Vascular Dermatoses
John C. Hall MD
Urticaria, erythema multiforme and its variants, and erythema nodosum are included under the heading of vascular dermatoses because of their vascular reaction patterns. Stasis dermatitis is included because it is a dermatosis owing to venous insufficiency in the legs. Vasculitis is due to inflammation on the arterial side of the vascular tree in small or large vessels. Pigmented purpura is due to microvascular capillary leakage of red blood cells and hence hemosiderin staining in a prone patient. It is called a benign hemosiderosis in contrast to the “malignant” type of hemosiderosis seen in hemochromatosis, where internal organs (especially the liver) may be involved. Pyoderma gangrenosum is an ulcerative inflammatory disease, mainly of the lower extremities. Cutaneous necrosis is end-stage vascular compromise with gangrenous disease.
Urticaria
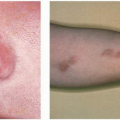
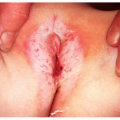
The commonly (10% to 25% of population at some time in life) seen entity of urticaria (Fig. 12-1), or hives, can be acute or chronic and due to known or unknown causes. Numerous factors, both immunologic and nonimmunologic, can be involved in its pathogenesis. The urticarial wheal results from liberation of histamine from tissue mast cells and from circulating basophils.
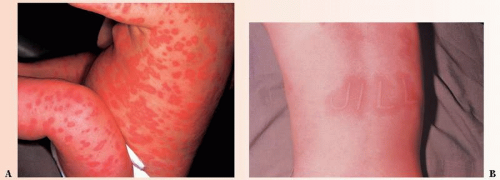 FIGURE 12-1 ▪ (A) Acute urticaria from penicillin in a 6-month-old child. (B) Dermographism on flexor wrist. (Courtesy of Dermik Laboratories, Inc.) |
Nonimmunologic factors that can release histamine from these cells include
chemicals,
various drugs (including morphine and codeine),
ingestion of fish (especially shellfish), nuts (especially peanuts), and other foods,
bacterial toxins, and
physical agents.
An example of the type of wheal caused by physical agents is the linear wheal produced by light stroking of the skin, known as dermographism. (Consult the Dictionary-Index at the end of the book for the triple response of Lewis reaction.)
Immunologic mechanisms are probably involved more often in acute than in chronic urticaria. The most commonly considered of these mechanisms is the type I hypersensitivity state, which is triggered by polyvalent antigen bridging that involves two specific immunoglobulin (Ig) E molecules that are bound to the mast cell or basophil surface (see Chapter 9).
Lesions
Pea-sized red papules to large circinate patterns with red borders and white centers that can cover an entire side of the trunk or the thigh may be noted. Vesicles and bullae are seen in severe cases, along with hemorrhagic effusions. A severe
form of urticaria is labeled angioedema. It can involve an entire body part, such as the lip or the hand. Edema of the glottis and bronchospasm are serious complications and are true medical emergencies.
form of urticaria is labeled angioedema. It can involve an entire body part, such as the lip or the hand. Edema of the glottis and bronchospasm are serious complications and are true medical emergencies.
Presentation and Characteristics
Course
Acute cases may be mild or explosive but usually disappear with or without treatment in a few hours or days. The chronic form has remissions and exacerbations for months or years. One definition of chronic urticaria is one episode at least twice weekly for 6 weeks.
Causes
After careful questioning and investigation, many cases of hives, particularly of the chronic type, are concluded to result from no apparent causative agent. Other cases, mainly the acute ones, have been found to result from the following factors or agents:
Drugs or chemicals: Penicillin and derivatives are probably the most common causes of acute hives, but any other drug, whether ingested, injected, inhaled, or, rarely, applied on the skin, can cause the reaction (see Chapter 8).
Foods: Foods are a common cause of acute hives. The main offenders are seafood, nuts, chocolate, strawberries, cheeses, pork, eggs, wheat, and milk. Chronic hives can be caused by traces of penicillin in milk products (Fig. 12-1A).
Insect bites and stings: Insect bites, stings from mosquitoes, fleas, or spiders, and contact with certain moths, leeches, and jellyfish may cause hives.
Physical agents: Hives can result from heat, cold, radiant energy vibration, water, and physical injury. Dermographism is a term applied to a localized urticarial wheal produced by scratching the skin in certain people (Fig. 12-1B).
Inhalants: Nasal sprays, insect sprays, dust, feathers, pollens, and animal dander are some common offenders.
Infections: A focus of infection is always considered, sooner or later, in chronic cases of hives, and in unusual instances it is causative. The sinuses, teeth, tonsils, gallbladder, and genitourinary tract should be checked.
Internal disease: Urticaria has been seen with liver disease, intestinal parasites, cancer, rheumatic fever, lupus erythematosus, vitiligo, pernicious anemia, rheumatoid arthritis, and others.
“Nerves”: After all other causes of chronic urticaria have been ruled out, there remain a substantial number of cases that appear to be related to nervous stress, worry, or fatigue. These cases benefit most from the establishment of good rapport between the patient and the physician.
Contact urticaria syndrome: This uncommon response can be incited by local contact on the skin of drugs and chemicals, foods, insects, animal hair or dander, and plants.
Cholinergic urticaria: Clinically, small papular welts are seen that are caused by heat (hot bath), stress, or strenuous exercise.
SAUER’S NOTE
Dermographism is commonly overlooked as a cause of the patient’s “welts” or vague itching.
Differential Diagnosis
Erythema multiforme: Systemic fever, malaise, and mouth lesions are noted in children and young adults (see the next section of this chapter).
Dermographism: A common finding in young adults, especially those who present complaining of welts on their skin or vague itching of the skin with no residual lesions. To make the diagnosis, stroke the skin firmly to see if an urticarial response develops. The course can be chronic, but hydroxyzine, 10 mg b.i.d. or t.i.d., is quite helpful. (Warn the patient about the possibility of drowsiness.) Nonsedating antihistamines can also be tried.
Urticarial vasculitis: Lesions may last more than 24 hours, may be painful, leave a bruise or hyperpigmentation, and be associated with hypocomplementemia and systemic lupus erythematosus. Skin biopsy is confirmatory.
Treatment
Case Example: A patient presents for a case of acute hives due to penicillin injection 1 week previously for a “cold.”
1. Colloidal bath
Sig: Add 1 cup of starch or oatmeal (Aveeno) to 6 to 8 in of lukewarm water in the tub. Bathe for 15 minutes once or twice a day.
2. Sarna lotion, Aveeno Anti-itch lotion, or PrameGel or any pramoxine-containing topical over the counter (OTC).
Sig: Apply PRN locally for itching.
3. Hydroxyzine (Atarax), 10 mg #30
Sig: Take 1 tablet t.i.d., a.c. (warn of drowsiness).
4. Diphenhydramine (Benadryl), 50 mg
Comment: Available OTC
5. Nonsedating antihistamines can also be used.
6. Betamethasone sodium phosphate (6 mgms/cc Celstone Soluspan), 3 mg/cc
Sig: Inject 1 to 1.5 cc intramuscularly.
For a more severe case of acute hives:
1. Diphenhydramine injection
Sig: Inject 2 mL (20 mg) subcutaneously, or
2. Epinephrine hydrochloride
Sig: Inject 0.3 to 0.5 mL of 1:1,000 solution subcutaneously, or
3. Prednisone tablets, 10 mg #30
Sig: Take 5 tablets every 2 days and decrease by 1 tablet every 2 days for a 10-day course.
For treatment of a patient with chronic hives of 6 months’ duration when cause is undetermined after careful history and examination:
1. Hydroxyzine (Atarax), 10 to 25 mg #60
Sig: Take 1 tablet t.i.d. depending on drowsiness and effectiveness. Continue for weeks or months.
Clemastine (Tavist) 1.34 or 2.68 mg #30
Sig: Take 1 tablet b.i.d., available OTC.
Cyproheptadine (Periactin) 4 mg #60
Sig: One tablet by mouth t.i.d.
2. Loratadine (Claritin) now OTC 10 mg #30
Sig: Take 1 tablet once a day.
Cetirizine (Zyrtec) 5 mg or 10 mg #30
Sig: Take 1 tablet once a day.
Fexofenadine (Allegra), 60 mg or 180 mg #30
Sig: Take 1 tablet once a day.
3. Cimetidine (Tagamet), 300 mg #60
Sig: Take 1 tablet t.i.d. (200 mg, 400 mg, or 800 mg).
Comment: This H2 blocker is of benefit in some cases and can be added to H1 blockers.
4. Suggest avoidance of seafood, nuts, chocolate, cheese and other milk products, strawberries, pork, excessively spicy foods, and excess of coffee or tea.
5. Keep a diet diary of everything ingested (including all foods, all medicines, even OTC, candy, menthol cigarettes, chewing gum, chewing tobacco, mouthwash, breath fresheners) and then see what items were used 12 to 24 hours before the episode of hives occurred.
6. A mild sedative or tranquilizer such as meprobamate, 400 mg t.i.d., or chlordiazepoxide (Librium), 5 mg t.i.d., may help.
7. Doxepin (Sinequan) 10 mg #60
Sig: 1 tablet t.i.d.
Comment: This is a tricyclic antidepressant with potent antihistaminic properties. It can cause drowsiness, dry mouth, and other side effects of this classification of drugs.
8. Immunosuppressive drugs such as prednisone are unfortunately necessary in severe cases.
9. Zaditor (ketotifen fumarate) is a mast-cell stabilizer with benefits in severe cases, but I have not used this drug.
10. Sulfasalazine (500 mg increased up to 4,000 mg by increasing by 500 mg each week) has been reported in chronic idiopathic urticaria to be a steroid-sparing or steroid-replacing drug in one report.
Erythema Multiforme
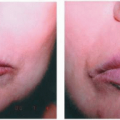
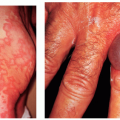
The term erythema multiforme introduces a flurry of confusion in the mind of any student of medicine. It is our purpose in this section to attempt to dispel that confusion. Erythema multiforme, as originally described by Hebra, is an uncommon, distinct disease of unknown cause characterized by red iris-shaped or bull’s eye-like macules, papules, or bullae confined mainly to the extremities, the face, and the lips (Fig. 12-2). It can be accompanied by mild fever, malaise, and arthralgia. It occurs usually in children and young adults in the spring and the fall, has a duration of 2 to 4 weeks, and frequently is recurrent for several years.
The only relation between Hebra’s erythema multiforme and the following diseases or syndromes is the clinical appearance of the eruption.
Stevens-Johnson syndrome is a severe and rarely fatal variant of erythema multiforme. It is characterized by high fever, extensive purpura, bullae, ulcers of the mucous membranes, and, after 2 to 3 days, ulcers of the skin. Eye involvement can result in blindness. It can be related to drugs and its severest form is considered by some to be the same as toxic epidermal necrolysis (see Chapter 18).
Erythema multiforme bullosum is a severe, chronic, bullous disease of adults (see Chapter 18). There is an opinion that this syndrome is completely separate from erythema multiforme. More macular truncal lesions and more epidermal necrosis and less infiltrate may be seen in Stevens-Johnson syndrome (toxic epidermal necrolysis). Sulfonamides, anticonvulsant agents, allopurinol, chlormezanone, and nonsteroidal anti-inflammatory drugs commonly cause erythema multiforme bullosum.
Erythema multiforme-like drug eruption is frequently due to phenacetin, quinine, penicillin, mercury, arsenic, phenylbutazone, barbiturates, trimethadione, phenytoin, sulfonamides, and antitoxins (see Chapter 8).
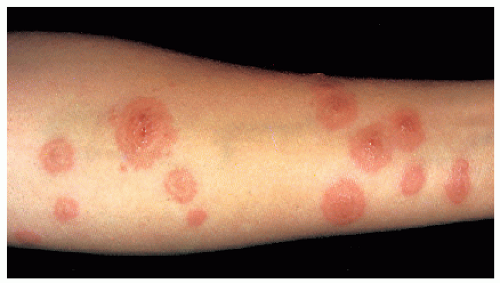 FIGURE 12-2 ▪ Erythema multiforme-like eruption on the arm during pregnancy. (Courtesy of Dermik Laboratories, Inc.) |
Differential Diagnosis
The erythema perstans group, or figurate erythemas, includes over a dozen clinical entities with impossible-to-remember names. (See Dictionary-Index under erythema perstans.) All have various-sized erythematous patches, papules, or plaques with a definite red border and a less active center, forming circles, half circles, groups of circles, and linear bands. Multiple causes have been ascribed, including tick bites; allergic reactions; fungal, bacterial, viral, and spirochetal infections; and internal cancer. The duration of and the response to therapy vary with each individual case.
Erythema chronicum migrans is the distinctive cutaneous eruption of the multisystem tick-borne spirochetosis Lyme disease. The deer tick, Ixodes dammini, is the vector for this spirochete. Early therapy with doxycycline or ampicillin may prevent late manifestations of the disease (see Chapter 22).
Reiter’s syndrome is the triad of conjunctivitis, urethritis, and, most important, arthritis, that occurs predominantly in men and lasts about 6 months. The skin manifestations consist of psoriasiform dermatitis, which is called balanitis circinata on the penis and keratoderma blennorrhagica on the palms and soles.
Behçet’s syndrome consists of the triad of genital, oral, and ophthalmic ulcerations seen most commonly in men; it can last for years, with recurrences. Other manifestations include cutaneous pustular vasculitis, synovitis, and meningoencephalitis. It is more prevalent in eastern Mediterranean countries and Japan. Skin hypersensitivity to trauma or pathergy is observed with sterile pustular formation 24 to 48 hours after an intradermal needle prick.
Urticaria: Clinically, urticaria may resemble erythema multiforme, but hives are associated with only mild systemic symptoms. It can occur in any age group; iris lesions are unusual. Usually, it can be attributed to penicillin or other drug therapy, and it responds rapidly but often not completely to antihistamine therapy (see first part of this chapter). It is evanescent and dissipates or moves to a new area in less than 24 hours.
Treatment
Case Example: A 12-year-old boy presents with bull’s eyelike lesions on his hands, arms, and feet, erosions of the lips and mucous membranes of the mouth, malaise, and a temperature of 101°F (38.3°C) orally. He had a similar eruption last spring.
1. Order bed rest and increased oral fluid intake.
2. Acetaminophen (Tylenol), 325 mg OTC
Sig: Take 1 to 2 tablets q.i.d., or Prednisone, 10 mg #16
Sig: Take 2 tablets stat and then 2 tablets every morning for 7 days.
3. For severe cases, such as the Stevens-Johnson form, hospitalization is indicated, where intravenous corticosteroid therapy (debatable), intravenous fluid replacement infusions, immunoglobulin, and other supportive measures can be administered.
Erythema Nodosum
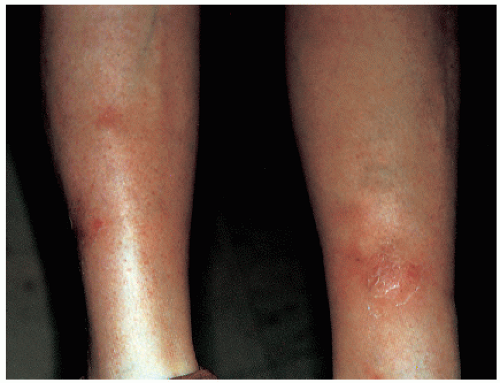
Erythema nodosum is an uncommon reaction pattern seen mainly on the anterior tibial areas of the legs (Fig. 12-3). It appears as erythematous nodules in successive crops and is preceded by fever, malaise, and arthralgia.
Presentation and Characteristics
Primary Lesions
Bilateral, red, tender, rather well-circumscribed nodules are seen mainly on the pretibial surface of the legs and, rarely, on the arms and the body. Later, the flat, indurated lesions may become raised, confluent, and purpuric. Only a few lesions develop at one time.
Secondary Lesions
The lesions never suppurate or form ulcers but can heal with a bruise.
Course
The lesions last several weeks, but the duration can be affected by therapy directed to the cause, if it is known. Relapses are related to the cause. The lesions can be idiopathic and have a chronic course.
Causes
Careful clinical and laboratory examinations are necessary to determine the cause of this toxic reaction pattern. The following tests should be performed:
Complete blood cell count
Erythrocyte sedimentation rate
Urinalysis
Strep screen, serum pregnancy test, angiotensinconverting enzyme, tuberculin skin test
Serologic test for syphilis
Chest x-ray
Specific skin tests, as indicated
The causes of erythema nodosum are
Streptococcal infection (rheumatic fever, pharyngitis, scarlet fever, arthritis)
Fungal infection (coccidioidomycosis, trichophyton infection)
Pregnancy or oral contraceptives
Sarcoidosis
Lymphogranuloma venereum
Syphilis
Chancroid
Drugs (contraceptive pills, sulfonamides, iodides, bromides, echinacea herbal therapy)
Hepatitis C
HIV infection
Celiac disease
Carcinoid syndrome
Tuberculosis
It is rare in children, but when it occurs, group A β-hemolytic streptococcal infection (which may be occult) is the most common cause. Oral contraceptives are a common cause in adult women. It is not uncommon to be unable to find a cause.
Age and Gender Incidence
The disorder occurs predominantly in adolescent girls and young women.
Laboratory Findings
Histopathologic examination reveals a nonspecific but characteristically localized inflammatory infiltrate in the subcutaneous tissue and in and around the veins.
Differential Diagnosis
Erythema induratum: Chronic vasculitis of young women that occurs on the posterior calf area and often suppurates; biopsy shows a tuberculoid-type infiltrate, usually with caseation. A tuberculous causation has been suggested.
Necrobiosis lipoidica diabeticorum: A cutaneous manifestation of diabetes mellitus, characterized by well-defined patches of reddish-yellow atrophic skin, often with overlying telangiectasias primarily on anterior areas of the legs. The lesions can ulcerate; biopsy results are characteristic, but biopsy may not be indicated because of the possibility of poor healing and the characteristic clinical presentation (see Chapter 38).
Periarteritis nodosa: A rare, sometimes fatal, arteritis that most often occurs in men. Twenty-five percent of patients show painful subcutaneous nodules and purpura, mainly of the lower extremities, which often show livedo reticularis. It is a multiorgan system disease; renal failure is often a component. There is a cutaneous variety. (+) p-ANCA blood test is needed for diagnosis.
Superficial thrombophlebitis migrans (Buerger’s disease): An early venous change of Buerger’s disease commonly seen in male patients, with painful nodules of the anterior tibial area. Biopsy is of value. Smoking has been suggested as an important contributing factor.
Nodular panniculitis or Weber-Christian disease: Occurs mainly in obese middle-aged women. Tender, indurated, subcutaneous nodules and plaques are seen, usually on the thighs and the buttocks. Each crop is preceded by fever and malaise. Residual atrophy and hyperpigmentation occur.
Leukocytoclastic vasculitis: Includes a constellation of diseases, such as allergic angiitis, allergic vasculitis, necrotizing vasculitis, and cutaneous systemic vasculitis. Clinically, palpable purpuric lesions are seen, most commonly on the lower part of the legs. In later stages, the lesions may become nodular, bullous, infarctive, and ulcerative. Various etiologic agents have been implicated, such as infection, drugs, and foreign proteins. Treatment includes bed rest, pentoxifylline (Trental), corticosteroids, and other immunosuppressive drugs (see Chapter 9).
For completeness, the following five rare syndromes with inflammatory nodules of the legs are defined in the Dictionary-Index:
1. Subcutaneous fat necrosis with pancreatic disease
2. Migratory panniculitis
3. Allergic granulomatosis
4. Necrobiotic granulomatosis
5. Embolic nodules from several sources
Treatment
1. Treat the cause, if possible.
2. Rest, local heat, and aspirin are valuable. The eruption is self-limited if the cause can be eliminated.
3. Chronic cases can be disabling enough to warrant a short course of corticosteroid therapy. Some cases have benefited from naproxen (Naprosyn), 250 mg b.i.d. (or other nonsteroidal anti-inflammatory drugs), for 2 to 4 weeks.
Stasis (Venous) Dermatitis and Ulcers
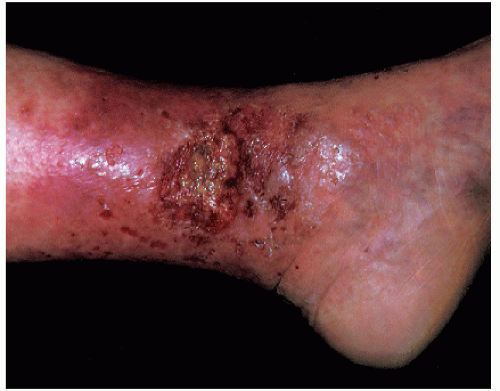
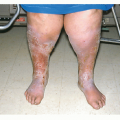
Stasis dermatitis is a common condition owing to impaired venous circulation in the legs of older patients (Fig. 12-4). Almost all cases are associated with varicose veins, and because the tendency to develop varicosities is a familial characteristic, stasis dermatitis is also familial. The medial malleolar area of the ankle is the most common location. Stasis ulcers can develop in the impaired skin. They are commonly accompanied by brownish discoloration, pruritus, excoriations, and dry, fine adherent scales. Late in the disease edema may be accompanied by lymphedematous blebs (elephantiasis verrucosa) and leakage of a serous thick yellow lymph fluid. Numerous conditions are associated with stasis dermatitis (Table 12-3).
Presentation and Characteristics
Primary Lesions
Early cases of stasis dermatitis begin as a red, scaly, pruritic patch that rapidly becomes vesicular and crusted owing to scratching and subsequent secondary infection. Bacterial infection may be responsible for the spread of the patch and the chronicity of the eruption. Edema of the affected ankle area results in a further decrease in circulation and, consequently, more infection. The lesions may be unilateral or bilateral.
Secondary Lesions
Three secondary conditions can arise from untreated stasis dermatitis:
Hyperpigmentation: This is inevitable following the healing of either simple or severe stasis dermatitis of the legs. This reddish-brown increase in pigmentation is slow to disappear, and in many elderly patients it never does so.
Stasis ulcers: These can occur as the result of edema, trauma, deeper bacterial infection, or improper care of the primary dermatitis.
Infectious eczematoid dermatitis: This can develop on the legs, the arms, and even the entire body, either slowly or as an explosive, rapidly spreading distant, symmetric, autoeczematous, or “id” eruption (see Chapter 21).
SAUER’S NOTE
Leg ulcer mantras
1. Look for underlying disease.
2. Look for an underlying malignant tumor, that is, basal cell cancer, squamous cell cancer, melanoma.
3. Look for clotting disorders.
4. Look for causes of ischemia, that is, arteriosclerotic vascular disease.
5. Look for an infection (primary or secondary).
6. Look for contact dermatitis.
7. Always consider a skin biopsy as part of the evaluation.
Course
The rapidity of healing of stasis dermatitis depends on the age of the patient and other factors listed under Causes. In elderly patients who have untreated varicose veins, stasis dermatitis can persist for years with remissions and exacerbations. If stasis dermatitis develops in a patient in the 40-to 50-year age group, the prognosis is particularly bad for future recurrences and possible ulcers. Once stasis ulcers develop, they can rapidly expand in size and depth. Healing of the ulcer, if possible for a given patient, depends on many factors. Ulcers less than 1 year old, less than 5 cm2, and ulcers that show significant healing after 3 weeks are more likely to heal by compression and bioocclusive dressings alone. Grafting procedures may be necessary for other venous leg ulcers. Negative pressure devices have shown promise.