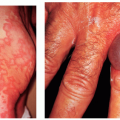
Bullous Dermatoses
John C. Hall MD
To medical students and practitioners alike, the bullous skin diseases appear most dramatic. One of these diseases, pemphigus, is undoubtedly greatly responsible for the aura that surrounds the exhibition and discussion of an unfortunate patient with a bullous disease. Happy would be the instructor who could behold such student interest when a case of acne or hand dermatitis is being presented.
In almost all cases of bullous diseases, it is necessary to examine a fresh tissue biopsy specimen for deposits of immune reactants, immunoglobulins, and complement components at or near the basement membrane zone. Routine histologic examination of a formalin-fixed biopsy specimen is, of course, also usually indicated.
Four bullous diseases are discussed in this chapter: pemphigus vulgaris, dermatitis herpetiformis, bullous pemphigoid, and erythema multiforme bullosum. However, other bullous skin diseases do occur, and in this introduction they are differentiated from these four.
▪ Bullous impetigo: Bullous impetigo is differentiated from the other bullous diseases by its occurrence in infants and children, rapid development of the individual bullae, presence of impetigo lesions in siblings, bacterial culture positive for Staphylococcus aureus, and rapid response to antibiotic therapy (see Chapter 21). It can be a recurrent problem in HIV-positive patients in the groin area.
▪ Contact dermatitis due to poison ivy or similar plants: Bullae and vesicles are seen in a linear configuration. A history of pulling weeds, cleaning out fencerows, or burning brush is usually obtained, and a past history of poison ivy or related dermatitis is common. It is important to remember that this is a form of delayed hypersensitivity and the time between the exposure causing the eruption and the onset of symptoms can be anywhere from 1 to 2 days to 1 to 2 weeks. This delayed nature of the disease commonly leads to an erroneous diagnosis or a correct diagnosis with inability to establish when the exposure occurred and to therefore eliminate all traces of the plant oil from objects where it may be contacted again and result in another outbreak of the disease. The duration of disease is 10 to 21 days if untreated and is quite uncomfortable (see Chapter 8).
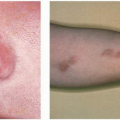
▪ Drug eruption: Elicit drug history (particularly of sulfonamides, nonsteroidal anti-inflammatory drugs [NSAIDs], and antiseizure medications). Fixed drug eruptions are not uncommonly bullous. Fixed drug eruptions are localized, very inflammatory, may blister, leave marked hyperpigmentation, and occur at the same site on drug rechallenge. The eruption usually clears upon discontinuing drugs but this can be delayed for 2 or more weeks. If the patient is not better within a few days of stopping the drug this does not mean that the drug is not the cause of the eruption. Bullae appear rapidly (see Chapter 8).
▪ Epidermolysis bullosa (see Chapter 40): This rare, chronic, hereditary skin disease is manifested by the formation of bullae, usually on the hands and the feet, following trauma. The full clinical and immunologic spectra of these diseases are protean in form of inheritance, severity of disease, and tendency to improve with age.
▪ The simple form (epidermolysis bullosa simplex) of dominant inheritance can begin in infancy or adulthood with the formation of tense, slightly itchy bullae at sites of pressure that heal quickly without scarring. Forced marches or jogging can initiate this disease in patients who have the heredity factor. Such cases are usually treated erroneously as athlete’s foot. The disease is worse in the summer or in climates with high humidity and may be present only at this time. This disease often improves with age.
▪ The dystrophic form of recessive inheritance begins in infancy, and as time elapses, the bullae become hemorrhagic, heal slowly, and leave scars that can amputate digits. Death can result from secondary infection and metastatic squamous cell carcinomas. Mucous membrane lesions are more common in the dystrophic form than in the simple form. Treatment is supportive. Gene therapy may be a future modality but has been disappointing so far. Surgical dressings and skin substitutes (Apligraf) are an
important part of care. Various surgical dressings may be helpful. Mepitel is a dressing I have found especially useful. The blisters should be immediately drained to relieve pain and keep them from enlarging. Secondary infection should be watched for carefully and treated immediately.
▪ A lethal, nonscarring form is also of recessive inheritance but is usually fatal within a few months (see Chapter 40).
▪ Epidermolysis bullosa acquisita: An autoimmune response to collagen where skin lesions can appear similar to bullous pemphigoid, cicatricial pemphigoid, and recessive epidermolysis bullosa. Bulla, scarring, and esophageal disease all occur in this acquired illness. Direct immunofluorescence (DIF) is positive in a linear pattern positive for IgA in the epidermal basement membrane. Dapsone and systemic corticosteroids may be helpful. Trauma can induce blisters that result in scarring.
▪ Familial benign chronic pemphigus (Hailey-Hailey disease): This is a rare, hereditary bullous eruption that is most common on the neck, groin, and in the axillae. It can be distinguished from pemphigus by its chronicity and benign nature and by its histologic picture. Some consider this disease to be a bullous variety of keratosis follicularis (Darier’s disease). It is very painful and can be debilitating. It is caused by a mutation of the ATP2C1 gene.
▪ Herpes gestationis (see Chapter 48): This is a vesicular and bullous disease that occurs in relation to pregnancy. It usually develops during the second or the third trimester and commonly disappears after giving birth, only to return with subsequent pregnancies. The histologic features are believed significantly distinctive so this disease can be separated from dermatitis herpetiformis. Immunologic findings of C3 bound to the basement membrane of the epidermis and occasional immunoglobulin (IgG) deposition may be significant. Therapy with systemic corticosteroids is usually indicated.
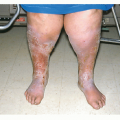
▪ Porphyria: The congenital erythropoietic type and the chronic hepatic type (porphyria cutanea tarda) commonly have bullae on the sun-exposed areas of the body (see the Dictionary-Index under Porphyria).
▪ Cicatricial pemphigoid: This disabling but nonfatal bullous eruption of the mucous membranes most commonly involves the eyes. The skin and mucous membranes may be involved, usually in a localized pattern. As the result of scarring, which is characteristic of this disease and separates it from true pemphigus, eyesight is eventually lost. Over 50% of the cases have skin lesions. Histologically, the bullae are subepidermal and do not show acantholysis. There is quite a bit of immunologic similarity between this disease and bullous pemphigoid.
▪ Linear IgA bullous disease: Most of the children and adults with this disease differ from classic dermatitis herpetiformis in the morphology and distribution of their lesions, have a poorer response to dapsone, and have linear IgA anti-basement membrane zone antibodies. Nontropical sprue is not a part of this illness.
▪ Incontinentia pigmenti: The first stage of this rare disease of infants manifests itself with bullous lesions, primarily on the hands and feet (see Chapter 41). This stage may appear in utero and may not be seen clinically.
▪ Toxic epidermal necrolysis (TEN): Most authors consider Stevens-Johnson syndrome a variant of TEN with less skin and more mucous membrane involvement but with the same clinical picture, histology, prognosis, and treatment. This rare disease is characterized by large bullae and a quite generalized Nikolsky’s sign, in which large sheets of epidermis become detached from the underlying skin with gentle pressure from a finger. The mucous membranes are frequently involved. The patient is toxic. Adults are most commonly affected. Drugs are usually the causative factor, especially in adults. Most commonly implicated are sulfonamides, anticonvulsants, and NSAIDs. There may be a genetic predisposition to this bullous drug reaction. Therapy is supportive, and an appreciable number of cases are fatal. Intravenous immunoglobulins (IVIG) may be lifesaving. Cyclosporine is a preferred mode of therapy by some authors. High-dose systemic corticosteroids are controversial, with opinions ranging from contraindicated to lifesaving if given in very high doses very early in the course of the disease. Some authors would argue that only supportive measures have been shown to be of any benefit. Wound care is essential. Debridement should be avoided. Silver nitrate irrigation and soft gauze dressings (SofSorb gauze, which may be fitted on as a garment) are used in wound care. This is usually done in an intensive care unit because electrolyte and fluid balance is crucial. A central venous line helps greatly in managing these patients. The most crucial factor in survival is stopping any potential offending drug as quickly as possible. Acute graft-versus-host disease can be an identical disease process and should be treated in a similar manner. Mortality for this disease can be significant. A helpful prognostic scoring system is as follows:
Age >40
Underlying malignancy
Heart rate >120
>10% epidermal detachment
BUN >10 mmol/L
Serum glucose >14 mmol/L
Bicarbonate <20 mmol/L
SCORTEN
Mortality
0-1
3.2%
2
12.1%
3
35.3%
4
58.3%
5
>90%
▪ Staphylococcal scalded skin syndrome: Clinically, this disorder is similar to TEN but has been separated from this disease because of the finding that phage group 2 S. aureus is the usual cause. In newborns, this formerly was known as Ritter von Ritterschein’s disease. It also occurs in children and rarely in adults. The prognosis is very favorable. If suspected, antistaphylococcus drugs should be started intravenously immediately. The break in the skin is higher in the epidermis than in drug-induced TEN, and this can be rapidly ascertained with a skin biopsy.
▪ Impetigo herpetiformis: One of the rarest of skin diseases, this disease is characterized by groups of pustules mainly seen in the axillae and the groin, high fever, prostration, severe malaise, and, generally, a fatal outcome. It occurs most commonly in pregnant or postpartum women. It can be distinguished from pemphigus vegetans or dermatitis herpetiformis by the fact that these diseases do not produce such general, acute, toxic manifestations. Laboratory abnormalities include elevated white blood count, elevated sedimentation rate, and low calcium, phosphate, albumin, and vitamin D levels. Bacterial cultures of skin and blood are negative; high-dose (60 to 100 mg q.d.) prednisone and fluid and electrolyte replacement can be life saving (see Chapter 48).
In spite of high medical student and general practitioner interest in the bullous skin conditions, the diagnosis and the management of the three main bullous skin diseases, bullous pemphigoid, pemphigus vulgaris, and dermatitis herpetiformis, should be in the realm of the dermatologist. In this chapter, the salient features of these diseases are presented, with therapy briefly outlined.