attempt to hide the macromastia or the inevitable result of excess weight on the anterior chest wall. 7 , 11 When present, kyphosis should be documented through plain film X-rays of the cervical and thoracic spine, and any patients with chronic back pain should be evaluated by a qualified spine surgeon to rule out neurologic pathology. 11
Patients may attempt to offset the added weight of their breast hypertrophy with use of wide-strap support bras or even multiple sports bras; however, this often fails to improve the pain and may actually cause new-onset shoulder pain and shoulder grooving due to the pressure of the bra straps. The use of multiple support or compression garments naturally leads to the onset of intertrigo. Baby powder or antiperspirant may improve the symptoms temporarily; however, chronic skin irritation will ultimately occur and lead to superficial bacterial or fungal infections and tissue maceration with skin breakdown. 9 , 10 Additionally, the long-term result of macromastia is ultimately breast ptosis. The weight of the excess breast volume will pull the tissues caudally, necessitating the use of constant support bras, which further exacerbates the issue of intertrigo, as just mentioned.
Other serious complaints often associated with macromastia include respiratory difficulty, which can lead to inability to exercise and, ultimately, decreased functional capacity. 3 In extreme cases, this debilitation can prevent patients from performing physically demanding jobs and cause lifelong disability. 3 Less common presenting complaints include neurologic symptoms such as ulnar paresthesias and chronic occipital headaches. 4 Since patients may not be aware of the association between breast hypertrophy and these complaints, they may not mention them unless specifically asked by the physician.
It is generally recommended that conservative treatments be attempted prior to proceeding with reduction surgery. Insurance companies may ask for documentation showing that the patient has failed conservative measures for at least 3 months prior to seeking approval for a therapeutic reduction mammaplasty. 9 , 10 Nonsurgical treatment options include trials of nonsteroidal anti-inflammatory medications, dermatologic intervention for skin concerns, and use of specialized support bras. Even physical therapy and chiropractic manipulation are encouraged before surgical intervention is considered indicated. However, these nonoperative interventions have been shown to be only rarely successful in improving symptoms in the long term. 12
In addition to the physical manifestations that can cause a patient to present for evaluation for possible reduction mammaplasty, the psychologic manifestations can also be profound. Specifically in younger patient populations, macromastia can lead to a decrease in self-confidence, particularly in social situations where sexual attention may occur and in athletic settings where the individual is required to wear activewear or swimwear. This is more than just a cosmetic concern; it has the potential to lead to an actual impediment to emotional development in adolescents. Despite this, some insurers will not cover breast reduction surgery in patients under the age of 18 years old. 4 , 6 Elective breast surgery in this adolescent population is discussed in detail in Section 7.2.5.
It is important to note that with all of the presenting complaints outlined here, the severity of symptoms does not always correlate with degree of breast hypertrophy. 13 Thus, physicians should not discourage patients with relatively mild macromastia from proceeding with surgery if it has been determined that the patient’s complaints are truly due to her breast hypertrophy and not other somatic or psychological pathology.
7.2.2 Medical and Surgical History
Once the chief complaint has been thoroughly addressed, it is important to obtain a complete medical and surgical history, as this can identify early risk factors for surgical complications and initiate the process for surgical optimization. Medications must be reviewed, specifically identifying any current or prolonged history of steroid use, which can negatively impact wound healing; any anticoagulation medications, which can lead to increased risk of intraoperative and postoperative bleeding and hematoma formation; and the use of hormonal birth control or oral estrogens, which can dramatically increase the likelihood of postoperative deep venous thrombosis (DVT) or pulmonary embolus (PE). In cases where these medications are identified, surgeons must work with the primary care and specialty care physicians to determine whether it is safe to discontinue their use temporarily for surgery or whether the risk of doing so outweighs the benefits of this elective procedure.
Several other topics are important factors in the preoperative planning of any breast-related surgery. One is the patient’s individual weight history, including any major weight loss such as in the postbariatric setting, which can have profound impact on the reduction technique employed and the surgical outcome. Additionally, a history of prior soft tissue infections, especially methicillin-resistant Staphylococcus aureus (MRSA) infections, should be identified, as these can increase the risk of future infections, and any intraoperative antibiotic therapy may need to be adjusted accordingly. Finally, a personal or family history of keloids or unfavorable scars should be reviewed. Since reduction mammaplasty requires long incisions and, therefore, results in extensive scars, the risk of scar hypertrophy, hyperpigmentation, or keloid formation should be discussed in the preoperative setting.
7.2.3 Breast History
A detailed breast history is absolutely essential to providing appropriate patient care and preventing potentially unfavorable postoperative complications. Any current or past breast masses should be thoroughly investigated to ensure that malignancy is ruled out. Additionally, any previous breast biopsies, whether benign or malignant; any personal history of breast cancer, with or without surgical treatment; and any family history of breast cancer need to be outlined. The date of the patient’s last mammogram should also be noted, along with the results and any secondary testing performed. In patients who are identified preoperatively as being high-risk for future breast malignancy, it is prudent to discuss with the patient the surgical plan if an occult malignancy is encountered intraoperatively.
Outside of breast cancer, A few other aspects of breast history should be discussed because they can have an impact on surgical planning. Any previous breast surgery, such as a prior augmentation, reduction, or mastopexy, needs to be identified. Additionally, any future plans for pregnancy should be explored, as this can dramatically change the breast volume and degree of ptosis. As such, some physicians recommend that elective breast surgery be deferred until no further childbearing is planned. Deferring surgery also alleviates concerns regarding the ability to breastfeed postoperatively, which is discussed in more detail in Section 7.5.1, Possible Complications.
7.2.4 Comorbidities
After thoroughly evaluating the physical and emotional symptoms and establishing an accurate diagnosis of symptomatic macromastia, the discussion should turn to the topic of comorbidities. Since the only true method for correcting the symptoms associated with breast hypertrophy and ptosis is surgery, which is discussed in detail in Chapter 8, Mastopexy Techniques—Basic Principles, identifying comorbid conditions that could threaten the success of a surgical intervention is essential.
Use of Tobacco Products
Regardless of whether a reduction mammaplasty or an isolated mastopexy is planned, a vascular pedicle to the nipple must be isolated, and tobacco use can have a major impact on wound healing or blood flow with nipple translocation. It has been reported that smoking can double or even triple the risk of major postoperative complications, specifically fat necrosis and other wound complications leading to reoperation. 2 , 14 , 15 , 16 If the patient is a current tobacco user, cessation of all tobacco products must be achieved for a minimum of 3 to 4 weeks before surgery. Even passive or secondhand smoke can have clinically significant negative effects on vascular perfusion and wound healing. This abstinence from nicotine products should, if at all possible, be continued for another 3 to 4 weeks after surgery as well, to facilitate wound healing. 16 , 17 There has been a recent trend toward preoperatively screening patients for tobacco exposure with urine cotinine tests. Most in-office tests can detect direct or passive exposure over the past 4 days and are an excellent way for nicotine abstinence to be verified in an economic and convenient manner. If, for whatever reason, complete abstinence is not achieved but surgery proceeds, the physician should limit the distance the nipple is translocated and perform a far less aggressive dissection in hopes of maintaining blood flow to the skin.
Obesity
Any patient with a body mass index (BMI) greater than or equal to 30 is considered obese. 11 A high BMI has been shown to be associated with wound healing complications, such as skin and fat necrosis, and a greatly increased risk of infection. 18 , 19 , 20 In one study in which patients were grouped based on the degree of obesity, those considered moderately obese (BMI 30–35) had a relative risk (RR) for major complications after reduction mammaplasty of 1.45 compared to the general population, and those considered severely obese (BMI 35–40) had an RR of 1.71 for major complications compared to the general population. 20 Additionally, obese patients have increased anesthesia risks.
Although it is certainly reasonable for the surgeon to calculate a patient’s BMI at the preoperative visit, the individual patient’s surgical risk stratification should be determined in collaboration with a primary care physician (PCP). Additionally, obese patients should be screened for diabetes, as this is a separate risk factor from obesity for postoperative complications and causes a significantly higher risk of nipple necrosis. 21 In cases where a reduction mammaplasty is being performed on an obese diabetic patient, the surgeon may need to accept a smaller volume reduction in order to prevent complications related to metabolic syndrome.
Since an increased BMI is considered a modifiable risk-factor, the option of preoperative weight loss should be encouraged in all overweight and obese patients if possible. In patients with a BMI over 30, this may even be required by some insurance agencies as a prerequisite for insurance coverage of the proposed breast reduction surgery. 4 , 6 However, some argue that weight loss may be difficult to achieve in patients with symptomatic macromastia due to the reduced functional capacity outlined in Section 7.2.1 and that surgery may promote additional weight loss after recovery. 22 It has been shown that obese patients lose an average of almost 9 lb (4 kg) after breast reduction surgery, which is far more than the weight lost through the surgical resection of breast tissue. 13 A large multicenter prospective trial called the Breast Reduction Assessment: Value and Outcomes (BRAVO) study showed that obesity did not change the benefits of reduction mammaplasty surgery and that, despite pressure from insurance companies, physicians should not use obesity as a justification for not surgically treating symptomatic macromastia. 12 However, patients should be informed of the effects of significant weight gain or loss after surgery, as this can permanently distort previously acceptable aesthetic results.
7.2.5 Age
Although most patients who present for evaluation of symptomatic macromastia are 30–40 years of age, there is a small proportion of patients who present well before or after this age seeking surgical intervention for their breast hypertrophy or ptosis. 3 Additional time should be spent in the preoperative setting when considering treatment of macromastia in such younger or older patients, as special consideration needs to be given to ensure proper management.
Adolescent Patients
The adolescent female patient population is usually defined as girls 11–17 years of age. In the past, there has been a general reluctance to treat these patients surgically, as it was felt that intervention for cosmetic reasons should be deferred until adulthood. However, recently, there has been a slowly growing trend to intervene at an earlier age, since multiple studies demonstrate the significant emotional sequelae that can occur if macromastia is left untreated. 23 For example, macromastia in the adolescent can cause social issues and stressors, leading the adolescent patient to avoid social situations where there is chance for ridicule or other undesirable peer responses. This reluctance to be involved in the social setting can ultimately impede emotional growth. 14 As such, increasing numbers of young patients are being referred by their pediatrician, PCP, or gynecologist for plastic surgical evaluation and possible treatment of their breast hypertrophy. 23 In these cases, physicians should encourage parental involvement and education, as patients who are under the age of 18 are considered a venerable population and will need parent or guardian consent for any surgical intervention. Additionally, it is important to note that adolescent patients tend to be more motivated by cosmetic concerns than the adult patient population is. Therefore, before proceeding with breast reduction surgery, the treating physician needs to be sure that the patient and her parents understand that they will be trading breast size for extensive permanent scars.
There is a general consensus among physicians that, regardless of age, it is better to wait for surgery until after complete breast development. However, in cases as just described where emotional disturbances are present because of the macromastia, surgery can reasonably be performed as early as after 1 to 2 years of stable breast size. This precaution is in place to decrease or prevent the risk of postoperative recurrence of excess breast tissue.
Additionally, in order to ensure proper treatment, it is important to identify the type of macromastia present in each patient, as certain types have a higher chance of recurrence and should be managed accordingly. Usually, adolescent patients have what is known as adolescent macromastia. In these cases, a reduction mammaplasty is a reasonable option once breast size has plateaued. However, there is a growing proportion of patients with BMI over 30 who have obesity-related breast hypertrophy. In these cases, patients should be strongly encouraged to lose weight, as doing so can often dramatically reduce breast size, which is not necessarily the case for other types of macromastia. Rarely, patients with juvenile gigantomastia will present for surgical evaluation. These patients have extreme cases of breast hypertrophy at a very young age and, due to the high rate of symptom recurrence, should be counseled on the increased likelihood of needing repeat reduction surgery. 8 , 23 , 24
Elderly Patients
Patients over the age of 65 occasionally present for breast reduction consultation; however, their issue is often more with breast ptosis than with actual macromastia. Additionally, they tend to be more motivated by symptom control than by aesthetic concerns. 1 In forming an operative plan in accordance with this, the physician must recall that the elderly patient population has significantly more comorbidities and, therefore, is at increased surgical risk. This risk includes not just wound healing but also increased risk with general anesthesia. As such, the preoperative evaluation of these patients should be coordinated with a PCP or medical specialist to order and review any necessary electrocardiograms (EKG), chest X-rays, or other screening exams. Approval from these consulting physicians should also be obtained in writing prior to scheduling of any elective surgery.
Patients need to be counseled on their individual risk of surgical complication to decide whether this outweighs the benefits of the procedure. Despite the need for this extended workup, physicians should remember that reduction mammaplasty and mastopexy can be safely performed in older patients with appropriate patient selection and collaboration from consulting physicians. 1 Elective breast surgery is, overall, considered a low-risk procedure with small chance for significant blood loss, and the elderly population should not be excluded from the documented benefits of surgery based on age alone. 1
7.2.6 Postradiation
Evaluating the postradiation patient for elective breast surgery can be a daunting task, since there is a reported complication rate of between 50 and 60% in this population. 25 , 26 It has been shown that the amount of radiation is directly proportional to risk for surgical complications such as delayed wound healing, nipple necrosis, and prolonged erythema. 27 Therefore, if surgery is attempted, it is important for the surgeon to be cautious intraoperatively; design flaps with shorter, wider pedicles; and avoid excessive undermining of flaps to give the tissue the best chance for survival. Additionally, the choice of pedicle may need to be based on the previous lumpectomy location, with the understanding that past surgery may have disrupted the normal blood flow, and therefore the lumpectomy site should, if possible, not be included in the pedicle. 27 In the event that a wound complication is encountered in the postoperative setting, physicians may consider ordering hyperbaric oxygen therapy, which has been shown to improve delayed wound healing in the irradiated patient. 28 Overall, as long as patients are educated on the risks of surgery on irradiated tissue, they should not be discouraged from undergoing reduction mammaplasty for symmetry or other cosmetic concerns.
Alternatively, as a way of avoiding additional surgery on irradiated tissue, some patients with a known existing breast malignancy who are undergoing lumpectomy may be offered the option of a simultaneous oncoplastic reduction at the time of mass resection. 29 Not only does this reduce the total number of operations, but it allows the reduction to be performed before any radiation treatment is begun, dramatically reducing the rate of wound healing complications. 30
7.2.7 Psychosocial Factors
Approximately 30% of patients who seek breast reduction surgery have a history of a psychiatric disorder that required some form of treatment. 31 Although most disorders are mild forms of anxiety or depression, identifying patients with a psychiatric history is important because patients with depression generally have unrealistic expectations and perceive their surgical outcomes as worse compared to the general population. 5 Even when patients do not have a diagnosed condition, those with poor coping mechanisms or poor support systems may not be good candidates for elective surgery. In these cases, surgery may not resolve their emotional distress, and an individual’s dissatisfaction about her breasts may just shift to another part of her body after surgery. 32
When assessing patients at their initial preoperative appointment, physicians should consider a complex psychiatric history or a history of multiple cosmetic procedures as indicators of a more complex emotional or psychological situation. However, in select cases, studies have shown that reduction mammaplasty may be considered as a possible way to significantly improve depression, anxiety, and low self-esteem in patients whose large breasts are the true source of their emotional distress. 31 , 32 In these patients, positive emotional results have shown to last for up to 5 years after surgery. 5
7.2.8 Physical Examination
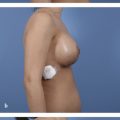
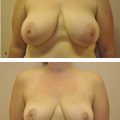
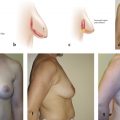
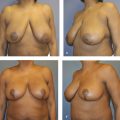
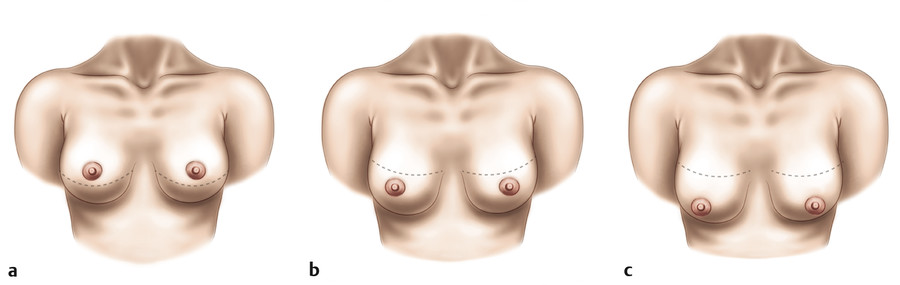
It is important to have a complete understanding of the patient’s preoperative breast aesthetics in order to plan for possible surgical intervention. Elements of the breast that should be examined include the preoperative breast size, the areolar diameter, the NAC position, and degree of nipple ptosis. Breast and nipple ptosis can be assessed by analyzing the NAC in relation to the inframammary fold (IMF). This technique was discussed in an early paper by Regnault in which breast ptosis was grouped into three broad categories. 33 He describes first-degree, or minor, ptosis as when “the nipple lies at the level of the submammary fold, above the lower contour of the gland and skin brassiere.” Second-degree, or moderate, ptosis occurs when “the nipple lies below the level of the fold but remains above the lower contour of the breast and skin brassiere.” Finally, third-degree, or major, ptosis is found when “the nipple lies below the fold level and at the lower contour of the breast and skin brassiere” (Fig. 7‑1). 33 , 34 Additionally, the physician should mention any preexisting asymmetry, for example, differences in shape, volume, or anatomy such as a constricted pole. Assessment of the breast skin should also be completed as part of the physical exam. The skin quality, the amount of skin excess, and the presence of scars that would interfere with pedicle design should all be noted. This is of particular importance for postbariatric patients, who typically have excessive skin laxity and deflated tissue (see Chapter 10). Additionally, the physician must palpate the entirety of the breast for any masses. 14 Finally, photographs of the patient in the anteroposterior (AP), oblique, and lateral views should be obtained. These images can then be used for the patient’s medical record, for preoperative planning, and for any required insurance documentation.
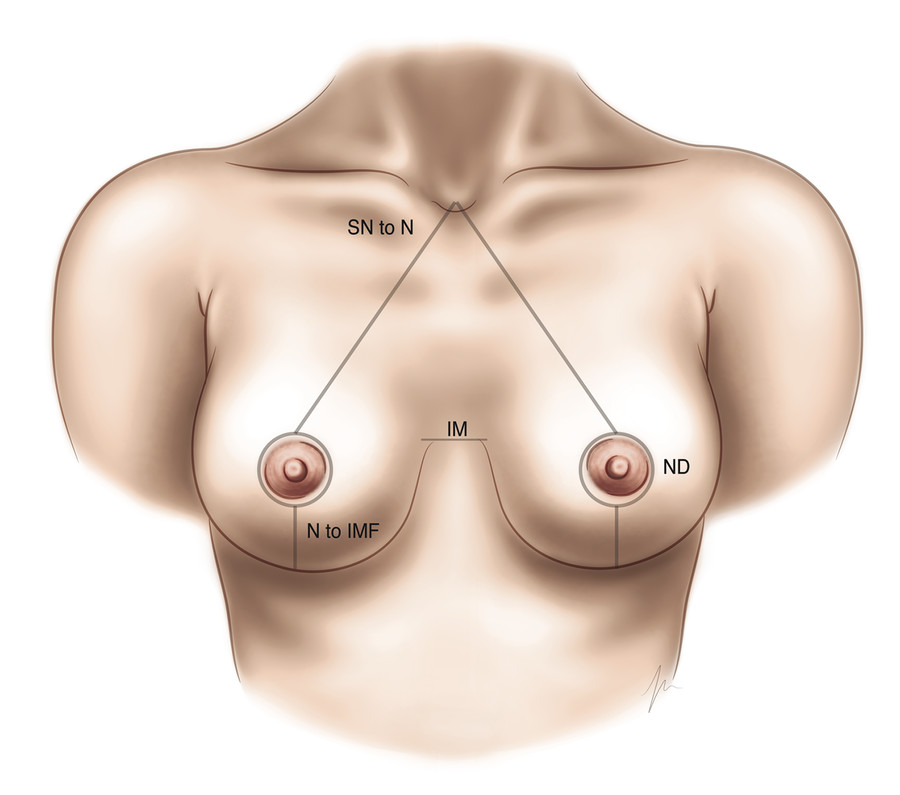
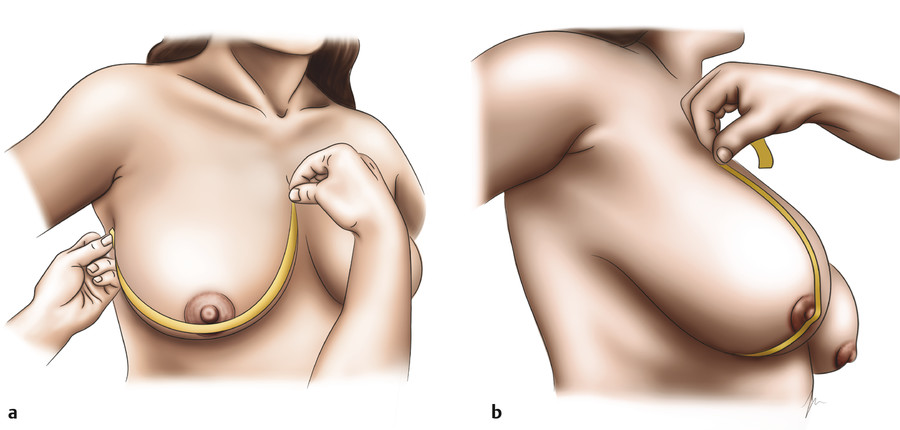
Some physicians advocate for recording specific breast surface measurements at the time of the preoperative appointment. Standard measurements that are often recorded include the sternal notch–to-nipple distance, the IMF-to-nipple distance, intermammary distance, and chest circumference. Additional measurements that have been proposed include orthogonal surface breast measurement (Fig. 7‑2). The horizontal breast distance is measured from the lateralmost aspect of the breast mound on the chest wall, over the nipple, to the medialmost aspect of the breast mound on the sternum. The vertical breast distance is recorded by measuring from the most cephalad point of the palpable breast tissue, over the nipple, to the IMF (Fig. 7‑3). 35 These measurements can be recorded not just for determination of the preoperative breast size and ptosis, but also to predict reduction mammaplasty resection weights, as discussed in Section 7.4, Preoperative Planning: Resection Weight and Size Goals. 35
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree