Clinical Presentation
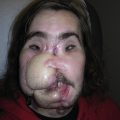
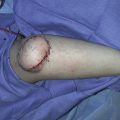
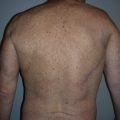
A 36-year-old White male sustained extensive thermal burn and had excisions and skin graft procedures on his trunk, axilla, and upper extremity. He also developed compartment syndrome and subsequently underwent a decompression procedure for compartment syndrome release. He unfortunately developed a large ventral hernia and previous abdominal wall reconstructions by the general surgery service failed. The plastic surgery service was asked by the primary service to perform a soft tissue coverage to the potential upper abdominal defect with exposed mesh after abdominal wall reconstruction ( Fig. 26.1 ). Because this patient had extensive burns over the trunk and had previously undergone a component separation procedure, there was no abdominal muscle or other flap that could safely be harvested to cover this potential soft tissue defect.
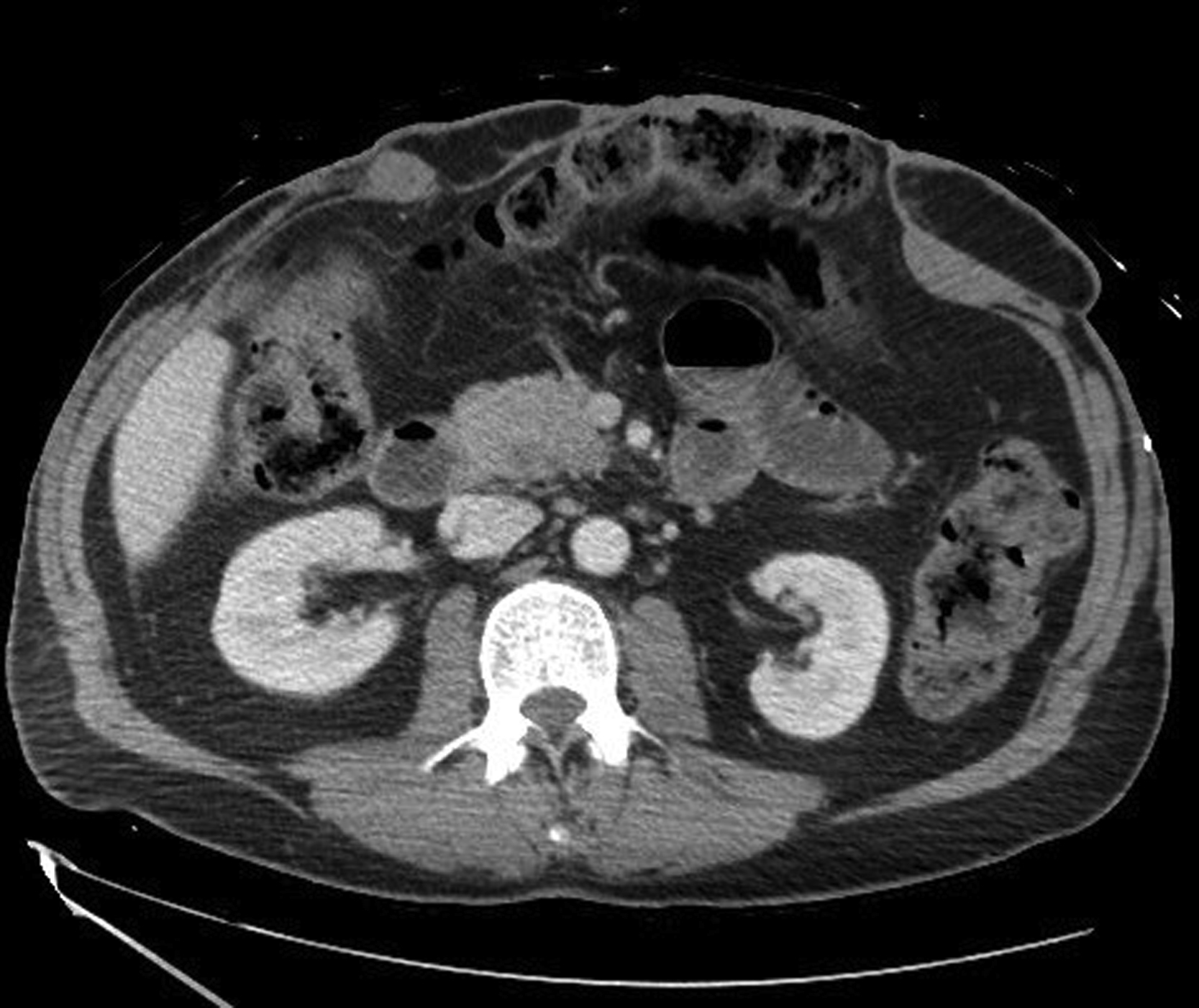
Operative Plan and Special Considerations
In this patient with a significantly large, healed skin graft over his trunk, a good soft tissue coverage to the upper abdomen after a mesh placement for abdominal wall ventral hernia repair was challenging because there was no local or distant flap that could be used for soft tissue reconstruction. A free latissimus dorsi myocutaneous flap could be selected to provide a good and reliable soft tissue coverage for potentially exposed mesh after abdominal wall reconstruction. The right internal mammary vessels at the third or fourth intercostal space could serve as recipient vessels for microvascular anastomoses. The right internal mammary vein is usually larger than the left, but a preoperative duplex scan could be performed to ensure good size and flow of those recipient vessels. The surgeons should anticipate some difficulties for the recipient vessel dissection.
Operative Procedures
Under general anesthesia with the patient in the supine position, the plastic surgery portion of the procedure started after the herniated bowels were taken back to the peritoneal cavity and the peritoneal closure was achieved with additional component separation technique and placement of Prolene mesh by the general surgery service. The upper abdominal soft tissue defect measured 15 × 7 cm with significant undermining and deep space ( Fig. 26.2 ).
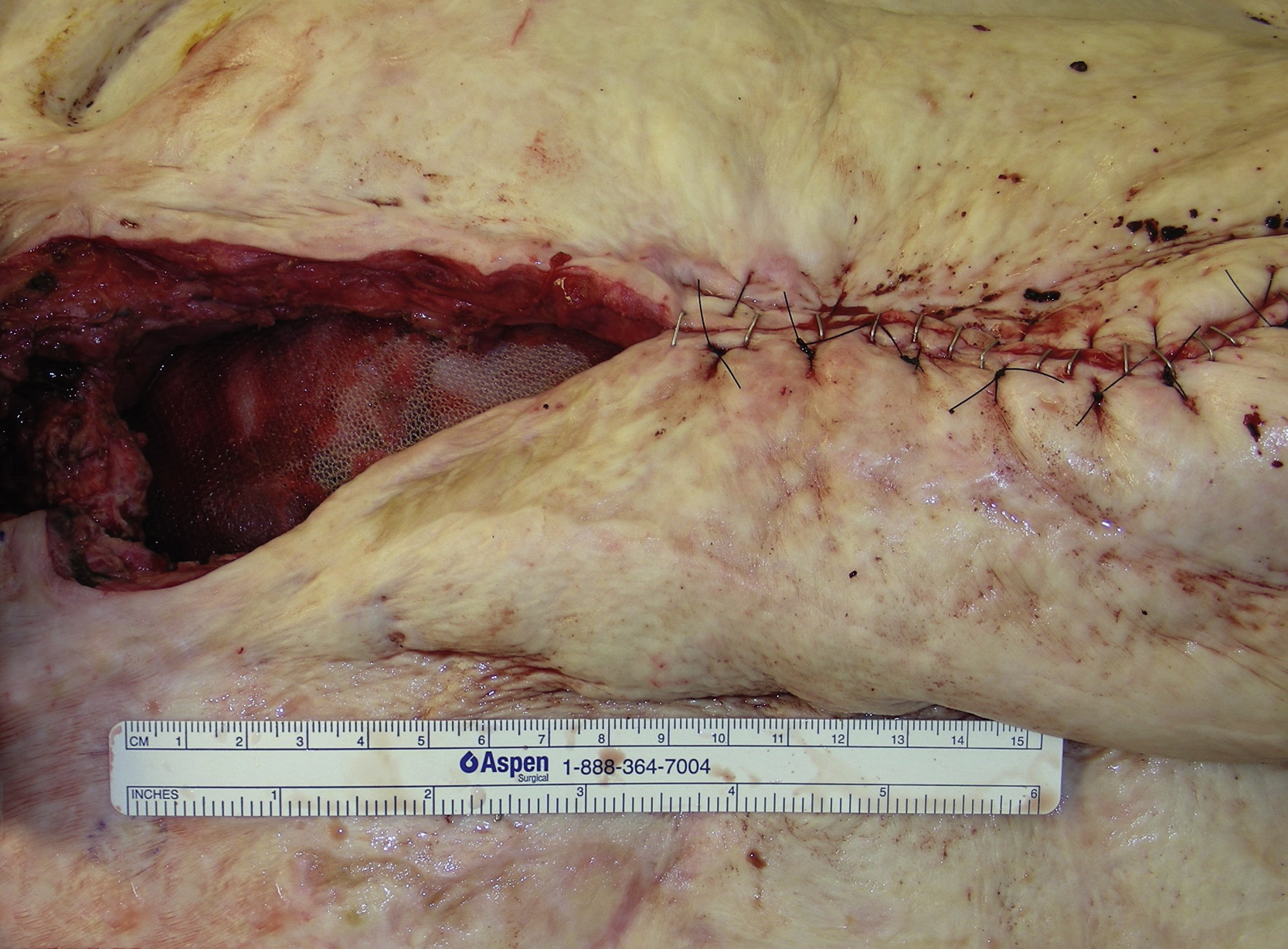
The right internal mammary vessels at the fourth intercostal space were explored first. After a skin incision and division of the medial portion of the pectoral major muscle, the fourth intercostal space was identified and a small portion of the rib connected to the sternum was resected. Both internal mammary artery and vein were identified and dissected out under loupe magnification.
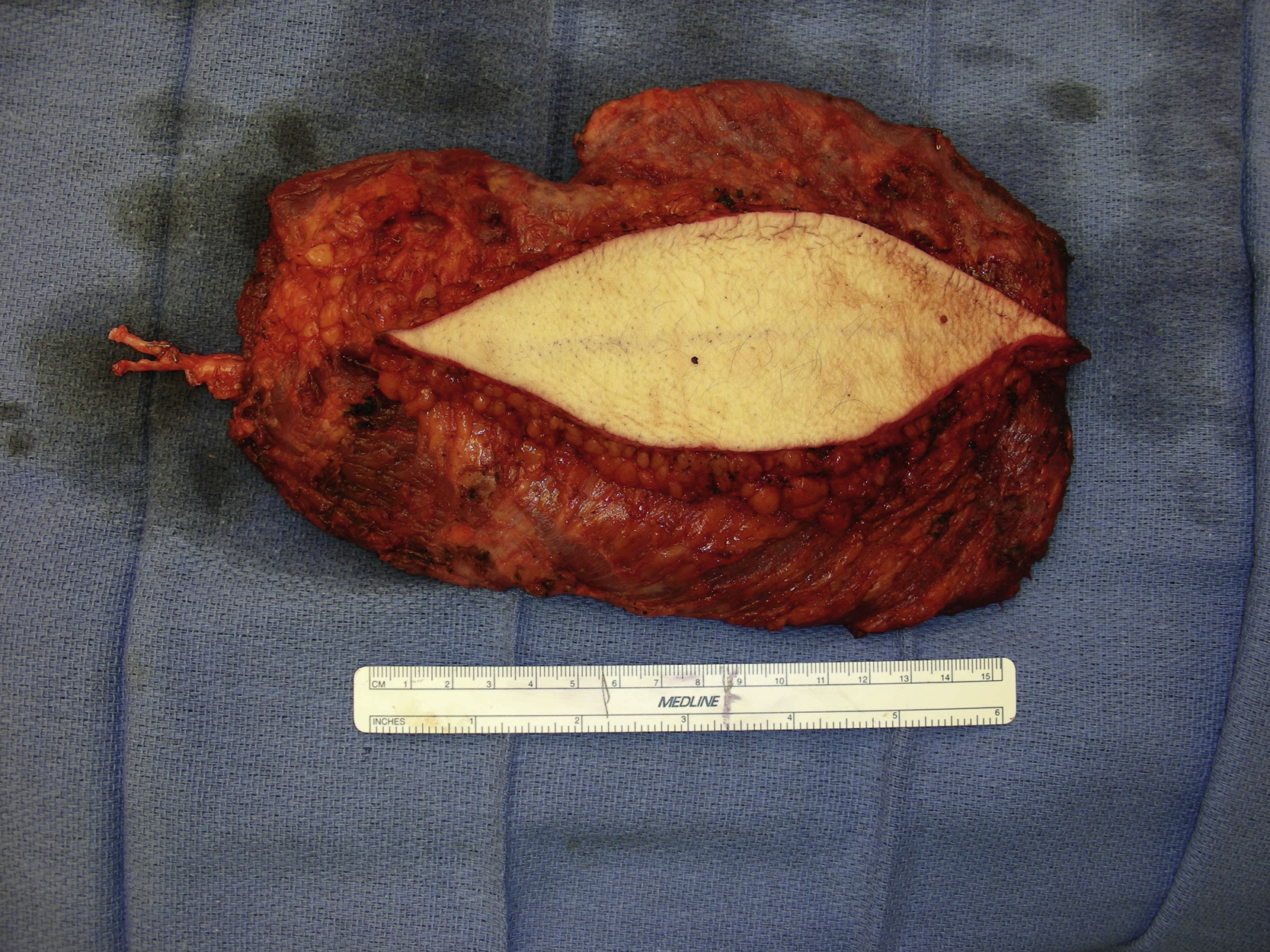
The patient was then changed to the right lateral decubitus position. A 15 × 7 cm skin paddle was marked and an incision was made down to the latissimus dorsi muscle fascia. Once both medial and lateral borders of the latissimus muscle had been identified, the muscle was divided with electrocautery medially, inferiorly, and laterally. Under direct vision, the latissimus dorsi myocutaneous flap was elevated along with the skin paddle. It was elevated from the chest wall and the serratus muscle was preserved. Once the serratus branch of the artery had been divided, the muscle attachment to the humerus was also divided with electrocautery. The pedicle dissection was performed under direct vision with proper retraction. The thoracodorsal nerve was divided first and both thoracodorsal artery and vein were divided after further pedicle dissection ( Fig. 26.3 ). The latissimus flap donor site was closed in three layers after placing two drains.