Orbital Decompression
SURGICAL INDICATIONS
Orbital Graves’ disease
The majority of orbital decompression procedures are performed for the treatment of dysthyroid orbital Graves’ disease. Most patients with orbital Graves’ disease have exophthalmos caused by orbital edema and enlargement of extraocular muscles. Spontaneous anterior displacement of the globe is usually sufficient to decompress the orbit and maintain normal optic nerve function. However, in 2% to 5% of patients, the extraocular muscles enlarge within the confines of the bony orbit and compress the optic nerve, causing dysfunction. Muscular enlargement in orbital Graves’ disease is often most pronounced in the posterior one third of the muscles, creating pressure in the orbital apex. Not only are the extraocular muscles in the apex much closer to the nerve, but they are also fixed in position by the annulus of Zinn.
Systemic steroid therapy is the preferred medical treatment for compressive optic neuropathy (CON). Unfortunately, not all patients respond to these medications, and there are frequent recurrences when steroids are withdrawn. Many patients cannot tolerate the high dosage required, and the complications of long-term steroids are well known. Beneficial effects usually occur within the first 2 weeks of treatment, and no further improvement can be expected after 6 to 8 weeks. When neuropathy is unresponsive to steroids, or recurs when steroids are withdrawn, surgical decompression is usually recommended.
In addition to visual loss from CON, potential indications for surgical decompression in orbital Graves’ disease include corneal exposure, strabismus, pain, choroidal folds, recurrent globe luxation, and cosmesis. Eyelid surgery is usually adequate for the management of corneal exposure. Strabismus, when stable, is best corrected with prisms or muscle surgery. In recent years, decompressions have been performed more frequently for cosmetic reasons. However, because of the serious potential complications of orbital decompression, we usually reserve decompression surgery for the preservation of vision in cases of CON.
Trauma
Direct trauma to the orbit can produce expansion of orbital contents from hemorrhage, edema, or emphysema. Proptosis relieves orbital pressure, but if this spontaneous anterior decompression is inadequate, then compression of the globe may cause an elevated intraocular pressure, with risk of central retinal artery occlusion. Pressure elevations within the orbit can also compromise blood flow to the eye or optic nerve, resulting in an ischemic optic neuropathy. The probable site of optic nerve compression in trauma is again the orbital apex, a rigidly confined space filled with vital structures.
Posttraumatic orbital hemorrhage and edema may occasionally require surgical treatment if proptosis is very severe and there are clinical signs of optic nerve dysfunction. Vision that is initially intact and subsequently deteriorates suggests reversible compression. Lateral canthotomy and cantholysis will decompress the anterior orbit, but posterior surgical decompression may be necessary in rare cases. Needle aspiration should be reserved for orbital emphysema.
Traumatic optic nerve injury usually results from mechanisms other than orbital compression. A history of immediate visual loss after trauma suggests optic nerve transection at the moment of impact. Visual loss from nerve edema within the osseous canal can occur without significant proptosis. Recognition of these other mechanisms for traumatic optic neuropathy can prevent unnecessary decompression surgery. Only patients with massive hemorrhage and extremely firm orbits should even be considered for decompression, as most cases of traumatic optic neuropathy are related to other mechanisms.
EVALUATION OF PATIENTS
Clinical evaluation
Patients followed for orbital Graves’ disease require repeated ophthalmic examinations, with special emphasis on optic nerve function. Examinations should be more frequent during active phases of the disease. Optic nerve dysfunction may occur at any time, even while the patient is receiving anti-inflammatory therapy. The degree of proptosis is not an accurate indication of risk for optic neuropathy. In fact, most patients with CON have only moderate exophthalmos. Patients with an initial diagnosis of orbital Graves’ disease also require evaluation of thyroid function by an endocrinologist.
Visual acuity is only a gross indication of optic nerve function. Examinations must also include evaluation of the pupils, visual fields, color vision, and dilated examinations of the optic disc (looking for pallor or edema). Motility examinations reveal extraocular muscle involvement. Slit-lamp examinations may disclose signs of corneal exposure. The same examination should be performed for trauma patients with suspected optic nerve injury.
Further diagnostic tests
If optic neuropathy is diagnosed, then a computerized tomography (CT) scan of the orbit provides the best image of the optic nerve and adjacent structures. Axial sections may demonstrate contact between the optic nerve and the enlarged extraocular muscles. Coronal sections are especially useful for evaluation of the orbital apex. In orbital Graves’ disease, the enlarged extraocular muscles may displace orbital fat, eliminating any perceivable space between themselves and the nerve. This CT scan image in association with clinical signs of optic neuropathy suggests the need for surgical orbital decompression, when medical therapy fails.
The diagnosis of orbital Graves’ disease with CON must be carefully documented before surgery. Most patients have classic eye findings of Graves’ disease and a past history of thyroid dysfunction. There may be other orbital disorders that mimic Graves’ disease, especially when the findings are asymmetric. A careful neuroophthalmic examination is needed to rule out other causes of visual loss or optic neuropathy. High-quality CT scans or magnetic resonance imagings are necessary to confirm the diagnosis of orbital Graves’ disease with optic nerve compression and to eliminate the possibility of other disorders.
SURGERY
Surgical anatomy of the orbit
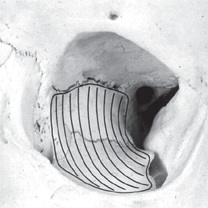
The most important anatomic consideration during surgical decompression is adequate expansion of the orbital apex. Decompression of this area, near the optic foramen, relieves pressure on the nerve. This can be accomplished only by bone removal from the posterior medial wall or the orbital roof. A simple lateral wall or orbital floor decompression does not adequately decompress the apex. Laterally, the temporal lobe of the brain prevents posterior access to the orbital apex. Expansion is further limited by the temporalis muscle. An inferior decompression also fails to achieve the necessary apical decompression because the floor does not extend as far posterior as the optic canal.
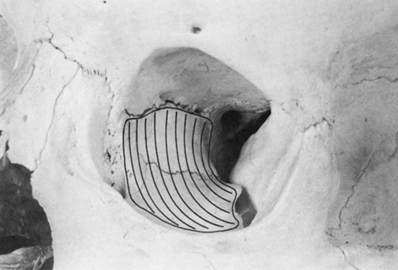
Figure 33-1. Although removal of the orbital roof by a subfrontal approach decompresses the orbital apex, this neurosurgical technique subjects the patient to greater risks. For these reasons, resections of the orbital floor and medial wall have been widely accepted as the best approach to orbital decompression for optic nerve dysfunction. Orbital tissues can expand into the ethmoid compartment once the lamina papyracea and ethmoid air cells have been removed.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree