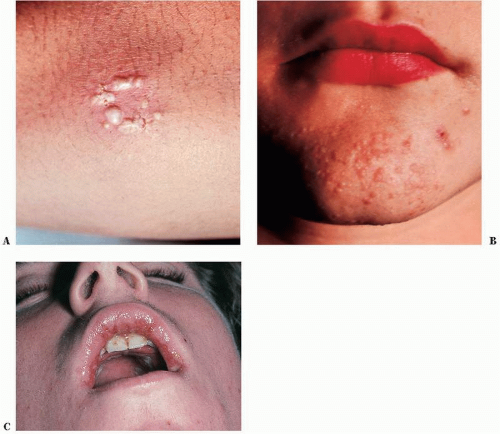
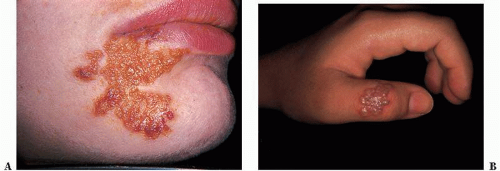
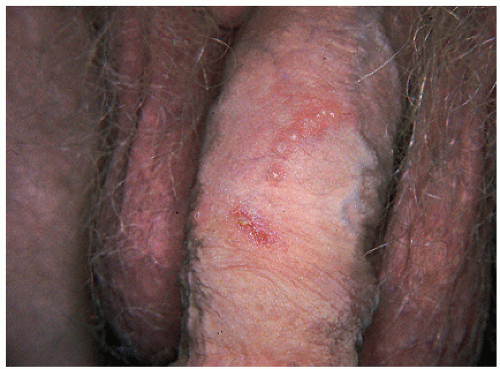
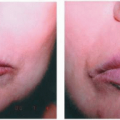
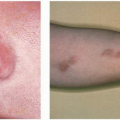
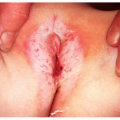
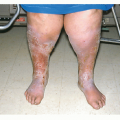
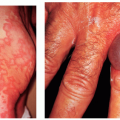
Herpes simplex virus 2 (HSV-2) is one of the most widespread sexually transmitted diseases (STDs) in the world. It causes 70% of primary genital herpes and over 95% of recurrent genital herpes (
Fig. 23-3). In the United States, the prevalence of genital herpes is 40 to 60 million, and the incidence is 500,000 to 1,000,000 cases per year, with approximately 22% of the general population being seropositive for HSV-2. Similar to HSV-1, HSV-2 causes primary, latent, and recurrent infections, and is transmitted during both asymptomatic and symptomatic phases, typically through sexual contact. Genital herpes infections caused by HSV-2 tend to be more severe than those caused by HSV-1, are more likely to have recurrent episodes, and have a greater frequency of subclinical viral shedding. HSV-2 can also cause neonatal herpes, with the highest risk occurring when the mother has primary genital herpes during delivery. In addition to cutaneous lesions, the infected neonate may develop multiorgan involvement, which carries a high mortality rate.
Presentation and Characteristics
Up to 90% of patients infected with HSV-2 become infected via asymptomatic viral shedding. Genital herpes infection is typically asymptomatic, because the lesions may be painless and inapparent. The first clinically recognized lesions of genital herpes may be either true primary or a first-episode, nonprimary. True primary genital herpes usually develops after 2 to 14 days of HSV exposure. There may be widespread vesicles and ulcers on the genitalia with inguinal adenopathy, and the patient may complain of discharge, dysuria, fever, lethargy, myalgias, and photophobia. The most common site of involvement in women is the cervix, although the classic painful clinical presentation is mostly that of vaginal and vulvar lesions.
More than half of patients with the first recognized signs and symptoms of genital herpes have a nonprimary first episode, which occurs when the initial infection is asymptomatic. This may occur weeks, months, or even years after initial HSV infection. A strong immune response may prevent the infection from becoming clinically recognizable. The initial immune response does attenuate the severity of first-episode nonprimary genital herpes. Lesions are often less extensive, and systemic symptoms are less common and severe compared to that of true primary genital herpes.