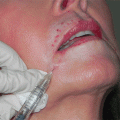
9 Blepharoptosis
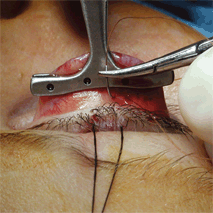
ACQUIRED PTOSIS
Preoperative evaluation
The vast majority of cases of acquired ptosis are aponeurogenic. Nonetheless, the causes of acquired ptosis are diverse, and it is helpful in evaluation and treatment to classify acquired ptosis into the following: aponeurogenic, from involutional or other disinsertional changes in the aponeurosis; myogenic, associated with decreased levator muscle function, as seen in myasthenia gravis or congenital progressive external ophthalmoplegia (CPEO); neurogenic, as seen in third-nerve palsy or Horner’s syndrome; and mechanical, associated with eyelid masses or scarring of the eyelid lamellae. Traumatic ptosis may be considered a separate category, although it actually is a subcategory of each of the foregoing categories.
In the patient workup and evaluation, one must begin with a careful history, with attention to duration and progression of ptosis, daily variation in the severity of ptosis, and any history of dry eye complaints. Examination should focus on determining the severity of ptosis, levator function, lid crease height, and coexisting eye problems, such as lower eyelid retraction, overhanging skin on the upper lid, or contralateral upper eyelid retraction, creating a pseudoptosis on the side in question. Clinical features of a patient with acquired aponeurosis disinsertion consist of good levator function, higher than normal eyelid crease, and a ptotic eyelid that assumes a lower position on down gaze. If a history consistent with myasthenia gravis is suspected, tests for fatigability as well as an edrophonium (Tensilon) test should be performed. The examiner should be cognizant of the frequency of bilateral ptosis that is more apparent on one side. Because of the equal innervation to both levator muscles, correcting only one upper lid may result in worsening the appearance of ptosis on the opposite side. This phenomenon follows Hering’s law and is especially frequent in aponeurogenic ptosis.
Indications for surgery
Adult ptosis is typically symptomatic, whether the complaints relate to visual obstruction or a tired, inattentive appearance. A patient may also complain of forehead fatigue caused by constant brow elevation in an effort to help lift a ptotic eyelid. If repair is being performed for functional indications, it is vital to document the severity of ptosis with diagrams, facial photographs, and perimetry, showing the superior visual field constriction produced by the ptosis. It is also helpful to have photographs and notes available for reference at the time of surgery. A ptosis repair may be performed in most patients at any time. After trauma, it is prudent to wait 6 months before ptosis repair, as function may improve during that time. In myasthenia gravis, or any medical or neurologic condition that may remit with therapy, it is wise to delay surgery until the condition is stable and optimally controlled.
Making procedural choices
With few exceptions, acquired ptosis can be treated by an aponeurotic resection or repair. An external aponeurotic approach directly treats the most common cause for acquired ptosis, aponeurotic rarefaction, or disinsertion. Aponeurotic surgery is also the preferred approach in myogenic or neurogenic ptosis with adequate levator function.
The mullerectomy procedure described by Urist and Putterman provides predictable correction of ptosis based on response to a phenylephrine test in the ptotic eyelid. The simplicity of this procedure and ability to perform formulaic surgery predicted by a pharmacologic test make this technique popular.
Frontalis suspension procedures (see section on “Congenital Ptosis”) may be required in severe neurogenic, myogenic, or traumatic ptosis with the loss of levator function. In acquired unilateral ptosis with poor levator function, it is unnecessary to extirpate the contralateral levator and then suspend both lids. It is much easier for an adult without long-standing visual suppression to learn to use brow function to help elevate a ptotic eyelid. When performing sling procedures or aponeurotic surgery on individuals with ptosis associated with weak eyelid closure (CPEO, myasthenia gravis), one must avoid overcorrection and exposure keratopathy.
Surgical procedure
Aponeurotic resection
The eyelid crease is generally marked along the entire eyelid to correspond with the natural skin crease of the opposite upper lid. In selected adult patients with good levator function, the repair can be accomplished through a small central 12 to 15 mm incision. Anesthesia is obtained by subcutaneous infiltration along the preplaced skin marking with 0.5 to 1.5 ml of 2% lidocaine with 1:100,000 dilution of epinephrine. It is important not to inject too deeply into the eyelid, thereby anesthetizing Müller’s muscle, which can influence intraoperative lid height adjustments. Topical tetracaine is instilled onto the cornea.
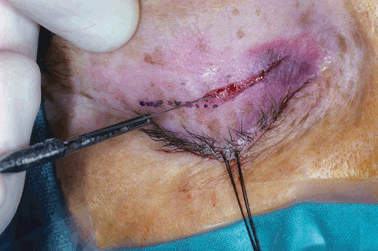
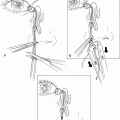
Figure 9-1. After subcutaneous infiltration, a 4–0 double-armed silk traction suture is placed at the central upper lid margin and secured to the surgical drape below with a hemostat. The suture is placed through the gray line at the lid margin to avoid the marginal arcade, thereby preventing unnecessary bleeding. When secured inferiorly, this traction suture puts all eyelid structures posterior to the orbicularis muscle on tension, while allowing the anterior lamella to be mobilized. The skin is incised along the previously marked lid crease with a scalpel.
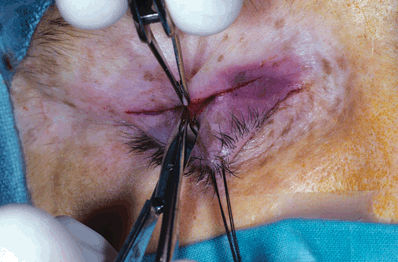
Figure 9-2. The orbicularis is tented anteriorly with a toothed forceps, and its full-thickness is incised centrally with a Westcott scissors oriented perpendicularly.
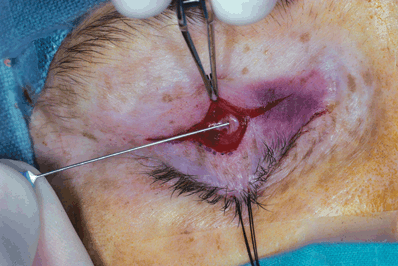
Figure 9-3. It is a key maneuver in this technique to make a full-thickness incision through the orbicularis muscle, as this avoids unnecessary bleeding from multiple cuts into the muscle and permits identification of the avascular posterior orbicular fascial plane (needle).
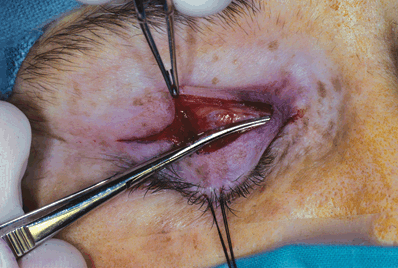
Figure 9-4. One blade of a scissors is then passed bluntly into the avascular plane, and the incision is completed medially and laterally. The superior edge of the incision is retracted upward with a skin hook, and the disinserted edge of the levator aponeurosis can oftentimes be identified through the translucent postorbicular fascia. The postorbicular fascia is recognized as a delicate layer overlying the aponeurosis. In this fascial plane, vertically oriented peripheral nerve fibers can sometimes be seen. Further dissection is required to expose the levator aponeurosis.
While retracting the superior edge of the incision with a double-pronged skin hook, gentle pressure is applied on the globe. With retrograde orbital pressure, the preaponeurotic fat pad bulges forward to tent up the orbital septum.
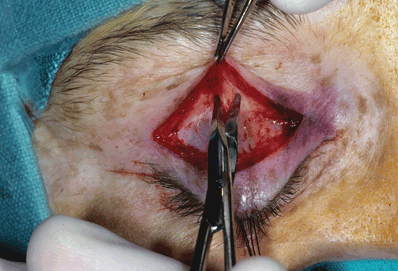
Figure 9-5. A horizontal incision is made with a Westcott scissors to buttonhole the orbital septum above its fusion with the aponeurosis. The incision should be directed superiorly to avoid transecting Müller’s muscle or the conjunctiva. This allows the preaponeurotic fat to herniate through the buttonhole. The entire orbital septum is then opened by placing one blade of the scissors behind the orbital septum and extending the incision medially and laterally.
The foregoing maneuvers are important to identify the preaponeurotic fat pad and to avoid making iatrogenic defects in the aponeurosis.
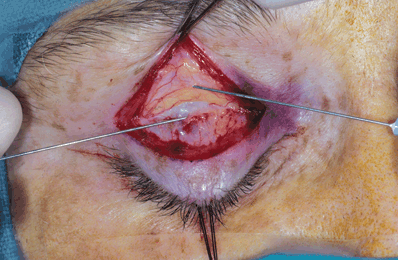
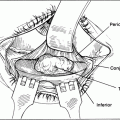
Figure 9-6. The skin and orbicularis muscle are retracted with a forceps. The preaponeurotic fat pad (indicated by the top needle) is the key anatomic landmark in this surgery, since the levator aponeurosis is located immediately beneath this structure (lower needle). Müller’s muscle lies immediately under the levator aponeurosis. In cases of repeated operation, trauma, or in eyelids infiltrated by tumor, such as neurofibroma, the preaponeurotic fat pad may be the only identifiable structure.
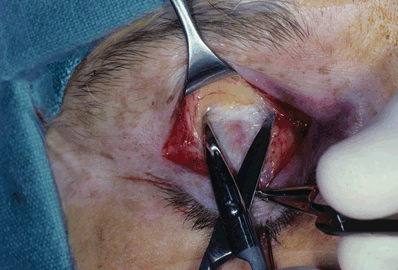
Figure 9-7. The preaponeurotic fat pad is retracted superiorly with a Desmarres retractor, and fine attachments to the underlying levator aponeurosis are lysed with a Westcott scissors.
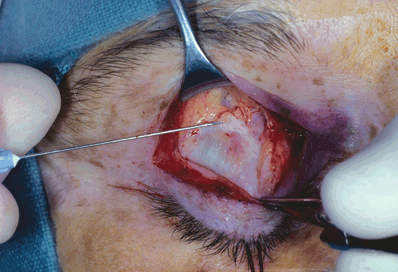
Figure 9-8. The disinserted edge of the levator aponeurosis is grasped with forceps. When the patient is asked to look superiorly, the surgeon can feel the force generated against the forceps, confirming the structure to be the aponeurosis. The Whitnall’s ligament can be seen at the superior limit of the aponeurosis (needle tip). Frequently, the disinserted edge of the aponeurosis can be recognized.
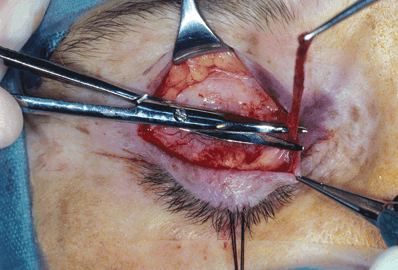
Figure 9-9. A strip of pretarsal orbicularis muscle, at the superior margin of the tarsus, is excised by bluntly undermining with a Westcott scissors, thus baring the anterior surface of the tarsal plate. In ptosis cases in which the levator aponeurosis is intact, the appropriate amount of aponeurosis is resected with Westcott scissors. In patients in whom a rarefaction or dehiscence of the aponeurosis is present, it is important to excise the rarefied area to create a free healthy muscle edge for anchoring onto the tarsal plate.
If the aponeurosis has been disinserted, the disinserted edge is grasped with a forceps and sutured to the anterior surface of the tarsal plate. If there has been no obvious disinsertion, the aponeurosis is then detached from the upper border of the tarsal plate. The peripheral vascular arcade in Müller’s muscle helps to identify this structure. If bleeding occurs in this plane, one should pick up the tissue with the bipolar tip before cauterizing, thereby preventing thermal injury to the underlying cornea.
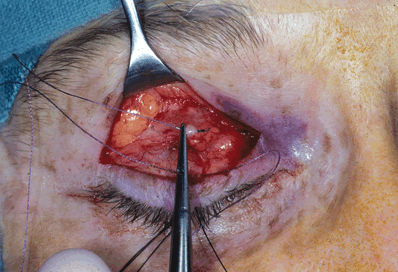
Figure 9-10. Once the full expanse of the aponeurosis has been separated from the tarsal plate and the appropriate amount of aponeurosis resected, it is then reattached onto the upper midportion of the tarsal plate with a 5–0 polyglactin 910 (Vicryl) suture on a spatula needle. A spatula needle facilitates a partial-thickness tarsal pass; the lid may be everted to confirm that full-thickness passes have not occurred. Full-thickness tarsal sutures should be avoided to prevent buckling of the tarsal plate and corneal abrasion. The first suture is placed just medial to the pupil, which is the highest point of the normal eyelid. The aponeurosis should be advanced and firmly fixed to the tarsus with a temporary tie first. “Tucking” of the aponeurosis does not result in a permanent correction, as no raw surfaces are opposed. The aponeurosis should be resected in all cases, except a complete disinsertion, to create a healthy, strong edge to suture to the tarsus. If the aponeurosis is advanced too low on the tarsal plate, eversion of the eyelid margin may occur.
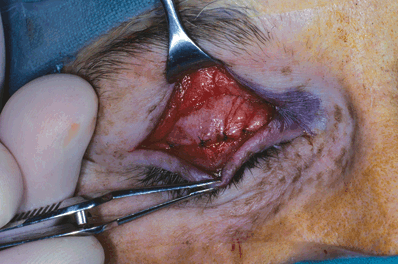
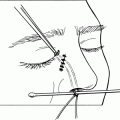
Figure 9-11. After the central suture placement, additional sutures are placed medial and lateral to the central suture to adjust eyelid contour and height.
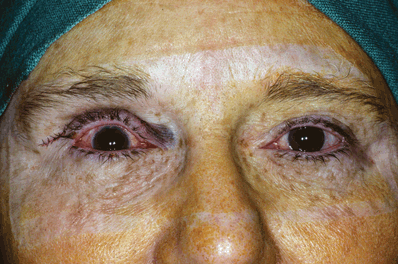
Figure 9-12. The lid height should be overcorrected about 1 to 1.5 mm at surgery to compensate for anesthetic paralysis of the orbicularis and to counteract a slight postoperative fall. When local anesthesia is used, the lid height and contour should be evaluated while the patient sits upright on the operating table. Eyelash position and the lid crease should be evaluated at the same time. Once the lid height and contour are judged to be satisfactory, additional sutures are used to firmly secure the aponeurosis to the tarsal plate. The eyelid is then everted to look for any exposed sutures on the tarsoconjunctival surface.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree