19 Lid Reanimation with the Palpebral Spring
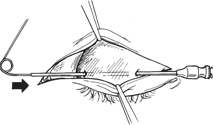
The inability to close the eye (lagophthalmos) or to blink leads to serious corneal complications, including chronic ocular discomfort, corneal ulceration, and loss of vision. In addition, the intensive regimen of frequent drops and ointment during the day or taping the eye at intervals or at night that may be required for the medical management of lagophthalmos can add to the disability. It is common to see patients who have recovered well from trauma, brain tumor, or other causes of facial paralysis, only to be limited by eye problems in their ability to resume a normal lifestyle. The treatment of severe lagophthalmos, then, becomes important, not only in preventing visual loss but also in rehabilitating the patient.
TARSORRHAPHY
The classic surgical answer to lagophthalmos has been tarsorrhaphy, just as the classic surgical answer to cataract was aphakia. Unfortunately, tarsorrhaphy, like aphakia, replaces the original problems with other problems.
Except for patients who had minimal lateral tarsorrhaphies, virtually all were unhappy with the results. Those who had extensive tarsorrhaphies had essentially lost the use of the affected eye. Those with lesser tarsorrhaphies complained of loss of visual field.
The tarsorrhaphy added significantly to the disfigurement and to the difficulty adjusting psychologically to the effects of facial paralysis. In those patients who recovered enough lower facial function so that the lower face looked relatively normal, at least in repose, the tarsorrhaphy continued to be disfiguring. Furthermore, despite the high functional, cosmetic, and psychologic cost of tarsorrhaphy, patients still had chronic discomfort from exposure keratitis.
METHODS OF LID REANIMATION
Because of the limitations of tarsorrhaphy, various procedures have been introduced to reanimate the paralyzed lids. The most physiologic solution is reinnervation of the lids. Unfortunately, even when reinnervation procedures, such as facial-hypoglossal anastomosis, are successful in reanimating the lower face, they may fail to supply enough innervation to the upper lid to restore closure and blinking. Temporalis muscle transplantation into the upper lid also has a low success rate. Closure may be accomplished by conscious “biting down” by the patient, but this has little to do with physiologic blinking and closure. Implanted magnets may hold the lid shut at night but do not contribute to lid closure during the day.
The most successful reanimation procedures have been those that attempt to create a force in the lids to act against the levator muscle (LM). For example, a small flat gold or platinum weight may be implanted above or on the tarsal plate. With the patient upright, the weight of the lid acts against the levator to close the eye. The effectiveness of this procedure is limited by the patient’s position (since the weight may not act to close the eye with the patient supine) and also by the size of the piece of gold that can be placed in the lid without disfigurement. Gold weights are most successful when lagophthalmos is not severe or when the need for complete lid closure is not critical. Patients with corneal anesthesia (neurotrophic corneas) secondary to fifth nerve involvement require complete lid closure both upright and supine. They do much better with springs than with weights.
The Silastic (polymeric silicone) elastic prosthesis devised by Arion uses a 1-mm Silastic band as the opposing force against the levator. The band is sewn through the medial canthal tendon. A special introducer is then passed between orbicularis and tarsus in the upper lid. The end of the band is attached to the introducer and brought through the lid laterally, where it is fixated to the periosteum. The other end is similarly passed through the lower lid and anchored. In general, this implant works quite well. Its long-term success, however, is limited by the loss of elasticity in the Silastic, or a loss of tension in the band as it migrates slightly medially through the tendon. The procedure may have a role in patients who are expected to recover normal facial function in 6 months. Unfortunately, in most instances of facial paralysis, it is difficult to predict the exact timing of functional return.
The device that is most successful in providing long-term lid reanimation is the palpebral spring implant. The original concept for this spring was described by Morel-Fatio and Lalardrie. The technique has been modified over the years by Levine.
The spring can provide reliable long-term complete closure of the lid, regardless of patient position. It also provides a simulated blink. Because closing tension is present even in the open position, frequently, there is some degree of pseudoptosis. Nevertheless, the lid can be opened enough to clear the visual axis, and the cosmetic result is generally acceptable. Extrusion and breakage of the spring (e.g., from vigorous rubbing of the eye or from metal fatigue) are uncommon events. Slippage of the spring toward the lid margin can occur, but this is an infrequent problem. If slippage does occur, repositioning the end of the spring is a relatively simple maneuver.
INDICATIONS FOR SPRING IMPLANTATION
The palpebral spring is indicated in any patient with lagophthalmos resulting from facial paralysis that is expected to persist for more than 6 months and in whom the eye problems cannot be readily managed by the use of drops and ointment. It may also be used as a permanent solution to a closure problem that is not expected to improve.
When recovery of facial function occurs and it is clear that the spring is no longer needed, it can be removed. If partial function returns, the spring can be retained and readjusted. If the patient fails to recover upper lid function, the spring can be left permanently.
Patients with severe paralysis who are expected to recover function in <6 months, but in whom conservative management is impractical, may also benefit from spring implantation. Consider, for example, a patient who could be managed for several months by taping the eye shut. If the affected eye were his only functional eye, long-term lid closure would not be a viable possibility, and a spring implant could be considered.
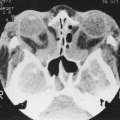
A decision for placement of a palpebral spring should be made cautiously in a patient who is known to need frequent magnetic resonance imaging (MRI) scans of the orbit, since the wire can cause artifact that can blur the image in that area. The currently used spring wire (alloy 35NLT from Ft. Wayne Metals, www.fwmetals.com) is nonferrous and poses no risk of spring migration with the MRI.
TECHNIQUE OF PALPEBRAL SPRING IMPLANTATION
Building the spring
The spring is prepared in advance of surgery, not only because it saves operative time but also because the configuration of the spring can be more carefully matched to the patient’s anatomy in the absence of infiltration anesthesia and lid swelling. In designing the spring, the posterior aspect of the loop is the superior end. Suitable nonferrous 35NLT wire (Ft. Wayne Metals, diameter 0.009–0.012 in.) is selected, depending on the force required to oppose the levator. Thicker wire may be used to balance the force of a strong levator, and lighter wire may be used if the levator is weak. In most patients, 0.011 in. wire is used. Diameters <0.010 in. should not be used if the levator is to be tightened. The curves of the spring must match the curvature of the lid. Place the spring on the closed lid and make appropriate bends in the wire.
The spring tension preoperatively is set somewhat tighter than will be required, as it is easier to loosen the spring intraoperatively than to tighten it. The spring must also be designed to track well with the upper lid as it moves from the open to the shut position.
Preparing the patient
The patient is prepared and draped in the usual manner for lid surgery. The eye is protected with a scleral shell. Lidocaine 2% with epinephrine mixed with an equal amount of 0.5% Marcaine is infiltrated along the lateral two thirds of the upper lid fold. An additional amount of anesthetic is infiltrated along the tarsus at the center of the upper lid. Infiltration is also given along the lateral orbital rim. The amount of infiltration should be limited, to avoid distortion of lid anatomy or levator function. Basal sedation, given preoperatively, should be limited to short-acting agents that will not interfere with the patient’s state of consciousness during the procedure, since cooperation is needed to open and close the eyes and to sit up on the operating table.
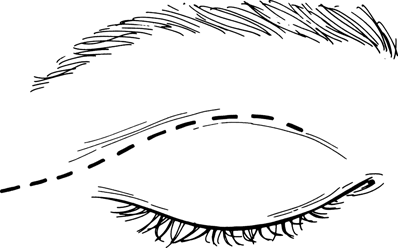
Figure 19-1. With a protective scleral shell in place, an incision is made along the lateral two thirds of the lid crease and carried across the orbital rim laterally. Dissection is carried downward at the medial end of the incision to expose the tarsal plate. Dissection is also carried upward and laterally to expose the orbital rim.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree