Clinical Presentation
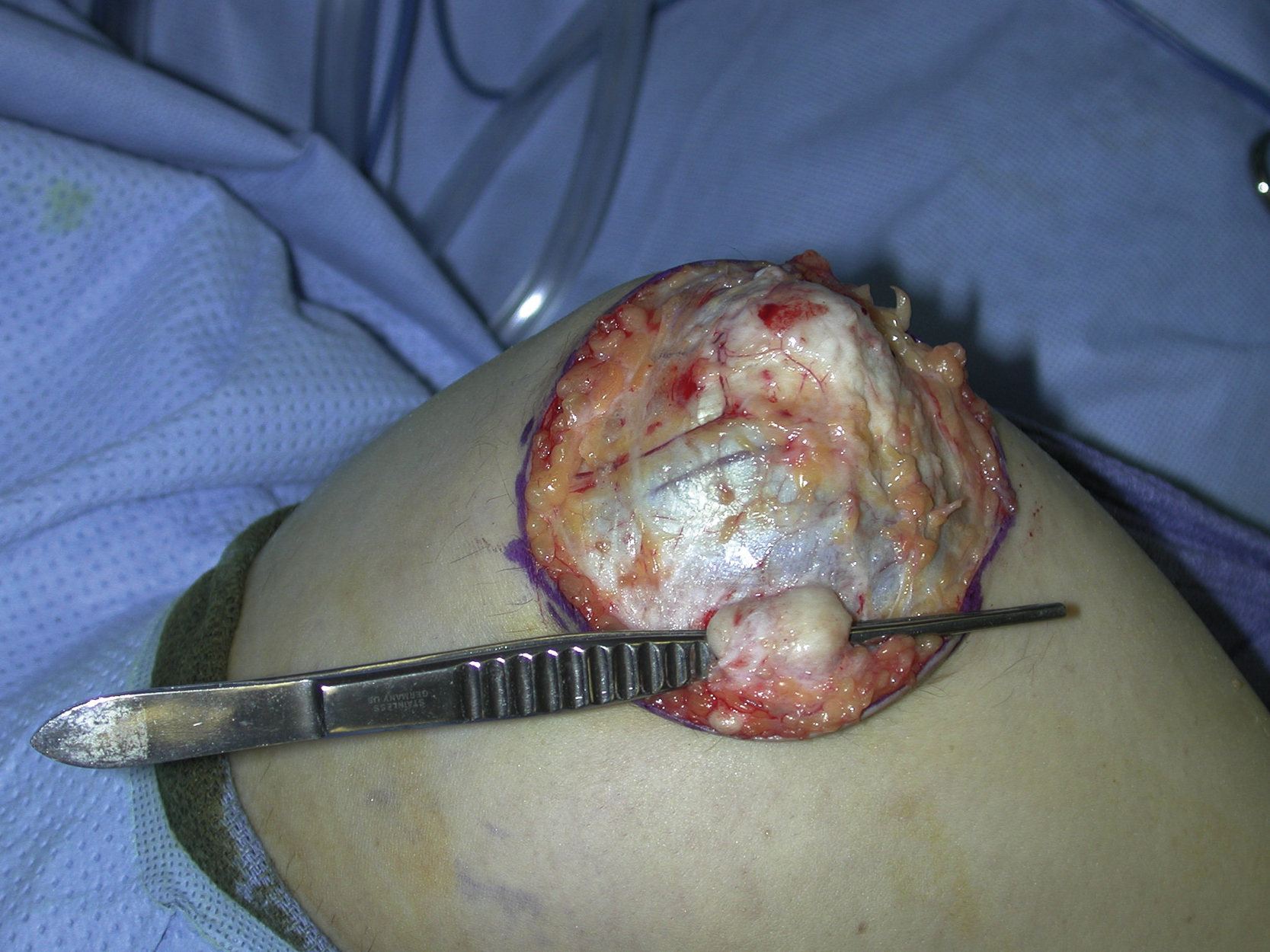
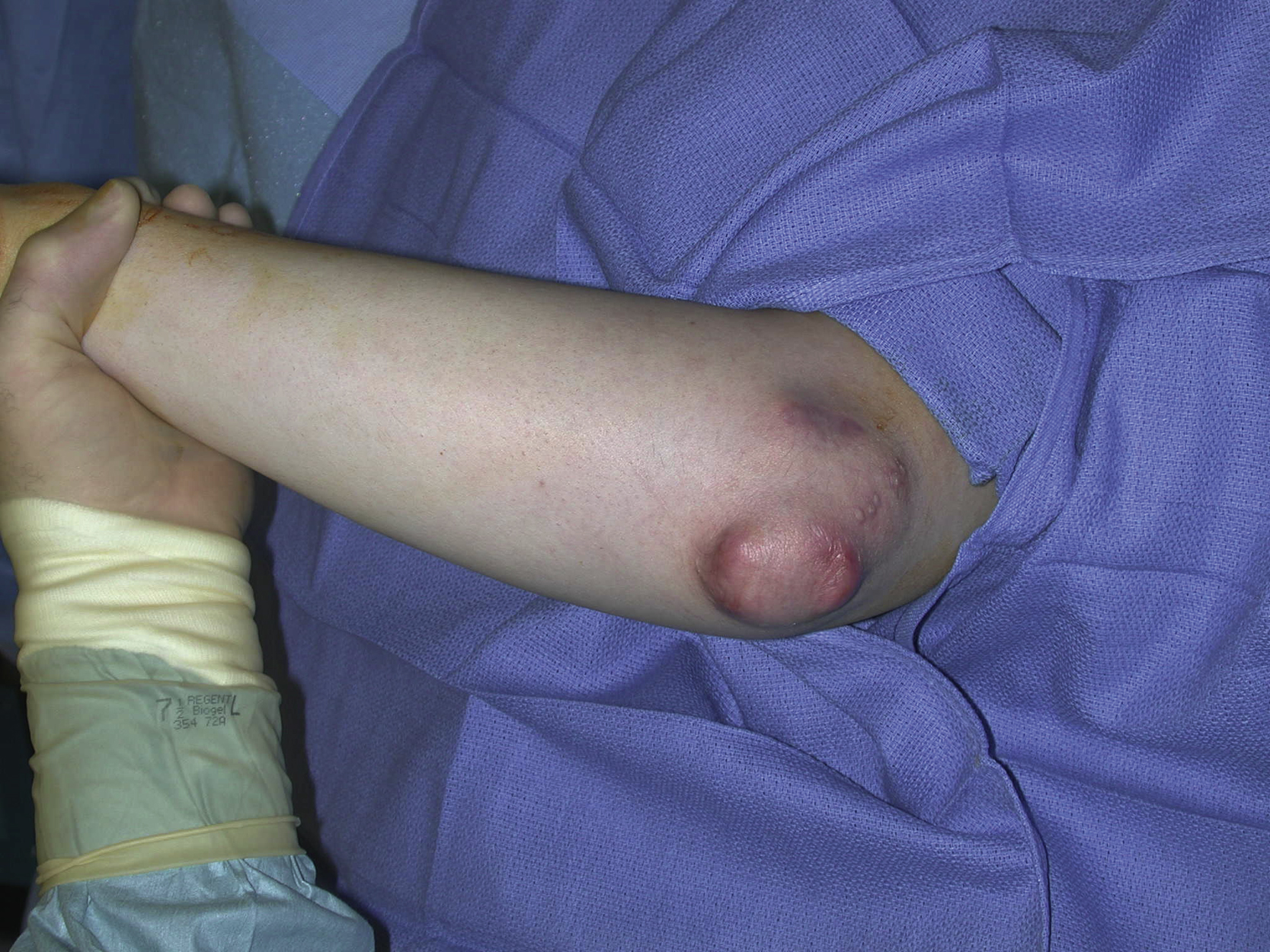
An 18-year-old White male had multiple subcutaneous rheumatoid nodules over his left elbow. He complained about pain and discomfort in the area and agreed to surgical resection to remove the subcutaneous lesions. Because of the large area affected, a large soft tissue defect was anticipated after surgical resection for these lesions ( Fig. 17.1 ).
Operative Plan and Special Considerations
Based on the size and location of the skin defect in the lateral elbow over the weight-bearing area, a more durable soft tissue reconstruction should be performed. The size of the soft tissue defect is too large for a lateral arm skin rotational flap. A pedicled radial forearm fasciocutaneous flap would be a good option for such a reconstruction. The flap is reliable and has a long pedicle for easy flap inset. It can provide durable soft tissue coverage to this weight-bearing area of the elbow. The Allen test should be done preoperatively to evaluate the patency and adequacy of the ulnar artery system when the radial artery is sacrificed during the flap elevation to ensure an adequate blood supply to the hand.
Operative Procedures
Under general anesthesia, the resection of rheumatoid nodules was done under a tourniquet control ( Fig. 17.2 ). All lesions and the affected skins were excised, which resulted in a 10 × 6 cm skin defect ( Fig. 17.3 ). A proximally based pedicled radial forearm flap was designed in the same forearm, oriented longitudinally, based on the distance from the defect to the distal tip of the flap ( Fig. 17.4 ). The flap dissection was again under tourniquet control. Once the skin incision had been made through the fascia, subfascial dissection was performed to elevate the skin paddle including the pedicle vessels. Once the distal radial artery and its venae comitantes as well as the cephalic vein were divided with hemoclips, the skin paddle was elevated freely. With a zigzag incision proximally to the skin paddle, the dissection of the pedicle in the forearm was performed between the flexor carpi radialis and brachioradialis muscles to the antecubital fossa. The flap was tunneled, based on the radial vessels proximally, through a skin bridge between the forearm and the elbow defect and was easily inset into the elbow defect. The flap was approximated to the adjacent skin with interrupted 3-0 nylon in half-buried horizontal mattress fashion. A drain was placed under the flap before final closure ( Fig. 17.5 ).