1 Surgical Anatomy of the Eyelids and Orbit
Appreciation of eyelid and orbital anatomy has dramatically changed our surgical approaches to problems in these areas. No longer are eyelids excised or distorted during attempted surgical repairs. Now, anatomic abnormalities are identified, and attempts are made to alleviate the underlying anatomic aberration. Patients with ptosis have an exploration of the levator aponeurosis and repair of defects or advancement of the levator. Patients with an ectropion have lateral tarsal strips created to strengthen the lower eyelid. Patients with entropion may have lower lid retractors reinserted in conjunction with a tarsal strip procedure to stabilize the eyelid.
Jones and Wobig (1976) were among the first authors to appreciate the significance of orbital and eyelid anatomy in surgical concepts. They went on to acknowledge two groups of surgeons of the eyelids.
1. One group comprises those who might appear to see how much damage they can do to the anatomy of the eyelid and still get good results.
2. The second group comprises those who try to inflict the least possible injury to the anatomy and also get good results.
It is this second group of surgeons we are attempting to enlighten and train.
OSTEOLOGY
The orbits are paired structures, lying on each side of the sagittal plane of the skull. The orbits are closely related to the paranasal sinuses, with the ethmoid sinuses, nasally; maxillary sinuses, inferiorly; and frontal sinuses, superior nasally. Bony contributions to the orbit are from the calvaria (frontal and sphenoid bones) and the facial bones.
The orbital cavity is pear-shaped, with its widest portion just within the orbital rim and then tapering posteriorly to the orbital apex. The medial walls of the orbits are parallel to one another, whereas the lateral orbital walls are divergent at a 90° angle. The central axes of the orbits, therefore, are directed 45° from one another. The floor of the orbit does not extend to the orbital apex but terminates approximately at the level of the posterior wall of the maxillary sinus.
The orbital rim is nearly rectangular, with a discontinuity at the inferior nasal margin, which forms the fossa for the lacrimal sac. The orbital margin acts as a buttress to protect the orbit and globe. It is produced by the frontal, zygomatic, and maxillary bones. If the orbit is struck with considerable force, it will produce a fracture at sites of potential weakness, normally the zygomaticofrontal and zygomaticomaxillary sutures. Associated fracture of the zygomatic arch will produce the characteristic trimalar (tripod) fracture.
The superior wall of the orbit is triangular, extending to the orbital apex. The orbital roof is composed primarily of the orbital plate of the frontal bone, with the posterior extent being formed by the lesser wing of the sphenoid. The orbital plate of the frontal bone meets with the ethmoid bone to form the frontoethmoidal suture. The anterior and posterior ethmoidal foramina, with associated arteries and nerves, are located within the frontoethmoidal suture. Care should be taken to identify and, if necessary, clip and ligate the anterior ethmoidal artery when performing surgical approaches to the medial orbit.
The medial wall of the orbit consists primarily of the lamina papyracea of the ethmoid sinus. The frontal process of the maxillary bone and the lacrimal bones contribute to the anterior portion of the medial wall, whereas the sphenoid bone contributes posteriorly. The lamina papyracea is extremely thin and provides a poor anatomic barrier, permitting the extension of infections or tumors from the ethmoid sinuses. The internal septated supporting structure of the ethmoid sinuses provides strength to the medial wall, so it is less commonly involved with blowout fractures of the orbit.
The orbital floor is composed of the maxillary, zygomatic, and palatine bones. The largest portion of the orbital floor is contributed by the orbital plate of the maxillary bone. As noted previously, the orbital floor does not extend to the orbital apex. The inferior orbital sulcus lies within the floor of the orbit and transmits the infraorbital nerve. The central portion of the orbital floor is thin and relatively weak.
The lateral orbital wall is triangular and consists of the zygomatic bone anteriorly and the greater wing of the sphenoid posteriorly. The prominent zygomatic bone will thin before fusing with the greater wing of the sphenoid. A thin bony plate separates the lateral orbit from the temporalis fossa anteriorly and the middle cranial fossa posteriorly.
The sphenoid bone has a pivotal role in orbital osteology. The superior orbital fissure is formed by a gap in the greater and lesser wings of the sphenoid. Structures passing through the superior orbital fissure (from lateral to medial) are the following: lacrimal nerve, frontal nerve, trochlear nerve, superior division of the oculomotor nerve, abducens nerve, nasociliary nerve, and the inferior division of the oculomotor nerve.
The inferior orbital fissure originates at the orbital apex and extends approximately 20 mm toward the central portion of the orbital floor. The fissure transmits the infraorbital nerve and artery and provides a route for the pterygoid plexus. The anterior and posterior alveolar nerves branch from the infraorbital nerve to supply the incisors and canines, and the cuspids, respectively. Injury to these nerves, such as in an orbital floor blowout fracture, may cause numbness in the canine and incisor teeth.
The optic canal connects the middle cranial fossa to the orbital apex. The optic canal is formed by the fusion of two roots of the lesser wing of the sphenoid. The posterior ethmoid sinuses and the sphenoid sinuses are adjacent to the medial wall of the canal. The optic canal transmits the optic nerve, ophthalmic artery, and ocular sympathetic nerves. Within the optic canal, the optic nerve is firmly adherent to the bone by dura. Within the orbit, the dura splits, forming the outer sheath of the optic nerve and the periorbita.
TOPOGRAPHIC ANATOMY
Eyelids
The various surface contours on the midface and upper face, coupled with varying skin thickness, produce characteristic folds in the periocular area. The palpebral fissure generally ranges from 10 to 12 mm in vertical dimension, and 25 to 30 mm in horizontal dimension. In primary gaze, the upper eyelid margin is generally 1 to 2 mm below the superior limbus. The upper eyelid position gradually lowers as the individual ages. It is important to appreciate that the peak of the upper eyelid margin is nasal to the center of the pupil with the eye in primary gaze. The upper lid contour is extremely important, particularly in ptosis repairs, for which novice surgeons often place the upper eyelid peak at the pupil or even lateral to the pupil. The lower eyelid margin is generally at the inferior edge of the corneal limbus. The lowest portion of the lower eyelid margin is slightly temporal to the pupil.
The upper eyelid crease is horizontally oriented approximately 8 to 12 mm above the eyelashes. It is formed by the subcutaneous insertion of the terminal fibers of the levator aponeurosis. These fibers will firmly adhere to the subcutaneous tissues below the eyelid crease to form the pretarsal portion of the eyelid. The skin overlying the orbital septum has no levator aponeurotic subcutaneous extensions and will fold over the eyelid crease in varying proportions. The lower eyelid has a poorly defined eyelid crease extending to within 2 to 3 mm of the eyelid margin nasally and 5 to 6 mm temporally. The nasojugal fold extends inferior and lateral from the medial canthal angle along the side of the nose. The malar fold extends from the lateral portion of the lower eyelid toward the inferior lateral extent of the nasojugal fold. The nasojugal and malar folds represent the junctions of the thin eyelid skin to the thicker skin of the cheek. In addition, the angular artery and vein will generally be located in the nasojugal fold.
Eyebrow
The eyebrow represents a specialized musculocutaneous plane that is extremely important in facial expression. The eyebrows are best considered an extension of the scalp, or as a cranial appendage. Recently, eyebrow variations have been appreciated in functional and aesthetic surgery in the upper face. In particular, gender variations of the eyebrow contour may influence the planning of cosmetic eyebrow and upper lid surgery.
The anatomy of the eyebrow has been thoroughly described by Lemke and Stasior (1982). These authors described four major layers of the brow: skin, muscle, fat, and aponeurosis. The muscular layer of the eyebrow and glabellar can be divided into three groups: superficial, intermediate, and deep. The superficial muscular group consists of the frontalis, procerus, and orbital portion of the orbicularis oculi muscles. The intermediate layer and deep layers consist of the depressor supercilii muscle and the corrugator supercilii muscles, respectively.
The frontalis muscle is encapsulated by an anterior and posterior muscular sheath, which is an extension of the galea aponeurosis. The posterior muscular sheath will split as it approaches the periosteum of the superior orbital rim. The multiple splits in the posterior muscular sheath will produce a potential space for the brow fat pad. The posterior muscle sheath of the frontalis muscle then extends into the eyelid to contribute to the orbital septum. The brow fat greatly enhances brow mobility and is present in varying degrees. Surgical dissections have demonstrated the correlation between the prominence of the pad with the degree of brow ptosis and fullness. The brow fat pad contributes to the sexual variation in brow anatomy; in masculine brows, the brow fat pad is more prominent and extends inferiorly into the eyelid directly anterior to the orbital septum. Nasally, the frontalis muscle will interdigitate with the vertically oriented procerus muscle, the obliquely oriented corrugator supercilii muscles, and the orbital orbicularis muscle. This intermixing of fibers supports the brow at this level nasally. The frontalis muscle may not extend to the superior orbital rim laterally, which may contribute to the brow ptosis that is frequently seen clinically in this area.
The corrugator supercilii muscle is the deep muscle of the eyebrow. The muscle is oriented obliquely in the nasal aspect of the eyebrow with a bony insertion in the frontal bone near the superior nasal aspect of the orbit. Muscular contraction results in vertically oriented forehead furrows and has been called the muscle of aggression. Again, chemical denervation is frequently required to eliminate these furrows.
Upper eyelids
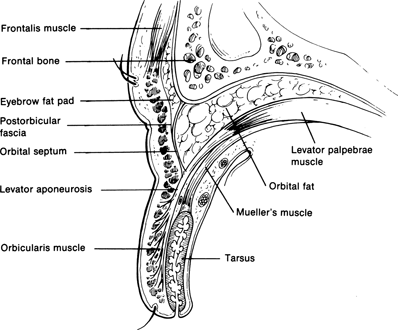
Figure 1-1. A sagittal view of normal upper eyelid anatomy. The eyelid has essentially six layers: skin, orbicularis muscle, levator aponeurosis, Müller’s muscle, tarsus, and conjunctiva. However, these layers are variable based on the level of eyelid examined. Near the eyelid margin, there are only four layers: skin, orbicularis muscle, tarsus, and conjunctiva. Directly above the tarsal border, five layers of the eyelid are present: skin, orbicularis muscle, levator aponeurosis, Müller’s muscle, and conjunctiva. Care must be taken to identify the level of the eyelid to appreciate its various layers.
The eyelid skin has unique features to enhance its mobility. The epithelial layer is thin and attaches to the orbicularis muscle by a loose connective tissue devoid of dermal-like tissue. In addition, sebaceous glands are not developed extensively in the eyelid, which would anchor the skin to the subcutaneous tissues. These distinguishing features of the eyelid skin account, in part, for its tendency to become redundant and, in exaggerated situations, fold over the eyelid, producing a visual field loss. As an involutional change, this excess skin is called dermatochalasis but may result from recurrent angioneurotic edema, producing the blepharochalasis syndrome.
The orbicularis muscle is the protractor for the eyelids and is under voluntary control from the facial nerve. The concentrically arranged orbicularis muscle is divided into three sections: pretarsal, preseptal, and orbital. The combined pretarsal and preseptal orbicularis muscles form the palpebral portion of the orbicularis and overlie the tarsus and orbital septum, respectively. The orbital orbicularis overlaps the orbital rims, interdigitating with the eyebrow muscles superiorly.
The pretarsal and preseptal orbicularis muscles contribute to the superficial and deep portions of the medial and lateral canthal tendon (LCT). The deep extensions of the pretarsal and preseptal orbicularis muscles are referred to as Horner’s and Jones’ muscles, respectively, and insert on the fascia overlying the lacrimal sac. In addition, the pretarsal orbicularis also contributes to the LCT. Giola et al. (1987) identified the pretarsal orbicularis muscle to extend beneath the orbital septum laterally to contribute to the tendinous component of the LCT. Laterally, the preseptal orbicularis muscle joins in the lateral raphe, oriented horizontally in the lateral canthal angle.
The medial canthal tendon (MCT) supports the nasal aspect of the eyelids. The MCT has superficial and deep components that anchor the eyelid nasally and posteriorly against the globe. Anderson (1977) emphasized the role of a superior branch of the MCT extending from the anterior portion of the MCT to insert onto the frontal bone. The superior limb of the MCT anchors the nasal eyelid, preventing dystopias of the medial canthal angle.
The LCT has been highlighted in the literature because of a variety of procedures described to correct canthal defects or lid malpositions. Giola et al. (1987) have identified both a tendinous and ligamentous component to the LCT. The tendinous portion of the LCT is from the pretarsal orbicularis muscle and inserts on the inner aspect of the lateral orbital rim at the lateral orbital (Whitnall’s) tubercle. The ligamentous component of the LCT is a direct extension from the tarsus, which slips posterior to the orbital septum to insert at the lateral orbital tubercle. This deep extension and attachment of the LCT draws the eyelid laterally and posteriorly, approximating the eyelids to the globe. Attempts to surgically reconstruct the LCT must reconstitute the deep posterior extensions of the tendon to maintain lid apposition with the globe (Anderson and Dixon, 1979).
The orbital septum forms the anatomic boundary between the eyelid and the orbit. At one time, the orbital septum was considered a sacred structure, not to be penetrated unless unavoidable. If the structure was violated, it was meticulously closed to reform the anatomic barrier it represented. This impression has changed dramatically.
The orbital septum originates at the arcus marginalis of orbital rim. The orbital septum extends toward the tarsus and fuses with the levator aponeurosis and the lower lid retractors prior to their insertion of the tarsus (Anderson and Beard, 1977). In the upper eyelid, variations in the level of fusion of the orbital septum and levator aponeurosis will produce changes in the level of the eyelid crease and fold. In the Oriental eyelid, the orbital septum fuses with the levator aponeurosis below the tarsal border, thereby eliminating the eyelid crease and producing a prominent lid fold (Doxanas and Anderson, 1984). The preaponeurotic or orbital fat is confined by the orbital septum and forms pockets; however, the multilaminated orbital septum may thin with age, allowing herniation of orbital fat. The nasal fat pockets in the upper and lower eyelids are white, instead of yellow, and should not be overlooked during blepharoplasty surgery. Occasionally, the orbital lobe of the lacrimal gland will prolapse, to produce fullness in the lateral portion of the eyelid. Care must be exercised during blepharoplasty to identify the prolapsed lacrimal gland and distinguish it from orbital fat to prevent its inadvertent excision.
The levator palpebrae superioris muscle provides a distinct eyelid retractor. The muscle arises at the orbital apex, directly above the annulus of Zinn. The levator muscle proceeds anteriorly from the orbital apex in the superior orbit adjacent to the periorbita. As the superior orbital rim is approached, the levator fans nasally and temporally.
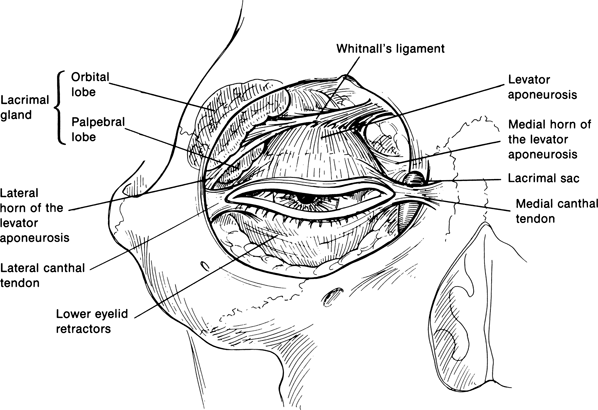
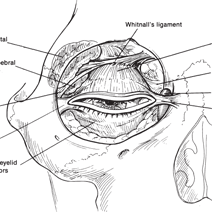
Figure 1-2. A frontal view of Whitnall’s ligament and anterior orbital structures. As the levator muscle extends below the superior orbital rim, it is redirected by the superior transverse ligament, also known as Whitnall’s ligament. The ligament acts as a fulcrum to redirect the muscle from an anteroposterior to superoinferior direction, enhancing its function. At the level of the superior transverse ligament, the levator muscle starts to transform into its aponeurotic extension. This transformation of the levator muscle to a white shiny structure is complete approximately 10 to 12 mm above the superior border of the tarsus. The aponeurotic fibers diffusely extend anteriorly through the orbicularis muscle overlying the tarsus to insert into the subcutaneous tissues. The superior-most subcutaneous extension of the levator aponeurosis will define the level of the eyelid crease. The posterior portion of the levator aponeurosis attaches to the lower 7 to 8 mm of the tarsus. The superior 2 to 3 mm of the tarsus has loose attachments of the levator aponeurosis, whereas the aponeurosis is most strongly adherent to the tarsus about 3 mm above the eyelid margin. The diffuse extensions of the levator aponeurosis produce a smooth, coordinated movement to the upper eyelid.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree