Key points
- •
The worldwide prevalence of atopic dermatitis (AD) has risen over recent decades, paralleling industrial and urban growth.
- •
Airborne pollutants induce oxidative damage at the skin interface with the outside world, setting in motion a cycle of inflammation, skin barrier disruption, and repeated irritant entry in AD.
- •
Common forms of environmental pollution found to affect the skin barrier and AD include cigarette smoke, particulate matter, volatile organic compounds, and traffic-related air pollution.
- •
Strategies to mitigate pollution-induced barrier dysfunction include avoiding and blocking pollutant exposure, regular skin cleansing, and emollient application to repair and bolster the skin barrier.
- •
Future research should aim to more fully characterize the mechanisms by which pollutants impact AD in real-world settings and seek to identify effective topical formulations to protect the skin against airborne pollutants.
Introduction
When we consider the variety of external factors that may influence the development of atopic dermatitis (AD), it is logical that environmental pollution comes to the forefront, as it has been strongly associated with the development of other atopic diatheses, including asthma, allergic rhinitis, and food allergies.
Before we discuss the impact of pollution, however, it would be prudent that we first define the term pollution . According to the Merriam-Webster Dictionary online , is “the action of polluting, especially by environmental contamination with man-made waste.” (Merriam-Webster). Thus human activities, whether intentional or unintentional, produce waste and byproducts that can become triggering factors for the development of AD. Having defined pollution, let us now delineate its impact on AD by examining published data in the literature.
The prevalence of AD has been steadily rising in recent decades, particularly in certain regions. Despite a global increase in the number of children with AD, developed countries such as New Zealand and the United Kingdom that previously reported high rates of AD have experienced a plateau at around 10% to 15% ( ). However, AD prevalence is growing in lower income developing nations, with rates higher than 15% and up to 24.6% reported in countries of Southeast Asia, Africa, and Latin America ( ). The increased incidence of AD parallels expansion in urbanization and industrialization worldwide, and investigation of the role of airborne pollution in relation to AD has become increasingly relevant. One of the major areas of study centers on the role of pollution in skin barrier dysfunction.
General mechanism of pollution-induced barrier dysfunction
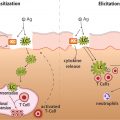
The general mechanisms of pollution-induced skin barrier dysfunction result from excess oxidative stress that in turn induces inflammation. Airborne pollution generates reactive oxygen species, which deplete the skin’s antioxidant defenses. This pro- versus antioxidant imbalance, favoring prooxidants, results in oxidative damage to keratinocytes, decreased cell adhesion, and barrier dysfunction as indicated by increased transepidermal water loss (TEWL), decreased hydration, and increased pH ( ). Compromised skin barrier integrity allows for easy entry of pathogens, irritants, and immunogens ( ), fueling inflammation and the itch-scratch cycle in AD ( ). Signaling cascades involved in pollutant-induced skin barrier damage include the NFκB inflammatory pathway ( ) and aryl hydrocarbon receptor (AhR) ( ). Airborne pollutants have been found to increase NFκB signaling and promote expression of proinflammatory cytokines that lead to skin redness, swelling, itch, and pain. AhR acts as a chemical sensor in keratinocytes, leading to downstream activation of inflammation and itch mediators as well as epidermal antioxidant defense mechanisms ( ).
Cigarette smoke
Cigarette smoke from burning tobacco contains antigenic and carcinogenic compounds such as nicotine, polycyclic aromatic hydrocarbons, and metal residues ( ). evaluated TEWL as an indicator of barrier function in a cohort of 100 patients, including active heavy smokers, passive smokers, and nonsmokers. Average TEWL did not differ between active and passive smokers but was significantly lower in nonsmokers compared to both active and passive smoking groups (11 vs. 16 g/m 2 /h, P < .001) ( ). These results suggest that both active and passive exposures to cigarette smoke are associated with reduced capacity of the epidermis to retain water.
Cigarette smoke has also been identified as an exacerbating factor in AD. Within a cohort of 7000 Korean schoolchildren, exposure to environmental tobacco smoke during the mother’s pregnancy and children’s infancy was associated with a twofold greater risk of AD development ( ). In a large survey-based study of over 145,000 Korean adolescents, more than 10,000 respondents reported AD symptoms within the last 12 months. Among this subset of adolescents with AD symptoms, researchers found a significant association with both active and passive cigarette smoking, and the strongest association was observed in those who actively smoked more than 20 days per month (odds ratio [OR] = 1.18) ( ).
While increased TEWL and higher prevalence of AD symptoms have been demonstrated in association with smoking, further research is needed to better understand the relationship between cigarette pollution and AD exacerbation. Nevertheless, convincing evidence exists to support smoking cessation for skin as well as general health.
Particulate matter
Particulate matter (PM) describes liquid or solid particles in gas suspension and is classified according to its aerodynamic diameter ( ). Ultrafine PM (<0.1 μm in diameter) is emitted from diesel engines. Fine PM (0.1–2.5 μm) is generated from open fires, power plants, and car exhaust. Coarse PM (2.5–10 μm) originates from soil, dust, and industrial emissions ( ).
PM has been demonstrated to induce skin barrier dysfunction in vivo. In a study using live pigs, which have skin similar in structure and function to that of humans, dorsal skin treated with solubilized PM exhibited a twofold increase in TEWL compared to vehicle control, as well as loss of epidermal structural proteins ( ). PM stimulates keratinocyte production of matrix metalloproteinases, induces inflammatory cytokines, and activates the NFκB signaling pathway ( ). Furthermore, PM has been shown to have dose- and time-dependent cytotoxic effects on cultured skin cells ( ).
PM has shown detrimental effects in both healthy and AD skin in animal models, with increased susceptibility to PM-induced damage in the barrier-disrupted state of AD. demonstrated the capacity of PM to penetrate barrier-disrupted skin and incite an inflammatory response in mice. PM was identified in the hair follicles of both intact and tape-stripped skin but was also present intercellularly in samples of barrier-disrupted epidermis. Repetitive topical application of PM followed by occlusive dressing led to neutrophil-predominant dermal inflammation in both intact and barrier-disrupted mouse skin ( ). used a rat model of capsaicin-induced AD to study the effects of vaporized glyoxal, a major source of PM production. Exposure to glyoxal vapor exacerbated pruritus and dermatitis in rats with existing AD but did not induce AD symptoms in healthy animals ( ), indicating that preexisting barrier disruption is required for PM to exacerbate AD. Increased skin Staphylococcus aureus colonization was observed in both AD and healthy animals following glyoxal exposure, demonstrating the potential of PM to contribute to cutaneous dysbiosis (imbalance of the microbiota), a major driving factor in AD pathogenesis ( ).
Studies in human populations have also identified correlations between PM and AD symptoms. A study of 21 Korean pediatric AD patients revealed a temporal association between elevated PM levels in urban areas and increase in reported AD symptoms ( ). Fine PM (<2.5 μm in diameter) levels had a stronger positive correlation with AD symptoms compared to coarse PM (2.5–10 μm in diameter) with respective ORs of 1.399 and 1.215 per 10-μg/m 3 increase in PM exposure ( ). A population-based cross-sectional study of over 5000 Taiwanese adults identified a modest association between frequent fine PM exposure and development of AD (adjusted OR = 1.05) ( ). Based on these findings, it appears that fine PM may be most detrimental, as it can penetrate the epidermal barrier of tape-stripped skin ( ) and may inflict greater damage with high PM concentrations or prolonged exposure time.
Volatile organic compounds
Volatile organic compounds (VOCs) are carbon-based substances that readily vaporize at ambient air pressure and are important contributors to indoor air pollution. Common VOCs are organic solvents such as benzene, toluene, xylene, and formaldehyde, which are released from household items, including cleaning supplies, wallpaper, new furniture, plastics, and plywood ( ).
Airborne formaldehyde has been demonstrated to induce skin barrier dysfunction. evaluated 12 AD subjects and 12 healthy subjects exposed to dust mite allergen and subsequently to a mixture of 22 VOCs in a total body chamber. Compared to purified air control, a mean 34% increase in TEWL was observed at 48 hours post-VOC exposure in both healthy and AD subjects, without significant difference between the two groups ( ). Furthermore, six of seven AD patients patch tested with house dust mite allergen exhibited an enhanced skin reaction following VOC exposure, demonstrating that VOCs can exacerbate the atopic response to allergens ( ). found that exposure to formaldehyde caused an increase in TEWL and skin pH in both healthy and AD subjects. The median increase in TEWL was 2.5 and 1.4 g/m 2 /h in AD and healthy skin, respectively ( ). A more pronounced increase in skin pH was also observed in AD compared to healthy skin (0.11 vs. 0.04 pH units), indicating that individuals with existing AD are more susceptible to VOC-induced barrier damage. These findings are in agreement with animal studies conducted by , who found that formaldehyde fume exposure exacerbated pruritus and dermatitis in a rat model of AD.
Investigations of real-world VOC indoor pollution exposure have also demonstrated a negative impact on skin barrier function. In a cross-sectional study of over 4000 Korean schoolchildren, those living in homes that had been remodeled within the preceding 12 months had more than a threefold greater risk of AD compared to those who did not live in areas of remodeling ( ). A combination of recent remodeling and food allergy synergistically increased the risk of AD in children by sevenfold ( ). studied the effects of plant-based wallpaper compared to PVC (polyvinyl chloride)-based wallpaper, and reported that AD children who live in apartments with higher formaldehyde and VOC levels in indoor air had significantly higher SCORAD indexes. The authors found that ecofriendly wallpapering was associated with an increase in natural VOCs, also known as phytoncides, that are given off by trees and plants. Higher levels of natural VOCs correlated with improvement in AD symptoms, suggesting that plant-based VOCs may have positive effects on barrier integrity ( ).
Traffic-related air pollution
Traffic-related air pollution (TRAP) includes both PM and VOC pollutants, which were described previously, in addition to gaseous components such as nitrogen oxides (NO, NO 2 , N 2 O), SO 2 , CO, and O 3 generated from gasoline and diesel-powered engines ( ). found that exposure of human skin to 0.8 ppm O 3 for 2 hours led to a nearly 50% reduction in colony-forming units of resident microflora compared to nonpolluted air exposure alone. This effect is of interest in relation to dysbiosis in AD, where alteration of resident skin flora and predisposition to S. aureus colonization are widely observed ( ), although a direct link between TRAP exposure and S. aureus colonization has not been established.
TRAP exposure is of particular relevance as many regions in the world become increasingly urbanized. To evaluate the health effects of this trend, a longitudinal study of the influence of air pollution in healthy German women was initiated in 1985. Follow-up during 2008–2009 identified a 7.9% incidence of AD symptoms after age 55. The investigators reported a significant positive association between incidence of AD symptoms and exposure to TRAP, with TRAP exposure determined by measuring levels of PM and nitrogen oxides in 2008–2009 and back-extrapolating to baseline levels ( ).
During the prenatal and infancy periods, TRAP exposure is associated with increased risk of AD. A prospective cohort of mother-child pairs in Osaka, Japan, was followed from mothers’ pregnancy to 16 to 24 months of children’s age and assessed for risk of asthma and AD development in relation to proximity of the child’s residence to the nearest main road ( ). Within this cohort of 756 children, 8.9% developed physician-diagnosed AD by age 16 to 24 months. Compared to children living more than 200 m from the nearest main road, those living within 50 m had a significantly higher risk of doctor-diagnosed AD (adjusted OR = 2.26, P = .03) ( ). Although this study does not distinguish the effects of pre- versus postnatal TRAP exposure, the findings indicate a role of TRAP in childhood development of AD and its possible contribution to the rising prevalence of AD in industrialized and developing countries over recent decades. However, direct effects of TRAP on the skin barrier have not been investigated.
A summary of study findings regarding the effects of specific pollutants on skin barrier function and AD is presented in Table 9.1 .