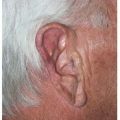
Lip Reconstruction
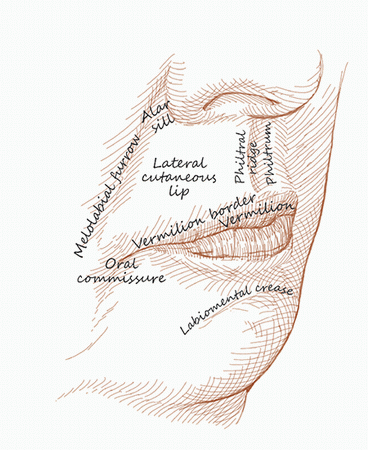 |
Critical in speech, sustenance, and conveyance of emotions, functional integrity of the lips requires preservation of oral aperture and competence as well as sensation and mobility. At the same time, the aesthetic importance of the lips is obvious by their central location, subtle variations in surface contour, color, and texture, and importance as a focus of facial beauty in society. Because of an absence of underlying cartilaginous or bony support, they are particularly sensitive to distortion of free margins and trapdooring (pincushioning) of flaps. In short, functional integrity and aesthetic appearance should be maintained, and unsightly scars, asymmetry, or distortion should be avoided.
6.1 LEFT UPPER CUTANEOUS LIP: SIDE-TO-SIDE REPAIR
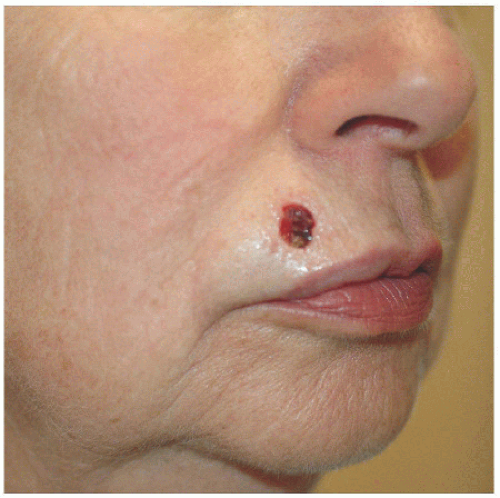
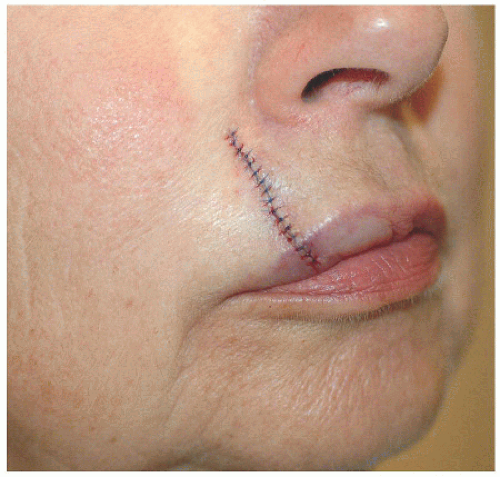
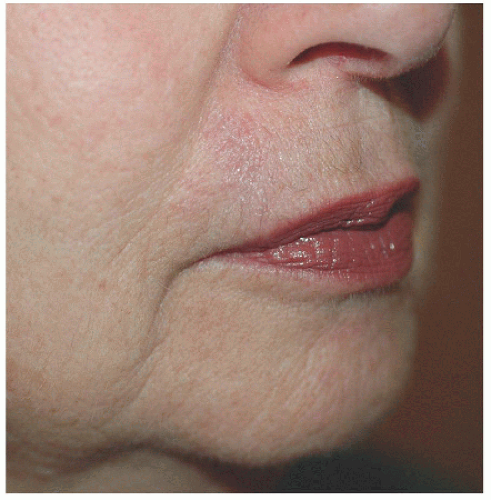
A side-to-side or complex linear closure is an excellent alternative for small defects on the upper or lower lip (Figs. 6.1A, B, C, D). Three key points should be stressed: (1) the wound should be closed in a direction perpendicular to the margin of the lip; (2) tricones or standing cones should be excised irrespective of whether or not excision will cross the vermilion border; and (3) the vermilion border, if crossed, should be accurately reapproximated. The first point avoids deviation of the free margin of the lip and places incision lines in actual or expected perioral rhytides. The second point prevents displacement of the vermilion border (Fig. 6.1E). And finally, if and when the vermilion is crossed, proper realignment should be ensured. The best approach is to mark out the border preoperatively with a surgical marker or to score the vermilion border. A poorly approximated vermilion border will likely require surgical revision subsequently.
Key Points
Wounds closed in a side-to-side fashion should follow the direction of perioral rhytides and approach the vermilion border at right angle to the border.
Do not hesitate to cross the vermilion border when excising standing cones. Too short of an excision will deviate the lip margin.
If you cross the vermilion border, carefully reapproximate it. (Start buried sutures at the vermilion border or just above it in order to ensure accurate reapproximation.)
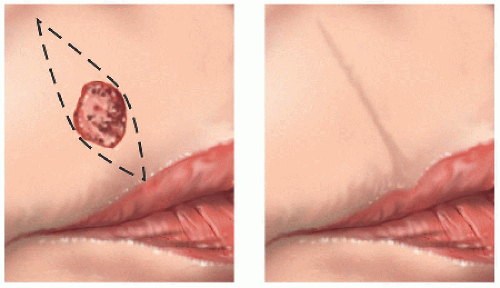
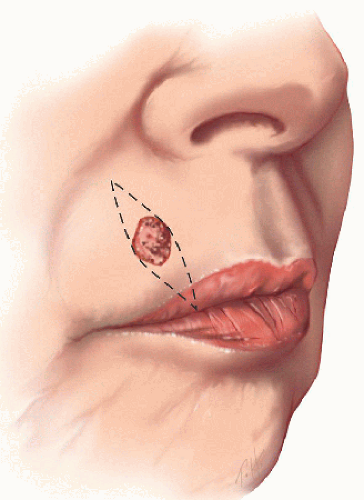 Figure 6.1B. Design of complex linear repair. Closed along relaxed skin tension lines in the direction of perioral rhytides. Appropriate-sized tricones must be removed and vermilion reapproximated. |
6.2 RIGHT UPPER LIP: ADVANCEMENT FLAP
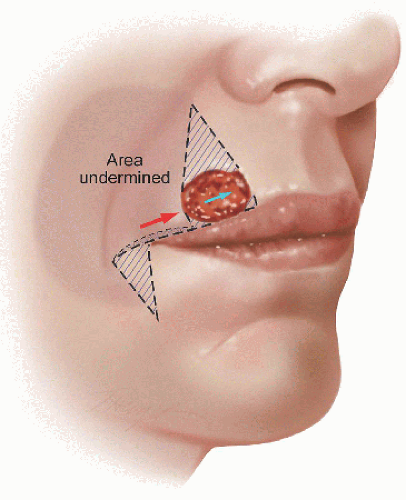
This defect is too large for a side-to-side repair unless the surgical defect was made full-thickness and the defect closed as a wedge excision (Fig. 6.2A). As the only tissue missing is the skin and subcutaneous fat, it is preferable to focus on reconstruction of those structures and leave intact the remaining healthy underlying tissues. Consider what is missing: skin and subcutaneous tissue, and consider where there is adequate tissue from which to borrow. In this case, the loose tissue is located laterally in the lateral lip and medial cheek.
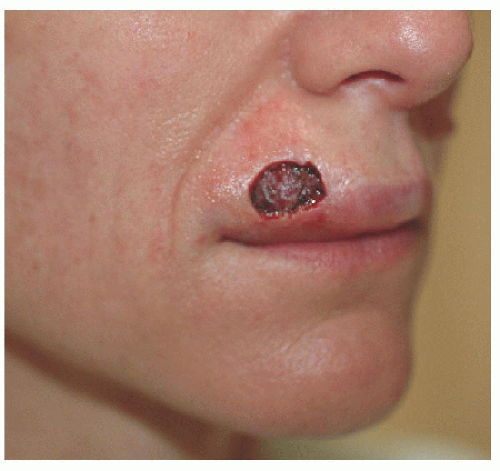 Figure 6.2A. Broad defect on the upper lip measures approximately 1.5 × 1.1 cm and is located just superior to the vermilion border. |
An advancement flap from the lateral lip and medial cheek is a good option for repair of this defect (Fig. 6.2B). Most of the incision lines will be well hidden, and the tissue is an excellent match for repair. To get started, if the defect does not extend to the vermilion border, it should be enlarged so that the repair and subsequent scar is located at the junction of the cosmetic subunits. The flap incision starts at the lateral-inferior aspect of the defect and continues laterally, following just above the vermilion border within what is referred to as the “white roll.” The incision continues past the oral commissure to the medial cheek, where a tricone is excised to allow advancement of the flap. The flap is undermined widely by blunt and sharp dissection in the superficial subcutaneous fat, extending onto the medial cheek from where the loose tissue is recruited. After adequate mobilization, the flap is advanced along the vermilion border and secured with absorbable buried vertical mattress sutures to the medial aspect of the surgical defect, being careful to avoid upward pull of the lip (eclabium) (Figs. 6.2B, C, D). Even with careful attention to the direction of flap movement, the flap may have a tendency to push downward the lateral aspect of the lip (“hooding”). This may be related to the progressive widening of the flap or to excessive soft tissue in the portion of the flap that extends lateral to the oral commissure onto the medial cheek. To avoid this downward pressure on the lateral upper lip, the flap should advance in the slight-upward direction of the vermilion border (slight-downward on the lower lip), avoiding upward or downward forces on the lip margin. If necessary, a very small crescentic portion of tissue may be removed along the flap border, but overly aggressive surgical resection and resultant eclabium should be avoided (Fig. 6.2B). It is easy to remove additional tissue in a secondary procedure, but much more difficult to add tissue when too much was removed in the first procedure.
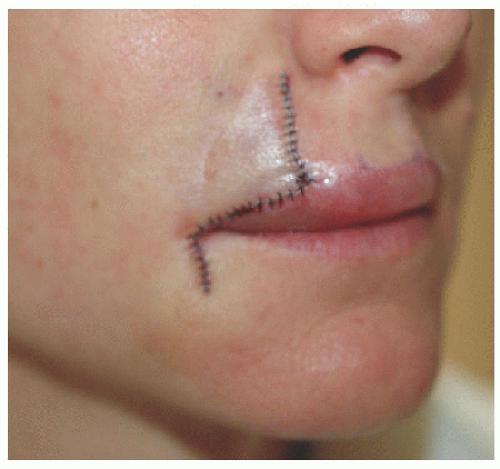 Figure 6.2C. The advancement flap sutured into place. The flap is advanced along the vermilion border, taking care to avoid downward or upward deviation of the vermilion border. |
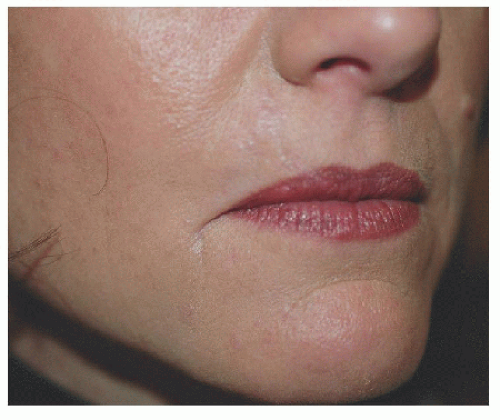
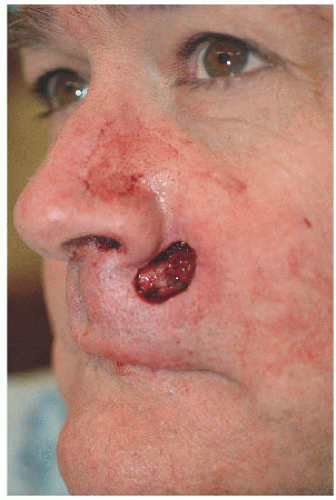
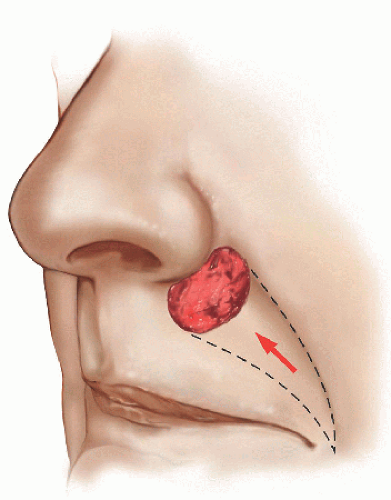
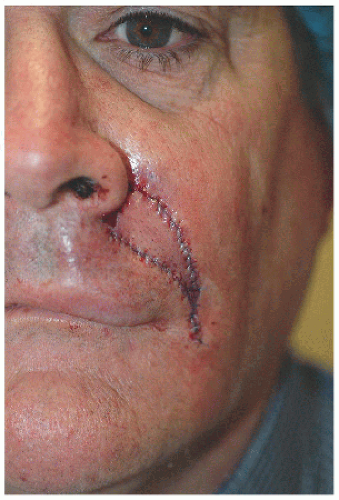
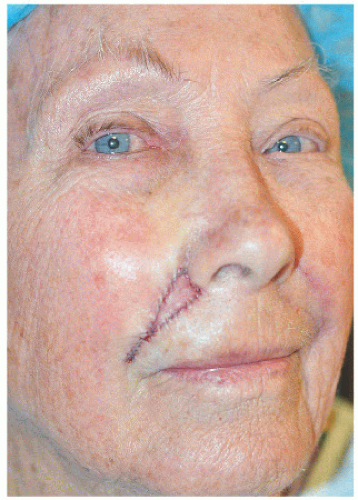
The second patient is older and the defect larger, but the principles remain the same (Fig. 6.2E). The adjacent loose tissue is located on the lateral upper lip and medial cheek. The advancement flap recruits tissue from these resources, and incisions are placed in locations where they will be best hidden within relaxed skin tension lines (perioral rhytide and marionette line) and a cosmetic subunit border (vermilion border) (Figs. 6.2F and G).
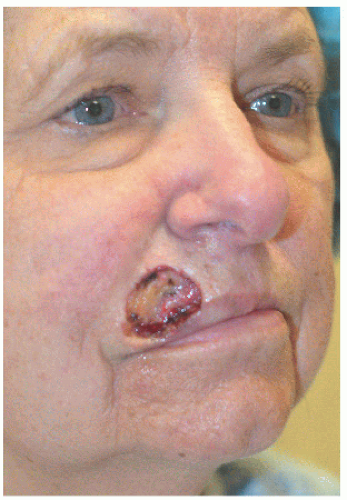 Figure 6.2E. Surgical defect on the right upper lip measures 2.9 × 2.2 cm and extends to the vermilion border. |
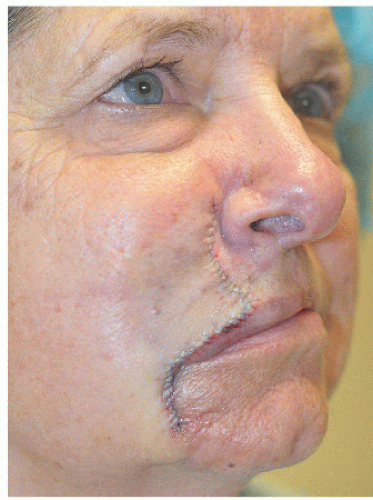
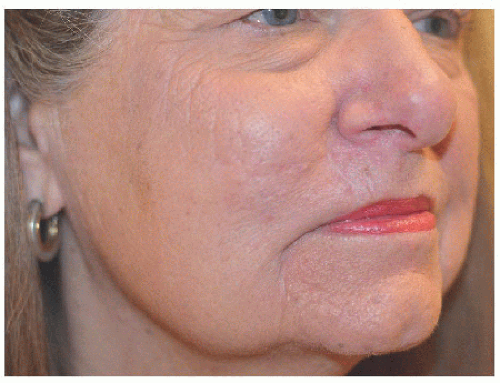 Figure 6.2G. Healed result at 5 months. Most incision lines are well healed along the vermilion border, marionette line, and perioral rhytide. |
Key Points
Incisions are placed just above the vermilion border within the white roll continuing past the oral commissure where a tricone is excised. Closure of this tricone falls within the marionette line.
Undermining is continued in the superficial subcutaneous plane onto the medial cheek from where the majority of loose tissue is recruited from.
The flap is advanced along the vermilion border, avoiding upward or downward deviation of the free margin.
Tricones excised upon advancement of the flap follow the direction of perioral rhytides.
6.3 UPPER LIP: ROTATION FLAP
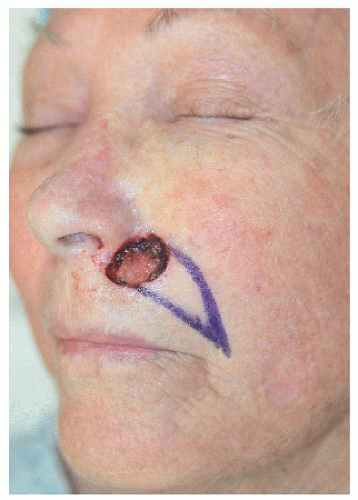
For many surgeons a defect such as this one on the upper lip near the alar sill is frequently repaired with a rotation flap (Fig. 6.3A). Although rotation flaps may work for this type of wound, they are not the author’s “go-to” repair for this region, especially for defects within the alar sill. Although much of the arciform incision is hidden within the melolabial fold, movement of the flap can cause some distortion or lifting of the oral commissure (as seen in Fig. 6.3B). At the same time, for a defect just outside the alar sill and perhaps too big for side-to-side repair, it may be the best option available. Transposition flaps tend to create too many additional incisions and scars, have a tendency to trapdoor, and may distort the lip if not designed properly. Crescentic advancement flaps may create asymmetry and blunting of the alar sill. In the author’s opinion, island advancement flaps are a better option for defects located within the alar sill (see Section 6.4); but for this defect sitting just outside the alar sill, the rotation flap worked fairly well. Much of the incision is hidden, and except for slight lifting of the oral commissure, the cosmetic result is quite acceptable (Fig. 6.3C).
Key Points
For small defects too large for side-to-side repair located just outside of the alar sill, a rotation flap may provide an aesthetic result, but too large of a rotation flap may cause lifting of the oral commissure.
The arciform incision should follow the melolabial furrow past the oral commissure, where a tricone may be excised or back cut created.
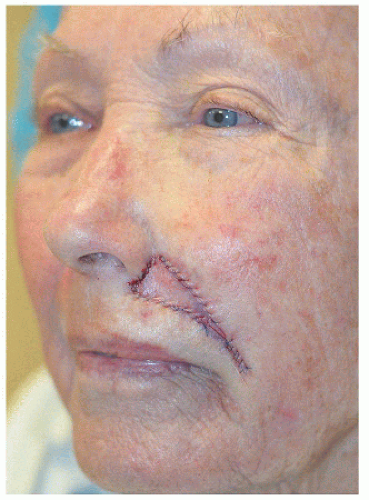
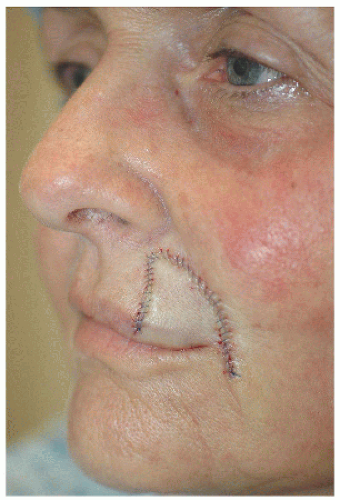 Figure 6.3B. Repair with rotation flap. Much of the incision is well hidden within the melolabial fold, but there is some mild lifting of the left oral commissure. |
6.4 ALAR SILL: ISLAND ADVANCEMENT FLAP
Unlike the example in Section 6.3, this defect falls within the alar sill, occupying the triangular peninsula of tissue bordered by the cheek, nose, and upper lip (Fig. 6.4A). Although some might consider rotation flap repair as seen in the earlier case, the same problems exist, namely lifting of the oral commissure or distortion of the lip. Another alternative that works well in this region is an island advancement flap. As these flaps lack a cutaneous attachment, they are more mobile than other random pattern flaps. The blood supply for this flap is entirely within the subcutaneous pedicle; so proper design of the flap and handling of the tissue is of key importance. There are a number of reasons that the island advancement flap works well here. The repair is kept within one cosmetic unit. One long side of the triangular flap and the base are placed at the junction of the cosmetic units; so the subsequent scars are fairly well hidden. The flap is very mobile, and secondary tension vectors do not lift the oral commissure or free margin of the lip as was seen with the rotation flap.
Successful design and execution of the island advancement flap in this location is dependent on a couple of key details. One long incision line follows the melolabial furrow while the second one crosses the lip, gradually tapering to a point where it meets the melolabial furrow incision (Fig. 6.4B). A more gradual taper minimizes secondary tension vectors and also minimizes the appearance of the more medial incision. After incision of the flap, the flap is mobilized by careful blunt and sharp dissection, first at the leading and trailing edges to minimize bulldozing and tethering, respectively. Next, undermining is continued along the sides of the flap. The key is to mobilize the flap while maintaining a healthy, robust vascular pedicle, which tends to be located approximately between the first and second third of the flap (measured from the leading edge). Use of blunt dissection scissors turned vertically and spreading the scissors help to divide the tissue and minimize trauma to the blood vessels. Once adequately freed, the leading edge of the flap is secured with absorbable, buried vertical mattress sutures (Fig. 6.4C). The secondary defect is closed and the long sides of the triangle are likewise secured with several buried, absorbable sutures. Finally, the epidermis is approximated and everted with a 6-0 polypropylene running percutaneous or with simple interrupted sutures (Figs. 6.4D and E).
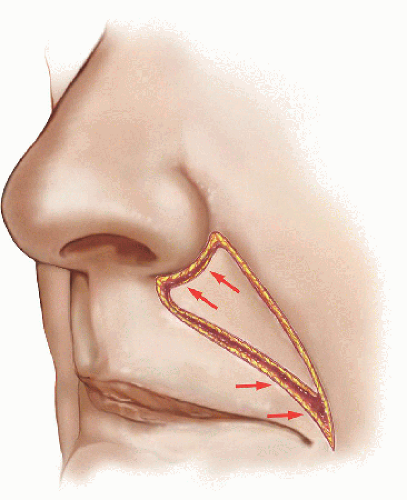 Figure 6.4C. Advancement of the flap. A long, tapering triangle decreases the secondary tension closure on the upper lip and makes the transition from cheek to upper lip natural in appearance. |
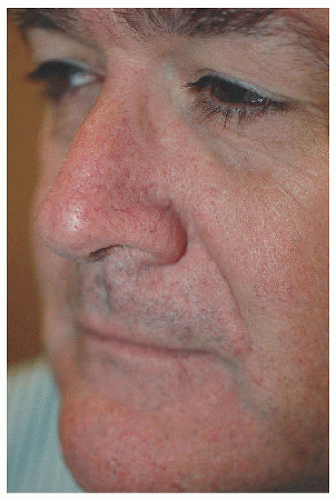 Figure 6.4E. Healed result shows incision line well hidden in melolabial furrow and good reconstruction of alar sill without blunting, which can be seen in some other types of repairs. |
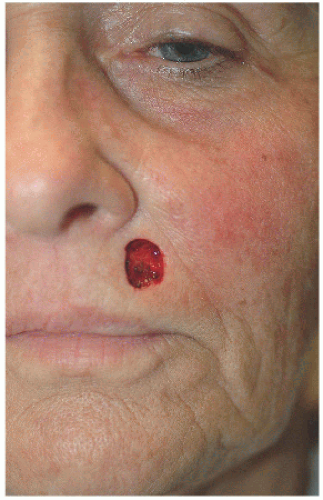
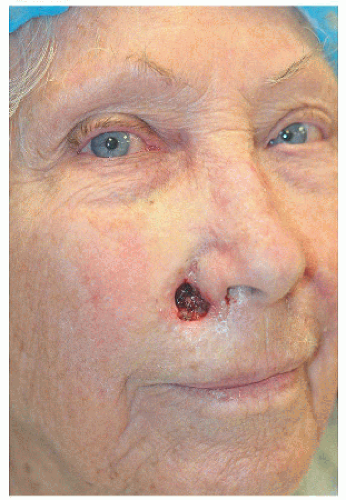
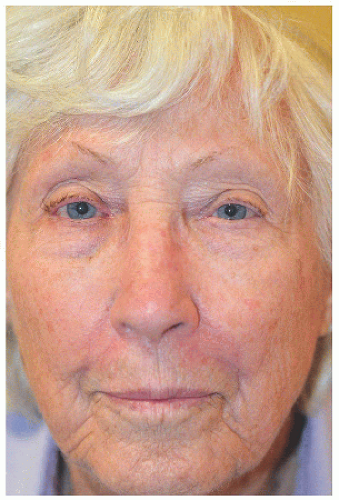
The second example is an unusual case with two basal cell carcinomas involving bilateral alar sills. The repairs demonstrate the utility of island advancement flaps in reconstruction of this important anatomical landmark, preserving the isthmus of tissue between the nose, cheek, and lip and concealing the incisions at the base and one long side of the triangular flap at the junction of anatomical units and within the melolabial furrow (Figs. 6.4F, G, H, I, J, K).
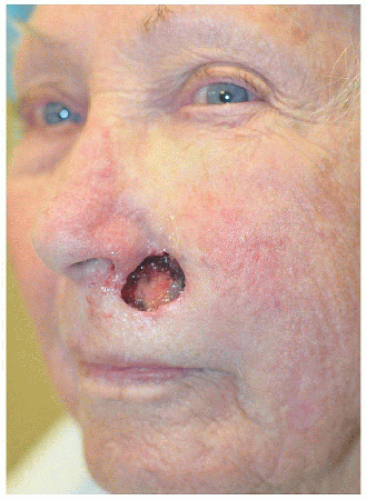 Figure 6.4F. Following a four-stage Mohs procedure for a basal cell carcinoma, the surgical defect measures 1.9 × 1.9 cm. |
Key Points
Island advancement flaps are useful for alar sill defects as one long incision line is placed within the melolabial furrow and the base incision line is hidden within the alar sill. In addition, one of the base angles of the flap may function well to replace the missing triangle- or peninsula-shaped alar sill, which separates the nose, lip, and cheek.
The long sides of the triangle should be elongated and gradually tapered to minimize secondary tension vectors and to produce a more natural transition between the cheek and lip.
The flap at the leading, trailing, and lateral edges should be carefully undermined, maintaining a healthy vascular pedicle located in the broader portion of the flap. Undermining is complete when the leading edge of the flap can be secured without significant secondary tension or pull back.
First, absorbable sutures should be used to secure the leading edge of the flap within the surgical defect, followed by closure of the secondary defects and finally securing the long edges of the triangle.
6.5 MIDUPPER LIP VERMILION AND MIDLOWER LIP VERMILION: VERMILIONECTOMY AND MUCOSAL ADVANCEMENT FLAP
This first defect measures approximately 2.2 × 1.1 cm and is located entirely within one cosmetic subunit on the upper lip: the vermilion (Fig. 6.5A). In addition, the patient has extensive sun damage, including changes of actinic cheilitis involving the upper lip. If the surrounding vermilion were healthy and not likely a source of future skin cancers, a repair utilizing the remaining vermilion tissue might be considered (e.g., Section 6.6), but instead, a vermilionectomy and mucosal advancement flap was selected. Apart from removing the precancerous changes on the upper lip, this procedure allows the repair to be completed within one cosmetic subunit and places the incision line along the border between two cosmetic subunits (i.e., vermilion and cutaneous lip) (Figs. 6.5B and C).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree