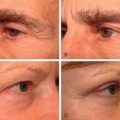
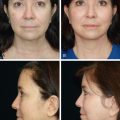
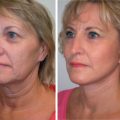
History
The history of facial rejuvenation has mainly focused on addressing cervicofacial laxity. In 1919 Bettman and Bourget simultaneously presented their experience with subcutaneous rhytidectomy . In 1960 Aufricht was the first to describe plication of the tissue deep to the superficial fat plane . Webster and other facelift surgeons used similar techniques of suturing the “deeper layers” to improve their results . During the same period Skoog had started performing facelifts utilizing the skin and platysma as a musculocutaneous advancement flap . In 1976 Mitz and Peyronie advanced the rhytidectomy procedure into the modern era by describing the anatomy of the superficial musculoaponeurotic system (SMAS) . They showed that a deeper fascial tissue layer exists between the subcutaneous fat and the parotidomasseteric fascia. Their anatomic studies established that the SMAS invests the muscles of facial expression and is contiguous with the frontalis and platysma muscles. Following Mitz and Peyronie’s description, the incorporation of the SMAS layer in cervicofacial rhytidectomy gained significant popularity . In the 1990s, the deep plane facelift and subperiosteal facelift also became increasingly used, specifically to address nasolabial folds . The deep plane rhytidectomy eventually became touted as the gold standard among all facelift techniques.
It was not until the latter half of the 20th century when surgeons started considering that facial rejuvenation requires three-dimensional considerations. In the 1970s Hinderer published studies on the use of alloplastic implants for chin and cheek skeletal enhancement . In the 1980s Binder introduced the concept of using midface implants for three-dimensional volume restoration and facial rejuvenation . The introduction of liposuction by Illouz in the 1980s gradually led to the use of autologous fat grafting for soft tissue augmentation, which was further advanced by Coleman and Glasgold in the 1990s and 2000s . In the 2000s and 2010s, Pessa, and Mendelson elucidated through elegant anatomic and radiographic studies that the aging process is not just due to gravitational laxity, but perhaps more importantly related to changes in the superficial and deep facial fat compartments, as well as facial skeletal remodeling .
Personal Philosophy
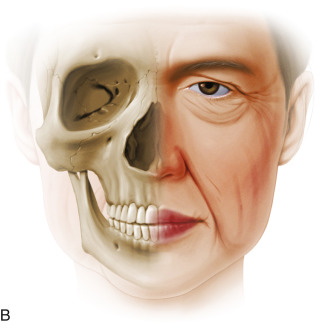
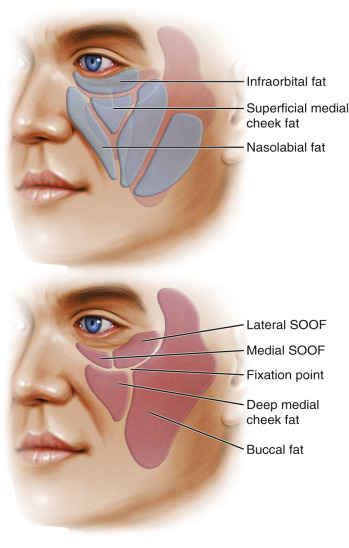
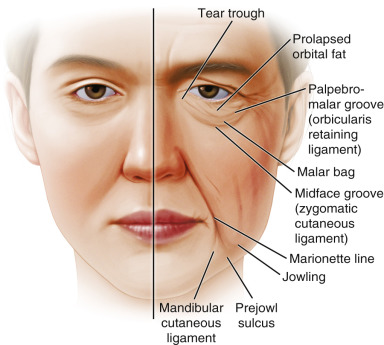
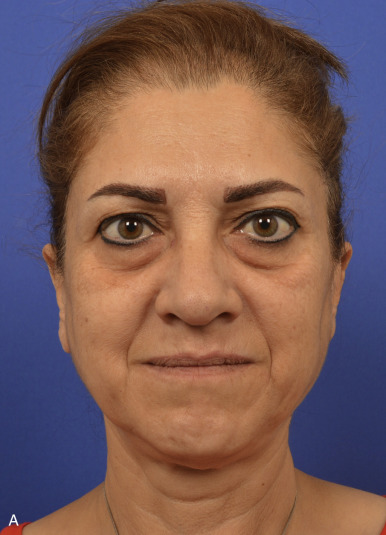
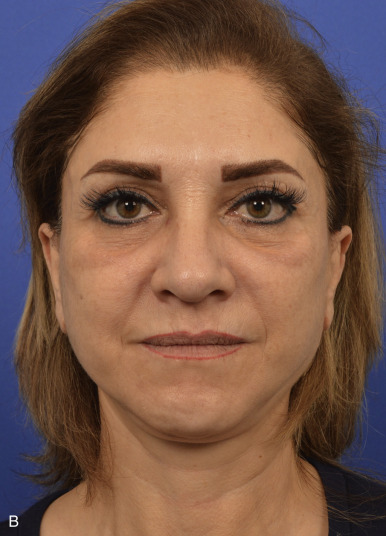
Aging is a multifactorial process that affects the skin, subcutaneous, and deep fat compartments, as well as the craniofacial skeleton ( Figs. 19.1–19.4 ) . The ultimate goal of facial rejuvenation is to improve the appearance of patients in a natural, youthful, attractive, and appropriate manner. Over the past decade, the author’s view relating to rhytidectomy as the cornerstone of facial rejuvenation has significantly changed due to a much better understanding of the anatomic changes that occur in the aging process . The principles of “facial anatomic subunits” that have long been the guiding principles in facial and nasal reconstruction but rarely considered in aesthetic procedures are now utilized by the author to improve the facial shape and surface topography of patients, as well as to create smooth transitions between the temple, zygomatic arch, lateral cheeks, lower eyelids, anterior midface, buccal space, mandibular jaw line, and neck to obtain ideal results ( Figs. 19.5 – 19.6 ) .

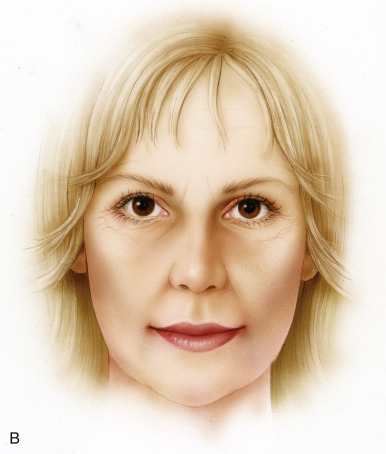
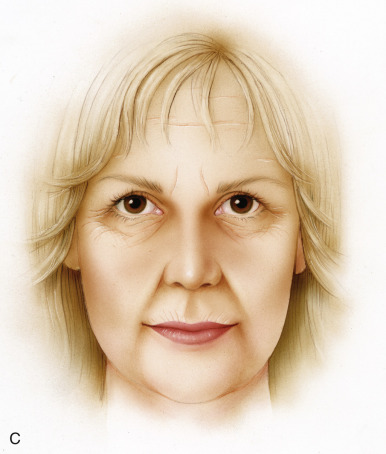
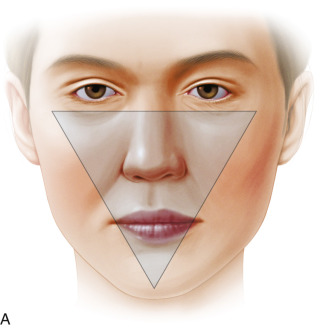
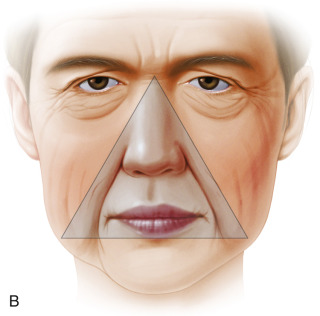
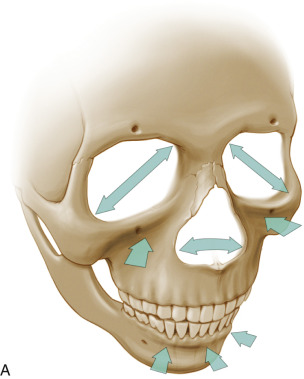
Henceforth, the rhytidectomy technique and complementary procedures should be modified to address a more holistic approach to facial rejuvenation. Whereas in the past, rhytidectomy was a standardized procedure performed in a cookie-cutter fashion for all patients with aging faces, it is now a customized procedure and just one of many tools in our armamentarium for comprehensive facial rejuvenation. Procedures such as autologous fat grafting, chin augmentation, conservative periorbital rejuvenation, and buccal space modification are often utilized in conjunction with rhytidectomy to create facial harmony and enhance youthful contours and shape . Today, we modify the SMAS technique, undermining, and suspension vectors to not only address jowls, cervicofacial laxity, and platysmal banding, but also to restore the triangle of youth that is more “heart shaped” and aesthetic .
The key components of our rhytidectomy procedure include limited skin undermining in the facial region, tunneling the undissected facial and cervical tissue with a cannula to create pockets of mechanical adhesions in the healing process, customizing the extent of sub-SMAS dissection depending on the desired outcome, performing the SMAS suspension in a vector that provides appropriate lifting and reshaping of the face, implementing horizontal platysmal myotomy at the level of cervicomental junction with corset platysmaplasty for individuals with prominent banding, and using judicious cervical suction-assisted lipectomy. By limiting facial skin flap dissection, we maintain the anterior dermal-SMAS attachments, which allow aggressive suspension of the face without significant tension on the skin . The SMAS serves as the carrier of the facelift flap. The undissected areas could safely undergo simultaneous cutaneous skin resurfacing and autologous fat grafting to address photodamage, fine or deep rhytids, volume restoration, as well as reshaping a more youthful appearance.
The vector of SMAS suspension is typically more posteriolateral in gaunt patients with major rhytids and vertical in individuals with a round, square, and rectangular facial shape. This approach addresses all aspects of the aging process beyond just cervicofacial laxity.
We have found our rhytidectomy technique to produce an extremely reasonable operative time, minimal complication rate, and postoperative recovery time. By limiting the subcutaneous dissection, the risk of facial hematoma formation and facial nerve injury is also likely reduced. Short skin flaps diminish the chance of flap necrosis in patients who have compromised vascularity, such as smokers, diabetics, and elderly patients . We have also seen less long-term skin atrophy and telangiectasias.
The general criticism of SMAS facelift in the 1980s and 1990s was that it did not address the “midface,” since it did not “flatten” the nasolabial fold. In that era, effacement of the nasolabial fold was an important goal of facelifts. In the past decade, our enthusiasm for effacing the nasolabial fold for midface rejuvenation has been largely replaced by facial reshaping and volume modification using the aesthetic subunit approach. The author no longer arbitrarily separates the upper, mid, and lower face. We focus more on the entire face as a continuum and look at creating soft transitions between the various facial subunits to address double-cheek convexity, infraorbital rim hollowness, tear trough deformity, retrusion of pyriform aperture, as well as the lateral cheek and buccal space disproportion. This approach results in a more natural facial aesthetic that creates an appropriate lateral projection of the zygomatic arch, restores an attractive facial shape, and improves the youthful arcs and highlights of the face . Our methodology is to combine a customized SMAS facelift with autologous fat grafting, fillers, conservative transconjunctival lower blepharoplasty (with or without fat repositioning), buccal space modification (augmentation or reduction), and preauricular volume adjustment (typically augmenting in skeletonized faces and narrowing in patients with round, square, or rectangular facial shape). Alloplastic midface and angle of the mandible implants may also be considered for patients with significant volume deficits, but must be used with caution due to potential risk of infection and steep learning curve .
Long-flap facelifts (SMAS or subcutaneous techniques) incorporating extensive skin undermining have long been advocated as a way of releasing the fascioosteocutaneous ligaments . In attempting to accomplish the ligamentous release, extensive flap elevation in the subcutaneous plane can destroy the dermal-SMAS attachments, hence invalidating the SMAS support for the lift. Anatomic studies by Muzaffar and Mendelson have also demonstrated that the release of retaining ligaments in the prezygomatic space through extensive subcutaneous dissection can potentially cause nerve injury to the motor branch of the orbicularis oculi . It is also well known that the facial nerve has a more superficial course near the oral commissure and midportion of the zygomatic arch, placing it at risk during the dissection of long skin flaps . If a surgeon desires release of the fascioosteocutaneous ligaments, we recommend utilizing the sub-SMAS plane, which can easily be done with the current technique.
The deep plane facelift also incorporates a short skin flap elevation and is an excellent rhytidectomy method. The true deep plane or composite facelift, however, does not have significant flexibility and requires complete sub-SMAS dissection over the zygomatic major muscle all the way to the nasolabial fold in all patients, regardless of their aging process and aesthetic goals . A lengthy anteromedial dissection can cause extensive postoperative edema as well as place the branches of the facial nerve at risk in every patient. In our experience as well as that of others, the results of the deep plane facelift and a well-executed SMAS rhytidectomy are similar, with the exception of outcomes in older patients with extensive rhytidosis . The outlined SMAS rhytidectomy may incorporate a significant sub-SMAS dissection similar to deep plane rhytidectomy benefiting older patients with significant cervicofacial laxity; however, it is customized to the aging process of the patient in terms of vector of suspension and extent of sub-SMAS dissection.
Facial Anatomy
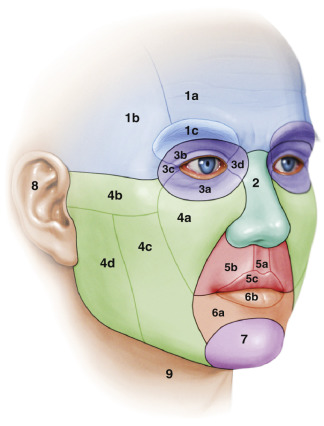
The salient features of the facial anatomy have been discussed in detail in other chapters. In consideration of obtaining an ideal aesthetic outcome with rhytidectomy and complementary procedures, the principles of facial anatomic subunits must be discussed in further detail. The surface anatomy of the head and neck region is divided into the various aesthetic units, including the nose, periorbital region, forehead, upper and lower lip, cheek, ear, neck, and chin ( Fig. 19.5 ). Some areas such as the nose, forehead, lips, and cheeks are further divided into additional subunits. These units and subunits represent regions of the face that have similar surface topography and three-dimensional quality based on the underlying anatomic structures, superficial and deep facial fat compartments, skin thickness, facial muscle activity, and curvature (flat, convex, or concave) . The confluence of and transitions between these subunits from the forehead to the neck formulate the patient’s facial shape and youthfulness. Although historically these units and subunits have been used as landmarks for planning scar revisions and facial/nasal reconstruction, the author has used the concept in obtaining a more natural and aesthetic facial rejuvenation outcome. Furthermore, a smooth transition between the various compartments of the face is paramount in creating a natural, youthful, and beautiful surface anatomy ( Fig. 19.6 ).
Although the ideal facial shape can differ depending on gender and ethnicity, there are some general characteristics that convey youth and beauty. The central oval of the face comprising the nose, eyelids, and lips is three-dimensional and forms the primary focus of an individual’s appearance. Even though the lateral subunits consisting of the cheeks and temple frame a secondary visual significance, these regions play an important role in an individual’s facial shape, attractiveness, and youthfulness. In the author’s view, the zygomatic cheek subunit (4b in Fig. 19.5 ) is the primary framework of a person’s facial shape, as it should form the most lateral position of the face. The tissue in this region is relatively fixed over the zygomatic arch (malar eminence), and as a result soft tissue laxity is not a concern during the aging process in this region. Patients with prominent malar eminence in the zygomatic subunit that softly transitions to the surrounding subunits will obtain better results from the rhytidectomy procedure . This subunit must be augmented if the area is underdeveloped due to congenital maxillary hypoplasia, remodeling, lipoatrophy, or trauma. The zygomatic subunit should not be augmented if patients have skeletonized, prominent, and/or excessive bizygomatic width. In fact, patients may have to have volume augmentation of the surrounding regions to improve the transition zones ( Fig. 19.7 ).


Superior to the zygoma lies the temple subunit (1b in Fig. 19.5 ) of the forehead. The temple subunit is comprised of the superior portion of the lateral temporal-cheek fat compartment, temporalis muscle, and superior extension of the buccal fat pad . The region should be flat or convex, and positioned slightly medial to the zygomatic subunit from the front view. Deep concavity of the temple subunit creates a gaunt and aged appearance, as well as significantly alters the shape of the face ( Fig. 19.8 ) . Volume augmentation with autologous fat grafting or fillers must be considered in every patient who presents with temple atrophy.
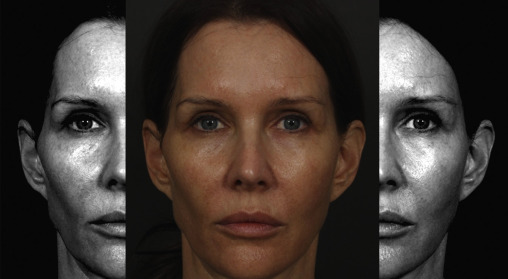
Inferior to the zygomatic subunit are the lateral (4d in Fig. 19.5 ) and buccal (4c in Fig. 19.5 ) subunits of the cheek. The lateral cheek subunit is comprised of the inferior portion of the lateral temporal-cheek fat compartment, parotid gland, and masseter muscles . The lateral cheek compartment is one of the main areas where gender differences are crucial in clinical outcomes. Male attractiveness is related to a more prominent lateral projection of this region and more defined angle of the mandible that forms the subunit’s inferior border. In females, the area should be more narrow, with a soft transition zone to the zygomatic arch. Regardless of gender, the subunit should be relatively flat and never be more lateral than the zygomatic arch ( Fig. 19.9 ). Careful attention must be paid to address this region if there is an underlying disproportion. For patients with prominent and hypertrophic masseters, neuromodulators may be used to reduce the bulk of the muscle ( Fig. 19.10 ). Customized SMAS imbrication techniques may also be used during rhytidectomy to narrow prominent parotid and masseteric fullness. Individuals who present with congenital or senile atrophy of the region must have volume augmentation at the time of the rhytidectomy utilizing SMAS folding, alloplastic implants, and/or autologous fat grafting (see Fig. 19.7 ).
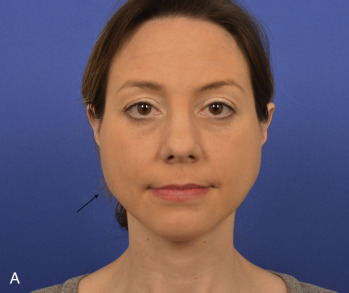

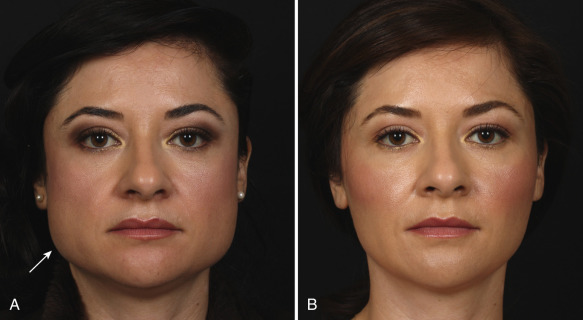
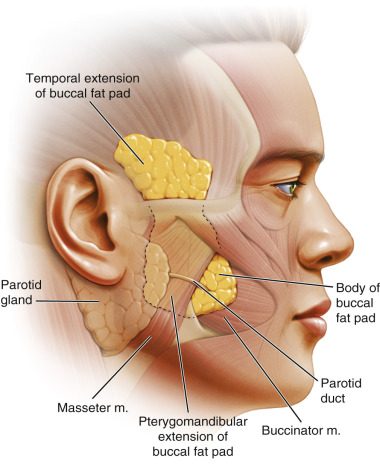
The buccal subunit lies medial to the lateral cheek subunit and inferior to the zygomatic subunit. The subunit encompasses the buccal space and midportion of the body of the mandible where jowling is visualized. Although jowls are one of the most common reasons individuals seek the rhytidectomy procedure, the buccal space plays just as important a role in one’s beauty and aesthetics. The buccal space is at the level of the oral commissure and comprised of the buccinator and buccal fat pads ( Fig. 19.11 ) . The buccal fat pad has multiple ligamentous attachments and extends beyond the buccal space into the pterygomandibular and temporal regions. The average volume is 8.9 and 10.2 mL for females and males, respectively . The parotid (Stenson’s) duct emerges from the parotid gland, travels along the masseter muscle in the buccal space, and pierces the buccinator muscle entering the oral cavity near the second superior molar . If the buccal fat pad is prominent, the shape of the face appears more round. The buccal fat pad may also be ptotic, leading to a more exaggerated jowling at the level of the mandible. The buccal space should be slightly medial to the zygomatic arch, with curvature that is either flat or slightly concave. The buccal space must always be addressed if the region has excessive convexity or concavity. Significant concavity gives an emaciated appearance, which is a sign of advanced aging. Convexity of the region results in rounding of the face, which is perceived as less attractive. As a result, addressing the buccal space is extremely important in our approach to facial rejuvenation, as some patients may require removal of buccal fat pad whereas others may require volume augmentation of the area. The most inferior portion of the buccal subunit, which overlies the midportion of the mandible, should be flat, smooth, and in the same plane as the mental subunit (7 in Fig. 19.5 ) and inferior portion of the lateral cheek subunit (4d in Fig. 19.5 ). This is the area that is directly addressed with most rhytidectomy procedures.
The medial cheek subunit (4a in Fig. 19.5 ) is positioned medially to the zygomatic and buccal cheek subunit, and is the region most commonly associated with the “midface” in traditional facial analysis. The pathophysiology of the aging process of this area involves inferomedial tissue descent, remodeling of the maxilla and orbit, as well as variable atrophy of the superficial and deep fat pockets (see Figs. 19.3 – 19.4 ). The lower eyelid subunit (3a in Fig. 19.5 ) forms the superior border of this subunit; the aging process of the two regions is therefore intimately associated with one another. The nasolabial fold, which separates the medial cheek and upper lip subunit (5b in Fig. 19.5 ), is an area where the cutaneous insertions of the lip elevators fuse onto the ligamentous structure formed by the SMAS and deeper facial fascia. The nasolabial fold becomes more prominent as the maxillary pyriform aperture remodels, various midface fat compartments atrophy, and the malar fat pad and suborbicularis oculi fat (SOOF) begin to descend . Progressive remodeling of the orbitomaxillary complex and facial fat atrophy results in pseudoherniation of the orbital fat pad, tear trough formation, as well as flattening and cavitary depressions of the medial cheek, contributing to the overall aging appearance. Our treatment of the region must therefore focus on creating soft transitions between the various surrounding subunits: zygomatic, lower lid, buccal, medial cheek, and upper lip. As a result of our improved understanding of these processes, the concept of volumization rather than “lifting” of medial cheek has significantly improved outcomes ( Fig. 19.12 ) .
The mental unit is made of the most anterior aspect of the mandible with the overlying soft tissue and muscles (7 in Fig. 19.5 ). The neck unit is inferior to the cheek and mental units (9 in Fig. 19.5 ). Ideally, patients should have well-defined cervicomental angles, with limited submental fat accumulation, minimal cervical platysmal banding, and sharp transition between the neck to the cheek and mental units. Male patients ideally should have a more projected mental unit, as discussed in earlier chapters. Individuals with poor chin projection and prominent prejowl sulcus will require further evaluation for simultaneous chin augmentation, autologous fat grafting, and/or fillers to enhance the results of the rhytidectomy. Submental fat accumulation can judiciously undergo suction-assisted lipectomy, and platysmal banding can be addressed with platysmal myotomy and corset platysmaplasty. Finally, patients with low and anteriorly positioned hyoid bone in the neck unit must be cautioned about the aesthetic outcome in cervicomental contour . Unlike the other skeletal regions, the hyoid cannot be manipulated during the rhytidectomy procedure.
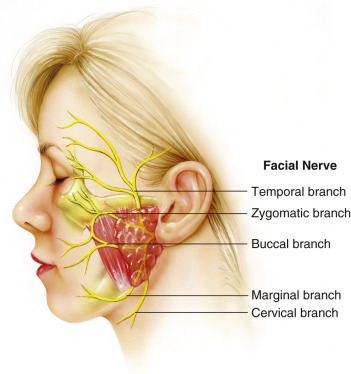
Finally, the safety of the facial nerve is perhaps the most important aspect of facelift surgery. The facial nerve exits the stylomastoid foramen and enters the body of the parotid gland ( Fig. 19.13 ). Within the parotid gland it bifurcates into an upper and lower division. It further divides into five main branches, namely temporal (frontal), zygomatic, buccal, marginal mandibular, and cervical. Permanent iatrogenic facial paralysis is rare owing to the extensive arborization of the buccal and zygomatic branches of the facial nerve. The marginal and cervical branches also may have arborization as the lower division separates from the upper division. The frontal branch is a terminal branch with limited redundancy. Injury to the frontal branch has the highest risk of causing permanent paralysis. The overall risk of permanent facial nerve paralysis in standard rhytidectomy is between 0.53% and 2.6% . There have been very few reports in the literature regarding the risk of facial nerve injury associated with more invasive facelifting procedures.
Preoperative Assessment
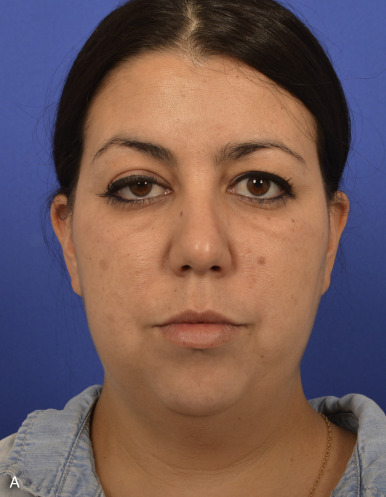
Rhytidectomy is typically indicated for patients with moderate-to-severe facial aging, as manifested by a change in facial shape, jowl formation, volume loss, and neck banding. Patients typically present for rhytidectomy between the ages of 45 and 65 years. Younger individuals with significant congenital jowling and a round or rectangular facial shape may also benefit from reshaping facial surgery that utilizes SMAS rhytidectomy, buccal fat pad removal, and autologous fat grafting to the zygomatic arch ( Fig. 19.14 ).


Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree