Facial fat grafting is a small-volume procedure and is primarily performed for facial rejuvenation, contouring, or regenerative surgery. The unsatisfying retention rate after fat grafting, however, led to unpredictable outcomes, subsequent multiple procedures, and even some complications. A variety of methods have been proposed to enhance the results of facial fat grafting, including several established surgical principles and many possible new techniques. Adding stem cells, fat preparations, and platelet concentrates may improve the survival after fat grafting but randomized controlled clinical studies are needed to determine their safety and efficacy as well as clinical indications for each technique.
Key points
- •
Fat grafts should be processed with centrifugation that can reliably produce high-density fat, which concentrates adipose-derived stem cells and reduces inflammatory response, all of which are beneficial to graft retention.
- •
Stem cells, such as adipose-derived stem cells and bone marrow–derived stem cells, have been reported to be cotransplanted with facial fat grafting, but the efficacy and safety still need further studies to support.
- •
Nanofat and stromal vascular fraction gel could largely facilitate the application of fat grafting for facial rejuvenation that can be injected intradermally.
- •
Platelet concentrates, such as platelet-rich plasma and platelet-rich fibrin, have been proposed to combine with facial lipofilling, although the results remain controversial.
Introduction
Fat grafting has been widely performed for reconstructive or cosmetic purpose around the world, attributed mainly to its rich sources, easy harvesting, and minimal invasiveness as a surgical procedure. It can be arbitrarily divided into 3 categories based on volume needed. The “3 categories” are small-volume fat grafting (<100mL), large-volume fat grafting (100–200 mL) and mega-volume fat grafting (>300 mL). Facial fat grafting is a small-volume procedure (<100 cm 3 ) and is primarily performed for facial rejuvenation, contouring, or regenerative surgery. The unsatisfying retention rate after fat grafting, however, led to unpredictable outcomes, subsequent multiple procedures, and even complications. A variety of methods have been proposed to enhance the results of facial fat grafting, including several established surgical principles and many possible new techniques. This article primarily summarizes recent scientific studies on standardized techniques for autologous facial fat grafting. In addition, several possible new techniques used in facial fat grafting are reviewed.
Surgical principles
Donor Site Selection
There are various donor sites with abundant adipose resources that are easily accessible in the supine position and suitable to harvest for facial lipotransfer, such as abdomen, thigh, flank, abdomen, knee, and buttocks. Until now, there has been little evidence of the optimal donor site for fat grafting. But the lower abdomen and inner thigh contain a higher density of adipose-derived stem cells (ADSCs) ; in addition, ADSCs isolated from thigh showed more robust adipogenic and angiogenic potential as well as higher expression of peroxisome proliferator-activated receptor γ2 (PPARγ2) and vascular endothelial growth factor (VEGF) than those from the abdomen. In addition, patients’ own characteristics play a critical role on ADSCs concentration, vitality, and functionality; for example, fat grafts harvested from a younger age group in women (<45 years old) show higher viability than older age groups. But considering the release of soluble regenerative-related growth factors, the abdomen may be a slight favorite than the inner thigh because of its higher soluble biomolecules concentrate. Moreover, the release of growth factors negatively correlated with age whereas the content of stromal vascular fractions (SVFs) and ADSCs showed no statistical significance between abdomen and inner thigh. Therefore, lower abdomen and inner thighs maybe more appropriate to be chosen as better donor sites for facial lipofilling.
Fat Graft Harvesting
The syringe aspiration could be considered a standardized technique of option for facial fat graft harvesting by using back-and-forth movement with a syringe which can mechanically and manually extract adipose tissue. It is especially practicable in facial fat grafting because of the small amount of fat requirement and its relatively less traumatic procedure. Generally, a selected and easy-operating incision could be performed with a no. 11 blade for the infiltration of the aesthetic solution. The tumescent solution is needed and usually infiltrated to the donor site 10 minutes to 15 minutes before adipose extraction for easier and less traumatic fat graft harvesting. It usually contains a low concentration (<0.05%) of epinephrine (for decreasing blood loss and bruising, hematoma, and possibility of fat embolism) and lidocaine (for donor site analgesia or hemostasis) in normal saline or lactated Ringer solution. Then, during fat graft harvesting, a 10-mL or 20-mL Luer Lock syringe is used and connected with a harvesting cannula. Previous research has demonstrated that liposuction by a barbed cannula yields more viable ADSCs than a smooth one without reduction the cell viability of the SVF. In addition, lipoaspiration is better performed within the superficial layer of the subcutaneous tissue because SVF cells are located more in the superficial layer. It should be performed evenly, and uneven changes on the skin surface should be avoided after liposuction. Aspiration should be performed gently with back-and-forth movements of the syringe with a 2-mL space vacuum of negative pressure generated in the syringe. Such lower suction pressure may cause less damage to adipocytes. Lipoaspirates are collected gradually inside the syringe.
Fat Graft Processing
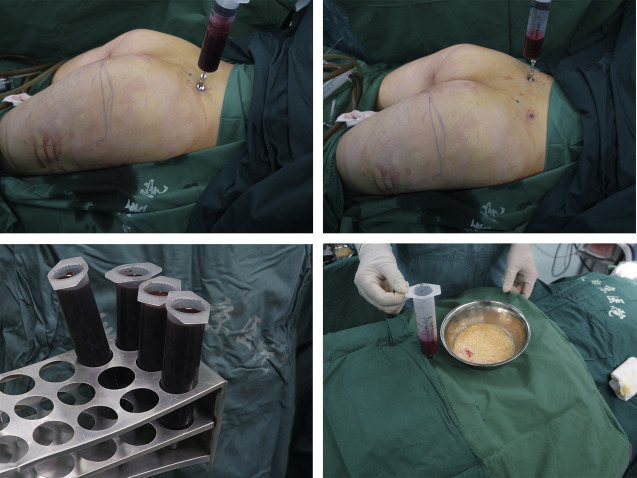
Various approaches have been developed to effectively concentrate aspirated fat before transplantation. Those popular techniques include centrifugation, filtration, washing, and gravity sedimentation. These diverse methods are controversial, however, and respectively focused on the most crucial factors among the regenerative remodeling procedures of fat grafts, such as maximizing the amount of ADSCs, preserving the greatest number of intact adipocytes, and decreasing the chance of contamination. Centrifugation at 1200 g (3000 rpm) for 3 minutes is a commonly used method to process harvested fat grafts, originally proposed by Pu. This process may yield more viable adipocytes with more optimal cellular functions. Further study demonstrated that centrifugation (1200 g, for 3 minutes) increases the density of SVFs proportional to the depth of grafts and more viable adipocytes mainly concentrated on middle and bottom layers. The bottom layer showed a higher tissue retention and a better histologic evaluation than the other 2 layers. Further clinical research has also proved that high-density fat that may yield more satisfying results. Possible mechanisms mainly contribute to its concentrating efficacy of viable cells and decreasing the inflammatory response by removing blood and debris.
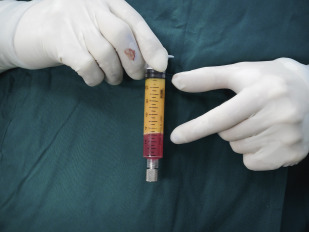
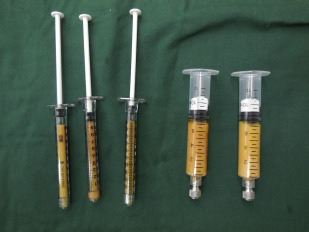
Harvested fat is transferred into several sterile 10-mL syringes and then carefully placed into a centrifuge symmetrically. After centrifugation in 3000 rpm (approximately 1200 g) for 3 minutes, lipoaspirates within each syringe are divided into 3 layers from top to bottom: top oil layer, middle adipose tissue layer, and bottom fluid portion layer ( Fig. 1 ). The top oil layer is decanted from the syringe and the bottom fluid is easily drained. The middle adipose tissue layer also can be divided equally into upper, middle, and lower layers, and the lower layer is primarily chosen and transferred into a 1-mL syringe for a more practicable facial lipotransfer whereas the middle layer of the fat is an alternative choice for further lipofilling ( Fig. 2 ). It is better to harvest more adipose tissue that may collect more high-density fat to yield better results for facial lipofilling. Based on the authors’ experience, the lower layer is injected for facial volume augmentation whereas the other 2 layers are then prepared as SVF-gel for intradermal injection that may improve the skin quality of the face.
Placement of Fat Grafts
The key to a successful fat graft injection is to achieve an even distribution of fat grafts in the recipient site that may improve the results and reduce the overall complications, such as fat necrosis. Further studies on the mechanisms of fat graft remodeling led to a better understanding of how to place processed fat grafts into the recipient sites, one of the most important techniques in facial lipofilling. The fat grafts should be placed dispersedly, which maximally contact with recipient site to facilitate infiltration of nutrients and neovascularization of fat grafts. A small amount of fat grafts (no more than 0.1 mL) in each pass may improve fat graft survival as well as avoid subsequent complications, such as oil cyst formation, fibrosis, calcification, and even fat embolism. A special device, the microautologous fat transplantation-Gun (MAFT-GUN, Taiwan) has been proposed. It is so delicate that it can inject each parcel volume at 1/60 mL to 1/240 mL. Fat grafts should be injected into multiple bypasses in multiple tissue planes and tunnels. The diameter of injected fat is directly dependent on the diameter of injection cannulas, and the most commonly used cannulas are 5 cm to 9 cm in length with a blunt tip and 1 opening on the side for facial lipofilling. Because the central necrosis of fat grafts may occur by using an injection cannula larger than 14G or injecting more than 0.1 mL in each pass, injecting very tiny volume in each pass and selecting smaller size of cannulas for facial fat grafting should be considred. Recipient site preparation, before facial fat grafting, also may be helpful to enhance the outcomes of lipotransfer. Microneedling has been shown to improve the retention of grafted fat by virtually increasing neovascularization via triggered complex cascade of multiple growth factors. Further studies are necessary to provide more convinced evidences for its clinical application.
Additional Considerations
A recent study proposed that the facial fat compartment plays a crucial role in improving the overall outcomes of facial lipotransfer. Facial fat compartment was first reported by Rohrich and Pessa through an anatomy study and the results found that the subcutaneous fat in the face was partitioned into several independent anatomic facial fat compartments. Those multiple fat compartments are separated by fascial condensations and form an interconnecting framework, which provides a retaining system for the face. Aging-dependent changes are strongly linked to the voluminal changes of facial fat compartments, which a significant volume of deep fat was decreased over time. Knowing these anatomic characteristics would largely help performing a more specifically and more precision preoperative analysis for facial lipotransfer and could subsequently yield more satisfying results for facial rejuvenation.
The fat graft site should be immobilized after the first 5 days to 7 days for a better remodeling by taping over the grafted areas. A previous study showed that regional immobilization of the recipient areas may help prevent damage to newly formed vessels and enhance the function of ADSCs. Therefore, it is also important to inform patients to avoid excessive facial movements during the postoperative recovering period.
Possible new techniques for facial fat grafting
With the continuous research on the mechanisms of fat grafting, several novel concepts and techniques have been proposed to enhance the quality and retention after facial fat grafting ( Table 1 ). These methods were based primarily on experiments and clinical studies and can be divided into 2 approaches: adding extra components (such as stem cells and platelet concentrates) and fat preparations (such as SVFs, SVF-gel, and nanofat).
| Methods | Mechanism | Clinical Relevance |
|---|---|---|
| Stem cells | ||
| ADSCs | Directly differentiation ability and paracrine capability | Abundant resources |
| BMSCs | Feasible for slim patients | |
| Fat preparations | ||
| SVFs | Heterogeneous cell population | Clinically feasible |
| Nanofat | SVF cells without adipocytes | Intradermal injection |
| SVF-gel | High density of SVF cells and extracellular matrix | Effective for both volumization and rejuvenation |
| Platelet concentrates | ||
| PRP | Growth factors and plasma | Food and Drug Administration approved |
| PRF | Growth factors and 3-D fibrin scaffold | Clinically feasible without any exogenous additives |
| CGF | Growth factors, 3-D fibrin scaffold, and CD34 + cells | The safety and efficacy not yet determined |
The Use of Stem Cells for Facial Fat Grafting
Bone marrow–derived stem cells
Bone marrow–derived stem cells (BMSCs) exhibit self-renewal capacity and multipotency and can be induced to differentiate into multiple cell lineages, such as adipocytes, osteocytes, and chondrocytes. It has been reported that BMSCs participate in the tissue regeneration/remodeling after fat grafting by contributing to form capillary networks and provide new ADSCs. Applying additional fresh BMSCs and expanded BMSCs could improve the outcome of fat grafting, as evidenced by a graft’s retention, quality, and neovascularization. It also is indicated that better efficacy has been achieved by using primary compared with expanded BMSCs, possibly because the multiple cell components found in freshly isolated BMSCs but not in homogeneous expanded BMSCs are important for graft retention. Moreover, cotransfer of bone marrow aspirate/bone marrow concentrate with fat grafting also has been proved a potential preferred choice to enhance the retention of grafted fat in a clinical setting ( Fig. 3 ). A further clinical trial has evaluated the applicability of BMSC-assisted fat grafting in patients with Romberg disease and found that it is more effective than conventional facial lipotransfer in terms of fat graft volume retention. This promising method may become the optimal choice for those patients who are thin, with minimal fat available for facial fat grafting. The mechanism of BMSCs enhancing the result of facial lipotransfer is possibly due to their promotion of neovasculogenesis and adipogenesis. The guidelines and standardized procedures for the clinical application of BMSCs, however, specifically those pertaining to their isolation, preparation, and injection and optimal numbers, have not been established, and the long-term safety of BMSCs and the detailed mechanisms remain to be confirmed.