Cheek Reconstruction
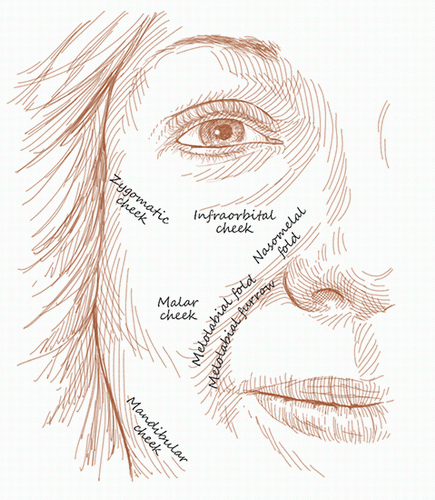 |
Compared with other cosmetic units, the cheek provides a wealth of adjacent loose tissue from which to borrow. As a result, many surgical defects may be repaired in a side-to-side fashion, and those that cannot may be repaired by a local flap. Grafts and second intention healing are not usually good options in this location. In designing a repair, closure should occur along relaxed skin tension lines (RSTL) whenever possible and free-margin deviation at other adjacent cosmetic units (e.g., eyelid, oral commissure) should be avoided at all costs.
3.1 MEDIAL CHEEK: SIDE-TO-SIDE REPAIR
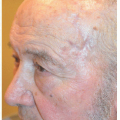
Surgical defects on the medial cheek can frequently be repaired in a side-to-side or complex linear closure (Figs. 3.1A, B, C, D, E, F, G, H, I). The key to reconstruction here is to place the incision line within RSTL or at the junction of cosmetic units or subunits (see Fig. 1.1). Another important point is that most of the cheek is not a flat surface. Some areas may be flat and adjacent areas, convex or concave. As a result, the incision line in a side-to-side repair may have to be lengthened from the usual 3:1 length-to-width ratio in order to avoid persistent redundant tissue or standing cones (Figs. 3.1D, E, F, G, H, I). In older patients, relaxed skin tension lines may be obvious, but in younger patients one may close the wound within what would be the “expected” or anticipated RSTL. And if the surgical defect is adjacent to or within the border between two cosmetic units (e.g., between the cheek and nose or cheek and lip), the wound may be easily closed along the direction of this border.
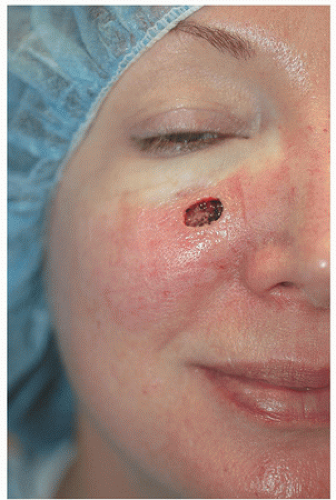
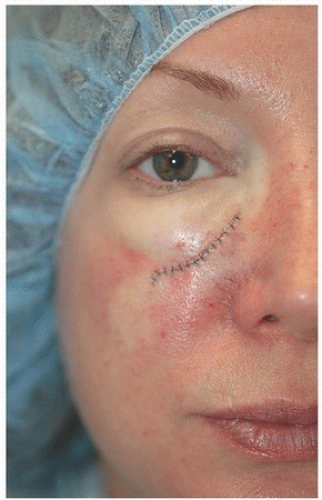
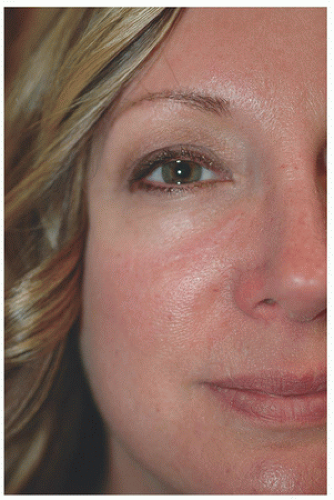
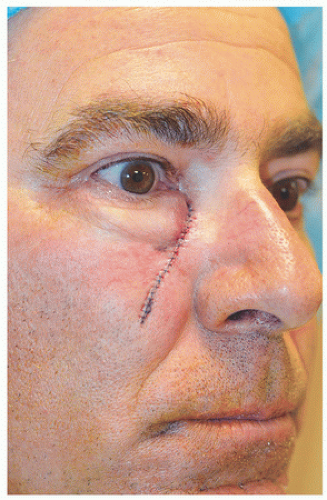
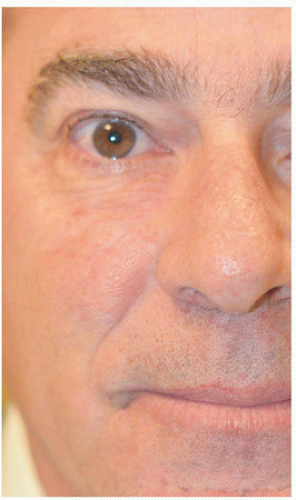
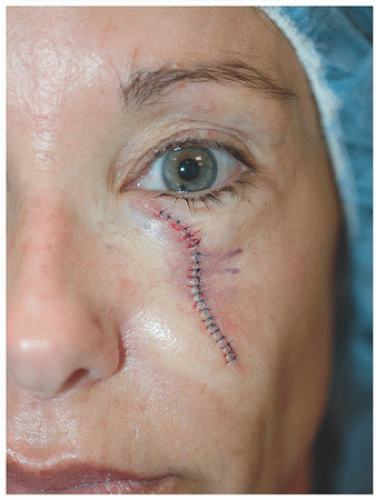
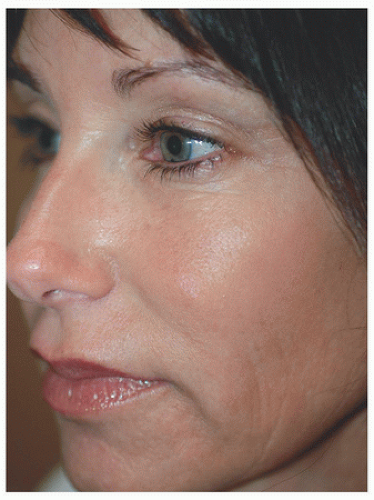
For surgical defects in other sections of the cheek, side-to-side repair may also be an excellent alternative. In the third patient, the defect is larger and located in the midinfraorbital cheek (Fig. 3.1G). There is adequate tissue laxity lateral and medial to the wound to close in a side-to-side fashion along RSTL, avoiding secondary tension vectors that might deviate the lower eyelid. The tissue redundancy or standing cone that develops superior to the orbital rim is excised as a tricone but slightly changes direction with the excision following the rhytides and RSTL of the lower eyelid. The tissue redundancy below the surgical defect is also excised within RSTL (Fig. 3.1H). As a result, the wound is closed as an S-plasty, which helps to redirect tension vectors and place incision lines in the natural curving RSTL of the cheek and lower eyelid. By following the RSTL of each particular cosmetic unit and avoiding tension on the lower eyelid, incision lines and scars remain well hidden (Fig. 3.1I).
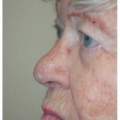
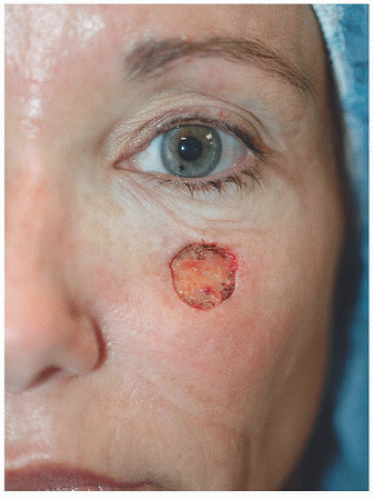 Figure 3.1G. Younger patient with a 1.9 × 1.7 cm defect on the midinfraorbital cheek following surgical excision of a lentigo maligna (melanoma in situ). |
Key Points
Small- to medium-sized defects on the cheek can frequently be closed in a side-to-side fashion along RSTL within rhytides or at the junctions of cosmetic units.
Over convex and concave surfaces, the incision line may have to be lengthened or an S-plasty incorporated to avoid redundant tissue at the poles of the incision.
In younger patients without obvious rhytides, wounds may be closed in the direction of anticipated rhytides (i.e., anticipated later in life).
3.2 MEDIAL CHEEK: ADVANCEMENT FLAP
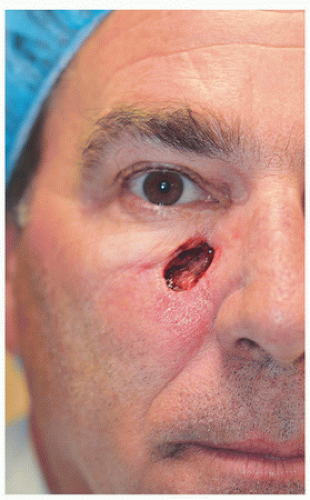
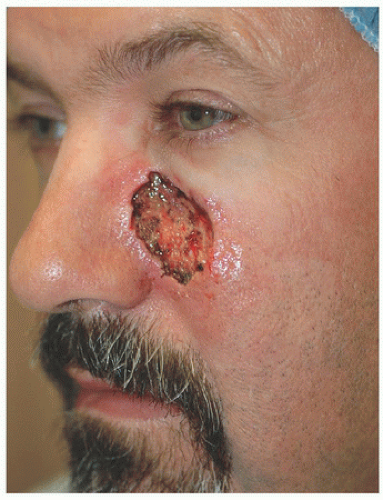
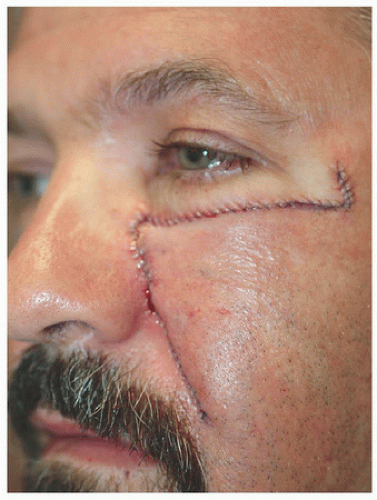
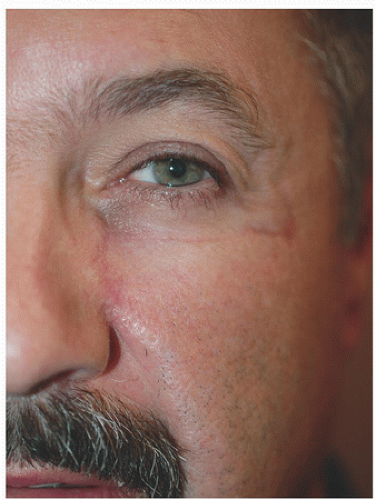
This 51-year-old man was left with a relatively large defect located on the left paranasal cheek following Mohs surgery for a basal cell carcinoma (Fig. 3.2A). The defect is located on the left paranasal cheek, essentially on the border between cheek and nose cosmetic units (i.e., nasomelal fold). Loose tissue from where to borrow is obviously lacking near the eyelid and nose; therefore, one considers borrowing tissue from either the lateral cheek (e.g., advancement flap) or the inferior cheek (e.g., rotation or island advancement flap). In this instance, there was enough tissue laterally to reconstruct with an advancement flap. The superior aspect of the defect is just at the junction of the eyelid and cheek cosmetic units, creating a good location to place the incision lines. (Remember, incisions at the junctions of cosmetic units or subunits tend to be better hidden than those crossing cosmetic units or subunits.) The incision is carried to the zygomatic cheek, where a tricone is excised to facilitate advancement of the flap, and that tricone placed such that it sits roughly in the direction of a periorbital rhytide (Fig. 3.2B). To adequately mobilize this flap, a good amount of undermining in the superficial subcutaneous plane is necessary. When the flap is advanced medially, it is important that the direction of movement and placement of sutures do not in any way distort the lower eyelid downward (note that the direction of the incision laterally climbs superiorly slightly, following the direction of the orbital rim and zygomatic arch). And finally, when the flap is advanced and sutured into place, a standing cone or dog-ear develops inferior to the surgical defect. That dog-ear is excised along the medial cheek and into melolabial furrow but does not violate the small triangular alar sill, which sits between the cheek, nose, and upper lip. The short-term result (Fig. 3.2C) demonstrates that these incisions are placed where they will be best hidden, and in a short time (with or without pulsed dye laser assistance), the pinkness to the scars will fade out.
Key Points
Advancement flaps recruit a small additional amount of loose tissue compared to side-to-side repair.
In this case, the incision line follows the junction between the cheek and lower eyelid laterally and recruits tissue from the lateral cheek.
Advancement and closure of the flap must be horizontal and must avoid secondary tension on the lower eyelid.
Upon advancement of the flap, a standing cone or dog-ear forms inferior to the defect. This is removed with an incision that follows the cosmetic unit junction between the cheek and nose and ultimately falls within the melolabial furrow.
3.3 MEDIAL CHEEK: ISLAND ADVANCEMENT FLAP
In this location, like the previous case, the loose tissue is located on the lateral cheek or inferior cheek (Fig. 3.3A). However, two other factors come into play here: (1) the long axis of the defect runs almost horizontally, and (2) the defect is immediately adjacent to the border between the cheek and the upper lip. Because the long axis runs horizontally, an advancement flap from the lateral cheek (e.g., Section 3.2) or a rotation flap from the lateral-inferior cheek will have to travel a greater distance to close the defect and avoid any potential tension being transferred to the lower eyelid. Also, an advancement or rotation flap from the lateral cheek or lateral-inferior cheek would cross the middle of the cosmetic unit and thus be more conspicuous (i.e., not at the junction of a cosmetic unit). We took advantage of the fact that the defect is immediately adjacent to the cheek-lip cosmetic border and that there is loose tissue inferior to the defect and designed an island advancement flap to advance tissue into the surgical defect (Fig. 3.3B). Formerly referred to as an island pedicle flap, this flap does not have any cutaneous attachment and therefore is a bit more mobile than a traditional advancement flap. A transposition flap (e.g., rhombic or bilobed) could have been used here, but transposition flaps tend to create more numerous and angulated incisions not easily hidden in RSTL or junctions of cosmetic units, and therefore an island advancement flap was preferred. Although not all incisions are within RSTL or at cosmetic unit junctions, one of the two long sides of the triangle is well hidden in the melolabial furrow and the other runs in the same direction, roughly the direction of the RSTL (Fig. 3.3C).
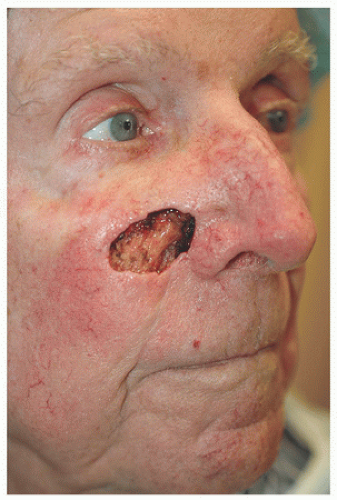 Figure 3.3A. This 77-year-old man was left with a 3.2 × 2.2 cm defect located on the right medial cheek following Mohs surgery for a basal cell carcinoma. The long axis of the defect is almost horizontal, and the defect is inferior to the orbital rim (junction between the eyelid and cheek cosmetic units), making an advancement or rotation flap from the lateral or lateral-inferior cheek more problematic.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|