Abstract:
These anatomic studies strongly support repositioning of ptotic midfacial tissues as a primary modality for midface rejuvenation and revolumization. This can be accomplished with the deep plane procedure and its modifications described within this chapter.
Keywords
Adjunctive Submental Procedures, Platysmaplasty, Deep Plane Rhytidectomy, Deep Plane Dissection, Zygomatic-Cutaneous Ligament, Zygomaticus Major Muscle Fibrous Attachments, Masseteric Cutaneous Ligaments, Lateral Platysma Suspension
Introduction
The gradual transformation of the aging face culminates in predictable changes in the surface topography and anatomical relationships of facial subunits. The morphogenesis affects individuals on a variable time course, as each person has a unique underlying bone structure and genetic predisposition. The progression of facial aging is therefore best evaluated on an individual basis, irrespective of chronological age. There are innumerable findings associated with facial aging; however, the consequences of volume depletion and gravitational tissue descent are the most germane to the rhytidectomy surgeon. Understanding and addressing these processes with a comprehensive treatment plan is essential to restore a natural rejuvenated appearance with long-lasting results.
Anatomy and Aging Pathophysiology With Surgical Implications
Midfacial Aging
A volumized face is the hallmark of youth. The “baby face” of infancy is characterized by full round cheeks and is essentially devoid of any recognizable underlying skeletal structure. During development into adulthood, the face progressively reveals a relative increasing prominence of bony structures and decreasing of the once omnipotent soft tissue structures. One noticeable change during maturation is a decrease in the volume of the inferior midface (centered around the nasal ala) that characterizes the “chubby cheeks” of childhood. This leads the way to the heart-shaped face of young adulthood . Most noticeable at this stage is volumization and fullness over the zygoma body tapering to a relative concavity in the perioral region, often referred to as an Ogee Curve.
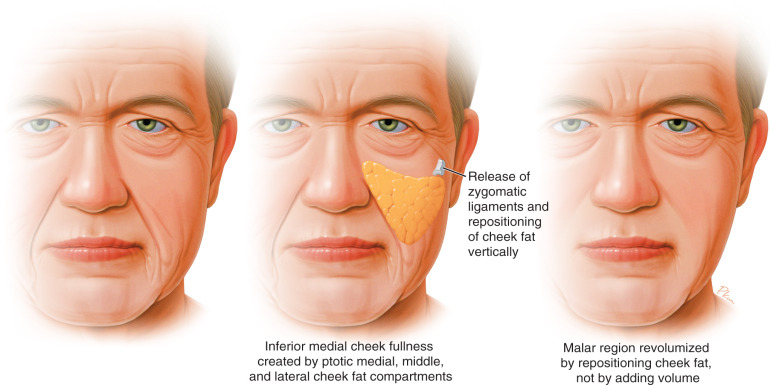
With aging, the prominence over the malar region flattens, and diminishing volume is most appreciable in the upper and lateral midface. Midface volume deflation decreases the malar prominence, hollows the subzygomatic areas, and deepens the lower eyelid cheek junction. Concomitant with these deflationary changes is an increase in the volume of the inferior midface in the perialar region, and a widening of the midfacial tissues just lateral to the nasolabial folds is noticed ( Fig. 17.1 ). The heart shape face of youth therefore becomes inverted, taking on the shape of a square or an inverted triangle. Cadaveric studies have shown that the face is comprised of many discrete fat compartments . With age, increased tissue in the inferior midface has been demonstrated in magnetic resonance imaging (MRI) studies comparing faces in their thirties with those in their sixties. These MRI studies of the medial cheek fat compartment have suggested that both inferior redistribution of fat and potential fat hypertrophy are plausible reasons for widening of the inferior midface and deepening of the nasolabial folds in older patients .

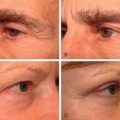
Photographic and surface anatomy studies have supported ptosis of the overhanging cheek mass as the primary causative agent in widening of the lower midface with aging . The stigmata of midfacial aging were compared between photographs of a patient in an upright versus supine position, and provide a compelling visual demonstration of the role that gravity plays in periorbital and midfacial aging. This study demonstrated improvement in characteristic manifestations of midfacial aging, including tear trough, cheek volume, and nasolabial folds, when comparing the upright photograph with the supine photograph of the same patient . Gravitational pull results in descent of the facial soft tissue, thereby creating a relative volume increase in the inferior aspect of the soft tissue compartment. This further supports the role of ptosis in the morphogenesis of midface aging.
