Keywords
Midface implants, Midface rejuvenation, Facial volume restoration
Introduction
The basis for all facial rejuvenation is an appreciation for normal aesthetic beauty and anatomy, the recognition of aging changes, and the knowledge to use various techniques, procedures, and biomaterials to recreate a more youthful face.
In the youthful face, roundness and volume abound and the beauty in the midface is frequently referred to as “apple cheeks.” This term pretty much says it all about youth; roundness and fullness. In many senses, youth is beauty and beauty is youth. As we age numerous changes occur in the hard and soft tissues that contribute to the aging face. Intrinsic factors such as heredity and extrinsic factors such as sun exposure and smoking all have an effect on how we look.
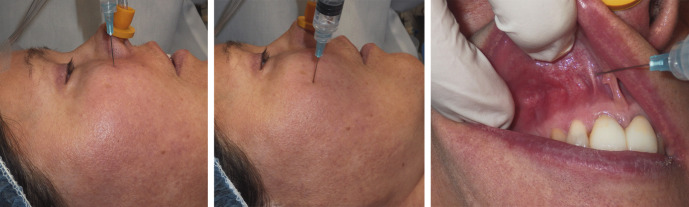
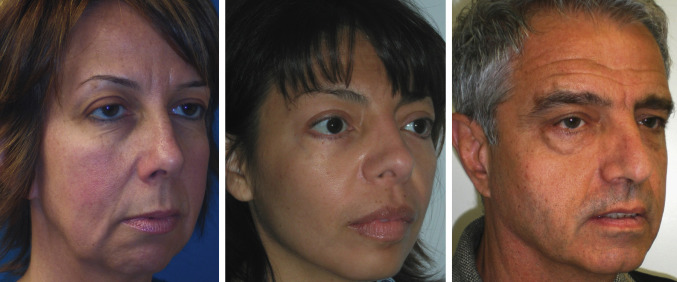
As early as the middle of the third decade, younger patients begin to experience subtle midface volume loss. As injectable facial fillers have become more common, one of my most frequent treatments is filler midface augmentation in patients in their 30s and 40s. Even patients realize that they lose volume at an early age ( Fig. 21.1 ).

Facial aging in many ways is a process of deflation from volume loss. It was only several decades ago that cosmetic facial surgeons simply pulled skin over a skeletonized face during facelift without restoring volume. This created a situation where patients look tighter but not younger. Over the past several decades facial rejuvenation has become more focused on creating natural and youthful results by adding volume to facelift surgery. Instead of just taking something away (skin and fat) we are adding something back (implants, fat transfer, fillers) to reinflate the aging face. Simply stated, contemporary cosmetic facial surgeons realize the importance of volume augmentation during rejuvenation.
One of the hardest things for the novice surgeon is to make an accurate diagnosis of midfacial volume loss and choose the proper treatment to correct it. Younger surgeons have always had fillers as an option for cheek enhancement, but those of us who have been practicing for decades well remember the days where the only fillers were collagen and they did nothing for the cheeks. In that era, both facial implants and fat transfer were scientifically studied and refined into the mainstays in volume enhancement they remain today.
Today’s facial surgeons can look at a patient with midfacial volume loss and decide on numerous treatments, including injectable filler, fat transfer, midface lifting procedures, and silicone midface implants. Which is the best option? That is a wide-open question and the true answer is whatever works best in the hands of a specific surgeon and provides a safe and natural patient result. Secondary to this broad answer, silicone implants have distinct advantages over other therapies for numerous reasons. Silicone implants are superior because:
- •
they are extremely biocompatible and inert
- •
they are permanent when anchored to the facial skeleton with screws
- •
they are reversible (very few procedures are permanent but reversible)
- •
they are adjustable as they can be trimmed, customized, or surgically exchanged for larger or smaller sizes
- •
they come in a vast array of sizes and shapes
- •
they can be customized from computed tomography (CT) scans
- •
they provide 3D augmentation
- •
they can be used in conjunction with other procedures or as a standalone treatment
- •
they have an easy learning curve with low complication rates when properly performed.
- •
midface fillers are temporary
- •
fat transfer to the midface can be problematic in longevity, mobility, and because it is placed in soft tissues, will sag with age
- •
lifting procedures for the isolated midface, although well described, have not made the impact that implants have on facial rejuvenation and are not permanent.
Diagnosis
Diagnosis of the aging midface is relatively straightforward, as it remains relatively constant in healthy individuals. The basis of a youthful midface is the malar fat pad. This structure is triangular in shape, with the base lying on the nasolabial fold and the apex lying on the malar region in younger patients ( Fig. 21.2 ).

As the hard and soft tissue aging progress, the fat pad descends and atrophies. As this occurs the nasolabial fold deepens and the tear trough region becomes more skeletal because of periorbital hard and soft tissue changes. If you ask a patient with an atrophic midface to smile, they look younger because the muscles elevate and fill the midface. Having a patient with midface loss lay back in a chair and look in the mirror will also illustrate the aging changes as well as show them a prediction how cheek implant results will look. When gravity is removed from the situation and the patient is supine, the jowls fall back and fill the cheeks. This is how I show patients “surgical predictions” ( Fig. 21.3 ).

As stated, accurate analysis of the aging face requires an understanding of the aging changes. My most basic diagnostic tool is to keep a mental image of a youthful midface and compare what is “missing” in the aging patient. For the most part, the cheek region can be grossly broken down into three regions ( Fig. 21.4 ):
- •
the infraorbital region
- •
the malar/submalar region
- •
the zygomatic region.

It was not that long ago that custom implants did not exist and surgeons had to fashion them manually by carving a silicone block during the operation. Today’s modern implants are produced on human skeletal models and conform to the underlying anatomy much like a store-bought shoe conforms to a foot.
The most common type of implant materials are porous polyethylene and silicone. Although both materials can produce a great result, there are numerous drawbacks of using porous polyethylene material.
Silicone implants form a dense, fibrous capsule and therefore do not integrate into the soft tissues. Porous polyethylene implants, on the other hand, do integrate with the soft tissues, and for this reason can be difficult and sometimes impossible to remove. Porous polyethylene implants most commonly fragment upon removal and are so attached to the soft tissue that muscle and perineural tissue can adhere to the implant and be damaged.
Although there are many shapes and types of implants, I have found over the three decades that I have been placing facial implants that there are three main sizes that will suffice in 99% of normal patients.
The most common type of aging change and configuration of implant I place is the submalar type ( Fig. 21.5 ). The Binder type II submalar silicone implant ( http://www.implantech.com ) is my preferred implant for most patients from the later third decade onwards. This implant is available in the solid configuration or the conform configuration, which has a cross-hatched posterior surface. I do not use the conform configuration, as it is overly flexible and I prefer the more rigid solid implant. The advantage of the conform configuration is that if it is not being screw fixated, the cross-hatched surface provides increased stabilization during healing. Because I fixate all implants it is of no benefit to me.
The malar shell–type implant is a configuration that I seldom use, but it remains common with some surgeons. This type of implant is used for either patients with developmental zygomaticomalar hypoplasia or patients that want the “high cheekbone” look, which I personally feel is less contemporary than it was several decades ago.
The third type of implant is the combined submalar implant configuration. This type of implant is basically a combination of the submalar and the malar shell styles, and is used to treat a broader range of volume loss or hypoplasia across the entire maxilla and lateral malar region.
In my practice 95% of facial implants are submalar, with the combined submalar making up the other 5%. I may insert a malar shell type implant every several years.
The Binder type II submalar implant is versatile, in that even though the configuration is the same, using different sizes can change the result ( Fig. 21.6 , left ). This implant has great submalar (and infraorbital) thickness and then thins out to a less prominent but still significant malar thickness, which finally totally feathers out for minimal zygomatic augmentation. The average patient (male or female) will use a medium-to-large implant. Bigger patients, or those with more volume loss, may use an extra-large submalar. In addition, all these implants may be trimmed with scissors to further customize the result.
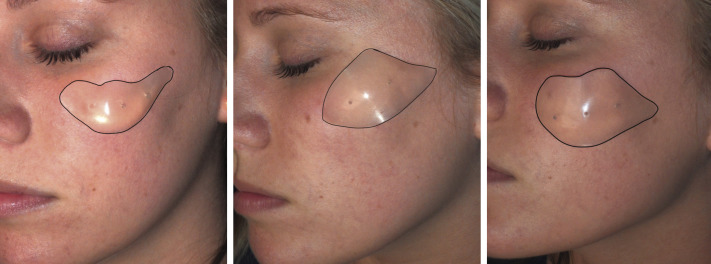
The malar shell implant is used primarily for lateral malar and zygomatic augmentation ( Fig. 21.6 , center ).
The combined submalar implant runs larger than the regular submalar configuration. Again, I use this for patients that have more extreme volume loss or developmental maxillary and malar hypoplasia ( Fig. 21.6 , right ). I use a small-sized combined submalar implant for most females or use a medium size and trim the edges. Males may require a medium or large size. The large size of the combined submalar implant is actually quite large and few patients require that level of augmentation. One general rule of implant placement is when in doubt, use a smaller implant. An implant that is a little too small may look fine, but an overly large implant can look very unnatural. Caution is also used with younger patients seeking “celebrity” cheeks. I require these types of patients to perform cheek filler first to make sure they truly like their look. The actual size selection is more of an art than a science and comes with experience. The use of intraoperative sizer implants will be discussed later in the chapter.
Presurgical Considerations
When patients present or consult for cheek implants, the entire dialog of diagnosis and treatment is presented. Cheek implant placement is very foreign to some patients, and having actual implants, models, figures, animations, and so on is very helpful for education. Viewing actual before and after pictures is also extremely useful.
A physical examination for any asymmetry or pathology is completed, as well a comprehensive dental and periodontal examination. Panoramic radiograph or cone beam CT is performed to rule out any osseous, dental, or sinus pathology that could affect the implants.
The sequelae and potential complications of implant placement are discussed, including swelling, temporary paresthesia, bleeding, infection, hardware rejection, overcorrection, undercorrection, and so on.
Surgical Technique
Cheek implant placement is a relatively simple and expedient technique with a short learning curve for surgeons who are familiar with the maxillofacial anatomy. Midface implants can be placed with local anesthesia, but in my practice virtually all surgery is performed with intravenous sedation or general anesthesia in an accredited ambulatory surgery center. All patients are placed on a cephalosporin for 1 week and given a prescription for analgesic. An intraoperative dose of intravenous antibiotics and steroid is given during the procedure.
The first step is local anesthetic infiltration at the periosteal level across the maxilla and zygoma, and intraorally in the mucosa for hemostasis ( Fig. 21.7 ).