12 Reduction Mammaplasty
Summary
Reduction mammaplasty is one of the most rewarding procedures performed in plastic surgery, for both the patient and the surgeon. Patients express high satisfaction rates after reduction mammoplasty, and surgeons who perform this procedure can provide both aesthetic and functional improvements to the patient’s life. This chapter will focus on historical perspective, pertinent breast anatomy, breast physiology relevant to performing breast reduction at various ages, the history and physical exam, common techniques, and complications.
12.1 Introduction
Reduction mammaplasty is one of the most rewarding surgical procedures performed by plastic surgeons. Patients report high levels of satisfaction after reduction mammaplasty, with significant improvement in pain and lifestyle. 1 Most complications are minor and easily manageable. In this chapter, we will review the anatomy of the breast relevant to parenchymal resection patterns, considerations in the initial workup of a patient presenting for reduction mammaplasty, preoperative markings, skin resection patterns, pedicle options, variations in surgical technique, and common postoperative complications with associated management.
In these cases, there is an excess of skin, fat, and parenchyma, usually coupled with an overall breast shape that is less than ideal aesthetically. Patients with mammary hypertrophy can also present with a variety of symptoms. Typical complaints include neck and back pain, shoulder grooving from bra straps, inframammary intertrigo, and limited ability to exercise. Psychosocial issues surrounding excessively large breasts also exist, creating embarrassment for women, especially teenagers and elderly women. 2 Netscher et al encourage a focus on the constellation of symptoms of a patient rather than absolute volume as an arbitrary criteria for reduction mammaplasty. Further, their work shows that disease-specific group of physical and psychosocial complaints are more directly related to large breast size than to being generally overweight. 3 Kerrigan et al demonstrated the superiority of surgical intervention over conservative measures such as weight loss and special bras. 4 The main purpose of breast reduction is to improve the quality of life of the women who suffer from mammary hypertrophy. Blomqvist et al used a standardized quality of life questionnaire to demonstrate the long lasting positive impact on women’s quality of life. 5 In addition to improvement in quality of life, creation of an aesthetically pleasing breast is clearly an important consideration as well. Spear may have put it best when he said that breast reduction represents “the clearest example of the interface between reconstructive plastic surgery and aesthetic plastic surgery.” 2
12.2 History of the Practice
One of the first cases of reduction mammaplasty was reported by Dieffenbach in 1848, who reduced the lower two-thirds of the breast via an inframammary fold (IMF) incision. 6 Over the next century there were many approaches to reducing breast tissue and correcting ptosis. Schwarzmann suggested that the perfusion and viability of the nipple areolar complex (NAC) could be improved by maintaining a ring of dermis around it, allowing more reliable transposition. 7 Penn in 1955 noted that sternal notch–to-nipple distances should be 21 cm and the nipple-to-nipple distance should be the same, to form an equilateral triangle. 8 Wise reported his keyhole pattern of skin resection in 1956. 9 Ultimately resulting in an inverted-T scar, the Wise pattern of breast reduction remains one of the most reliable and popular breast reduction techniques to this day.
Subsequent decades have seen continued evolution of techniques involving choice of blood supply and skin resection and scar patterns. Pitanguy and Weiner described the superiorly based dermoglandular pedicle in 1973. 10 Orlando and Guthrie devised the technique of the superomedial dermoglandular pedicle shortly thereafter in 1975. 11 McKissock described a vertical bipedicle technique. 12 Claude Lassus developed his technique in 1970 using a vertical scar. 13 Many other plastic surgeons around the world further developed short-scar, superior pedicle techniques for reduction mammoplasty in the 1980s and 1990s, including Lejour, Marchac, Peixoto, Sampaio Góes, and Benelli. 14 , 15 , 16 , 17 , 18 , 19 Techniques to avert the vertical scar, such as the technique of Passot, have been refined by various authors in the 1990s and 2000s, including Lalonde, Matloub, and Pribaz. 20 , 21 , 22 Hammond’s short-scar periareolar inferior pedicle reduction (SPAIR) technique for breast reduction combines a short-scar skin resection with an inferior pedicle, in contrast to most other short-scar techniques, which implement a superior or superomedial pedicle. 23 Hall-Findlay describes a medial pedicle technique with minimal skin undermining. 24 The overall goal of these techniques is to fight the tendency to bottom out while reducing overall scar burden.
12.3 Anatomy
In reviewing the anatomy of the breast relevant to reduction mammaplasty, this section will focus particularly on blood supply. The parenchymal resection pattern is less important in planning the operation than focusing on the parenchymal pattern that is left behind and what pedicle remains to provide robust blood supply to this residual breast tissue. In particular, the NAC not only is a key aesthetic landmark of the breast but unfortunately is also the tissue the farthest away from any given pedicle and thus most prone to necrosis in case of vascular insufficiency.
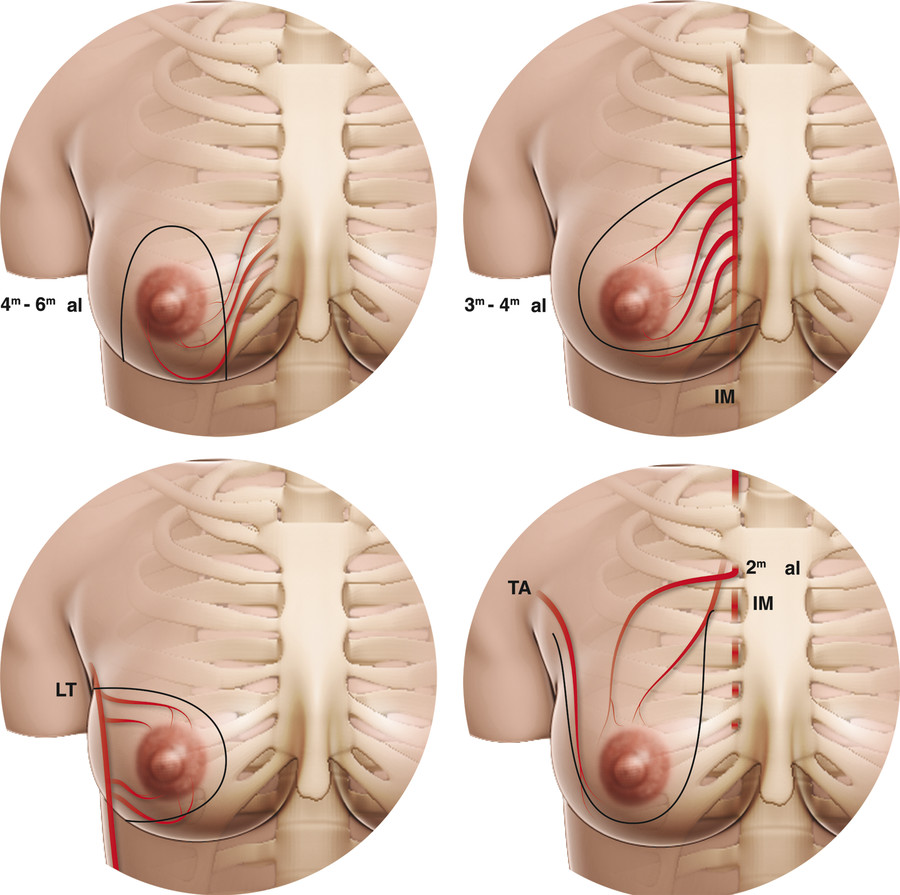
The landmarks of the breast commonly referred to in oncologic surgery include the latissimus dorsi muscle laterally, the clavicle superiorly, the sternum medially, and the inframammary fold (IMF) inferiorly. Given the rich, overlapping vascular network to the breast, it is possible to design a pedicle from virtually any direction. There are four major arterial networks supplying the breast: the internal mammary medially, the lateral thoracic laterally, the thoracoacromial superiorly, and the intercostal perforators arising both medially and laterally (Fig. 12‑1). The NAC is supplied by both glandular perforators and the subdermal plexus; hence the importance of leaving dermis behind when de-epithelializing around the NAC. The skin is supplied only by the subdermal plexus, likewise pointing to the importance of leaving thick skin flaps. Venous drainage occurs primarily via the axillary vein but also via internal mammary and intercostal veins. There can be considerable anatomic variability between breasts, and our understanding of these variations is still evolving. 25
12.4 Physiology
Mammary hypertrophy is primarily the result of an abnormal sensitivity of the breast to circulating estrogens, causing breast proliferation that is predominantly adipose and connective tissue rather than glandular parenchyma. Most women with mammary hypertrophy have normal levels of serum estrogen as well as normal amounts of estrogen receptors in the breast tissue. 26 , 27
Cases of true juvenile virginal hypertrophy of the breast can present in the age range of 11–14 years. 27 Durston reported the first case of juvenile virginal breast hypertrophy in 1670. The woman in his case report died at age 24 and was found to have a 64-pound (29-kg) right breast with no evidence of disease. 28 Recurrence in these patients is common, and they should be counseled for the likely need for secondary reduction mammaplasty. 29
12.5 Patient History and Physical Exam
Preoperative evaluation of the patient presenting for reduction mammaplasty should focus on symptoms caused by the macromastia and any medical comorbidities that may impair wound healing or otherwise increase surgical risk. For insurance to cover reduction mammaplasty, certain symptoms not amenable to medical management should be documented. 30 These include chronic back pain requiring the use of pain medications, bra strap grooves in the shoulders, nerve pain, breast pain, intertrigo or rash within the IMFs, and restriction of physical activities. While not always necessary, a history of attempted weight loss with diet control and exercise shows patient motivation and failure of nonsurgical management. It is important to inquire whether the patient has a history of gastric bypass surgery or is considering weight loss surgery, as this may affect breast volume. If a patient is planning to undergo weight loss surgery then reduction mammaplasty may be better delayed until 6 months to 1 year after the patient’s weight is stable and there is less risk of nutritional deficiencies that may impair wound healing.
Other comorbidities that are important to ask about include anything that would impair wound healing, such as diabetes or history of immunosuppression; anything that may increase risks associated with general anesthesia, such as significant cardiac or pulmonary history; and anything that may increase risk of postoperative complications, such as hypertension and coagulopathies.
While a physical exam is helpful to get a sense of the volume of breast tissue the patient would like removed, it is important to counsel the patient that it is impossible to give her an exact bra size she will be postoperatively. That will depend on how much breast tissue is removed in the operation, but it may also change somewhat as postoperative swelling goes down. Additionally, bra size is not standardized across retailers. The patient’s height, weight, and body habitus are often mandatory for insurers to calculate the amount of breast tissue they require for the reduction procedure to be covered. This amount can vary from insurer to insurer. Some insurers use an absolute mass based on the patient’s height. Others use calculations involving the patient’s height and weight, such as the Schnur sliding scale, to approve or reject patients’ insurance claims for breast reduction. Schnur et al developed this scale in 1991 after analyzing surveys of plastic surgeons. 31 In their study, women whose removed breast weight was under the fifth percentile sought the procedure for cosmetic reasons, while women whose resected breast weight was above the 22nd percentile reported medical reasons. Many U.S. health insurers approve only patients whose predicted resected weights fall above the 22nd percentile based on the Schnur scale. 32 Most plastic surgeons agree that such a formulaic approach is flawed and that greater emphasis should be placed on individual patient characteristics and symptomatic considerations.
As part of the physical exam, it is also helpful to show the markings of where the final scars will be on the breast, as most patients are not aware of the scarring to be expected afterward. The degree of ptosis can be noted, and the patient should be shown where to expect the new nipple position. Body mass index (BMI) should also be documented as part of the physical exam. The risk of postoperative complications increases with increasing weight of breast resection and increasing BMI. 33 , 34
Finally, it is important to document any family history of breast cancer. While American College of Surgeons and the American Cancer Society recommend screening mammograms starting at age 40, the United States Preventative Task Force recommends screening mammograms starting at age 50. 35 Most plastic surgeons will order a preoperative screening mammogram in any patients aged 40 or greater. In patients with a significant family history of breast cancer or BRCA-positivity, it may be reasonable to order a screening mammogram even in patients less than 40 years old.
12.6 Operative Technique
12.6.1 Preoperative Markings
The preoperative breast markings are perhaps the most important step of the operation. These markings help ensure symmetry between the breasts and guide the surgeon once anatomic landmarks get displaced as the patient lies supine on the operating table. Additionally, these markings help remind the patient of the scars to expect postoperatively so that there are no surprises afterward.
The breast markings should be made with the patient in the upright position. Ensure that the patient’s shoulders are relaxed, she is not leaning to one side or the other, and her legs are not crossed. First, mark the sternal notch (1 in Fig. 12‑2). From there, mark the midline of the chest down the sternum (2 in Fig. 12‑2). Next, mark the meridian of each breast extending from approximately the junction of the medial and middle thirds of the clavicle down through the nipple, typically 6–8 cm from the midline (3 in Fig. 12‑2). This breast meridian will help to determine placement of the new nipple position. Next, mark the IMF (4 in Fig. 12‑2). This can be done by gently raising the breast with the back of your nondominant hand and allowing the marking pen to fall gently into the crease between breast and upper abdominal wall. Once the IMF is marked, the new position of the nipple is ready to be placed. This can be done by placing your four fingers of your nondominant hand into the IMF and using your thumb to mark where this position translates onto the top of the breast. This is called Pitanguy’s point, and the new nipple position will lie approximately at the intersection of the IMF translation onto the breast and the line created previously by the breast meridian (5 in Fig. 12‑2). The final markings are to be placed around the new nipple position and depend on the skin resection pattern that has been decided upon. The most traditional and common, the Wise pattern, consists of both vertical and horizontal limbs of skin resection. These can be extended from a preset keyhole pattern that is marked using a template. The round part of the keyhole template marks the new position of the areola and is centered around the new nipple position. Oblique limbs extending from the round part of the keyhole mark the vertical skin resection pattern. From these limbs, horizontal extensions should be marked that meet at either end of the previously marked IMF to create the horizontal skin resection pattern. Alternatively, instead of using the preset keyhole pattern, the surgeon can mark an equilateral triangle with its superior point at the position of the new nipple. The limbs of the triangle should range between 7 and 10 cm, and these limbs extending obliquely will be the vertical skin resection pattern (6 in Fig. 12‑2). Again, from these limbs, markings can be extended horizontally to connect to each end of the IMF marking to create the horizontal skin resection pattern (7 in Fig. 12‑2). The new areolar position is then decided upon in the operating room after the reduction is complete and is marked with a cookie cutter at that time.
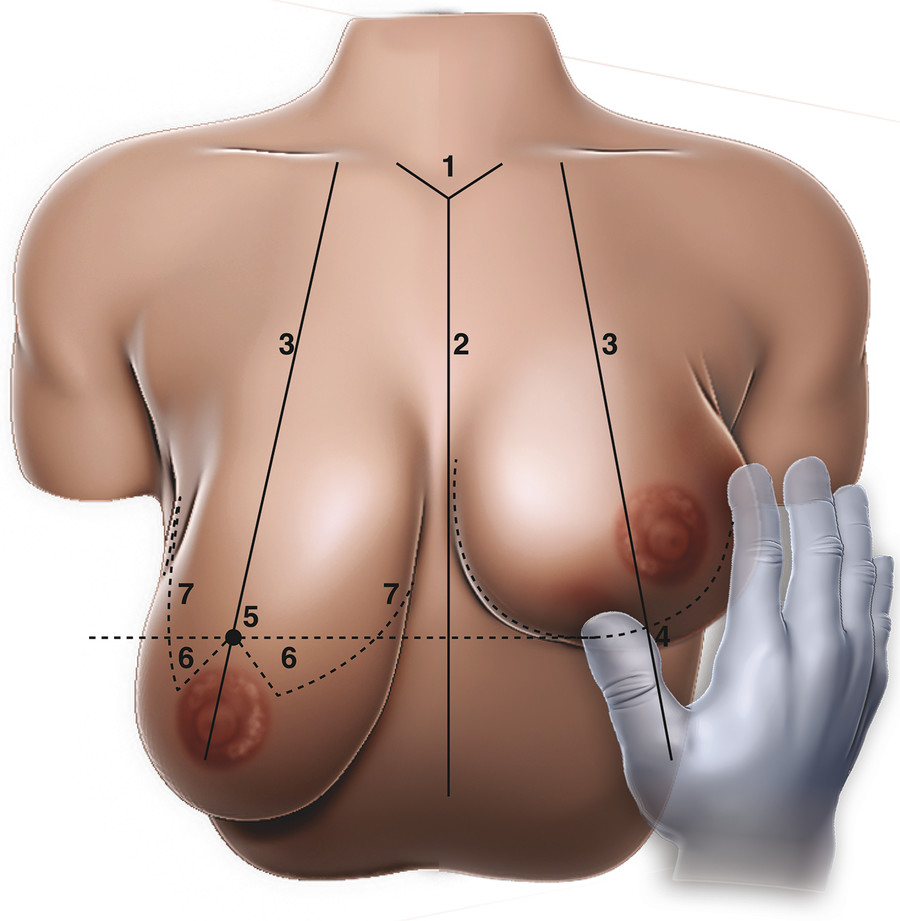
Finally, the pedicle itself can be outlined as markings on the breast. The base of the pedicle should be approximately 8–10 cm. This base can be measured on the breast and the pedicle subsequently outlined.
If an alternative pattern of skin resection is chosen, such as a vertical skin reduction mammaplasty or a periareolar skin reduction mammaplasty, then these markings will need to be modified accordingly to reflect the skin resection pattern.
12.6.2 Skin Resection Patterns
Various skin resection patterns exist for tightening the skin envelope over the reduced breast. Commonly used patterns include the Wise pattern (inverted T), vertical only, short-scar periareolar, and no-vertical-scar (Fig. 12‑3).
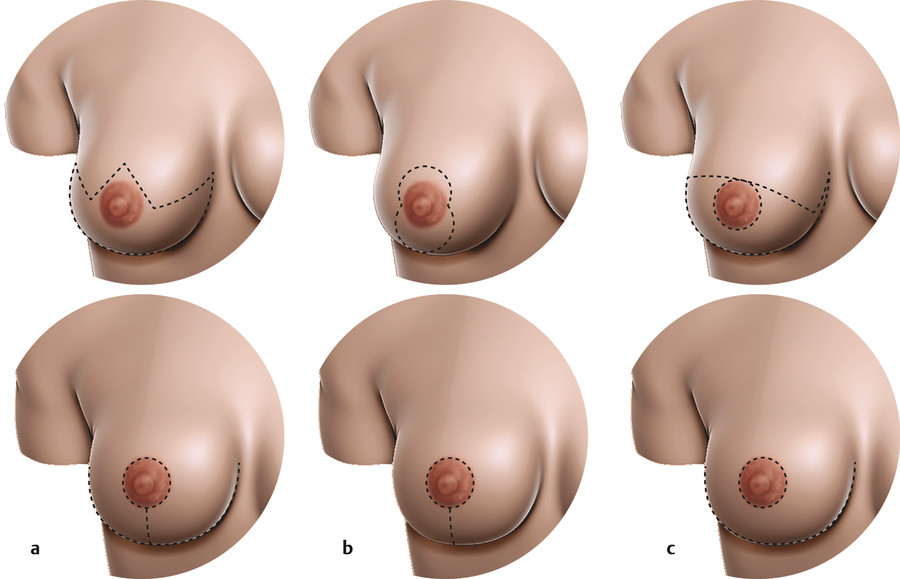
The Wise pattern is probably the most common (Fig. 12‑3a). This is frequently performed in conjunction with an inferior pedicle. The Wise pattern can be marked out either using a Mosque template, which resembles a keyhole pattern, to mark out the new NAC, or with a simple equilateral triangle whose side lengths will become the new nipple-to-IMF distance. With the former, it is important not to place the new nipple position too high, as this is very difficult to correct. With the latter, the nipple position is chosen intraoperatively after the skin flaps have been closed.
The vertical-scar-only incision is best used in smaller breast reductions (Fig. 12‑3b). The incision resembles a snowman, with a periareolar incision and a larger ellipse inferior to this. It is important with this incision pattern to keep the lower border of the elliptical incision at least 2 cm above the IMF. Once the ellipse is closed, the incision will lengthen and can potentially fall below the IMF if placed too close.
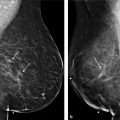
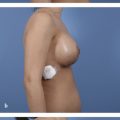
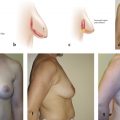
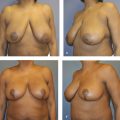
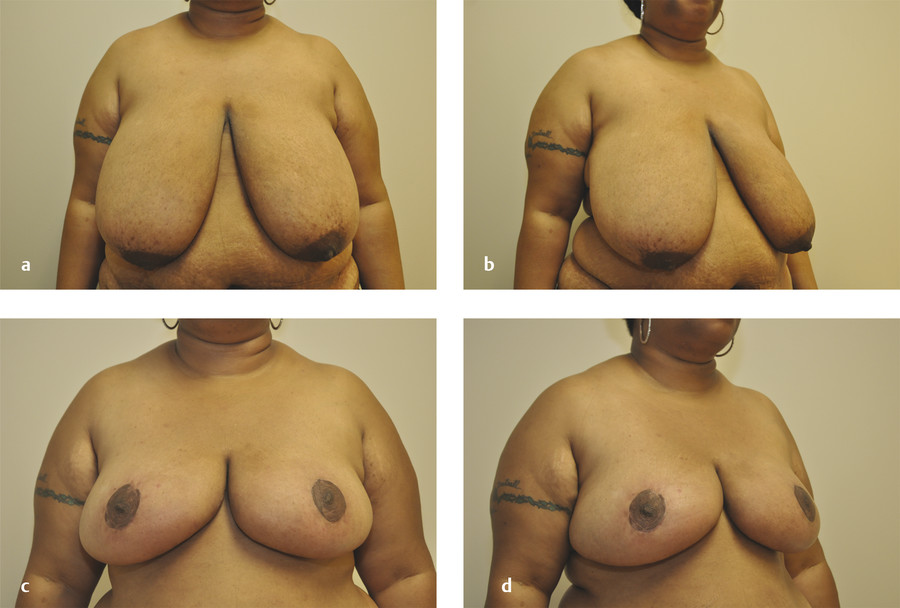
The no-vertical-scar technique utilizes both a periareolar skin excision and a separate IMF excision (Fig. 12‑3c). The breast skin flaps act as an apron that is then pulled down and over the breast parenchyma after resection. With this technique, it is imperative not to overresect skin from the IMF excision. Ideally, the excision width should not exceed 7 cm; otherwise, one risks not being able to close the skin over the breast parenchyma. See Fig. 12‑4 for an example of a no-vertical-scar breast reduction.
12.6.3 Pedicle Options
Pedicle selection should be based on the surgeon’s understanding of the most reliable blood supply to the NAC as well as considerations involving long-term maintenance of superior pole projection. Most proponents of the superior or superomedial pedicle techniques will argue that retaining the more cephalic breast tissue encourages long-term maintenance of superior pole fullness while ameliorating the phenomemon of pseudoptosis or “bottoming out.” Proponents of the inferior pedicle will point out that, particularly in a more ptotic breast, this is likely to be the most reliable blood supply to the NAC. Superior or superomedial pedicles tend to be associated with short-scar or vertical-scar techniques as an additional consideration of pedicle selection. If a short or vertical scar is being utilized, the decision between a superior or medial pedicle will typically be determined by the position of the NAC relative to the planned location of the new areola. As this is marked preoperatively in the mosque or keyhole pattern, assessment can be made as to whether the NAC will translate easily into its final position with a simple vertical advancement or whether more significant ptosis would benefit from the 90° rotation associated with a medial pedicle to allow the areola to rotate into its final, more cephalic position.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree