36 Myectomy Surgery for Essential Blepharospasm
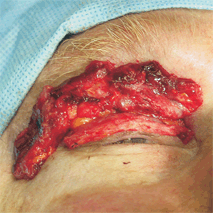
INTRODUCTION
Benign essential blepharospasm is a form of focal dystonia with involuntary contractions of the eyelid protractors. Since its approval by the FDA in 1989, serial injections of botulinum toxin type A have become the first-line therapy targeting the involuntary protractor spasms associated with essential blepharospasm. While the injections do provide a relatively safe, nonsurgical treatment option, many patients are not adequately controlled with botulinum-A toxin injections alone. This may be due to associated apraxia of eyelid opening, progressive worsening of their disease, or development of immunoresistance to the botulinum toxin. Botulinum-A toxin injections also do not address the many eyelid deformities associated with essential blepharospasm such as brow ptosis, dermatochalasis, blepharoptosis, entropion, and blepharophimosis. These eyelid deformities may in fact worsen or become more pronounced after treatment with botulinum-A toxin injections.
Eyelid protractor myectomy involves extirpation of the orbicularis oculi and corrugator supercilii muscles. It can be performed in the upper eyelids alone or in both the upper and lower eyelids. The procedure is an extremely effective treatment for blepharospasm patients inadequately managed with botulinum toxin injections alone. Not only does the procedure alleviate much of the eyelid spasms, but the associated eyelid deformities can also be concurrently addressed with levator aponeurotic advancement, removal of excess tissues, and horizontal eyelid tightening. Protractor myectomy also avoids the complications associated with facial nerve avulsion such as facial paralysis, lower eyelid ectropion, and high recurrence rates. Patients who are unwilling to undergo long-term serial injections may also benefit from eyelid protractor myectomy. While most commonly used in the treatment of essential blepharospasm, eyelid protractor myectomy can also be performed in patients with hemifacial spasm who are unwilling or unable to undergo neurosurgical decompression of the facial nerve root and unable to be adequately treated with serial botulinum toxin A injections.
PREOPERATIVE EVALUATION
Prior to considering myectomy surgery, the patient should undergo a complete ophthalmic examination with particular attention to the ocular surface and lacrimal function. Many patients develop lagophthalmos in the immediate postoperative period; therefore, any preexisting lacrimal dysfunction or ocular surface pathology should be identified and maximally treated prior to undergoing myectomy surgery.
Since the eyelid musculature is extremely vascular, the patient must avoid anticoagulative medications prior to surgery. These medications include acetylsalicylic acid (aspirin), aspirin-containing products such as Alka-Seltzer, nonsteroidal anti-inflammatory medications such as ibuprofen (Motrin, Advil) and naproxen (Aleve), warfarin, heparin, low-molecular weight heparin, and other platelet inhibitors such as clopidogrel (Plavix). Nonprescription medications such as high-dose vitamin E, ginko biloba, and ginseng have also been reported to have anticoagulative properties. Uncontrolled hypertension can also result in excessive bleeding; blood pressure control is mandatory both during the surgical procedure and postoperatively as well.
Most essential blepharospasm patients that undergo surgical eyelid myectomy have already received treatment with serial injections of botulinum toxin A. Since there can be significant postoperative edema associated with the myectomy procedure, botulinum toxin A injection in the perioperative period can result in unexpected spreading of the medication to undesired locations such as the midface or lower face. In planning for an eyelid myectomy, regardless if it is upper eyelid or lower eyelid or both, it is best to avoid botulinum toxin A injections for at least 2 weeks prior and 2 weeks after the surgery.
SURGICAL TECHNIQUE
Skin marking
When performing the upper eyelid myectomy, an eyelid crease incision similar to that used in upper eyelid blepharoplasty may be used. As most patients with long-standing essential blepharospasm will also have some degree of dermatochalasis, a conservative skin excision can also be marked; however, the surgeon must be judicious in skin removal as aggressive excision may exacerbate postoperative lid closure. When performing the lower eyelid myectomy, a subciliary incision should be used and no skin excision should be planned to avoid the risk of postoperative lower eyelid retraction.
Regardless of whether the patient is to have general anesthesia or local anesthesia, use of infiltrative local anesthetic with epinephrine is necessary to provide adequate hemostasis during the procedure. Lidocaine 2% with 1:100,000 dilution of epinephrine is infiltrated in the subdermal plane using a 27-gauge needle for the entire extent of the myectomy. The injection should be performed several minutes prior to surgery to achieve adequate vasoconstriction prior to the incision. The patient is then prepared and draped in a manner similar to that of a blepharoplasty procedure.
Skin incision
The skin incision over the previously placed markings is performed with a No. 15 Bard-Parker blade. This incision is made with a technique identical to what one would use for a standard blepharoplasty procedure. Excision of the skin and orbicularis muscle corresponding to the area previously demarcated is then performed using Stevens scissors. It is preferable to leave the underlying orbital septum intact at this time. After excising the demarcated skin and muscle flap, the orbital septum should be left intact to prevent prolapse of preaponeurotic fat and minimize the risk of inadvertent injury to the levator aponeurosis.
The eyelid protractor myectomy involves extirpation of the pretarsal, preseptal, and a portion of the orbital orbicularis oculi muscle. The corrugator supercilii muscle is also a strong protractor and should be excised during the procedure as well. In most patients with essential blepharospasm, the upper eyelid myectomy is adequate to provide significant relief of their eyelid spasms. In severe cases where eyelid spasms persist after the upper eyelid myectomy, a lower eyelid myectomy of the pretarsal and preseptal orbicularis oculi muscle should then be performed.
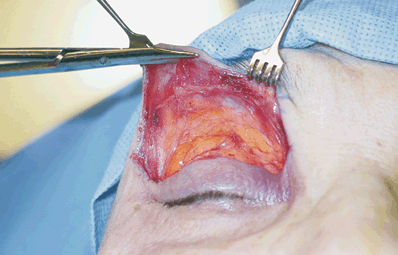
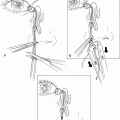
Figure 36-1. Using two rake retractors, the skin superior to the incision should be placed on tension and Stevens scissors can then be used to create a dissection plane between the preseptal orbicularis oculi muscle and the overlying dermis. The subdermal dissection plane is extended superiorly above the orbital rim and eyebrows to allow extirpation of a portion of the orbital orbicularis oculi.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree