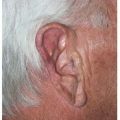
Forehead and Temple Reconstruction
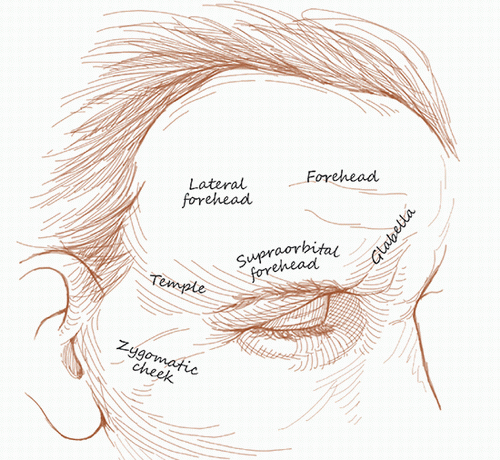 |
The forehead and temple make up a large portion of the face, but there are significant differences between these two adjacent cosmetic units. The forehead is a convex structure with relatively sebaceous, inelastic skin overlying the frontalis muscle. Relaxed skin tension lines (RSTL) tend to run in the same direction as horizontal forehead rhytides except in the central forehead and laterally at the border with the temple. On the other hand, the temple is a concave structure whose overlying skin tends to be thinner, less bound down to the underlying temporalis fascia, and therefore more mobile. The temple is also home to one of the “danger zones” in facial reconstruction: the superficial location of the temporal branch of the facial nerve. The surgeon should be particularly cautious in the use of scalpel or undermining scissors in this region as the nerve runs just deep into the subcutaneous fat from the zygomatic arch to the inferior aspect of the lateral forehead. RSTL on the temple tend to run in a radial direction similar to the direction of periorbital rhytides.
4.1 MEDIAL, LATERAL, AND SUPRAORBITAL FOREHEAD: SIDE-TO-SIDE REPAIR
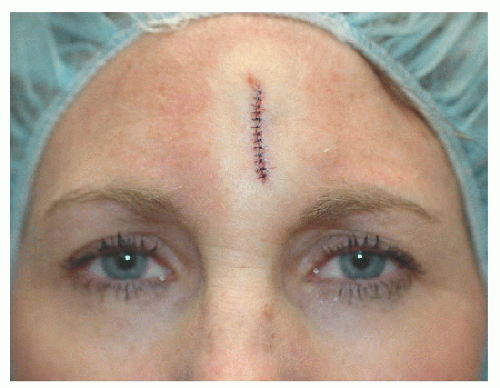
Smaller defects on the forehead can be closed in a side-to-side fashion. The long axis of the direction of closure (i.e., RSTL) varies depending on the exact location. Defects in the midforehead frequently close easiest in a vertical direction as the frontalis muscle is sparser and considerably weaker in the central forehead (Figs. 4.1A, B, C).
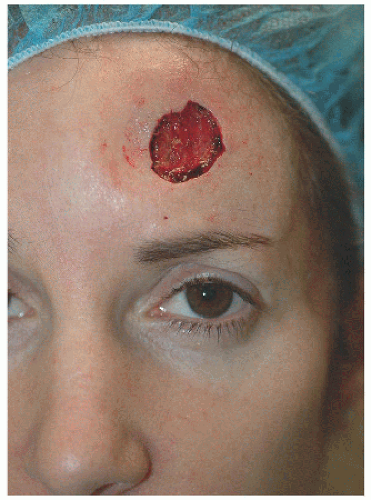
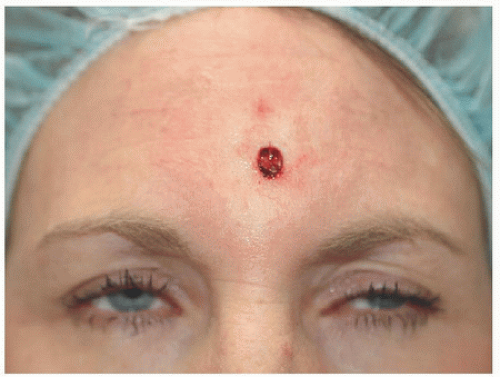 Figure 4.1A. This woman was left with a 0.9 × 0.7 cm defect located on the medial forehead following Mohs surgery for a small basal cell carcinoma. |
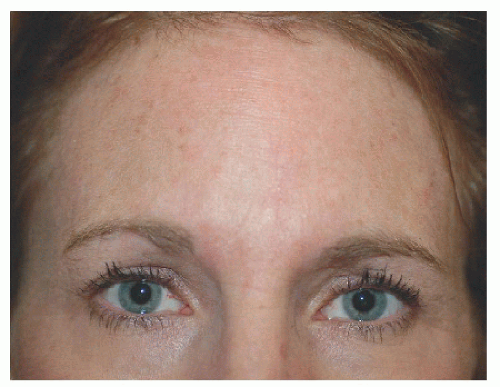
In the lateral forehead where the frontalis ends, the RSTL are somewhat mixed. For many defects, closure in the direction of the frontotemporal fusion point is preferred especially if closure in a nonvertical direction might distort a free margin like the eyebrow (Figs. 4.1D, E, F).
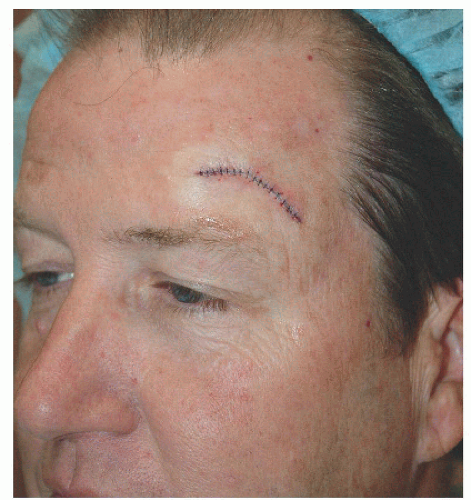
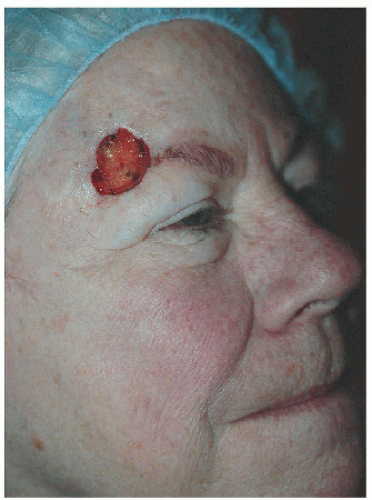 Figure 4.1D. This defect on the right lateral supraorbital forehead measures approximately 2.3 × 1.7 cm. |
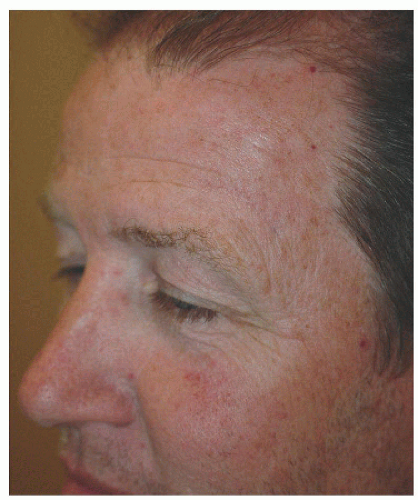
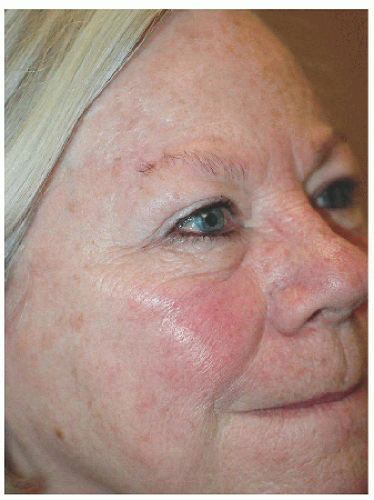 Figure 4.1F. Final healed view. Closure in this direction avoided deviation of the lateral aspect of the eyebrow. |
Defects in the central aspect of the right or left forehead where the belly of the frontalis muscle is thickest can be closed along RSTL in the same direction as the horizontal forehead rhytides (Figs. 4.1G, H, I). Defects up to about 1.0 cm wide can be closed without prolonged upward deviation of the brow, and defects farther (i.e., more superior) from the eyebrow or in older patients can particularly tolerate side-to-side closure without long-term eyebrow elevation.
Key Points
Small defects can be closed in a side-to-side fashion on the forehead with the direction of closure dependent upon location. RSTL on the central forehead are somewhat ambiguous, but usually the defect closes easiest in a vertical direction. Lateral forehead defects may close in a horizontal direction, but if near the frontotemporal fusion point, closure in a vertical direction may be preferred. Defects in the midportion of the right or left forehead may close in the direction of horizontal forehead rhytides as long as the eyebrow is not persistently elevated (usually defect size ≤ 1 cm).
4.2 FOREHEAD (EYEBROW): ADVANCEMENT FLAP
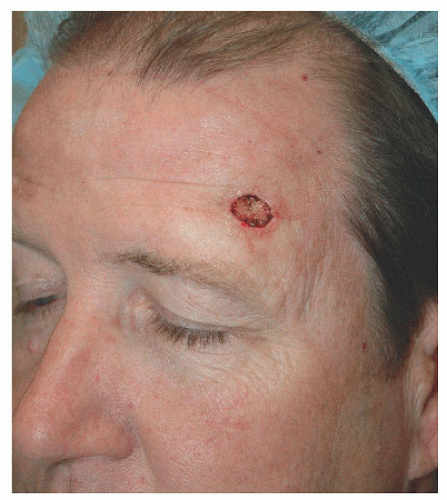
As with any surgical defect, one starts by asking, “What is missing?” (Fig. 4.2A). The answer will make it clear as to which reconstruction methods will be successful. As the hair-bearing eyebrow is missing, the only way to successfully reconstruct this defect is to replace or restore the middle of the eyebrow with hair-bearing tissue. As such, grafts or local flaps from the forehead will not provide the necessary tissue. The answer to the question, “Where are you going to find the tissue to restore the defect?” is optimally going to be the ipsilateral eyebrow, either medial or lateral to the defect. The medial eyebrow is a paired feature of the central face and therefore any movement of this structure will be immediately visible, both because of its central location and asymmetry with the contralateral eyebrow. A better option is to recruit from the lateral eyebrow, where movement is not readily noticeable. So the best answer to the question “How are you going to move this tissue to where you need it” is either advancement flap or island advancement flap. Both of these options advance the lateral eyebrow medially, filling the surgical defect and making the eyebrow contiguous. In this case, an advancement flap was selected to minimize potential for trapdoor (as may happen with island advancement flaps) and to maintain cutaneous connection (and possibly better vascular supply) for the hair-bearing flap. This second point might be somewhat controversial as island advancement flaps tend to be very mobile and have a strong vascular pedicle; however, the farther the flap travels, the greater the pedicle may need to be released and therefore the greater the risk to the vascular supply. In any event, an advancement flap was designed to reconstruct the defect (Fig. 4.2B). The inferior incision was placed just inferior to the eyebrow, extending to the lateral upper eyelid where a tricone was excised to facilitate advancement of the flap and fall in the direction of a periorbital rhytide. After undermining widely by blunt dissection and adequate spot electrodesiccation for hemostasis, the flap was advanced and sutured into place with absorbable, buried vertical mattress sutures. This created a tricone or standing cone superior to the eyebrow, which was excised in a vertical direction. The lateral shortening of the eyebrow is barely noticeable, but maintaining the contiguity of the eyebrow is what makes this repair work so well (Fig. 4.2C).
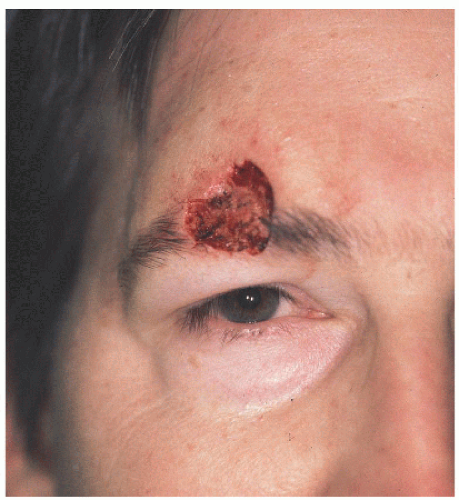 Figure 4.2A. This man was left with a moderate-sized defect after Mohs surgical excision of a basal cell carcinoma involving primarily the midportion of the eyebrow. |
Key Points
Careful evaluation of the wound and repair options help to determine the two best options for repair of this defect: advancement flap and island advancement flap, both of which will recruit hair-bearing lateral eyebrow.
Advancement of the flap medially helps to maintain symmetry and balance in the central face.
Wide undermining of the flap and excision of a tricone at the distal aspect of the incision facilitate advancement of the flap into the defect.
A standing cone or dog-ear forms when the flap is advanced into the surgical defect, and this is excised as a tricone on the forehead.
4.3 LATERAL FOREHEAD: ADVANCEMENT FLAP
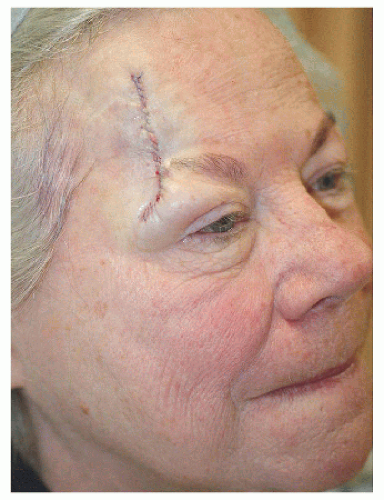
Most of the adjacent lax tissue in this location is lateral to the surgical defect (Fig. 4.3A). In addition, by recruiting tissue laterally one minimizes the chance of distortion or lifting of the eyebrow, an oft-forgotten free margin. An advancement flap does not recruit a significant amount of tissue, but there is adequate tissue laterally to close a defect this size with proper mobilization (Fig. 4.3B). One word of advice here is to place the horizontal incision line within or immediately adjacent to a horizontal forehead rhytide. By doing this, a large portion of the surgical scar is optimally hidden on the forehead (Fig. 4.3C). The distal portion of this incision (where the tricone is excised) is at the junction of the forehead and temple. This serves two purposes: improves mobility of the flap (as undermining is carried to the temple) and hides the scar better at the junction of the two cosmetic units. After the flap is advanced and sutured into place, a tricone or dog-ear forms superior to the defect. This is easily excised in a vertical direction.
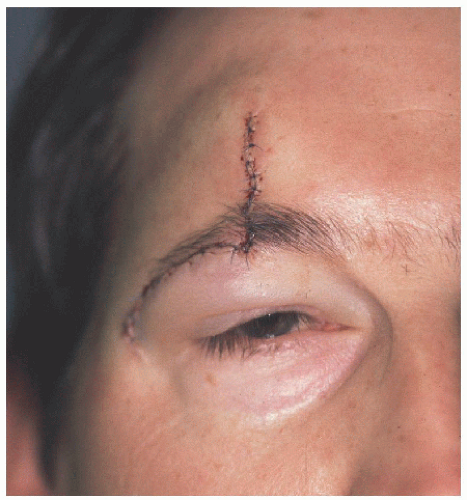
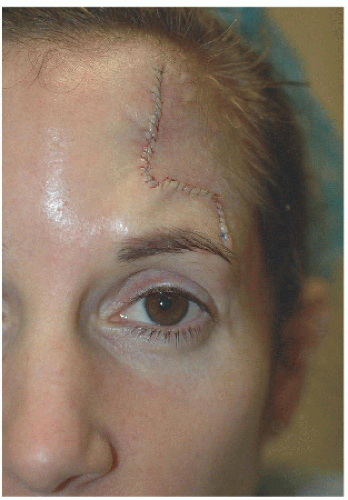 Figure 4.3B. An advancement flap mobilizes lax tissue from the lateral forehead, avoids deviation of the eyebrow, and hides most incision lines. |
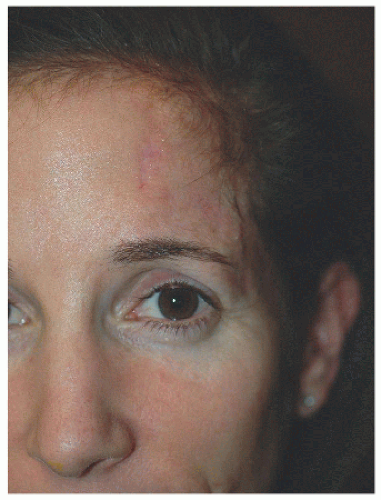 Figure 4.3C. Short-term healed result shows mild pinkness still remaining along incision line but otherwise well healed. |
Key Points
Defects too large for side-to-side repair may close more easily with an advancement flap repair. This is because advancement flaps may recruit a small amount of additional lax tissue in comparison to side-to-side closure.
Advance the flap medially and avoid tension on the eyebrow.
The flap incision follows the horizontal forehead rhytide laterally, where a dog-ear is excised at the junction of the forehead and temple.
4.4 LATERAL FOREHEAD (EYEBROW): FULL-THICKNESS SKIN GRAFT
The lateral aspect of the eyebrow is lost in this young woman status-post skin cancer surgery (Fig. 4.4A). As pointed out in Section 4.2, one should avoid moving the medial eyebrow laterally. While moving the mid or lateral brow medially may be acceptable in reconstruction of the medial brow, moving the medial brow laterally will not provide an aesthetic result. The difference between moving the brow medially or laterally is that the former changes the central face, altering a paired central landmark and making the central face asymmetric. The best option here for this particular patient (who wanted to avoid additional scars from creation of a local flap) was a full-thickness skin graft (Fig. 4.4B). A rhombic transposition flap from the temple would have easily recruited adequate tissue to fill the defect but would have created additional incision lines and scars and could have potentially disturbed the position of the eyebrow. The patient was very happy with the result and chose to use eyebrow pencil to finesse the final result (Fig. 4.4C).
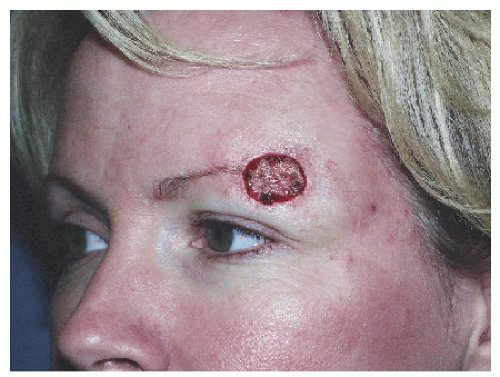 Figure 4.4A. Surgical defect of the lateral eyebrow. Patient wished to avoid any procedure that might make additional scars or potentially change the position of the eyebrow. |
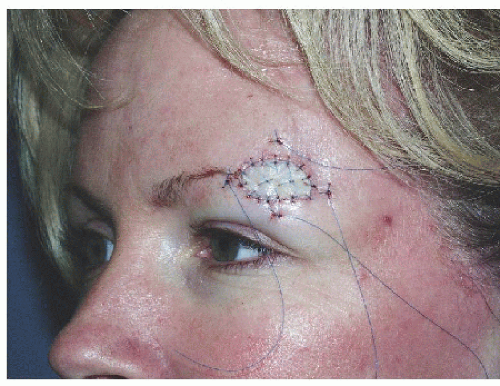 Figure 4.4B. Repair with a full-thickness skin graft (donor site preauricular cheek, placing incision line in pretragal crease). Graft is sutured into place with 6-0 polypropylene sutures, although 5-0, fast-absorbing gut suture would have worked well. Two tacking sutures at the center of the graft were used to approximate the graft to the wound bed, and four sutures outside of the graft to hold a tie-down dressing in place.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|