Reparative, angiogenic, and immunomodulatory properties have been attributed to the cells in the adipose tissue–derived stromal vascular fraction. Because of these characteristics, in the last decade, fat grafting for treatment of autoimmune diseases has grown. This article focuses on systemic sclerosis, a rare autoimmune disease characterized by skin fibrosis and microvascular damage. Lesions of the face are almost always present; however, current therapy is insufficient and patients have considerable disability and social discomfort. This article presents our approach to using fat grafting in the face as an innovative and promising therapy for patients with systemic sclerosis.
Key points
- •
Systemic sclerosis is a rare autoimmune disease characterized by skin fibrosis, microvascular damage, and organs dysfunction.
- •
Facial signs are frequent and include perioral skin thickening, facial atrophy, and microstomia.
- •
Facial manifestations are disfiguring and lead to social disability with psychological distress.
- •
Autologous fat tissue grafting has emerged as a treatment of localized scleroderma and patients with systemic sclerosis–related perioral thickening and mouth opening limitation.
- •
Cell-based strategies to enrich fat grafts is a promising option in regenerative medicine.
Video content accompanies this article at http://www.plasticsurgery.theclinics.com .
Introduction
Systemic sclerosis (SSc) is a chronic systemic autoimmune disease characterized by progressive skin and internal organ fibrosis and microvascular abnormalities. Life-threatening organ lesions only affect a minority of patients. By contrast, lesions of the hands and face are almost always present. Although not life threatening, these manifestations are obvious, hard to conceal, and lead to disability and worsening quality of life. No antifibrotic treatment has proved effective. Unlike other autoimmune diseases, immunosuppressive drugs have a limited clinical interest. Thus, improvement of face motion and appearance represent a real challenge for physicians and a priority for patients who often think that this aspect of their disease is neglected.
Use of adipose tissue as filling product in plastic and aesthetic surgery is an ancient technique. Significant renewal of interest in this approach was observed after the description of the Lipostructure technique by Coleman. This approach, using the patient’s own body fat as a natural filler to achieve structural modifications, takes advantage of its abundance and accessibility. Elective liposuction for fat transplant is nowadays considered a safe and well-tolerated procedure. Identification of the adipose tissue–derived stromal vascular fraction, which includes mesenchymal stem cell–like cells, endothelial progenitor cells, and hematopoietic cells, has revolutionized the science showing that adipose tissue is a valuable source of cells with multipotency, angiogenic, and immunomodulatory properties that facilitate tissue repair. In SSc, the Coleman Lipostructure technique is not adapted because instruments do not enable direct fat grafting at a subdermic level or in layers that are poorly extensible or fibrotic. Microfat grafting, described by Nguyen and colleagues, is now currently used to restore soft facial tissue. The authors previously reported an improvement of facial handicap in 14 patients with SSc after autologous perioral microfat injection. However, the clinical success of fat grafting is limited by its variable and unpredictable local survival rate. One of the most promising developments in recent years is the use of prosurvival strategies to improve maintenance of fat volume and trophicity.
Recently, plastic surgeons have added platelet-rich plasma (PRP) to injected fat, hypothesizing that growth factors produced in vivo would enhance the neovascularization, proliferation, and differentiation of adipose stem cells, improving patient outcomes. More recently, the skin regenerative potential of nanofat grafting was studied by Tonnard and colleagues. The process consists of mechanical emulsification by manually repeatedly shifting the fat between 2 connected syringes followed by filtration of the lipoaspirate to obtain a homogeneous liquid suspension, defined as nanofat, which can be directly administered to patients. Because the obtained product does not meet the true dimensions required of nano sizes, the term emulsified fat is more accurate.
This article presents the authors’ clinical approach using microfat and emulsified fat enriched in PRP in the treatment of the face in patients with SSc.
Preoperative evaluation and special considerations
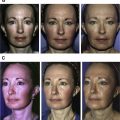
Involvement of the face, with associated oral complications, aesthetic changes, and impairment of the patient’s self-image, is found in more than 90% of patients with SSc. Table 1 and Fig. 1 show the main orofacial findings in patients with SSc.
| Orofacial Findings | Commentaries |
|---|---|
| Skin sclerosis of the face | Very frequent, around 90% of cases. The face becomes amimic, cutaneous wrinkles disappear, vertical furrows develop around the mouth caused by retraction of the skin, the nose becomes sharp and lips thin |
| Telangiectasia | Especially located in the face, lips, or the inside of the mouth, they can lead to severe aesthetic concerns |
| Skin pigmentation abnormalities | Hypopigmentation and hyperpigmentation mostly observed in the diffuse cutaneous form of scleroderma. Vitiligo is possible |
| Sicca syndrome | Sicca syndrome is detected in approximately 70% of patients with SSc. It is secondary to salivary gland fibrosis |
| Diminished mouth opening | Frequent, around 60%. Thinning of lips and reduction of mouth width (microcheilia) and opening (microstomia) with, as a consequence, difficult dental care |
| Osteolysis of mandibular angles | Mandibular bone resorption is mainly encountered in patients with marked facial skin fibrosis: chewing and swallowing movements may be impaired, pain is often reported |
| Altered dentition and difficulties during dental care | Oromucosal involvement include ulcerations, dry mouth, periodontitis, wide periodontal ligament space, dental root resorption, and loose teeth |
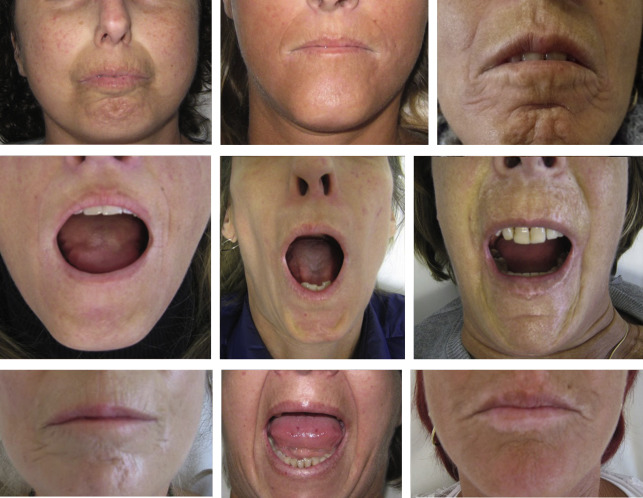
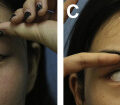
Facial involvement is associated with disfigurement and limited expression with a masklike stiffness of the face. The loss of elasticity and the thickening of the skin in the perioral area and lips form perioral radial furrowing and narrowing of the oral aperture, leading to mouth opening reduction that interferes considerably with basic functions such as eating, speaking, oral hygiene, and professional dental care. Furthermore, xerostomia because of salivary gland fibrosis and reduced saliva production increases the risk of periodontal diseases and caries.
Several validated tools have been developed for assessment of the involvement of the face. Skin involvement is usually assessed by the Rodnan skin score. This semiquantitative score rates the severity of skin sclerosis from 0 (normal) to 3 (most severe). Xerostomia can be easily measured by sugar test (time to melt a sugar cube on the tongue, without crunching it) and with the Xerostomia Inventory Index. Mouth opening is assessed in centimeters by measuring the distance between the tips of upper and lower incisor teeth. Elastosonography and three-dimensional photographs can also be used. Mouth-related disability can be assessed by the Mouth Handicap in Systemic Sclerosis (MHISS) scale, which is the first mouth-specific disability outcome measure designed for patients with SSc. This scale evaluates 3 factors: reduced mouth opening, sicca syndrome, and aesthetic concerns. The MHISS score explained up to 36% of the variance of the Heath Assessment Questionnaire score. This finding highlights the need to specifically assess disability involving the mouth in patients with SSc. Rehabilitation and management of the face is mainly based on physiotherapy with mimic exercises, massage, and self-administered home-based exercises. Mouth care and dental care are not specific.
Surgical technique using microfat and emulsified fat–enriched platelet-rich plasma
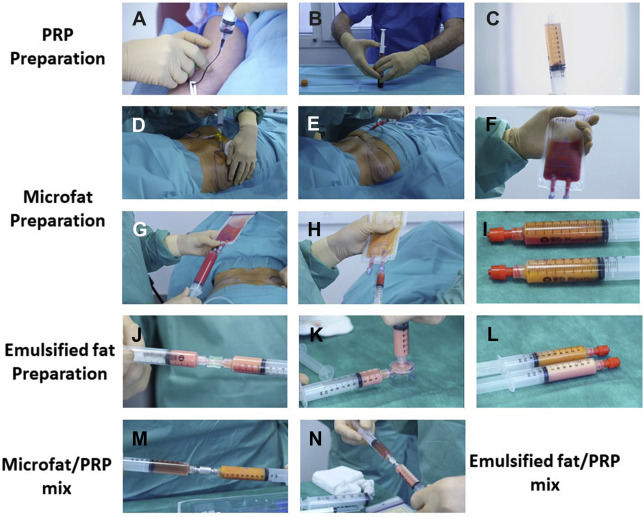
Reinjection of autologous fat tissue has volumizing and trophic properties. Coleman formalized the technique and nowadays most surgeons consider adipose tissue to be the ideal filler. However, the special context of SSc requires certain modifications to this approach; in particular, the use of harvest and implantation of smaller morsels or packets of adipose tissue. Thus, microfat grafting has been the first evolution of the art. This minimally invasive technique is now enriched with PRP, which contains high level of growth factors to improve microfat retention. Treatment of face disability in patients with SSc is currently completed with emulsified fat enriched with PRP for regenerative purposes, which has the advantage of passing through smaller needles (25–30 gauge) ( [CR] ).
Patient and Donor Site Selection
During the first consultation (after a clinical and photographic analysis), the surgeon checks the venous access for blood harvesting and defines the amount of adipose tissue necessary and the areas from which this tissue can be harvested. Preferred harvesting areas include the inner side of the knees, abdomen, external thigh, internal thigh, and back. The preferred location for small quantities is the inner side of the knees. In cases of previous adipose tissue harvesting or cryolipolysis, a nontreated area is preferred to avoid any fibrosis tissue. The procedure takes place under local anesthesia (supplemented with conscious sedation if needed) and can be performed either as outpatient or inpatient care.
Infiltration and Microfat Sampling
The first step is anesthesia of the entry points with a small syringe and a 30-gauge needle with pure lidocaine 1% and epinephrine (1 mg/L) to avoid bleeding. For infiltration of the harvested area, the authors use a modified Klein solution containing 200 mL of physiologic serum and 40 mL of lidocaine 1% and epinephrine (1 mg/L). Entry points are made with a 14-gauge needle, before inserting the infiltration/harvesting St’rim cannula (Thiebaud Biomedical Devices, Paris, France; 14 gauge, 2-mm external diameter, 8 holes of 0.58 mm square). Infiltration is performed in a closed system between a bag containing anesthetic solution and a cannula using the 3-way valve Fat Lock System (Benew Medical, Melesse, France) (yellow) ( Fig. 2 D). Diffusion of the anesthetic solution during 10 minutes before microfat harvesting is recommended. Microfat is harvested with the same St’rim cannula connected to both a 10-mL syringe and a purification Puregraft 50 (Solana Beach, CA) bag through a Fat Lock System (red) under a low vacuum keeping the plunger in contact with the fat ( Fig. 2 E). Approximatively 45 mL of microfat was collected ( Fig. 2 F).