In addition to soft tissue changes, degenerative changes occur in the midfacial skeleton. Shaw et al. demonstrated resorption of the zygomatico-maxillary complex when comparing computed tomography scans of those in their thirties with others in their fifties and sixties . There was a statistically significant derotation or inward rotation on lateral projection of the maxilla of six degrees that was statistically significant. Quantitatively, this small bony change between these age groups accounts for a minority of the midfacial volume change.
These anatomic studies strongly support repositioning of ptotic midfacial tissues as a primary modality for midface rejuvenation and revolumization. This can be accomplished with the deep plane procedure and its modifications described later. Patients with more significant facial atrophy or thin faces may require volume supplementation with fat grafting or injectable fillers, as there is insufficient volume reservoir to reposition. One exception is the lower eyelid cheek junction, where progressive volume loss exposes the bony architecture of the inferior orbital rim. This requires volumization in all cases, either with a fat transposition lower blepharoplasty, autologous fat grafting, or injectable fillers. Treatment of the lid-cheek junction is beyond the scope of this chapter.
The malar region is not one confluent soft tissue mass, but is a conglomeration of individual fat compartments separated by fascial septa. Rohrich and Pessa have defined the cheek fat into malar and nasolabial fat compartments. The malar fat pad has a medial, middle, and lateral anatomic division. These fat pads are tethered in place by the zygomatic cutaneous ligament, a strong dense fascial attachment from the periosteum to the soft tissues of the midface .
Biomechanical studies have shown that the zygomaticocutaneous ligament is the strongest of all of the facial ligaments, elongating by a mere 9 mm . Mobilization and elevation of the malar fat pad therefore requires division of this ligament. The nasolabial fat compartment, which exists just lateral to the nasolabial fold, is the most medial of the fat compartments, and is also tethered by fascial attachments to the zygomaticus major muscle.
These attachments are released along the plane superficial to the zygomaticus major and minor until reaching the nasolabial fold medially overlying the maxilla. This has been defined as the premaxillary space, and a dense maxillary ligament that tethers the midface is bluntly dissected to further release the midface .
The deep plane rhytidectomy rejuvenates the deflated upper midface by releasing the ligamentous attachments noted previously, and repositioning the ptotic fullness of the inferior and medial midface to its former position on the malar prominence. In this model, the malar region is revolumized by vertically repositioning the midfacial fat compartments while simultaneously decreasing the presence of the excessive inferior midfacial tissue ( Fig. 17.2 ). In traditional superficial musculoaponeurotic system (SMAS) flap and SMAS plication procedures very limited or no dissection is performed in the midface, and the zygomaticocutaneous ligament remains uninterrupted. Gassner et al. have shown in histologic studies that the SMAS does not exist in the midface medial to the lateral aspect of the zygomaticus musculature. For this reason, SMAS flap and superficial plication rhytidectomy techniques are plagued by failure in the midface because traction on the SMAS does not mobilize the midface soft tissue structures .
In deep plane rhytidectomy, the vector of suspension of the composite flap should be vertical oblique to maximize revolumization of the midface. The individual’s anatomy will dictate the exact angle. On average, this angle approaches 60 degrees in most patients. When examining the vectors of redraping in over 300 patients, this angle varies from the upper 40s to 70 degrees. Still, the angle is always more vertical than an exact superolateral vector of 45 degrees . Volumetric analysis with a 23-month follow-up has shown that patients gain 3.2 cc of volume in each hemi midface following vertical vector deep plane rhytidectomy as a result of adequate repositioning of the ptotic cheek fat compartments . There is no statistical difference between the cheek volume gain from vertical vector deep plane rhytidectomy and that achieved 16 months after 10 cc of autologous fat transfer per cheek for midfacial rejuvenation .
Jawline and Neck
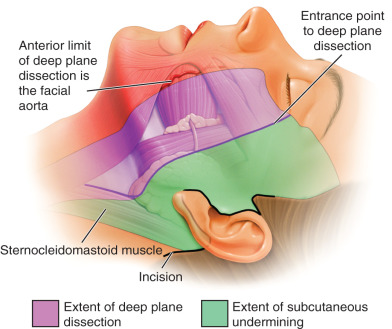
Just below the subcutaneous fat layer of the face exists the SMAS, a dense fibrofatty layer originally described by Mitz and Peyronie . The SMAS is contiguous with the platysma in the neck, and the junction between the two exists high in the cheek, not along the margin of the mandible. The platysma has been shown in surgical dissection of over 70 patients during deep plane rhytidectomy to exist 4 cm above the angle of the jaw along a line drawn between the lateral canthus and the mandibular angle, thereby occupying 57% of the face . The SMAS and platysma in the face are held to the deeper facial structures with masseteric cutaneous ligaments that extend from the masseter muscle, through the SMAS/platysma, to the skin. With aging, gravitational weakening of these ligaments allows the SMAS to slide over the masseter and the SMAS becomes redundant, and jowls form. To completely release these ligaments, dissection must continue in the sub-SMAS plane to the anterior border of the masseter .
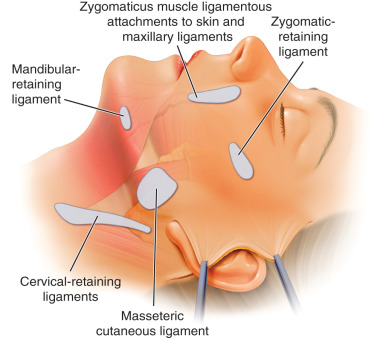
In the neck, vertical descent of the platysma that was once positioned in the face creates redundant platysma in the neck. This, along with degeneration of the platysma, creates vertical cording or banding that is often described as a “turkey gobbler deformity.” Similar to the retaining ligaments in the midface, retaining ligaments also exist in the neck, tethering the platysma to the deep investing fascia . These cervical-retaining ligaments restrict the ability to mobilize and redrape the platysma, limiting rejuvenation of the neck. The retaining ligaments of the neck are reproducibly found along the posterior border of the platysma at its junction with the sternocleidomastoid (SCM) muscle, along the anterior inferior portion of the parotid gland, and along the posterior body of the mandible . Extending subplatysmal dissection below the angle of the mandible with a lateral platysmal dissection to release the cervical retaining ligaments allows for improved rejuvenation of the neck
In patients with more significant neck skin redundancy, the mandibular ligaments may tether the skin at the mandibular border, preventing anterior submental skin tightening and necessitating release. The tethering effect of the mandibular ligaments is variable and depends upon their elasticity and position. In some patients, the mandibular ligaments have greater flexibility or elasticity and their tethering effect is less significant. They have the greatest distensibility of all the facial-retaining ligaments in biomechanical studies . Additionally, the further posterior the ligament is displaced from the symphysis, the greater tethering effect it has in the neck. We have noted this point to be on average 5 cm lateral to the symphysis in our examination of 108 patients, which would restrict skin redraping of the neck 5 cm posterior to the pogonion .
The Deep Plane Rhytidectomy
The deep plane rhytidectomy was first described by Hamra . Unlike SMAS rhytidectomy, it does not delaminate the skin from the SMAS in a biplanar fashion. Deep plane surgery elevates the facial tissues in a sub-SMAS plane, creating a composite flap of skin, subcutaneous fat, and SMAS in the lower face, above the margin of the mandible but below the cheek. Because the SMAS is tenuous in the midface, the flap in the upper cheek is developed by lysing the zygomatic cutaneous ligaments and elevating the facelift flap off the surface of the zygomaticus musculature. This creates a flap that is a composite of skin and the malar fat pad. The upper and lower composite flaps are then connected. Hamra’s deep plane facelift does not elevate the platysma below the angle of the mandible into the neck. Neck rejuvenation is accomplished with a midline platysmal plication through a submental incision, along with a plication of the lateral platysma to the SCM muscle and mastoid fascia, creating a corset in the neck.
Modifications of the Deep Plane Rhytidectomy
What follows is a description of the surgical technique for our modification of the deep plane rhytidectomy. The deep plane is entered after the skin is elevated in the subcutaneous plane to a line drawn from the angle of the mandible to the lateral canthus ( Fig. 17.3 ). While we lyse the zygomatic-cutaneous ligaments similar to Hamra, we have incorporated more extensive release of the facial-retaining ligaments to allow for greater face and neck redraping ( Fig. 17.4 ). These include the ligamentous attachments of the medial aspects of the zygomaticus major, the anterior extensions of the masseteric cutaneous ligaments, and the mandibular cutaneous ligaments. In addition, we have extended the deep plane dissection below the angle of the mandible inferiorly. The platysma is elevated from its fascial attachments to the SCM muscle and inferior body of the mandible 5 cm inferiorly into the neck. This releases the cervical-retaining ligaments that limit platysma motion during surgery, allowing for greater platysma redraping. This approach can limit the need to open the neck during rhytidectomy in a majority of cases. There are specific indications for opening the neck, and treating the platysma and subplatysmal contents. Another modification we discuss is the method and vectors of suspension we employ once the deep plane and tendinous structures are released.
Surgical Technique
Preoperative Marking
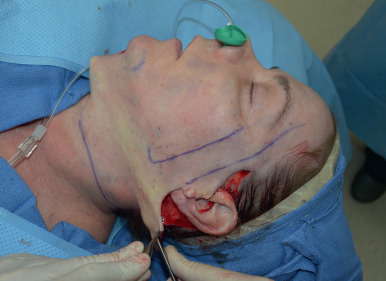
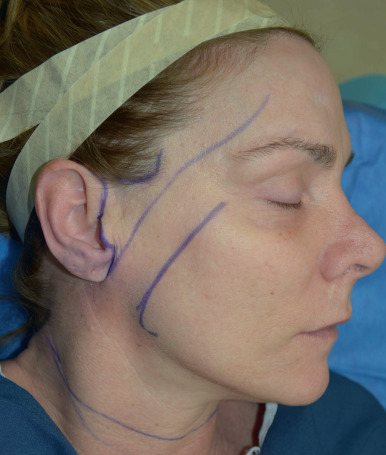
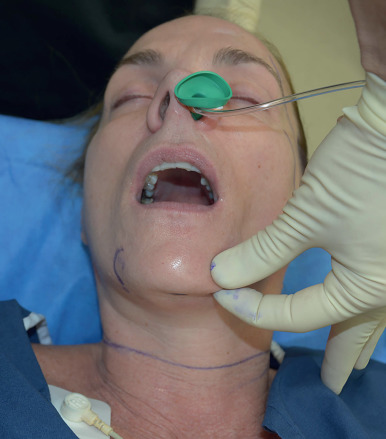
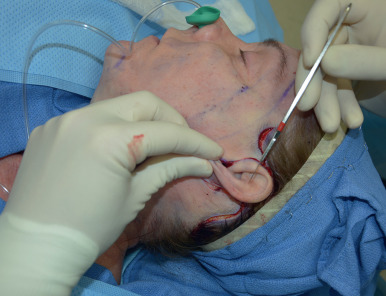
The patient is positioned upright preoperatively and important landmarks are drawn with a marking pen ( Fig. 17.5 ). The path of the temporal branch of the facial nerve is marked beginning at the root of the ear lobule, traversing at a point halfway between the lateral canthus and tragus, and ending approximately 1.5 cm from the lateral brow. Next the deep plane entry point is marked as a line extending from the angle of the mandible to the lateral canthus. A horizontal line is drawn across the neck at the level of the cricoid to mark the minimal inferior extent of neck skin elevation. The perimandibular skin is mobilized to identify where the mandibular ligament tethers the perijowl and submental neck skin, and this is marked ( Fig. 17.6 ). A submental incision is marked in the submental crease. Incision lines are then drawn beginning in the anterior temporal hairline, typically at the height of the lateral brow. This incision follows around the temporal tuft and into the hairless recess between the sideburn and helical root, turning downward into the preauricular crease, paralleling the curve of the helical margin and approximately at the width of the crus of the helix. This incision is similar to that described by other authors with several minor modifications . In the majority of patients, the incision proceeds in a retrotragal manner, just along the posterior margin of the tragus. We council male patients about the potential for transposition of bearded skin into the ear canal with a retrotragal incision and discuss a preauricular incision as an option. Ultimately, we allow them to decide on the approach, and we note that approximately 75% of men choose the retrotragal approach for improved incision camouflage. The incision then continues in a counter clockwise manner down the lobule-facial crease and around the lobule onto the posterior conchal cartilage skin to the level of the triangular fossa. In patients with greater neck skin laxity, the incision transitions down and follows the anterior edge of the occipital hairline several centimeters depending on the anticipated amount of cervical skin resection.
Anesthesia
The senior author (AAJ) performs rhytidectomy under local anesthesia, conscious sedation, or general anesthesia solely based on patient preference. Roughly 20% of these patients elect to receive only local anesthesia, typically for financial reasons or fear of general anesthesia, while the remaining patients choose to receive local anesthesia with intravenous sedation with propopfol. A mixture of five parts 0.5% lidocaine with 1 : 200,000 units of epinephrine, five parts 0.25% bupivacaine with 1 : 200,000 epinephrine, and one part 0.9% bicarbonate is used. This mixture provides a rapid-onset, long-duration, adequate hemostasis, and greater comfort given the inclusion of buffer. Tissue resistance is noted during injection as it provides a preview of how easily the tissue planes will dissect and the extent of ligamentous attachments throughout the cervicofacial region.
Incision and Skin Flap Elevation
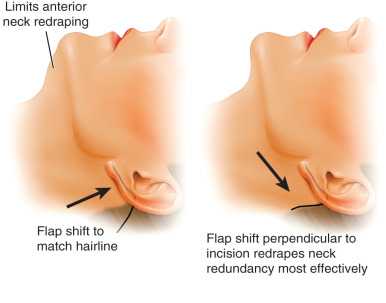
Skin incision is initiated at the anterior temporal hairline at the level of the lateral brow with a No. 10 scalpel cutting perpendicular to the skin. This can be extended superiorly during the operation if needed to redrape and remove the vertically elevated skin. In the past we implemented a beveled trichophytic incision but noted depression of the incision in a significant percentage of cases. We believe this occurs because the skin of the anterior temporal region is thin and the skived edge of the beveled incision tends to become devitalized and heal in a contracted fashion. This is different from the thicker anterior forehead/scalp skin in the area of the frontal hairline where trichophytic incisions were first described. We have noted temporal scars that are barely perceptible with this modification ( Fig. 17.7 ). The incision is then carried down the preauricular path described earlier. The incision should not be placed at the anterior edge of the helical crus cartilage because it can make the root of the helix appear unnaturally wide. It should be placed at the natural highlight that reflects the apparent width of the helical crus. It should then traverse along the posterior edge of the tragus, but not on its inner surface as this can create an unnatural folding of the cheek skin that blunts the tragus and can be a tell-tale sign of a facelift incision. A small step in the incision is placed at the inferior tragus to preserve the natural depression at the intertragic incisure ( Fig. 17.8 ). Around the earlobe, the incision should continue 2 mm inferior to the lobule cheek junction to preserve the natural sulcus between the lobe and the cheek ( Fig. 17.9 ). Posteriorly, the incision should continue a few millimeters onto the posterior conchal cartilage rather than directly in the postauricular crease. This helps minimize later inferior descent of the posterior auricular scar into a more visible location with age. In patients with less neck laxity the incision ends here. If the surgeon is uncertain of the amount of neck skin that will need excision, the incision can always be extended to remove redundancy. In cases of more significant neck skin excess, the incision is transitioned at the level of the triangular fossa down the anterior aspect of the occipital hairline posteroinferiorly ( Fig. 17.10 ). Here we utilize a beveled trichophytic incision because the scalp skin is thicker here and the attendant problems discussed before have not been noted. In the past, we utilized a high transverse incision that was hidden into the occipital hair. This incision requires that the neck skin flap be shifted anteriorly and vertically in order to prevent hairline margin step offs, which limits the amount of redundant neck skin that can be removed ( Fig. 17.11 ).
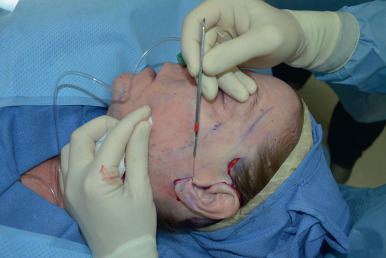
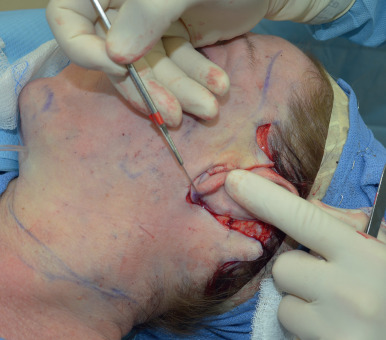
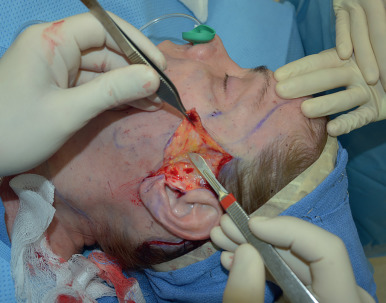
The length of the incision in the occipital region depends on the amount of cervical skin to be excised in the posterior flap. We prefer to be conservative with the initial length of this incision to limit scarring, as it can always be extended to remove a dog-ear deformity.
The initial portion of the subcutaneous flap is then elevated using Brown-Adson forceps and a No. 10 scalpel beginning with the superior preauricular point. The plane should be elevated just deep to the reticular dermis, leaving a very thin layer of fat attached to the flap. The temporal region skin is elevated with a broad, parallel stroke of the blade for 2 cm ( Fig. 17.12 ). After elevating the 2-cm skin pocket, the flap will be able to accommodate an Anderson multiple-prong retractor. This is used to place superior and lateral tension on the flap. Direct counter-tension is placed by an assistant manually retracting the skin in the opposite direction and the flap is back lit with an operating room light to visualize the subdermal plexus ( Fig. 17.13 ). Flap elevation continues with facelift scissors, tips pointed upward, making small, forward snipping motions to create an even-thickness flap. The intensity of the transilluminated light gives the surgeon the ability to gauge the thickness of the flap and create a uniform depth. Elevation in the cheek ends at the marked line of the deep plane entry point ( Fig. 17.14 ).
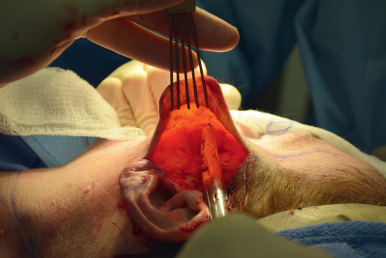
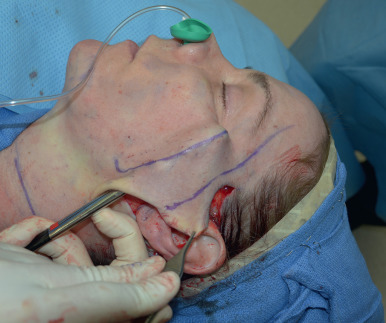
The postauricular skin is then grasped at its postauricular peak with Brown-Adson forceps and sharp dissection with a No. 10 blade is carried inferiorly. The skin in this region has a paucity of subcutaneous fat and tightly adheres to the fascia overlying the SCM muscle and mastoid so blade dissection is more expedient. This continues inferiorly to the level of the angle of the mandible and connects to the anteriorly created cheek subcutaneous flap. At this point inferior and medial dissection in the neck in a subcutaneous/supraplatysmal plane is accomplished with a lighted retractor to provide tension while vertical blunt spreading with facelift scissors. Dissecting inferiorly over the SCM in this manner will preserve the great auricular nerve, which courses from the posterior border of the SCM anterosuperiorly to the region of the lobule. Dissecting on top of the supraplatysma fascia during the medial neck skin elevation preserves a blanket of fat on the skin flap that prevents irregularities and adhesions between the deep dermis of the skin and the platysma postoperatively. This dissection is continued to the midline using a longer lighted retractor and long facelift scissors, and extending inferiorly just below the level of the cricoid ( Fig. 17.15 ). This pocket will be connected to the opposite side when it is elevated.