Fat grafting is as a unique regenerative filler with soluble factors and progenitor cells that may remodel scar tissue in an easy yet effective way. A combination of microfat grafting, lipococoncentrate injection, scar subcision, and platelet-rich plasma supplementation may be used to treat the majority of facial scars. The lipoconcentrate technique condenses the lipoaspirate to a progenitor cell-rich fluid of low volume by a combination of centrifugation and emulsification steps. In this article, the authors’ methods for scar treatment by fat grafting are discussed. Choice of technique for facial scars, precise indications, and contraindications are introduced.
Key points
- •
Growth factors and adipose-derived stem cells are the molecular and cellular sources respectively for the regenerative effect of fat grafts.
- •
The addition of platelet-rich plasma may support the effect of fat grafts.
- •
Facial scars require accurate preoperative evaluation in order to use the right technique.
- •
Emulsified nanofat, also called lipoconcentrate, is particularly useful in facial scar treatment due to its low volume and high content of regenerative cells.
Introduction
The regenerative effect of adipose tissue and its inherent cells is unquestioned, as intense research efforts over many years have shown. The source for the reparative function of adipose tissue is believed to be of cellular as well as molecular nature. The multipotent mesenchymal stem/stromal cells within adipose tissue, called adipose-derived stem cells (ASCs), are widely accepted as cells with broad differentiation and proliferation capacity. Moreover, soluble factors, including enzymes, cytokines, and growth factors, add to the tissue modulation.
Besides cosmetic facial and body contouring, fat grafting has emerged as a credible solution for the reconstructive treatment of facial scars in particular. Facial scars, often perceived as extremely disfiguring as well as stigmatizing for patients and at the same time tedious to treat, seem to greatly benefit from the regenerative properties of autologous fat tissue.
In the present work, the technique for regenerative fat grafting of facial scars as applied and optimized over many years by the first author is presented and discussed in detail.
Preoperative evaluation and special considerations
A careful patient selection is the first and probably the most important step of successful treatment. Although fat grafting is an undeniably powerful tool in plastic surgery, it cannot eradicate scars completely, as requested by some patients. Thus, thorough consultation, even more so in patients with unrealistic expectations, is mandatory.
Fat grafting should be considered for patients with mature, flat, and even facial scars at the level of the skin. Also, mature scars with signs of moderate or even severe retraction are good indications. Finally, mature scars with loss or disturbed pigmentation are regarded as feasible for autologous fat grafting, although a complete restoration in color may be difficult.
Scars that cause an intrinsic/extrinsic ectropion of the eye or lead to contractions of the mouth are regarded as contraindications for lipofilling and should be addressed by alternative surgical procedures. Moreover, immature scars are a relative contraindication for fat grafting. Scars that did not pass a maturation period of a minimum of 3 months should be treated only in special cases because, during this early period, the scar tissue undergoes a considerable remodeling processes with an inflammatory component. Although the current literature does not deliver exact definitions on the precise timing of fat grafting of scar tissue, the authors do not recommend fat grafting during this period for 2 reasons: on the one hand, the true extent and character of the scar cannot be assessed, and, on the other hand, it is not fully understood whether fat grafting may fuel the inflammation during this active remodeling stage. Patients have to be carefully advised to patiently wait for complete scar maturation and undergo close reevaluation. Also, scars that may be older than 3 months but still show signs of inflammation, such as redness, itchiness, and pain, are first treated with repetitive sessions of topical intradermal corticosteroid injections. The authors specifically use triamcinolone applied by Dermojet (Dermojet, Friedrichshafen, Germany), a needleless high-pressure injection device. Another rare but strict contraindication are scars that show signs of malignancy where fat grafts seem to promote cancer growth.
Surgical procedure
Liposuction
The procedure starts with the harvest of adipose tissue. The authors prefer the abdomen ( Fig. 1 A) as the primary donor site, but other areas, such as flanks or thighs, may be selected, depending on the preference of the performing plastic surgeon and patient. The authors investigated the content of soluble factors, stromal vascular fraction (SVF) cells, and ASCs in lipoaspirates from the abdomen, knee, and thighs earlier. Although the content of matrix metalloproteinase (MMP)-9 was significantly higher in lipoaspirates from the abdomen compared with the knee, the concentration of other growth factors, SVF cells, and ASC count showed no statistical difference between the 3 donor sites. Therefore, the authors conclude that the donor site for fat harvest can be well discussed with patients before surgery.
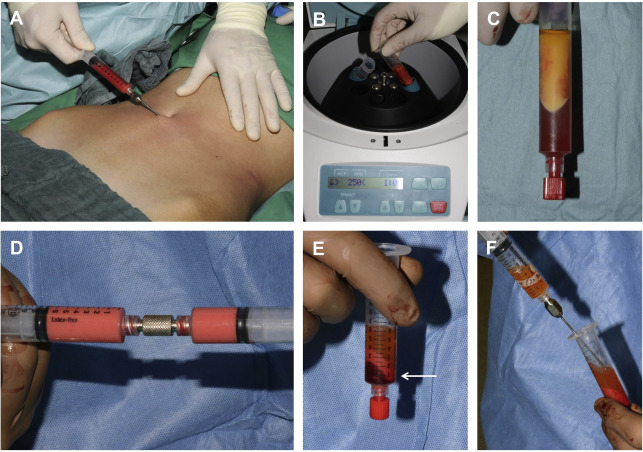
The harvest site is injected with tumescent solution containing adrenaline suspended in saline solution in a ratio of 1:200,000. Liposuction is performed by a handheld 10-mL syringe connected to a blunt-tipped thin cannula, with a diameter of 2 mm, and 4 orifices, each gauge measuring 600 µm (Thiebaud Biomedical Devices, Margencel, France). The lipoaspirate harvested by this method is called microfat. In an earlier study, the authors showed that microfat has significantly higher vascular endothelial growth factor (VEGF) and insulinlike growth factor levels compared with conventional lipoaspirates harvested by a thicker single-hole cannula with a diameter of 3 mm.
Processing
For facial scar tissue, 2 different types of fat grafts generally are used: microfat and the recently described lipoconcentrate.
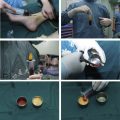
For processing of microfat, the lipoaspirate is centrifuged at 1200 g for 3 minutes (see Fig. 1 B). This leads to an upper oily, central fatty, and lower watery layer (see Fig. 1 C). The oily and watery layers are removed and the purified fat is injected.
For lipoconcentrate processing, microfat is emulsified by shifting between 2 syringes connected by a female-to-female connector for a total of 30 times (see Fig. 1 D). The second round of centrifugation, at 1200 g for 3 minutes, again leads to 3 layers, with the lipoconcentrate being the middle layer (see Fig. 1 E). The upper oily and lower watery layers are discarded manually (see Fig. 1 F) with great care not to disturb the lipoconcentrate. The remaining lipoconcentrate, a cellular suspension with low volume and high numbers of SVF cells, including progenitor cells, is injected.
Recipient Site Preparation and Injection
Microfat is injected subcutaneously through a 21G cannula whereas the lipoconcentrate can be injected subcutaneously and/or intradermally through a 27G cannula. Optionally, microfat or lipoconcentrate can be further enriched by platelet-rich plasma (PRP) in a ratio of lipoconcentrate 70%:PRP 30%. The authors commonly use the A PRP Kit (Regen Lab SA, Lausanne, Switzerland) for PRP isolation.
For flat scars and plaque-like plane scars, the scar tissue is first infiltrated with modified tumescent solution (adrenaline in saline solution, ratio of 1:200,000). After an interval of approximately 10 minutes, the lipoconcentrate is injected into the flat scars by mesotherapy technique (Steriject Wanted Biophymed U225 Mesotherapy Injector, TSK Laboratory Oisterwijk, Netherlands). For hyperpigmented scars, lipoconcentrate enriched with PRP is used because in the authors’ experience, PRP is an easy albeit effective measure for hyperpigmentation. Similar observations were made by Cayırlı and colleagues, who successfully treated melasma patients with PRP and found more than 80% of reduction in epidermal hyperpigmentation after 3 PRP sessions.
For retracted scars, the scar area is first injected by tumescent solution followed by subcision underneath the scar by a cannula. By this technique, also called rigottomy, the fibrous bands that strongly tethers the scar to deeper layers is mechanically released and then can be filled with microfat, which is subdermally injected. PRP may be added to the microfat to enhance the survival and ingrowth of the transplanted fat and increase ASC proliferation. Finally, lipoconcentrate is injected via mesotherapy technique with additional supplementation of PRP in case of hyperpigmented scars.
Postoperative care
The postoperative care in all cases consists of careful application of antibacterial ointment to the treated area. Administering additional heparin cream may help to resolve ecchymosis. Compression dressings, cooling, and topical/systemic corticosteroids should strictly be avoided to allow the transplanted fat grafts and PRP to exert their reparative functions and support fat grafts to settle at their recipient site. Manual lymphatic drainage should be started in the third postoperative week; gentle scar massage should commence approximately 6 weeks after surgery.
Expected outcome and management of complications
The whole extent of scar improvement by fat grafting with or without PRP treatment is evident a few months after surgery. During that time, the transplanted cells adjust to their new environment and gradually exert their regenerative effect. Because this is an overall slow process, patients need to be consulted accordingly. Preoperative and postoperative photographs as well as regular reevaluation may help during this stage.
Complications of microfat, lipoconcentrate, and PRP treatment are extremely rare. Minor complications include ecchymosis, pain, swelling, and light infections at the donor as well as recipient site. Major complications in the face are mostly vascular incidences that may result in skin necrosis or even blindness as reported in the literature. The authors have not experienced any major complications so far by adhering to following key rules: no injection under high pressure, aspiration prior to injection, injection while withdrawing the cannula, and most importantly a detailed knowledge about the anatomy and the course of facial blood vessels. The authors also strictly refrain from injection of fat tissue into the facial muscles.
Revision or subsequent procedures
In severe cases of extensive scar tissue, multiple sessions of microfat/lipoconcentrate with or without PRP may be required to reach the optimal results. Overcorrected areas may be treated by careful liposuction after a minimal interval of 6 months to 12 months.
Case demonstrations
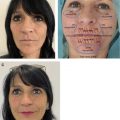
Case 1
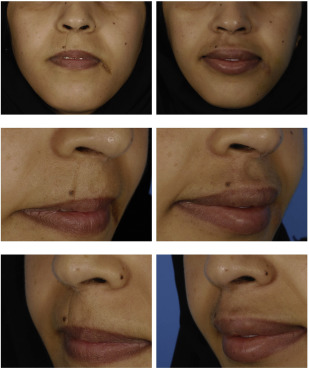
This 27-year-old female patient presented with posttraumatic scars after injury in her childhood on the upper right lip and lateral to the lower left lip ( Fig. 2 ). The vertical scar on the upper lip showed no significant change of pigmentation but a certain degree of retraction. Due to its thin straight line-like shape parallel to the rather poor developed right philtral column, the scar was fairly visible even from long distance. The scar lateral to the left lower lip showed a patch-like appearance with significant hyperpigmentation and tension that troubled the patient. Both scars were mature with no signs of inflammation. Aside from scar correction, the patient also asked for augmentation of the lips. She was informed that the hyperpigmented scar on the left lower lip may be difficult to treat in its color by a single treatment. In 1 surgical session, fat was harvested from the abdominal area. A total of 3 mL of microfat was injected into the upper lip and 3 mL to the lower lip for cosmetic augmentation, which also resulted in a better-defined philtrum as requested. The scar on the upper lip underwent rigottomy and was treated with a total of 1.5 mL of lipoconcentrate. The scar lateral to the left lower lip was infiltrated with 2 mL of lipoconcentrate supplemented by PRP. Postoperatively, the upper lip scar was markedly less visible. The lower lip scar tissue became more flexible and less irritating during opening of the mouth and showed slight improvement in color. The hyperpigmentation was not fully improved, however, and additional surgical sessions may be performed in the future.