31 Anterior Orbitotomies
There are important fundamental prerequisites to successful orbital surgery. The surgeon must have a thorough working knowledge of orbital anatomy, orbital diagnosis and diseases, and orbital diagnostic imaging techniques, including computed tomography (CT) scan, ultrasound (echography), and magnetic resonance imaging (MRI).
Modern orbital surgery is deliberate meticulous microsurgery performed in a bloodless field. Preoperative localization and assessment combined with excellent intraoperative exposure and direct visualization will be emphasized as the key elements toward safe and successful orbital surgery.
PREOPERATIVE DECISIONS
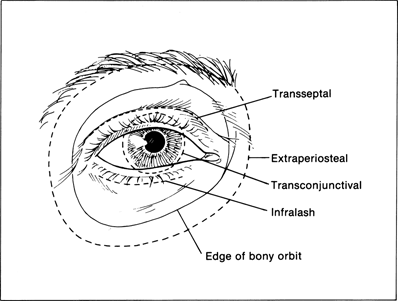
Figure 31-1. Localization will generally determine which surgical approach is used. Lesions palpated anteriorly in the orbit are usually approached through a transseptal (translid) orbitotomy. If CT scan, ultrasound, or MRI demonstrates the lesion to be in the posterior orbit, an extraperiosteal approach is chosen to safely gain access to the deep orbit. Intraconal lesions located between the medial rectus muscle and optic nerve are approached through a transconjunctival medial orbitotomy.
Assessment of the nature of the lesion will modify the surgical approach that has been chosen, based on localization only. Proper preoperative assessment is critical toward formulating the correct surgical plan. Thus, the “goals” of orbital surgery are determined preoperatively (Table 31-1). The surgeon must assess whether the lesion represents a localized or diffuse process. A plan for total excision is formulated if a localized tumor is present. Diffuse infiltrative tumors are approached for diagnostic biopsy only.
Kersten RC, Kulvin DR. Vertical lid split orbitotomy revisited. Ophthal Plast Reconstr Surg 1999;15:425.
The patient is instructed to discontinue aspirin products 10 to 14 days preoperatively. Control of hypertension is very important, and general medical evaluation is sought when necessary. Patients are asked not to drink alcohol within 2 days of the surgery. Oral corticosteroids are commonly given to the patient the night before surgery to help reduce the postoperative swelling and inflammation.
SURGICAL TECHNIQUE
Transseptal anterior orbitotomy
The transseptal or translid orbitotomy is perhaps the simplest of the anterior orbitotomies. The transseptal approach may be performed in the upper eyelid or the lower eyelid. The transseptal anterior orbitotomy is most commonly used to treat lesions that are visible within the substance of the eyelid or palpable within the anterior orbital space.
This surgical approach is commonly used for excision if the lesion is well demarcated (e.g., dermoid cyst or cavernous hemangioma), for diagnostic biopsy if the lesion is diffuse and infiltrative (e.g., inflammatory pseudotumor or metastatic carcinoma), and for drainage (e.g., infectious abscesses within the anterior orbit).
The transseptal anterior orbitotomy may be performed under local or general anesthesia. The more localized anterior tumors are most amenable to excision under local anesthesia. Straight local anesthesia may fail to achieve the desired effect in patients with larger infiltrative tumors of the orbit. The surgical site is infiltrated with lidocaine 2% with 1:100,000 epinephrine. Adequate time is allowed for the hemostatic effect of epinephrine to begin before any incisions are made. The mixture of lidocaine 2% with epinephrine is infiltrated locally; even in cases in which general anesthesia is used. The addition of 150 units of hyaluronidase into the mixture of local anesthetic allows the rapid dissolution of the mixture and prevents the local anesthetic from causing any undue distortion of the tissues.
In the upper eyelid, the transseptal orbitotomy incision line is concealed within the upper eyelid crease. After marking the lid crease incision, the skin incision is made with a size 15 blade. A hard corneal protector is used. With the lid held under tension, the orbicularis muscle layer is incised across the width of the lid. Meticulous hemostasis is maintained during all phases of the procedure. Gentle pressure placed on the globe will prolapse the orbital fat forward and bulge the orbital septum forward. Sharp dissection is used to open the orbital septum across the entire width of the upper eyelid. One may take a biopsy of the lesion, excise the entire lesion, or drain an abscess if present. Closure of the transseptal anterior orbitotomy involves re-formation of the upper eyelid crease. This re-formation is accomplished by suturing the pretarsal skin muscle edge to the levator aponeurosis. Three cardinal sutures are adequate to form a good eyelid crease. The remainder of the myocutaneous incision is closed with running or interrupted sutures. In situations during which a moderate amount of postoperative oozing of blood is anticipated, interrupted sutures are selected. In procedures for which drainage of an orbital abscess was involved, a postoperative drain is left in place for 24 to 48 hours.
The lower eyelid transseptal anterior orbitotomy is very similar, in principle, to the upper eyelid procedure. The surgical site is infiltrated with lidocaine 2% with epinephrine and hyaluronidase, allowing adequate time for onset of the hemostatic effect. The translid incision is made within 1 to 2 mm of the lower eyelid lashes. Following the skin incision, the orbicularis muscle is incised across the width of the eyelid.
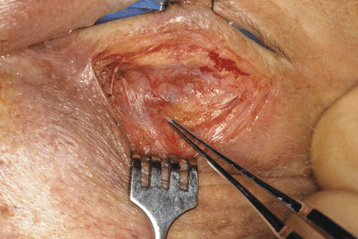
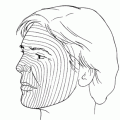
Figure 31-2. The entire lower eyelid myocutaneous flap is then elevated using sharp and blunt dissection and retracted downward with multiple rake retractors. The anterior orbital lesion is either palpated or visualized at this point.
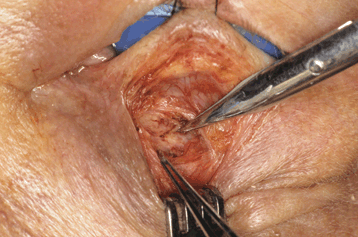
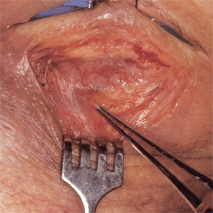
Figure 31-3. The orbital septum is “tented” with fine forceps. It is then opened widely with Westcott scissors to expose the lesion.
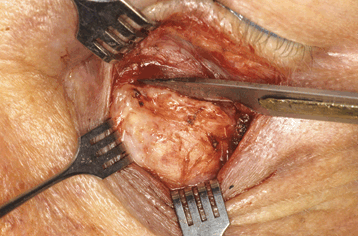
Figure 31-4. Surgical retractors or traction sutures are used as is necessary to achieve good exposure. A large tumor mass is exposed in the anteroinferior orbital space. As with the upper eyelid transseptal orbitotomy, the lesion at this point is biopsied, excised, or drained. The lower lid incision is closed with running or interrupted sutures. Some patients are susceptible to developing postoperative lower eyelid ectropion following this simple transseptal orbitotomy. Such patients include those with significant horizontal laxity of the eyelid and patients with long-standing infiltrative tumors in whom extensive biopsies are performed. In these patients, the use of postoperative temporary tarsorrhaphy sutures or upward traction sutures through the lower lid margin may help avert postoperative ectropion.
Tumor biopsy for purpose of diagnosis is among the most common indications for anterior orbitotomy. Although the technical aspects of the surgery are of utmost importance, the surgeon should discuss the diagnostic possibilities with the pathologist, and a mutual understanding should be reached before surgery concerning proper tissue handling for the specific case.
In many circumstances, standard formalin tissue fixation is adequate. Alternatively, if a lymphocytic tumor is suspected, fresh (nonfixated) tissue must be sent to the pathologist for immunologic marker studies. With lymphomas, it is important to obtain a deep incisional biopsy into the tumor as well as to obtain a large biopsy specimen. Lymphomatous tumors may be composite, and sampling errors may occur if smaller biopsy specimens are submitted for cell surface immunoglobulin studies. Fresh tissue is also necessary for all immunofluorescent, immunoperoxidase, and immunohistochemical enzyme studies. Estrogen receptor assays are similarly performed on unfixed tissue; this assay is important if metastatic breast carcinoma is known or suspected. It is important that the surgeon knows the minimum volume of tissue required to perform the estrogen receptor assay. This information is gained by contacting the appropriate pathologist preoperatively. With orbital tumor biopsy specimens, obtaining an adequate volume of tissue can be difficult.
If the orbital tumor is a metastasis of unknown primary source, consider fixing a tissue specimen in glutaraldehyde for transmission electron microscopy. A 2 × 2 × 2-mm biopsy is adequate for electron microscopy. It is a common error to place too large a biopsy specimen in glutaraldehyde; the end result of this may be uneven or poor tissue fixation. The electron microscopy findings “may” elucidate the source of the primary tumor in many situations, including neuroblastoma (neurosecretory dense-core vesicles and neurotubules), breast carcinoma (mucin-producing cells or secretory granules), renal cell carcinoma (glycogen granules or lipid inclusions), oat cell carcinoma or carcinoid tumor (electron-dense granules), metastatic melanoma (cytoplasmic premelanosomes), colon carcinoma (elaborate cellular brush border), and bronchogenic carcinoma (Clara cells of alveoli).
The ongoing advances in tissue diagnosis occur rapidly, and a careful review of the subject is warranted each time the situation arises.
Transconjunctival anterior orbitotomy
The transconjunctival surgical approach allows the simplest and most direct access to lesions located in the subconjunctival space and lesions in the anterior portion of the orbit located outside the muscle cone. This approach can be applied to any quadrant of the globe. The transconjunctival orbitotomy can be used to gain access to the intraconal space by disinserting the appropriate rectus muscle. This approach to the intraconal space is most commonly performed medially.
The transconjunctival orbitotomy remaining outside the muscle cone is commonly performed to drain a localized abscess, to partially resect a benign tumor, and to biopsy a malignant tumor. Indications for the intraconal transconjunctival orbitotomy with disinsertion of the medial rectus muscle include excision of localized tumors (e.g., cavernous hemangioma or neurilemoma), excision or biopsy of primary optic nerve tumor (e.g., glioma or meningioma), and decompression of the optic nerve sheath.
The transconjunctival orbitotomy for an extraconal lesion is performed under local or general anesthesia, when appropriate. An adequate conjunctival peritomy is made for good exposure in the appropriate quadrant. Relaxing incisions are made in the conjunctiva at each end of the peritomy. Biopsies are taken of infiltrative tumors, with appropriate handling of the specimen. Localized abscesses are drained. Other benign tumors, such as lipodermoids, are partially resected. It is important to limit the resection of these lesions to the proximal portion overlying the epibulbar surface. Overzealous excision of such lesions carried up under the eyelid or into the posterior orbit can result in significant complications. These complications include hemorrhages that are difficult to control, severe symblepharon formation, and ptosis of the upper eyelid, because of either levator damage or cicatrization. The conjunctiva is closed with loose interrupted sutures to permit postoperative drainage. In treating orbital abscesses, the use of a thin transconjunctival Penrose drain as well as appropriate subconjunctival antibiotic injections is indicated.
The medial transconjunctival orbitotomy is among the most difficult of the orbital surgeries. The complications of optic nerve damage and visual loss are real. Although good exposure is important for all orbital surgery, it is especially important for medial orbitotomy of the intraconal space. It is critically important to recognize important anatomic landmarks. The vortex veins number between four and eight and lie 5 to 8 mm posterior to the equator of the globe. They are close to the vertical meridian and are most commonly seen in the temporal quadrants. The short posterior ciliary arteries branch from the ophthalmic artery to encircle the optic nerve. The paired long posterior ciliary arteries also course on either side of the optic nerve.
Violation of any of these vascular structures can lead to serious hemorrhaging, which could jeopardize the surgical procedure or visual function of the eye. The surgeon must remain patient and meticulous in all phases of this orbitotomy, always maintaining good exposure and direct visualization.
The medial transconjunctival orbitotomy is most commonly performed under general anesthesia. The surgeon will, nonetheless, infiltrate the subconjunctival space with local anesthetic containing epinephrine. As with other orbitotomies, the head of the bed is elevated 15° to 20° to decrease venous congestion of the head and orbit. The medial conjunctival peritomy should be a “full” 180°.
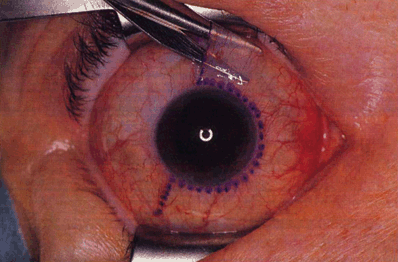
Figure 31-5. A transconjunctival medial orbitotomy incision line has been outlined in methylene blue. A Westcott scissors has been introduced to undermine the conjunctiva and begin the peritomy. Smaller conjunctival incisions may limit the exposure. A conjunctival relaxing incision is made superiorly and inferiorly and the edges of the conjunctiva tagged with suture. Gentle blunt and sharp dissection of Tenon’s fascia is performed to expose the medial rectus tendon. The tendon is gathered on a muscle hook and good exposure of the medial rectus is obtained. The medial rectus muscle is traced posteriorly to its point of penetration through Tenon’s capsule.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree