Abdominoplasty
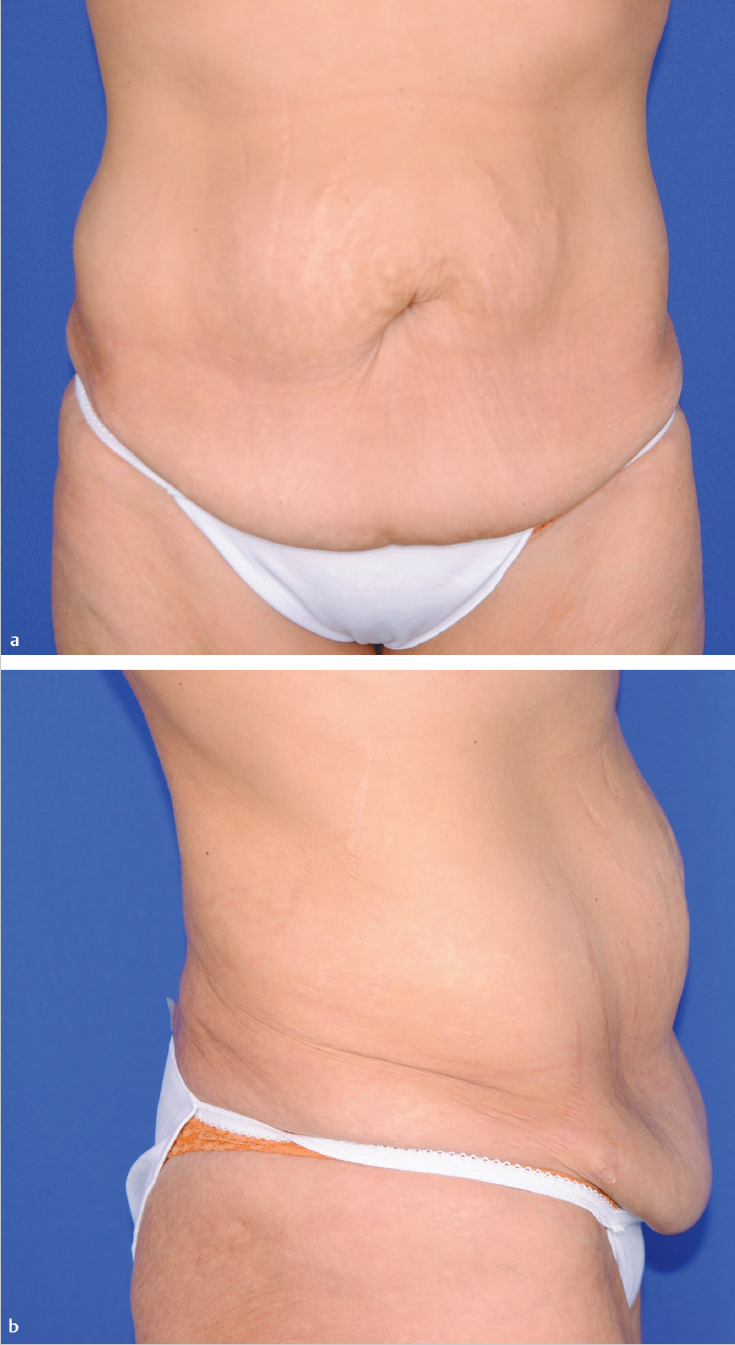
Description
Excess skin and subcutaneous tissue of the central abdomen.
Laxity of the abdominal wall musculature (consistent with weight loss and pregnancies).
Residual localized adiposity of both flanks.
Work-up
History
Assess patient suitability for the procedure and general anesthesia, as well as risk factors for deep venous thrombosis (DVT) and wound-healing problems.
Previous abdominal surgery (including laparoscopic surgery).
History of pregnancies and their effect on the abdomen. Possibility of future pregnancies.
History of weight changes: Weight should be stable and within 10 lb of final desired weight for ~ 3 months before surgery.
Heart disease, peripheral vascular disease, diabetes, steroid use, connective tissue disease.
Smoking history: Must stop smoking 6 weeks before surgery.
History of DVT or pulmonary emboli (PE).
Physical examination
Examine excess skin and soft tissue with the patient in the standing, sitting, and supine positions.
Document any hernias, diastasis recti, or asymmetries.
Note and document the location and size of all abdominal scars.
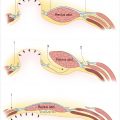
A thorough understanding of the abdominal blood supply is essential.
Pertinent imaging or diagnostic studies
Complete blood cell count (CBC), basic metabolic panel, prothrombin time (PT)/international normalized ratio (INR), activated partial thromboplastin time (aPTT) may be considered.
Urine β-human chorionic gonadotropin level to confirm absence of pregnancy.
Albumin/prealbumin level to assess nutritional status (especially in patients with weight loss).
Urine cotinine level to gauge patient compliance with smoking cessation (if indicated).
Consultations
If an abdominal wall defect or hernia is encountered on examination, a general surgery consultation may be made for intraoperative assistance.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree