14 Direct, Midforehead, and Pretrichial Browplasty
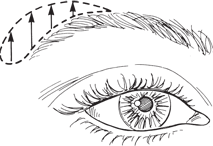
Eyebrow ptosis is frequently encountered by the ophthalmologist and must be distinguished from upper lid dermatochalasis. Both will result in the appearance of redundant tissues in the upper lid. The surgeon must determine which of these is present, or if there is a combination of both, before deciding on appropriate treatment.
In women, the brow tends to be higher and more arched in its contour, with the high point over the lateral canthus, whereas the male brow is lower and less arched. The resting height of the brow diminishes with age. The amount of resultant brow ptosis depends upon heredity, history of smoking, sun exposure, and skin thickness, oiliness, and color. The individual patient’s pattern of facial animation also contributes to the development of brow ptosis, typically resulting in a more pronounced lateral droop in patients who squint frequently, and in more medial brow ptosis in patients who frown frequently.
Some surgical procedures are directed strictly toward elevating and repositioning the ptotic brow. Others also remove excessive forehead, glabellar, and temporal wrinkles and skin. These latter procedures are more often performed for cosmetic purposes, whereas the former are used to correct functional brow position abnormalities.
ANATOMIC CONSIDERATIONS
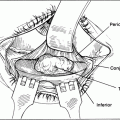
Any operation to elevate the brows must be planned to avoid damage to the sensory and motor nerves of the forehead. The supraorbital nerve provides sensation to the forehead and scalp. It lies on the surface of the frontalis muscle in the central third of the forehead and runs vertically from the supraorbital notch toward the crown. The temporal branch of the facial nerve provides motor innervation to the forehead muscles. This branch courses deep to the frontalis muscle in the forehead, running horizontally from lateral to medial. The nerve runs on the superficial temporalis fascia, descending beneath the frontalis muscle at a point approximately two finger breadths above the temporal orbital rim. Skin incisions should be placed either above or below this point to avoid nerve injury. Similarly, dissection must be carried out either superficial or deep to the frontalis muscle to avoid the sensory and motor nerve branches.
DIRECT BROWPLASTY
Direct browplasty involves the excision of tissue immediately above the brow. Closure results in elevation of the brow. The procedure is usually performed under local anesthesia.
Preoperatively, one must determine the amount of medial, central, and lateral brow droop. Discussion with the patient should determine the desired postoperative appearance of the brow.
The superior several rows of brow hairs should be included with the incision to better camouflage the scar. If there is a large degree of temporal brow ptosis, the incision can be carried temporally beyond the lateral aspect of the brow in an S-shaped fashion. Although the scar lateral to the brow will be fully exposed, the thinner temporal skin results in a less noticeable scar than occurs in the thicker, more sebaceous skin that is present immediately above the brow. If the excision does not extend temporal to the brow, only minimal elevation of the temporal brow can be achieved.
The superior half of the incision should be marked out to approximate the desired height and contour of the brow, as direct closure will result in the brow directly following the superior incision. The amount of skin to be excised is determined by elevating the brow to its desired position and estimating the amount of the excess forehead tissue that results. It is preferable to do this with the patient sitting upright. The desired high point of the brow is marked directly above the lateral canthus. The superior skin line is tapered medially and laterally from this point. The superior incision should be slightly overelevated, as there is usually some decay several months after surgery.
Local anesthetic with epinephrine is then directly infiltrated within the outlines of the proposed excision. It is important to wait 10 minutes, to allow maximum vasoconstriction to occur following injection, before making the incision.
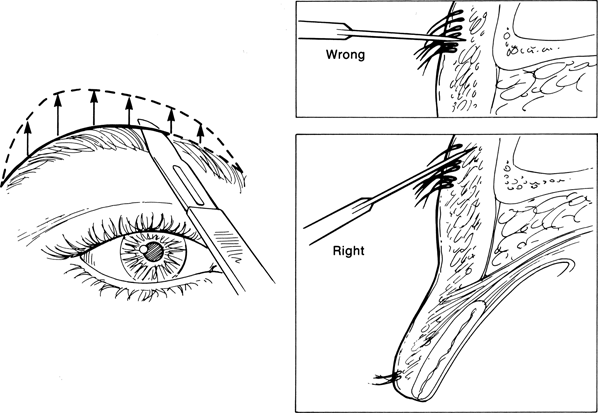
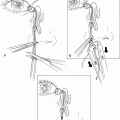
Figure 14-1. A scalpel is used to incise the skin markings, starting with the inferior line. The knife handle is beveled in a cephalad fashion so that it parallels the plane of the emerging superior brow hairs. This prevents transection of underlying follicles, which may result in some hair loss inferior to the healed wound. Beveling of the superior incision must also be done in the same direction so that the wound edges heal properly. The cephalad orientation of the brow incision is less important over the lateral one third of the brow where the hairs tend to lose their caudad orientation. After hemostasis is obtained, excision of skin and underlying subcutaneous tissue is carried out with Stevens or other curved scissors.
There are two alternative methods of skin and soft-tissue excision in direct browplasty.
Most surgeons favor excision of skin and subcutaneous tissue, leaving the frontalis muscle undisturbed. Others feel that excision of underlying orbicularis and frontalis muscle down to the pericranium is desirable to provide a more permanent result and to avoid “bunching up” of the frontalis muscle and resulting contour irregularities. If such a full-thickness excision is carried out, care must be taken to remain superficial in the medial portion of the browplasty that overlies the supraorbital neurovascular bundle. In addition to the risk of damage to the supraorbital neurovascular bundle, excision down to the pericranium also tends to give a more depressed scar. Consequently, it is preferred to excise skin and subcutaneous fatty tissue only, staying just above the frontalis muscle.
Resuspension of the brow
The orbicularis muscle directly beneath the brow (at the inferior edge of the excision) is imbricated to the frontalis muscle at the superior incision border with 4–0 clear nylon sutures. Three to four sutures are placed in an inverted fashion.
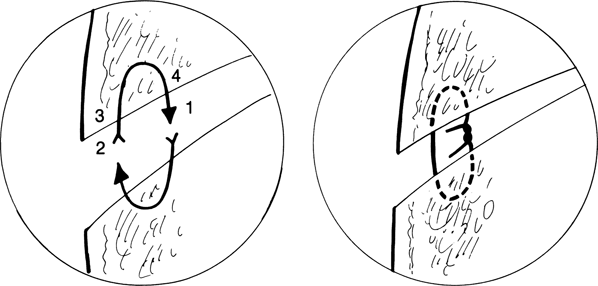
Figure 14-2. Subcutaneous closure is performed with 4–0 chromic sutures placed in an inverted fashion. One must initiate the interrupted suture from a deep entry to a superficial exit, and then a superficial entry to a deep exit, to bury the knot. The suture ends must be cut flush with the knot or they tend to migrate through to the surface of the skin. Meticulous approximation of the subcutaneous tissues in superior and inferior incisions is required to avoid an unnecessarily prominent scar. If the subcutaneous sutures are properly placed, the epithelium should be exactly approximated.
After this subcutaneous closure has been carried out, it is important to inspect the two brows for symmetry. If one brow is lower than the other, the additional skin above the lower brow must be marked in a symmetric fashion with a marking pen, the sutures released, and additional skin excision carried out with repeated layered closure. Intraoperative asymmetry of the brows will persist postoperatively and must be dealt with directly if it is noted.
Once the symmetry of the two brows is assured, skin closure is carried out in two layers. A running 5–0 Prolene subcuticular suture is left in place for 10 days, and then a 6–0 Prolene running baseball closure of the skin is performed, which is removed on the 4th postoperative day. This provides the benefits of a long-lasting skin closure; yet, the most superficial sutures can be removed before the development of cross-hatching.
Postoperative management
Polysporin (bacitracin-polymyxin) ointment is applied to the incision at the completion of the procedure, and ice packs are used for 48 hours. The patient is encouraged to sit upright and to elevate the head during sleep to reduce edema, which can be substantial.
Problems with direct browplasty
The advantages of direct browplasty are its effectiveness and simplicity. The desired contour of the brow can be directly marked on the forehead and effectively achieved. No undermining is required, and bleeding is minimal. Significant disadvantages relate primarily to the contour of the reconstructed brow and the incision placed directly above the brow.
Direct excision of a crescent of skin above the brow will necessarily result in an arched brow. An excision limited to tissue lying within the brow (to hide the scar in the brow hairs) will have no effect on the medial and lateral ends of the brow and its maximum effect at the widest point of excision. The resulting arched or “feminine” eyebrow is not desirable in men. Even in women, when significant brow ptosis exists, an unnatural arch will be created, as a large amount of tissue must be removed centrally above the brow, resulting in a perpetually “surprised” look.
Regardless of the care with which wound approximation and closure is undertaken, the healed incision is frequently more noticeable than one would like. Excision of tissue immediately above the brow results in a wound with thinner forehead skin superiorly and thicker brow skin inferiorly. Closure of these disparate tissues results in some degree of step-off. In addition, the skin adjacent to the medial brow contains prominent sebaceous elements, and when incisions are made in this thicker sebaceous skin, wound contracture with a depressed scar may result. This depressed scar will be even more noticeable if the incision is not beveled and thus transects the follicles deep to the skin, causing additional brow hair loss inferior to the incision, leaving it more exposed. If the incision is properly beveled and placed within the brow to include several rows of superior brow hair, exposure of the incision is less of a problem. For these reasons, a full direct browplasty is now infrequently used.
DIRECT TEMPORAL BROW LIFT
For temporal brow ptosis, which is more prevalent and more likely to infringe on the peripheral field of vision, many patients will benefit from direct excision carried out over the lateral 30% to 50% of the brow. This minimizes depressed scarring, maintains a more horizontal brow contour and is very effective in eliminating the more functionally significant temporal brow ptosis. Such a limited temporal elevation is especially helpful in men, as it will prevent formation of an arched brow contour. Because the forehead skin above the brow becomes thinner temporally and has fewer sebaceous elements, depressed scars are less likely to form. This allows the temporal incision to be carried beyond the lateral end of the brow without concern for camouflage by the brow hair. In addition, there frequently are wrinkles in the temple in which the incisions can be inconspicuously placed.
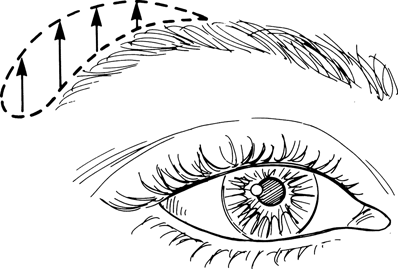
Figure 14-3. The technique is identical with that previously described, except that the skin markings are shifted temporally and sweep to an S-shaped curve temporal to the brow.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree