Key points
- •
Allergen-specific B cells are differentiated into plasma cells producing immunoglobulin E (IgE) antibodies. Through binding to the receptors (FcεRI and FcεRII), IgE induces cytokine and chemokine production from immune cells.
- •
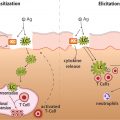
Intrinsic atopic dermatitis is T-cell mediated, involving Th2 cytokines that cause skin inflammation and pruritus.
- •
Extrinsic atopic dermatitis is IgE mediated, involving allergen-specific IgE, including autoreactive IgE.
- •
Cytokines and chemokines that play a key role in the inflammatory lymphocytes’ infiltration into skin can be potent biomarkers and therapeutic targets.
Introduction
Humoral factors (i.e., IgE antibodies, cytokines, and chemokines) play a key communication role in the development of atopic dermatitis (AD) that involves various types of immune and nonimmune cells. They also play a driving role in amplifying the inflammatory response during the disease transition from the acute to chronic phase. IgE antibodies are produced by skin B cells, whereas cytokines and chemokines are produced essentially by all types of cells involved in AD, including keratinocytes, epidermal-derived immune cells, as well as migrating lymphocytes and granulocytes from the skin draining lymph nodes and the circulation. Following skin barrier disruption, keratinocytes start secreting chemokines and cytokines such as thymic stromal lymphopoietin (TSLP), leading the maturation and migration of antigen-presenting cells such as epidermal Langerhans cells and dermal dendritic cells. Those antigen-presenting cells carry skin-associated antigens (including allergens and microbiota) to the skin draining lymph nodes. In the lymph nodes, they activate B cells and T cells, leading adoptive humoral response with IgE production, as well as Th2 cellular response with Th2-type cytokine production. Accordingly, AD has been classified into intrinsic and extrinsic phenotypes on the basis of serum IgE levels, IgE-mediated sensitization, and personal and family history of AD. Intrinsic AD is mostly T-cell mediated and represents 10% to 20% of AD. Extrinsic AD is IgE mediated, representing 80% of the patients. Importantly, cytokine profiles that contribute to the pathophysiology of AD are distinct, in intrinsic versus extrinsic types of diseases, children versus adults, and in acute versus chronic diseases. In this chapter, the roles of cytokines and chemokines are discussed with consideration of phenotypic variations of AD. Cellular responses in AD are discussed in Chapter 14 . Please refer to Figure 14.1, Figure 14.2 , which illustrate the immune pathophysiology of AD that involves both humoral and cellular responses.
IgE antibodies in atopic dermatitis
B cells as the IgE producer
As a major part of the humoral response, B cells are lymphocytes specialized in differentiating into plasma cells (PCs) that produce antibodies. While B cells provide defense against infections via antibody production, they also adversely mediate autoimmune diseases and allergies such as AD. During development in the bone marrow, through the VDJ gene recombination mechanism, each B cell is programmed to express immunoglobulin (Ig) with a unique single specificity as its B-cell receptor (BCR). Similar to T-cell selection, B cells expressing a BCR with strong self-reactivity are eliminated by a variety of mechanisms. Selected immature B cells migrate to the peripheral tissues and lymphoid organs such as the spleen, to further differentiate into several B-cell subsets ( ).
Upon binding to specific antigens via BCR, innate type B cells such as B-1 cells with conserved pathogen-specific Ig repertoire can mount rapid T-independent response with polyreactive IgM and IgA production. On the other hand, conventional B-2 cells capture antigens and present peptides to CD4 + T cells in MHC-II–restricted manner. The cognate T-B interaction, in turn, supports B-cell differentiation into either short-lived PCs producing low-affinity antibodies or germinal center (GC) B cells that further differentiate into memory B cells and long-lived PCs carrying BCR with improved higher affinity to cognate antigens. Within GC, B cells undergo BCR affinity maturation via somatic mutation. They also undergo BCR class switching from IgM to another isotype such as IgG, IgA, and IgE, which allows acquisition of different effector properties while maintaining the same antigen specificity ( ). In AD, B cells are thought to play a driving role in skin inflammation by producing IgE antibodies. Also, as discuss in the Chapter 14 , some B cells can regulate inflammatory response by secreting IL10. B-cell accumulation is evident in inflamed skin. Higher B-cell activation status reflects accumulative antigen exposure and the ability to contribute to T-cell activation, leading to pathogenic IgE production ( ), which can be destructive to skin tissues especially in the case of IgE autoantibody production.
Mechanisms of IgE production
IgE is the immunoglobulin isotype providing a first-line defense against parasite infection. However, in response to allergen exposures IgE adversely mediates type I hypersensitivity reactions, including anaphylactic reaction by sensitizing mast cells and basophils for rapid degranulation. Although the mechanisms leading to IgE production remain poorly defined, evidence suggests that IgE production is tightly regulated by multiple mechanisms. In healthy humans, the concentration of free serum IgE is maintained at 50 to 200 ng/mL, which is extremely low compared to other Ig isotypes that range from 1 to 10 mg/mL. The half-life of IgE in humans is the shortest of all Ig isotypes, which is ~2 days compared to ~20 days for IgG ( ). However, elevated levels of total serum IgE in association with various environmental allergens and autoantigens are reported in approximately 80% of the patients with severe AD ( ). In the patients with severe extrinsic AD, the concentration of total IgE was correlated with the severity of the disease ( ).
IgE is produced by B cells through class-switch recombination (CSR) mediated by Th2 type cytokines such as IL4. In the Ig gene locus, constant region genes for isotypes are localized in the order of IgM (Cμ), IgG1 (Cγ1), IgA (Cα), and IgE (Cε). The Cε locus is farthest from the Cμ, which may limit the direct CSR from IgM to IgE. In theory, B cells can also sequentially rearrange the constant region gene to another downstream isotype, such as first from Cμ to Cγ1, and then to Cε. However, analysis of Ig rearrangement in B cells from patients with AD showed no evidence of sequential CSR ( ).
The mechanisms of IgE B-cell differentiation have been mainly studied in mouse models in which either transcription or translation of membrane IgE is tagged with fluorescent protein ( ; also reviewed in ). Based on these studies, IgE GC response is transient. As a result, IgE antibody repertoire shows less diverse specificities and lower affinity than that of IgG1 ( ). The latter is thought to be due to lower expression levels of IgE BCR, which limits BCR-mediated signaling required for survival and affinity maturation in GCs. Overall, IgE response is shifted toward short-lived extrafollicular PC generation rather than GC pathway. In fact, IgE B cells express higher levels of Blimp1 compared to IgG1 B cells, which likely predisposes IgE B cells to differentiate into PCs over GC pathway ( ). In mice, IgG GC B cells have been shown to give rise to both IgG1 and IgE memory cells, and a small number of long-lived IgE PCs are detected in the bone marrow ( ; also reviewed in ). However, more studies are needed for better understanding human IgE memory B cells.
Effector properties of IgE
IgE exhibits its effector properties through binding to two types of IgE receptors on immune cells. The high-affinity IgER (FcεRI) carrying immunoreceptor tyrosine-based activation motif (ITAM) is expressed on mast cells and basophils as a tetramer (α, β, γ, γ), the activation of which mediates degranulation, eicosanoid production, and cytokine production ( ). In humans, FcεRI is also expressed by DCs and macrophages as a trimer (α, γ, γ), the activation of which mediates the internalization, processing, and presentation of IgE-bound antigens, leading to cytokine production supporting Th2 type immune responses ( ). The low-affinity IgER (FcεRII or CD23) is a C-type lectin, expressed on B cells, which regulates IgE production, antigen processing, and presentation ( ). A study with B-cell–deficient mouse model indicates that FcεRII regulates the levels of free IgE in the blood by passively binding to IgE ( ). FcεRII is also expressed on macrophages and epithelial cells, and is involved in uptake of IgE-antigen complexes ( ).
Regarding specificities of IgE antibodies, a recent large-scale meta-analysis provided an important conclusion that AD is associated with IgE-autoreactivity ( ). In fact, patients with severe AD show signs of multiple allergen-sensitizations, including aero, food, and microbial antigens ( ). Furthermore, significant percentage of AD patients carry IgE antibodies cross-reacting with human proteins and fungal proteins (i.e., autoallergens) (reviewed by ). However, clinical trials with anti-IgE monoclonal antibody omalizumab showed limited efficacy in the control of AD symptoms ( ), suggesting that IgE reactivity in AD patients may be a result of other allergies often seen in the patients with severe AD.
Cytokines in atopic dermatitis: An overview
Roles of cytokines
AD is thought to arise because of barrier dysfunction of the skin and aberrant activation of Th2 responses. Characteristics of AD patients—especially patients with extrinsic AD (see later)—include elevated serum levels of total IgE and IgE specific to environmental or food allergens ( ). However, AD has recently been considered a T-cell–mediated disease, involving excessive activation and imbalance of T-cell subsets ( ). Recent studies analyzing gene expression have shown that excessive Th1, Th17, and Th22 responses tend to build pathophysiology of AD, although Th-cell polarization into Th2 responses parallels activation of the other Th phenotypes. Understanding the contribution of each cytokine in this complex and integral (systemic as well as localized) disease has been markedly advanced by the use of cytokine inhibitors, such as anticytokine antibodies, administered in clinical trials of targeted therapeutics ( ). The success of dupilumab, an anti-IL4 receptor (IL4R) monoclonal antibody, in blocking both IL4 and IL13 signals through binding to their common receptor expressed on the target cells, has advanced new therapies and clarified key roles of Th2 responses as critical mediators in controlling the skin disease ( ). As mentioned, the cytokine profile that contributes to the development of AD is distinct (e.g., in intrinsic vs. extrinsic disease, children vs. adults, and acute vs. chronic disease). Clarifying and defining the phenotypes of AD in accordance with the status of AD patients should lead to more personalized AD treatment in the future ( ). Cytokines are produced by epithelial cells (including keratinocytes) and epidermal-derived immune cells; cells infiltrate the skin region in response to chemokines or other chemical substances, such as prostanoids (lipid mediators that include leukotrienes) ( ). It is also important to understand the types of cells involved in cytokine responses.
Cytokine effects on phenotypes of AD
Acute and chronic
In the acute phase of AD, Th2, and Th22 responses are augmented by Th17 response; these responses contribute to the further impairment of barrier function and activate epithelial cells, especially keratinocyte, increasing the severity of the disease and promoting its chronicity. Th1 skewing toward the Th2/Th22 response plays an important role in the progression of the disease (i.e., chronicity).
Mutation in the FLG gene is a strong risk factor for inducing barrier dysfunction in AD patients. Barrier defects promote cutaneous penetration of allergens and bacterial or viral products, which then stimulate the production of epithelial cell–derived proinflammatory cytokines such as TSLP, IL33, and IL25 ( ). These events further impair barrier function and potentiate inflammatory responses of epidermal infiltration of inflammatory cells, activation of Th2 cells and innate lymphoid cells (ILCs), and expansion of multicytokine responses (Th2, Th22, and Th17) in the acute phase. Abnormal cytokine responses are observed in both lesional and nonlesional skin of AD patients. In chronic AD, unlike in acute AD, Th1 (but not Th17) attends to the expansion of Th2/Th22 responses and the upregulation of IgE-mediated responses, but the mechanism remains to be clarified. The profound Th2 response stimulates cutaneous neuronal itch response via IL31. Pruritus exacerbates AD by promoting scratching and sleep deprivation, which decrease the quality of life of AD patients.
Children and adults
Our understanding of the transition in AD phenotype from the acute to the chronic state relies on recent data obtained by analyzing the skin of adults who have suffered chronic AD since the first 5 years of life. To characterize the changes in skin immunity and barrier function that occur from the onset of the disease, several researchers have investigated the cytokine phenotype of early pediatric lesional and nonlesional AD skin, comparing it with age-matched healthy individual skin and adult skin with AD ( ). Such analysis has enabled us to advance targeted treatments for children with AD. The cytokine phenotype differs between early pediatric AD skin and adult moderate-to-severe AD skin. Similar to that in the acute phase of adult AD, the lesional skin in pediatric AD is characterized by strong Th2 (IL13, IL31, CCL17) and Th22 (IL22) activation, with some IL9, IL33, and Th17 skewing (IL17A, IL19, CCL20). In pediatric skin, IL8, IL17A, and antimicrobial peptides (AMP) produced by commensal bacteria to protect against Staphylococcus aureus are increased, reflecting a response to infectious agents in children without fully acquired immunity. However, these inflammatory responses further injure epithelial cells and promote Th2/Th1 imbalance, contributing to AD pathophysiology. In pediatric skin, IL19 is upregulated in lesional and nonlesional skin. Because IL19 amplifies the effects of IL17 on keratinocytes, it indirectly promotes Th2 activation. Thus IL19 is thought to bridge the Th2 and Th17 responses in AD. In addition, in the nonlesional skin of pediatric AD patients, abnormalities and inflammatory responses are enhanced (keratinocyte hyperactivation; increased TSLP, IL17, and IL19 production), indicating a disease-initiation state. Therefore, to prevent AD chronicity in pediatric AD patients, treatment targeted to various cytokines distinct from targeted approaches in adult AD may be necessary ( ).
Intrinsic and extrinsic
The phenotype of AD has been classified into intrinsic and extrinsic types on the basis of total and specific serum IgE levels, IgE-mediated sensitization, and personal and family history of AD (Suárez-Fariñas et al., 2014). Intrinsic AD (also known as pure or nonallergic type) is thought to be T-cell mediated and represents 10% to 20% of AD. Extrinsic type (also known as mixed or allergic type) is IgE mediated; 80% of the patients are classified as having this type. Analysis of mRNA expression in skin lesions showed that Th2 cytokine (IL4, IL5, IL13, and IL31) expressions were augmented in both AD phenotypes, whereas higher IFN-γ levels are detected in only intrinsic-type AD compared with extrinsic AD. Intrinsic AD is thought to be closely linked to metal allergy, and IFN-γ plays a role in contact sensitivity ( ). In addition, Th17 and Th22 subsets are activated in intrinsic AD, and 61.3% of patients report allergy in response to one or more metals, including nickel, cobalt, or chrome. In some cases, AD patients with known allergies to nickel may not tolerate eating nickel-containing foods, such as chocolate. (Suárez-Fariñas et al., 2014; ). Food allergies and intolerance are further discussed in Chapter 8 .
Cytokines: Detail analysis
Epithelial cell–derived cytokines
AD pathogenesis is characterized by Th2 skewing and barrier dysfunction. TSLP, IL33, and IL25 are regarded as inducers of excess production of Th2 cytokines in the lesional skin of AD patients. The mechanism by which these cytokines are upregulated in epidermal keratinocytes remains unknown. Scratching or signals through human intelectin-1 (ITLN1), which is a soluble lectin on keratinocytes that recognizes galactofuranose of bacterial cell wall, are candidate upregulators of epithelial cell–derived cytokine expression in the lesional skin of AD patients ( ).
TSLP is a cytokine that has been suggested to be an initiator of Th2 response. Keratinocytes and Langerhans cells function as antigen-presenting cells and were reported to express high levels of TSLP through the OX-40 ligand pathway in the injured skin of AD patients ( ). TSLP transduces signals to different cells via its heterodimeric receptor that comprises the IL7 receptor α-chain and the TSLP receptor (TSLPR). Dendritic cells are primary targets of TSLP ( ). By binding to TSLP, dendritic cells (in this instance, dermal Langerhans cells) express OX40L, CD80, and CD86 on their surfaces and produce IL4, IL5, and IL13, which cause naïve T cells to differentiate into the Th2 phenotype. TSLP also promotes Th2 cytokine production by mast cells, ILCs, epithelial cells, macrophages, and basophils ( ), thus exacerbating Th2 immune activation. In contrast, the cytokines produced by keratinocytes activate regulatory T cells, leading to inhibition of excessive inflammatory responses ( ). In infantile AD, analysis of the expression of several epidermal proteins has revealed that TSLP may be an effective biomarker for predicting the development of AD ( ).
IL33 is a member of the IL1 family and binds to a heterodimer of ST2 (suppression of tumorigenecity 2) and its coreceptor of IL1RAcP (IL1 receptor accessory protein). Because IL33 is produced in response to tissue damage, stress, and scratching of the skin, it is classified as one of the alarmins, which are also known as endogenous substance in danger-associated molecular patterns (DAMPs). DAMPs are released during cell necrosis, transduce danger signals, and are associated with Th2 skewing. IL33 is constitutively released by human tissues ( ), but in the skin of AD patients its expression is further increased, especially in children compared with adults ( ). Keratinocytes are producers of IL33, and IL33 can decrease filaggrin (FLG) expression at the gene and protein levels in keratinocytes from the skin of AD patients ( ). IL33 is specifically expressed in the skin and is associated with Th2 cells and ILC2 (group 2 innate lymphoid cells, which produce Th2 cytokines) infiltration, activation, as well as with Th2 cytokine production ( ). In addition, IL33 affects mast cells in that it colocalizes with IL2-producing mast cells in chronically inflamed skin ( ).
IL25 (also known as IL17E) is a member of the IL17 family and binds to a heterodimeric receptor complex of IL17RA and IL17RB ( ). It is important in inducing Th2-skewing immune responses, and it is produced by epithelial cells (including keratinocytes) and endothelial cells, as well as by DCs. Its level is elevated in the skin of AD patients and negatively affects FLG expression at the gene and protein levels ( ). IL25 links impaired skin barrier function with Th2-mediated skin inflammation in AD patients. Because ILC2 expresses IL17RB as well as ST2 or TSLPR in human injured skin, IL25 can activate ILC2, but the functions of IL33 and TSLP to ILC2 differ from IL25. For example, KLRG1 (killer cell lectin-like receptor G1), which is a marker of ILC2 and highly expressed on these cells in AD patients, is upregulated by IL33 and TSLP, but not by IL25 ( ). In addition to ILC2, mast cells, basophils, and eosinophils are activated by IL25. The interaction among TSLP, IL33, and IL25 and the mechanism responsible for the differences in their roles remain to be clarified, but it is clear that Th2 cells and ILC2 respond to these cytokines and further exacerbate the lesional skin in AD.
Th2 cytokines
IL4, IL13, IL5, and IL31 are Th2 cytokines that play critical roles in the pathogenesis of AD. The importance of Th2 responses in the pathophysiology of patients with moderate-to-severe AD has been demonstrated by the marked improvement in skin barrier function, skin lesions, pruritus, and serum biomarker levels obtained following treatment with dupilumab (a human anti-IL4Rα antibody that blocks signals via both IL4 and IL13). IL4 and IL13, in particular, play central roles in development of AD pathogenesis. They bind a common heterodimeric receptor composed of the IL4Rα and IL13Rα1; IL4 also binds a heterodimeric receptor complex composed by IL4Rα and γC ( ). IL4 and IL13 are thought to be produced by mainly Th2 cells and ILC2. Mast cells, basophils, and eosinophils can also produce these cytokines. The receptor is expressed on DCs, keratinocytes, and eosinophils ( ). Keratinocytes differentiated under high IL4 and IL13 conditions show reduced FLG gene expression, even in the absence of FLG gene mutations. Binding of S. aureus and AMP production by keratinocytes trigger dysfunction of the skin barrier, promote TSLP production, and facilitate the Th2 injury responses in AD. This Th2 response induces IgE production. IL5 acts on eosinophil chemotaxis and activation. In the lesional skin and blood of AD patients, eosinophil numbers are increased ( ).
Other cytokines
IL31 belongs to the IL6 family. IL31 is produced by mainly activated Th2 CD4 + T cells and has proinflammatory and barrier-disrupting roles ( ). Granulocytes and mast cells are the additional sources of IL31 in AD patients ( ). IL31 gene expression and production are induced by IL4 and further promoted by IL33. IL31 signals to and functions in cutaneous nerves, dorsal root ganglia (DRG), epithelial cells, and keratinocytes through IL31 heterodimeric receptor complex, which is comprised of IL31 receptor A (IL31RA) and the oncostatin M receptor. Staphylococcal enterotoxin B is a potent inducer of IL31 from peripheral mononuclear cells of both healthy individuals and AD patients. IL31 binds IL31 receptor expressed on sensory nerves, facilitates the elongation and branching of the nerves, and causes pruritus. IL31 also stimulates the expression of IL-1β and the Th2-specific chemokine of CCL17 or CCL22, and decreases FLG expression, thus contributing to AD pathology. Control of the severe itching sensation that disturbs the sleep of AD patients can be improved by subcutaneous injection of anti-IL31RA antibody nemolizumab. Other targets for inhibition of IL31 activation include potential molecules of JAK (Janus kinase) inhibitors (targeting the signal pathway from IL31R engaged by IL31 in Th2 cells), dupilumab (an anti-IL4 receptor-α antibody), and EPAS1 (endothelial PAS domain–containing protein 1, a transcription factor that binds to the promotor region of the IL31 gene) ( ).
The IL17 cytokine family, produced by Th17-type helper T cells, contributes to host protection against infectious pathogens, but it also promotes the pathology of autoimmune diseases. IL17A (and its receptor IL17RA/IL17RC) is a founding member of this family ( ) and plays a major role in AD phenotype development. IL17A expression in the skin of AD patients is increased, especially in the acute phase, in pediatric patients, and in Asian AD patients ( ). In moderate-to-severe psoriasis showing similar pathogenesis with AD, IL17 also contributes to cause the pathophysiology. Ustekinumab, an IL12/IL23p40 blocker that inhibits Th1 and Th17/Th22 responses, effectively treats psoriasis. IL17A produced by Th17 cells affects keratinocytes to induce TSLP and CCL17, and is involved in the critical upregulation of IL4 signaling in mouse model ( ).
IL22 is a member of the IL10 family and binds a heterodimeric complex with IL22R1 and IL10R2. The main producers of IL22 are thought to be CD4 + T cells, CD8 + T cells, and mast cells in AD patients ( ). Recent studies have shown that a newly discovered, unique phenotype of Th22 cells can produce IL22, not IL4, IFN-γ, and IL17 ( ). Functional IL22 receptors are expressed on nonhematopoietic cells (i.e., epithelial cells) ( ) most highly in the skin. Keratinocytes produce higher levels of AMPs (β-defensins, lipocalin, LL37, S100A7, 8, 9) in response to IL22 in AD patients than in their healthy counterparts or in psoriasis patients, leading to enhanced proliferation of epithelial cells and induction of epidermal hyperplasia. Although AMP production is effective in protecting the skin from microbial invasion, excess AMP production promotes skin barrier dysfunction, leading to severe and chronic AD. In one study, the blood of adult AD patients had significantly higher levels of IL22-producing T cells expressing the skin-homing receptor cutaneous lymphocyte antigen (CLA) (IL22 + CLA + T cells) than did control adult or pediatric AD patients ( ); there was no difference in IL22 + CLA + T-cell numbers between healthy adults and pediatric AD patients. AD in infants and young children is thought to represent the initiation of AD pathology, with patients exhibiting the acute phenotype of adult AD, thus fewer IL22 + CLA + T cells in pediatric AD patients would suggest a role for IL22 in the progress of chronicity of AD, not its initiation.
Chemokines
Chemokines in atopic dermatitis: An overview
The pathophysiology of AD is characterized by inflammatory cell infiltration into the enflamed skin. Chemokines play a key role in promoting these infiltration events, and excess chemokines production can be observed in the skin lesions. Chemokines are cytokines with chemotaxis activity; they have a low molecular weight (8–14 kDa) and are divided into four classes (CC, C, CXC, CX3C) on the basis of their N-terminal conserved cysteine residue ( ). Chemokines are produced by various cell types; in AD they are produced mainly by epithelial cells, including keratinocytes, Langerhans cells, lymphocytes, vascular endothelial cells, and fibroblast. They bind to receptors expressed on target cells and induce chemotaxis. Chemotaxis is the migration of cells induced by chemical substances; by chemotaxis, cells can move toward or away from the source.
Many chemokines, such as CCL1 (I-309), CCL2 (MCP-1), CCL3 (MIP-1α), CCL4 (MIP-1β), CCL5 (RANTES), CCL11 (eotaxin), CCL24 (eotaxin-2), CCL26 (eotaxin-3), CCL13 (MCP-4), CCL17 (TARC), CCL18 (PARC), CCL20 (LARC/MIP-3α), CCL22 (MDC), CCL27 (CTACK), CXCL12 (SDF-1α), CXCL9 (Mig), CXCL10 (IP-10), CXCL11 (ITAC), and CX3CL1 (fractalkine), are associated with the pathophysiology of AD ( ) ( Table 13.1 ).