2 Fundamental Techniques in Ophthalmic Plastic Surgery

Fundamental techniques in ophthalmic plastic surgery are similar to those shared by all surgical specialties. The goal of the operative procedure is to alleviate an existing abnormality, with minimal surgical disturbance of the adjacent tissues. This requires the proper orientation of incisions, utilization of anatomic planes to facilitate surgical dissection, and the appropriate closure of incisions. Adherence to these principles, coupled with gentle handling and cauterization of periorbital and orbital structures to minimize tissue necrosis and devitalization, will help to achieve a satisfactory functional and cosmetic result.
ANESTHESIA
Before the initiation of any surgical procedure, appropriate anesthesia is required. Anesthetic options available to the patient are local, local with sedation, and general. Medical or emotional considerations are important factors in determining the anesthetic option, as this decision is individualized for each patient. Those with preexisting medical conditions, especially cardiac abnormalities or hypertension, will benefit from intravenous sedation to reduce anxiety associated with the procedure.
Local anesthetic agents with epinephrine are preferred to enhance vasoconstriction of the highly vascular eyelids; however, these may be contraindicated in patients with hypertension or cardiac arrhythmias. The onset and duration of action of commonly used local anesthetic agents are summarized in Table 2-1.
Lidocaine 2% with epinephrine 1:100,000 is effective for most oculoplastic surgeries. For procedures of longer duration, though, an equal mixture of lidocaine 2% with epinephrine and 0.5% bupivacaine with epinephrine provides prolonged anesthesia. Local anesthetics should be injected subcutaneously with a 30-gauge needle between the thin eyelid skin and orbicularis muscle. One should avoid visible vessels and penetrating the muscle to minimize hematoma formation. The orbicularis muscle and deeper tissues are eventually anesthetized by diffusion of the anesthetic agent. After approximately 10 minutes, the vasoconstricting effects of the epinephrine will help to further reduce bleeding tendencies and hematoma formation. Injection of anesthetics in the periorbital region, excluding the eyelids, should be in the subcutaneous plane. The use of a 25- or 27-gauge needle may facilitate its passage in these thicker tissues.
Neuroleptic sedation or analgesia is the preferred method of anesthesia during oculoplastic procedures. The patient has the advantages of being monitored during the procedure to ensure that there are no hypertensive episodes, cardiac arrhythmias, or respiratory problems. Intravenous diazepam or midazolam reduces patient anxiety and is also a potent amnestic agent. Intravenous sedation with thiopental (Pentothal) or methohexital (Brevital) will temporarily sedate the patient, to eliminate recall of the periocular injections. These agents are slowly titrated until the patient achieves an adequate level of anesthesia without respiratory suppression. The specific anesthetic agents to be used are best determined by the preference of the anesthesiologist. When the patient becomes cognizant of his surroundings, the procedure is well underway, and cooperation may be elicited from the patient to monitor eyelid position. With the proper utilization of pharmacologic agents, patients experience little discomfort intraoperatively or postoperatively.
Indications for general anesthesia are diminishing with the improvement of neuroleptic anesthesia. General anesthesia is usually reserved for those patients undergoing more invasive procedures, such as orbital procedures, or in whom cooperation is difficult, such as children. General anesthesia presents minimal risk of long-term morbidity or mortality; however, it involves a more prolonged recovery period compared with alternative anesthetic methods.
HEMOSTASIS
Patients taking aspirin, dipyridamole (Persantin), or warfarin (Coumadin) will have an increased bleeding tendency. Aspirin inhibits platelet function and should be discontinued 2 weeks before surgery. Patients receiving anticoagulant therapy should consult their internist concerning a short-term discontinuation of its use preoperatively. In this group of patients, the prothrombin time should be obtained before surgery to ensure adequate coagulation control. Patients with a long smoking history may have a greater tendency for more bleeding during surgery, in spite of normal coagulation studies.
Two coagulation modalities currently exist: thermal and electrical. Thermal hot-wire cautery generates heat, far in excess of that necessary to produce cellular destruction and control bleeding. In addition, tissues not directly in contact with the cautery may be devitalized owing to channeling effects. Electrical cautery with unipolar, bipolar, or wet-field modalities is the preferred method to obtain hemostasis. Bipolar cautery destroys less surrounding tissues and produces more effective coagulation. In patients with diffuse oozing from the operative site, bleeding can be controlled with direct pressure or the use of epinephrine-moistened cotton pledgets. Another method includes the application of absorptive agents that promote thrombogenesis such as absorbable gelatin sponge (Gelfoam), oxidized cellulose (Surgicel), and microfibrillar collagen (Avitene). In addition, bone wax is effective in controlling bleeding from bone edges and bony foramen.
BIOPSY TECHNIQUES
Biopsy methods for eyelid lesions include the shave, punch, incisional, excisional, and full-thickness eyelid resection techniques. The tumor size, location, and suspected preoperative diagnosis will determine the biopsy method of choice. Eyelid margin tumors, either a dermal nevus or papilloma, should be treated with a shave biopsy. A diffuse melanotic tumor should have incisional biopsies to determine if dermal extension occurs. Other tumors may lend themselves to excisional biopsy. As such, the biopsy technique is modified to the clinical situation, based on the surgeon’s preference and experience.
The punch biopsy is preferred by dermatologists to obtain tissue for pathologic examination. This technique utilizes a 1- to 8-mm punch to obtain a core of tissue including subcutaneous tissues. The round defect is then allowed to granulate. This method is most efficacious in skin with a thick dermal connective tissue layer and not the thinner skin with subcutaneous tissue of the eyelid. The punch biopsy technique should not be used in the eyelids, since a full-thickness eyelid biopsy may inadvertently be obtained.
The shave biopsy is a helpful diagnostic and therapeutic modality for tissue procurement. This technique involves the use of a size 11 Bard-Parker blade or sharp iris scissors to excise a lesion flush with the surface of the surrounding skin. The tissue obtained is generally readily differentiated between a benign and a malignant lesion; however, the differentiation of squamous cell carcinoma from benign lesions, such as an inverted follicular keratosis, keratoacanthoma, pseudoepitheliomatous hyperplasis, and actinic keratosis, is not possible, owing to the lack of subcutaneous tissues. As such, the pathologic diagnosis of squamous cell carcinoma should be closely scrutinized following a shave biopsy and warrants further investigation.
Dermal nevi and papillomas have a tendency to occur on the lid margin. Overzealous excision of these tumors can result in lid margin irregularity or trichiasis. The use of the shave biopsy technique will effectively reduce alterations of the eyelid margin. The tumor is removed flush with the lid margin, with a chopping block technique or a sawing motion after the size 11 blade is placed in the center of the lesion. Care should be taken not to violate the eyelashes.
Incisional biopsy is indicated when additional deeper tissue is required to determine dermal extension of an epithelial tumor. This technique is useful for epithelial lesions, such as basal cell carcinoma, squamous cell carcinoma, keratoacanthoma, and acquired melanosis. A wedge from a suspected keratoacanthoma can demonstrate the overall configuration of the tumor, which is helpful in its pathologic evaluation. Areas of a superficial spreading melanotic lesion, which has become raised or indurated, can have a biopsy specimen taken to rule out malignant degeneration.
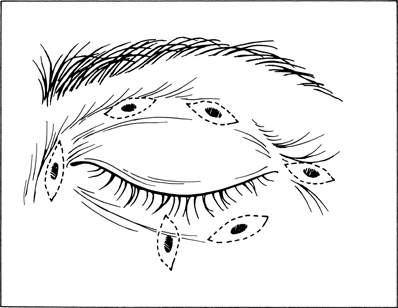
Figure 2-1. Excisional biopsy is effective for both diagnostic and therapeutic purposes. The tumor is incorporated into an ellipse, which is oriented parallel to normal tissue tension lines. An ellipse oriented perpendicular to these tension lines will amplify scar appearance. Care should be exercised when removing lower eyelid tumors, because excessive skin excision with a horizontally oriented ellipse may produce a postoperative ectropion. If a question exists about a horizontally oriented lower lid excisional biopsy, it should be rotated vertically to prevent the development of postoperative ectropion.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree