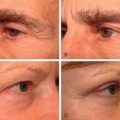
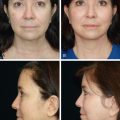
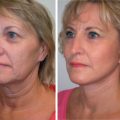
Abstract
There are several advantages of lateral SMASectomy in comparison with traditional elevation. First, because the procedure does not require traditional SMAS flap elevation, there is less concern about tearing of the superficial fascia. Second, the potential for facial nerve injury is lower because most of the deep dissection is over the parotid gland. If the SMASectomy is performed anterior to the parotid, the deep fascia will similarly provide protection for the facial nerve branches as long as the resection of the superficial fascia is done precisely and the deep fascia is not violated. Third, because SMAS flaps have not been elevated, they tend to hold suture fixation more strongly, and the potential for postoperative dehiscence and relapse of contour is decreased.
Keywords
Lateral SMASectomy facelift, Defatting, Open submental incision, Medial platysma approximation, Lateral SMASectomy
History
The senior author’s first experience with rhytidectomy was during residency in the late 1970s. At that time, the emphasis was on extensive defatting of the neck with complete platysma muscle transection, plicating medial borders and pulling laterally. However, several years of patient complaints, complications, and overoperated necks led to a modification of this technique. With the advent of liposuction in the 1980s, the author found that he could obtain excellent neck contouring in many patients utilizing liposuction combined with strong lateral platysmal suturing.
When superficial musculoaponeurotic system (SMAS) dissection first became popularized in 1976, it became fashionable to include a dissection of the lateral SMAS directly overlying the parotid gland. The senior author initially utilized this form of SMAS dissection beginning in the late 1970s and continued using it into the mid-1980s, but overall was disappointed with the effects of a simple elevation and tightening of the lateral superficial fascia. Specifically, he saw little difference in overall facial contour whether he had performed a lateral SMAS dissection or had omitted it.
As he gained greater experience with SMAS dissection, it became obvious that for the superficial fascia to produce any effective contour change in face lifting, it was necessary to elevate the SMAS anterior to the parotid gland. The problem of more extensive SMAS dissection is that facial nerve branches are in greater jeopardy. He also noted that the superficial fascia tends to thin out as it is dissected more anteriorly, making the SMAS easy to tear. A SMAS dissection that is not raised as a continuous fascial sheet but rather is raised with several tears in it is a poor substrate for holding the tension of contouring the face. For these reasons, he felt that an extensive SMAS dissection was not warranted in most patients as it offered little long-term benefit when compared with SMAS plication.
In 1992 Dr. Baker realized that an alternative to formal elevation of the superficial fascia was a “lateral SMASectomy,” removing a strip of the SMAS in the region directly overlying the anterior edge of the parotid gland, and extending to the lateral canthus. Excision of the superficial fascia in this region secures the mobile anterior SMAS to the fixed portion of the superficial fascia overlying the parotid. The direction in which the SMASectomy is performed is oriented so that the vectors of elevation following SMAS closure lie perpendicular to the nasolabial fold, thereby producing improvement not only of the nasolabial fold but also of the jowl and jawline. In 2001 this technique was further developed and refined into the minimal incision rhytidectomy (short scar facelift).
Senior Author’s Personal Philosophy
For many years I have listened to panels and presentations and have read articles about the “super-SMAS,” “deep plane,” “subperiosteal,” and various other extended rhytidectomy procedures. In their search for the penultimate facelift, these pioneering surgeons demonstrate superb anatomic studies, beautiful illustrations, and impeccable photographs. Their presentations are well organized, stimulating, and seductive.
I have always considered myself a bold and aggressive surgeon, and the temptation to utilize these new, deeper dissections is extremely appealing. However, I am reluctant to employ them, and I keep asking myself why? The explanation is partly that I am not convinced that the results are superior to those obtained by the standard SMAS-platysma techniques. More important, I do not yet believe that the implied “benefits” outweigh the increased morbidity and risks, especially to the facial nerve.
The presentations on deep dissection and subperiosteal rhytidectomies recall the period between 1976 and 1980, when virtually all panels and courses were advocating complete platysma muscle transactions and a multitude of platysma flaps. As a plastic surgeon just completing residency, I was highly impressed; I became a believer and a convert: the only way to get the “best result” in rhytidectomy was with these techniques. However, many years of patient complaints, complications, and overoperated necks occurred before most of these techniques were abandoned. I can only speculate on whether the deep plane rhytidectomy techniques will have a similar evolution.
In the 21st century, the consumer’s preference has been for minimally invasive and noninvasive techniques: fillers, Botox, endoscopy, and limited incision aesthetic surgery. The rationale for any minimal incision surgery is evident: less invasiveness, less bleeding, presumably less pain, faster healing, and less scarring. The primary advantages of minimal incision rhytidectomy, however, are that it preserves the posterior hairline and avoids retroauricular scars, which are particularly important for a woman with a pulled-up or swept-back hairstyle. It is a ponytail-friendly facelift. The primary goal of any surgeon performing rhytidectomy should be to utilize a technique giving consistently good results with minimal risk, complications, morbidity, and a speedy postoperative recovery.
My intention is neither to discredit these deep dissection techniques nor to deplete the splendor of creative surgery. Their contribution is already evident: an increased and clearer knowledge of facial anatomy, muscle function, and human expression. I am certain that some aspect of these techniques will be incorporated by many plastic surgeons. The questions that remain to be answered are: (1) what are the indications for these newer techniques? (2) How great are the risks and complications? And, most important, (3) do the benefits significantly outweigh the risks to justify using these techniques routinely?
There are several advantages of lateral SMASectomy in comparison with traditional SMAS elevation. First, because the procedure does not require traditional SMAS flap elevation, there is less concern about tearing of the superficial fascia. Second, the potential for facial nerve injury is lower because most of the deep dissection is over the parotid gland. If the SMASectomy is performed anterior to the parotid, the deep fascia will similarly provide protection for the facial nerve branches as long as the resection of the superficial fascia is done precisely and the deep fascia is not violated. Third, because SMAS flaps have not been elevated, they tend to hold suture fixation more strongly, and the potential for postoperative dehiscence and relapse of contour is decreased.
There are certainly other rhytidectomy techniques that produce excellent results. Each surgeon must adopt a technique that serves his or her patients best. Ideally, the technique should be safe, consistent, easily reproducible, and applicable to a variety of anatomic problems. The surgeon also must have the versatility to adapt and modify his or her technique to the needs and desires of each patient. At present, the lateral SMASectomy provides this for most of my patients. In the future, as endoscopy and fixation techniques advance, I will seek to modify and further improve my present rhytidectomy operation.
It must be emphasized that I do not perform SMASectomy in every rhytidectomy. Patients with thin faces and minimal subcutaneous fat undergo simple plication or imbrication.
Surgical Technique
Anesthesia
Virtually all of our facelifts are performed with the patient under monitored intravenous propofol sedation. Patients are given oral clonidine, 0.1 to 0.2 mg, 30 minutes before surgery to control their blood pressure. The face and neck are infiltrated with local anesthesia, 0.5% lidocaine with 1 : 200,000 epinephrine, through use of a 22-gauge spinal needle. The face is injected before we scrub to provide the requisite 10 minutes for vasoconstriction.
Incisions
When the temporal hairline shift is assessed as minimal, the preferred incision is well within the temporal hair. With this incision, it is often necessary to excise a triangle of skin below the temporal sideburn at the level of the superior root of the helix. Keep in mind, this incision will move the natural hairline. This may be acceptable if the shift is minimal or if the hairline is low.
However, when larger skin shift is anticipated (frequently the lift is more vertical with minimal incision rhytidectomy) or the distance between the lateral canthus and temporal hairline is greater than 5 cm, we prefer an incision a few millimeters within the temporal hairline ( Figs. 18.1–18.3 ). Although this is a compromise, the alternative of a receding temporal hairline is never acceptable to a female patient. When the incisions are properly executed, these scars heal well and are easy to revise or camouflage. The only exception might be in a patient with deeply pigmented skin in whom the scar will contrast and appear as a white line. The temporal hairline incision should be made parallel to the hair follicle and no higher than the frontotemporal hairline.

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree