Case 1
Clinical Presentation
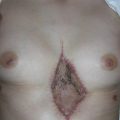
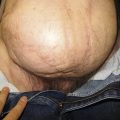
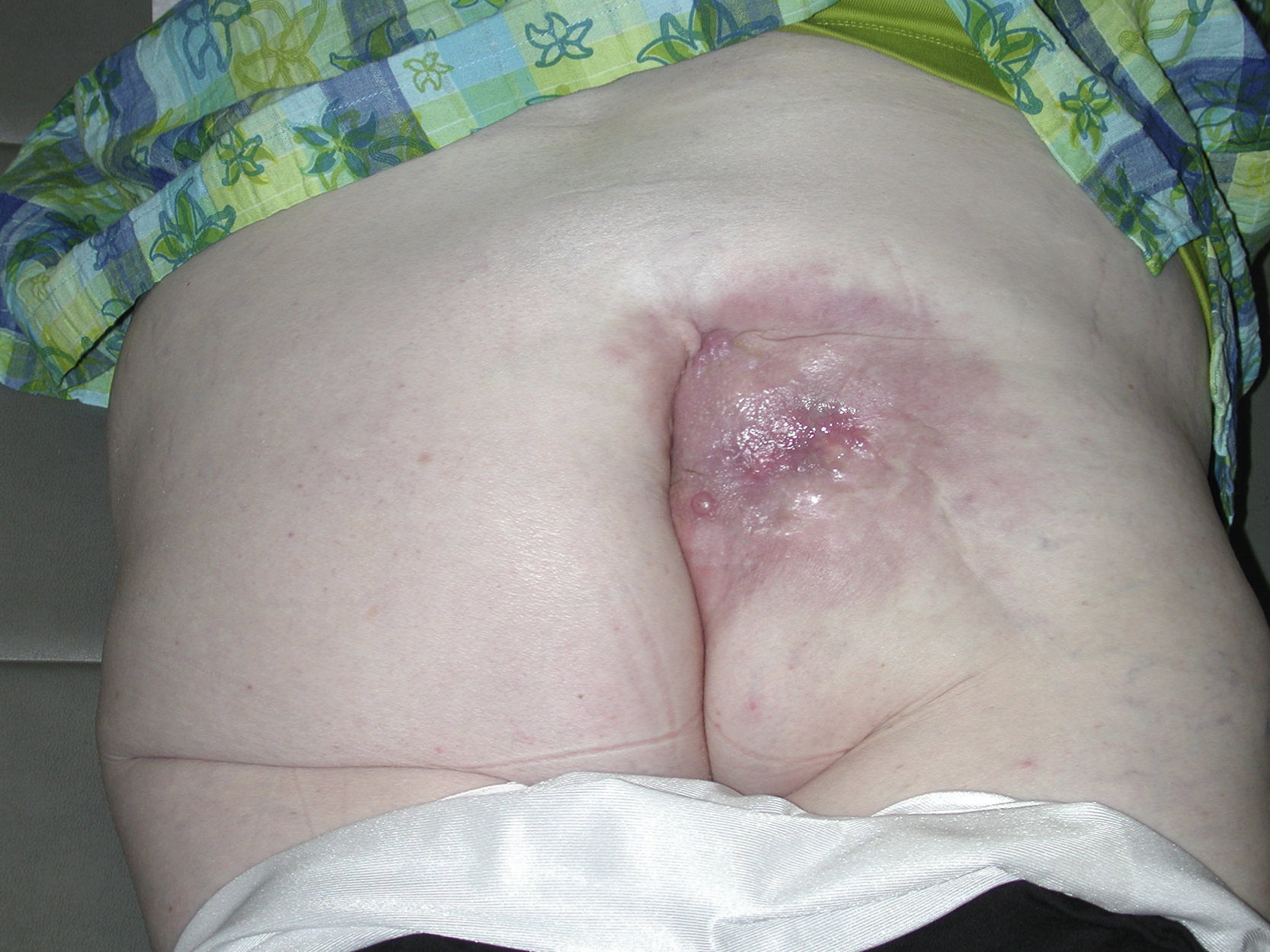
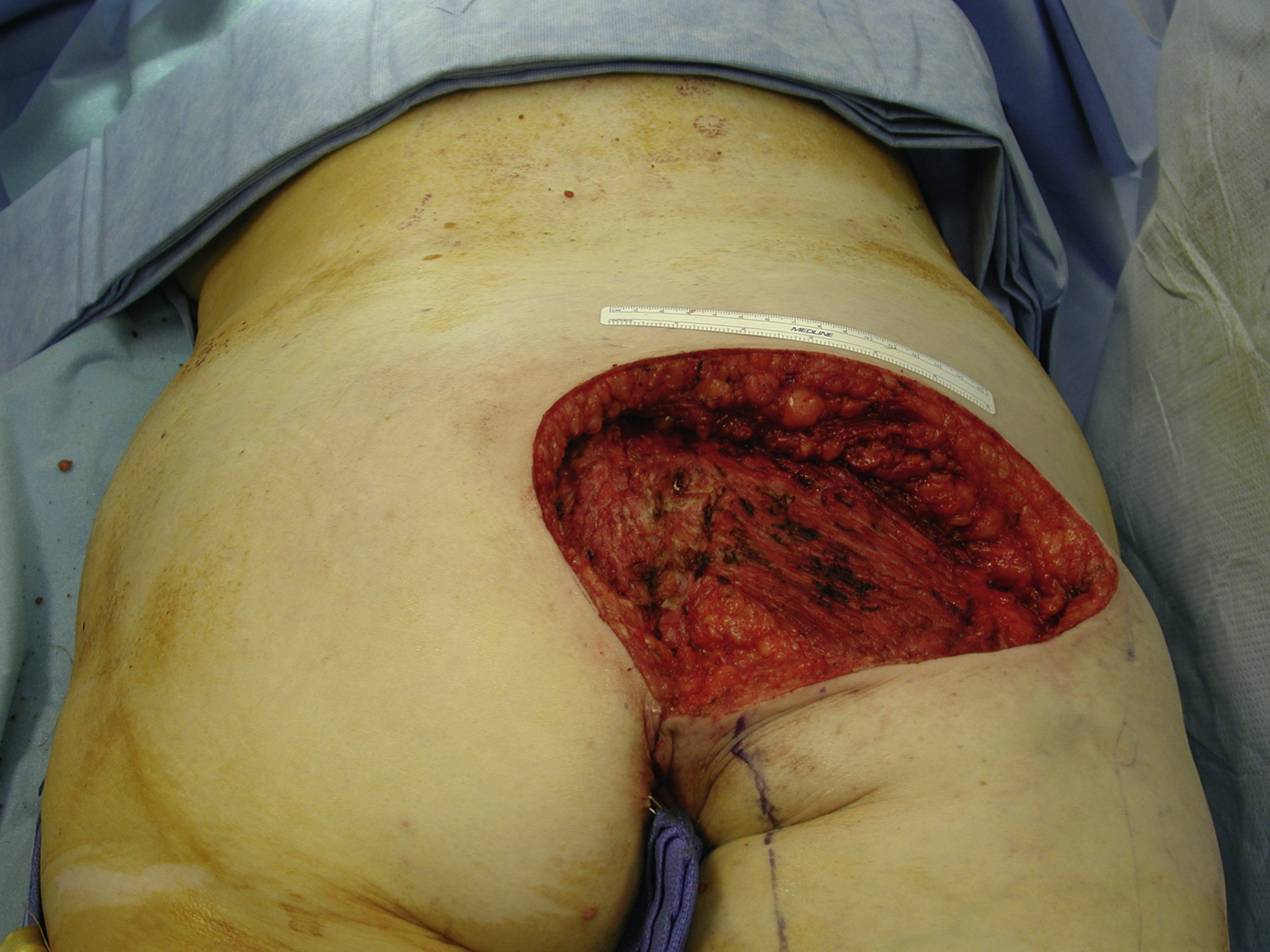
A 63-year-old White female had chronic recurrent drainage from her right buttock for the past 2 years. She had a resection of malignant fibrohistiocytoma and postoperative irradiation in the region approximately 20 years ago. She was evaluated by the surgical oncology service and multiple biopsy specimens from the region were negative for recurrent sarcoma ( Fig. 34.1 ). Wide local resection was performed by the surgical oncologist and all irradiated tissues and a chronic drainage tract were excised. A 20 × 15 cm gluteal soft tissue defect with an exposed small area of the sacrum was left after resection. The gluteus maximus muscle appeared to be fibrotic ( Fig. 34.2 ).
Operative Plan and Special Considerations
For a large gluteal soft tissue defect, reconstruction with local flaps is usually possible because there are some redundant tissues in the adjacent areas. Double-opposing V-Y fasciocutaneous advancement flaps could be designed based on the size of the defect with mobilization of the excess adjacent gluteal tissue in both superior and inferior directions. Each fasciocutaneous flap would be designed as a V-to-Y advancement flap and both flaps could be approximated in an opposing fashion for the final wound closure. A single large fasciocutaneous rotation flap may also be an option, but it would create more surgical incision and dissection for the same wound closure. In terms of blood supply to these flaps, it is possible that the superior flap receives its blood supply from the superior gluteal artery perforators and the inferior flap receives its blood supply from the inferior gluteal artery perforators.
Operative Procedures
Under general anesthesia with the patient in the prone position, the gluteal soft tissue defect was assessed for size and dimensions. Each V-Y fasciocutaneous flap was designed superiorly or inferiorly to the defect and opposing to each other. The length of each flap measured 1.5 or 2 times the longitudinal diameter of the defect. The maximal width of the flap was equal to the width of the defect ( Fig. 34.3 ).
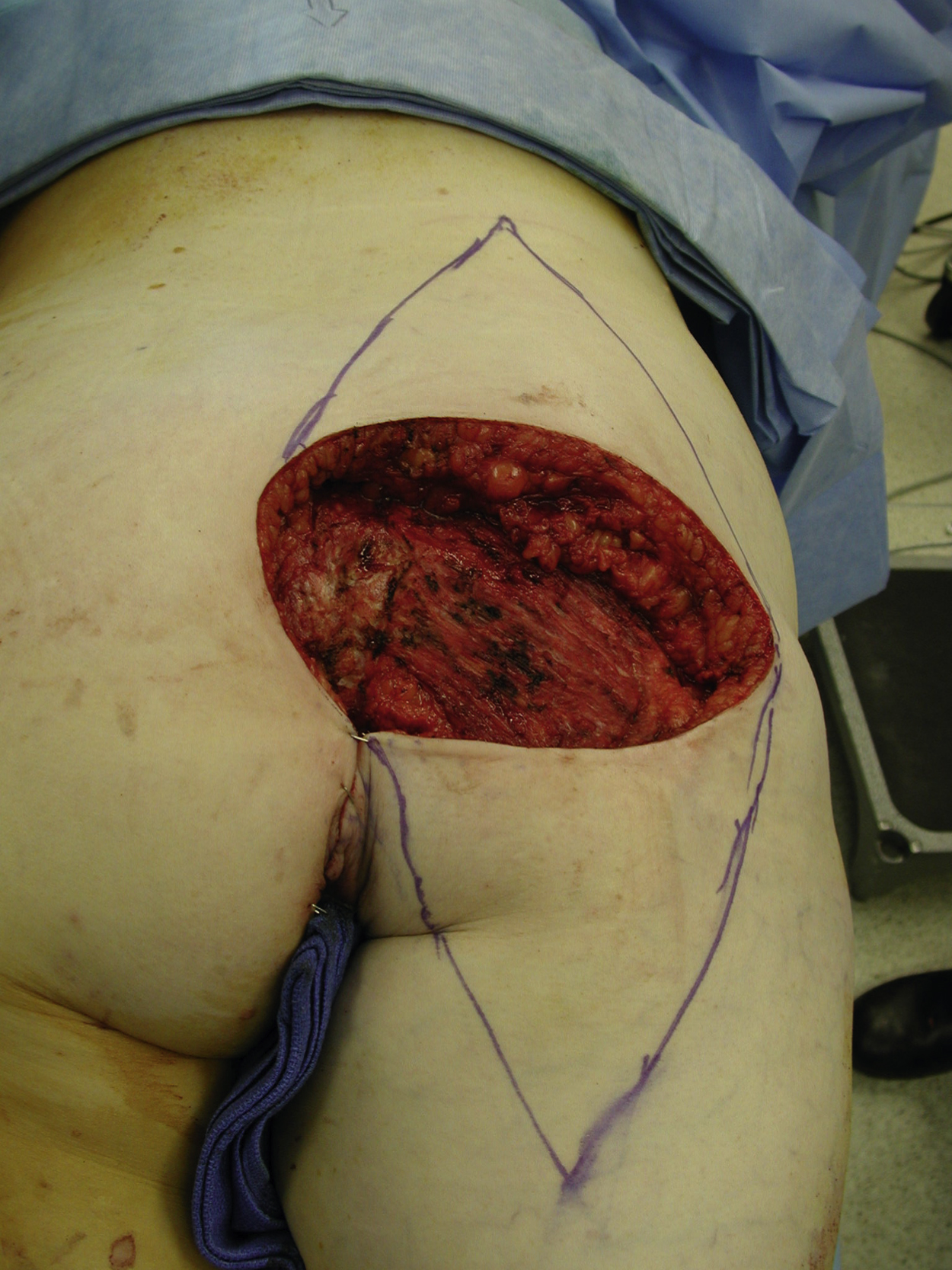
The incision was made on the arms of the V and the subcutaneous tissue was incised and beveled away from the flap, possibly catching more direct cutaneous blood supply to the flap, down to the deep fascia. The deep fascial layer was incised in a V fashion according to the flap design to aid advancement of the flap. Both flaps were approximated to each other temporarily and additional flap dissections were performed if necessary. Any fibrous connections that might restrict the advancement of the flap were divided between the flap and the adjacent tissues.
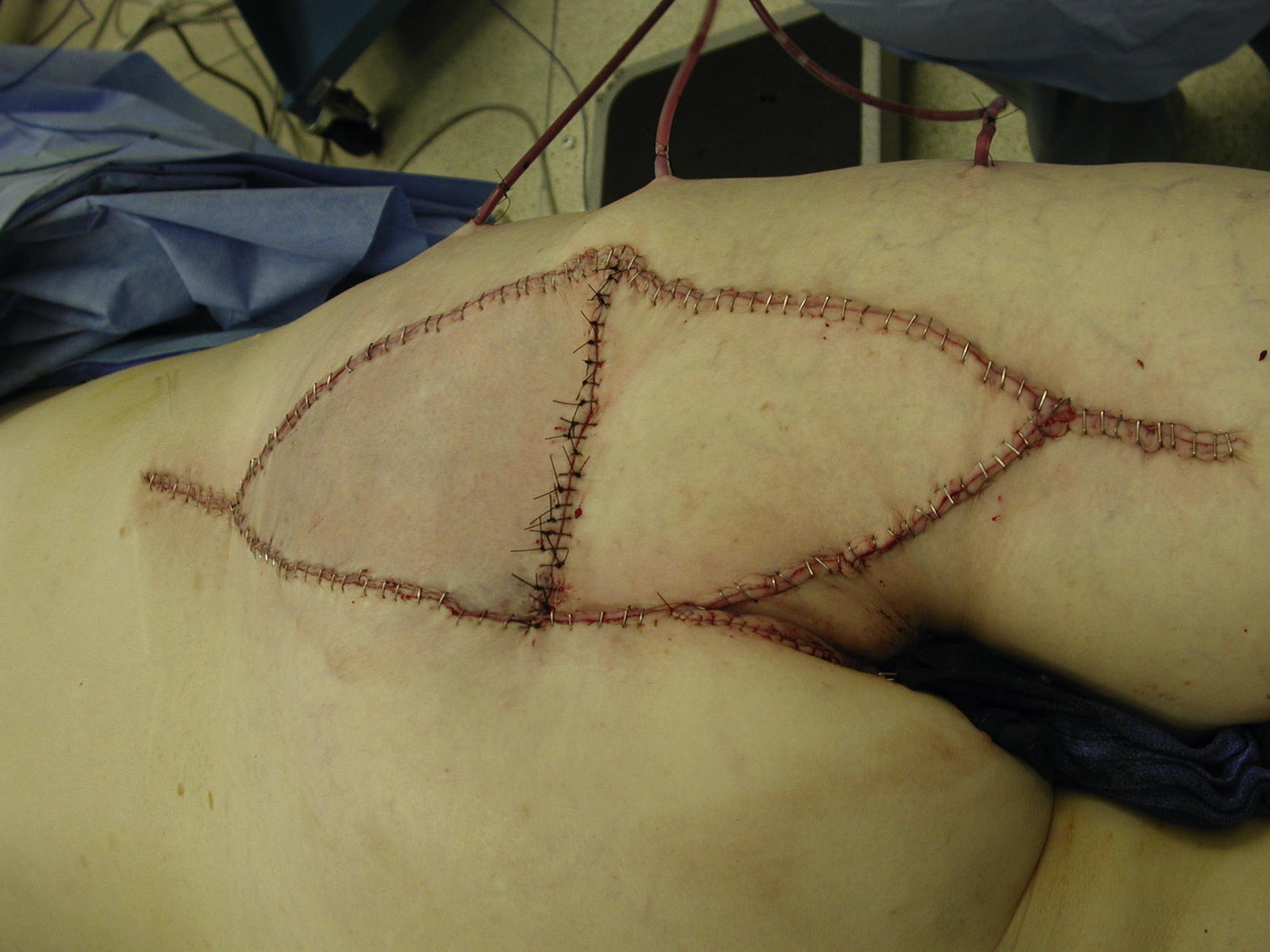
Once sufficient advancement of the flap had been accomplished, the flap donor site was closed over a suction drain in two layers (deep dermis with interrupted 3-0 Monocryl sutures and skin with skin staples) primarily in V-Y fashion. The approximation of two opposing V-Y fasciocutaneous advancement flaps was performed in three layers over one suction drain. The deep subcutaneous was approximated with interrupted 2-0 PDS sutures and the deep dermal closure was done with interrupted 3-0 Monocryl sutures. The skin was closed with interrupted 3-0 nylon sutures ( Fig. 34.4 ). Postoperatively, the patient was placed in the lateral decubital position with the operated side of the buttock up for the first several days. Patients would be allowed slow ambulation afterward but should avoid sitting or flexing their hips for approximately 6 weeks.
Follow-Up Results
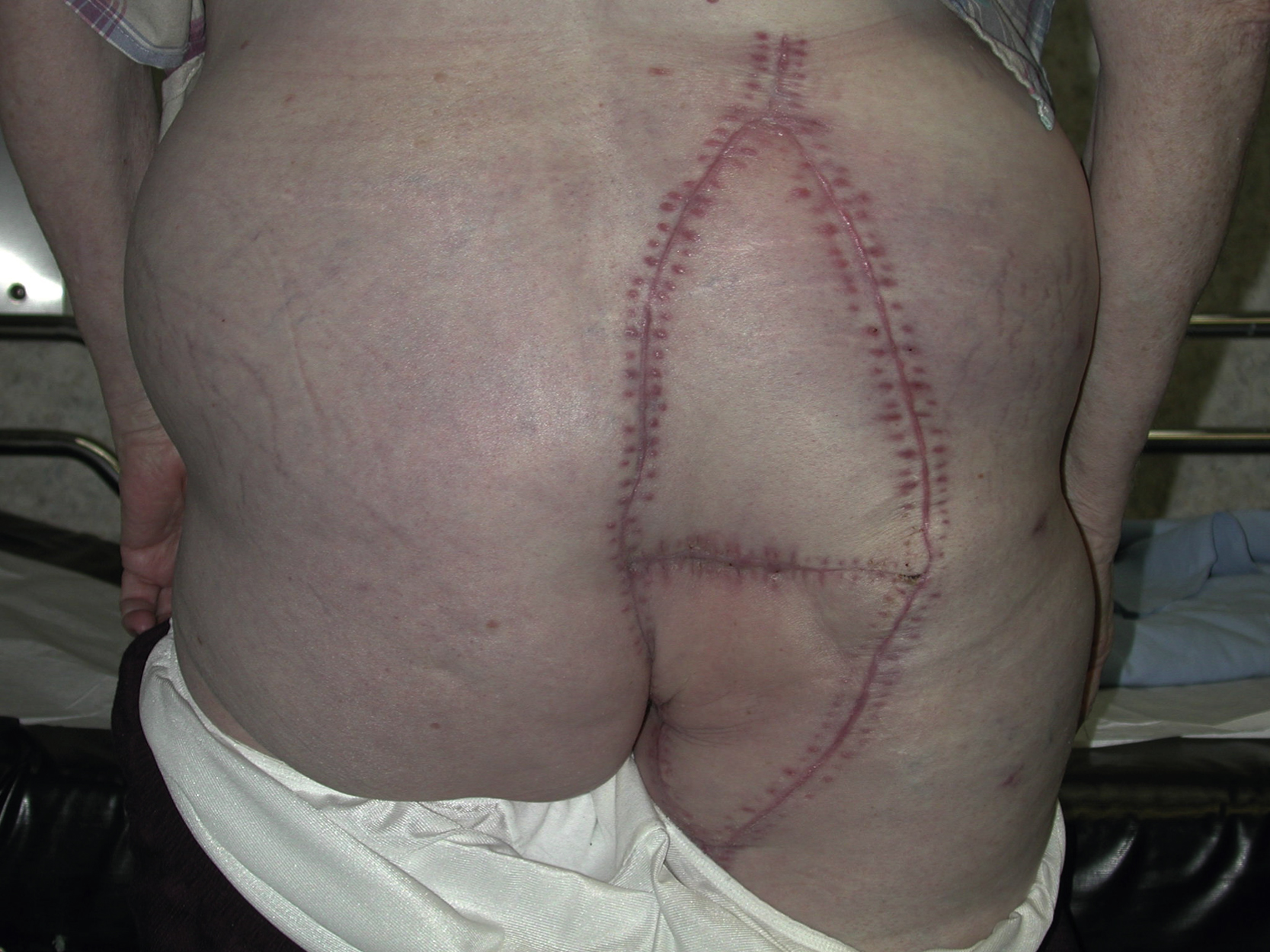
Moderate venous congestion of the superior flap developed at the end of the procedure but was resolved with application of nitroglycerin ointment during the first 2 postoperative days. The postoperative course was also unremarkable and the patient was discharged from the hospital on postoperative day 6. During subsequent follow-up visits, she had well-healed flap sites in the gluteal region and all drains were removed. She was able to ambulate without problems ( Fig. 34.5 ).

Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree