4 Orbital Blowout Fractures
DEFINITION
The term blowout fracture of the orbit refers to a fracture of an orbital wall, typically the orbital floor or medial wall, or both, with an intact bony orbital rim. This was felt to be caused by an isolated blow to the eye, displacing it posteriorly, and thereby, hydraulically increasing orbital pressure to the thin bony orbital walls, rupturing them outward. Recent evidence has suggested that this fracture may also result from a blow directed to the orbital rims, causing them to bend without fracturing, resulting in buckling of the thinner bone of the orbital walls.
These fractures may occur after any blunt frontal trauma to the globe or orbital rims and may occur even in the absence of sufficient force to cause a “black eye.”
DIAGNOSIS
Signs and symptoms suggestive of an orbital blowout fracture should be sought in all patients who have sustained blunt periorbital trauma. These include eyelid ecchymosis, limitation of extraocular muscle excursion, subcutaneous emphysema, and enophthalmos or hypo-ophthalmos. A pathognomonic sign of an orbital floor fracture is the finding of hypesthesia of the ipsilateral cheek, upper teeth, or tip of the nose. This occurs because the fracture usually extends through the infraorbital groove and canal along the floor of the orbit, injuring the infraorbital neurovascular bundle.
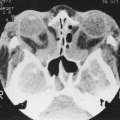
Radiographs may show disruption of the orbital floor and opacification of the maxillary sinus. However, some fractures will not be evident on plain films, and if one’s index of suspicion is high, coronal and sagittal computed tomography (CT) scans are indicated to definitively examine the orbital walls.
INITIAL MANAGEMENT
At the time of the initial consultation, a thorough ocular examination should be performed. Significant ocular injuries have been reported to occur in 10% of patients. Any limitation of extraocular excursion should be quantitated, and if the degree of swelling allows, forced duction testing should be performed to distinguish restrictive from paretic motility dysfunction. Exophthalmometry should also be performed.
The patient is instructed to refrain from taking any anticoagulants and advised not to blow the nose. If there are no contraindications, oral prednisone, 1 mg/kg daily, may be given for 1 week. Prednisone reduces long-term motility dysfunction as well as more rapidly delineates those patients who will require surgery. Fractures involving the medial wall have a greater incidence of orbital cellulitis, and some authors have recommended broad-spectrum antibiotic prophylaxis for 5 days in this subgroup.
SURGICAL INDICATIONS
Fewer than 50% of patients with orbital wall fractures will require surgical intervention. Orbital blowout fractures likely to require treatment fall into two categories: small fractures, which are more likely to result in tissue entrapment and motility dysfunction, and large fractures, which are more likely to cause ocular displacement owing to a substantial increase in bony orbital volume. Historically, the practice was to observe the patient every few days during the first 2 weeks after the injury, looking for change in extraocular motility dysfunction and forced duction testing as well as assessing enophthalmos, prior to recommending surgery. However, we now know that patients with tight entrapment of the inferior or medial rectus muscles in a “trap door” fracture should be operated urgently to prevent permanent dysmotility. Conversely, patients with larger fractures can be operated upon after extensive delay without suffering adverse outcomes. In fact, delay in surgery until enophthalmos is fully expressed may result in a better long-term volume correction.
One should obtain coronal and sagittal reconstructed orbital CT scans of all patients to allow assessment of soft tissue entrapment and remaining orbital bony support, which may be helpful in planning surgical placement of implants.
TIMING OF SURGERY
As mentioned above, surgery should be performed urgently on patients with true entrapment of an extraocular muscle. These patients will usually show marked restriction of globe excursions, often associated with pain and nausea and sometimes bradycardia may occur due to an oculocardiac reflex. If a patient has less marked restrictions of gaze, this usually will clear over time with observation but may take longer than the 2-week period that was historically recommended for observation prior to operation. Several studies have shown that delay for even many months prior to surgery in this group of patients does not negatively impact ultimate motility. As previously mentioned, delay until enophthalmos is maximally evident is actually associated with improved outcomes when compared to patients whose fractures are treated early in the postinjury period.
GOALS AND PRINCIPLES OF SURGERY
Orbital blowout fracture repair is performed on those patients with persistent tissue entrapment, resulting in a mechanical restriction of ocular movement, or noticeable enophthalmos. The goal is to elevate orbital contents out of the fracture site and then to resurface the orbital floor with either an alloplastic implant or an autogenous graft.
Patient Preparation
General anesthesia is used. A broad-spectrum antibiotic and 12 mg of dexamethasone are given intravenously at the start of the procedure. Before the surgical scrub, local anesthetic with epinephrine is infiltrated across the width of the lid, so that 10 minutes will have elapsed before the incision is made, allowing maximal vasoconstriction. A full-face preparation is performed. When draping the patient, both eyes should be left exposed so that bilateral forced ductions can be made and compared intraoperatively.
Selection of Approach
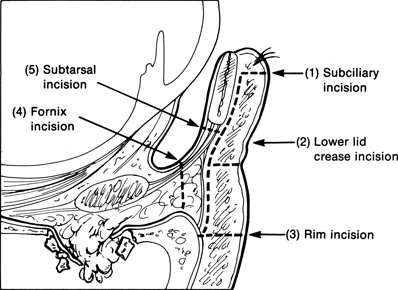
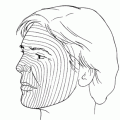
Figure 4-1. Several different approaches can be used to access the orbital floor. One can perform either an anterior approach through a lower lid crease incision or a posterior approach through the conjunctiva, in conjunction with a lateral canthotomy and inferior cantholysis. Either approach allows entry into the plane between orbital septum and orbicularis muscle. Dissection is then performed within this plane, down to the infraorbital rim.
The percutaneous approach is a simpler procedure without the need to disrupt the lateral canthus. The disadvantages are that it leaves a facial scar (although usually almost imperceptible) and, especially in younger patients, it may cause contracture of the skin-muscle flap postoperatively, resulting in lower lid retraction. The advantages of the conjunctival approach are the lack of a visible scar and reduced risk of lid retraction. The disadvantages are that disinsertion of the lateral canthal tendon is required and medial exposure is more limited. More extensive canthotomy and incision of orbicularis muscle laterally are required to fully expose medial wall fractures.
Lid Crease Approach
The lower lid crease is marked across the width of the lid, and forced ductions of each eye are performed and compared, to establish a baseline. An incision of the lower lid crease is made with a size 15 Bard-Parker blade or straight iris scissors. This begins medially at the punctum and extends laterally to a point at or just beyond the lateral canthus. A bipolar cautery is preferred for maintenance of hemostasis in blowout fracture repair and other orbital surgery, as a unipolar cautery may be preferentially conducted along orbital nerves. After the skin is incised, scissors are used to snip full-thickness through the orbicularis muscle to expose the postorbicular fascia. This is a thin layer of connective tissue on the surface of the tarsus and septum. Dissection is then carried interiorly between the orbicularis muscle and the orbital septum. Scissors are quite helpful in separating the orbicularis fibers from the underlying orbital septum, and Guthrie skin hooks are used to place anterior traction on the skin-muscle flap to keep the plane of dissection well defined. Dissection is carried down to the infraorbital rim in this fashion.
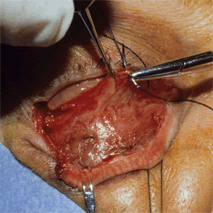
Transconjunctival Approach
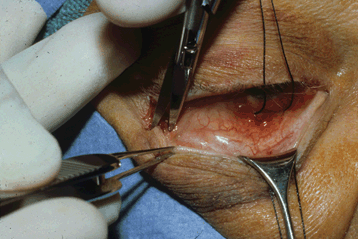
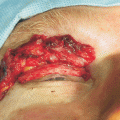
Figure 4-2. At the start of the procedure, a lateral canthotomy is carried out, with a scissors directed horizontally, extending 3 to 5 mm in length. The scissors are then rotated 90° interiorly and insinuated between skin and conjunctiva, cutting all the tissues of the lateral retinaculum in between. Several snips are required to cut through the lateral canthal tendon and the overlying orbicularis muscle until the lateral edge of the lid can be completely distracted from the orbital rim.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree