Introduction
Burns constitute a high-acuity fraction of the total number of trauma patients treated yearly in the United States. For 2021, the Centers for Disease Control and Prevention (CDC) reported 404,000 ambulatory healthcare visits to emergency departments (EDs) in the United States for burns and corrosions, constituting 2.02% of all ED visits for injuries. However, burns are associated with higher risks and costs than other diagnoses. The Health Care Utilization Project of the US Agency for Healthcare Research and Quality (AHRQ) in its most recent report on burns (for the year 2013) assessed that burns were the primary diagnosis for 53,220 inpatient stays, or 0.15% of total admissions. Length of hospital stay was nearly twice that of other diagnoses (8.1 vs. 4.5 days), cost over twice as much ($24,000 vs. $10,700), had a higher death rate (2.2% vs. 1.9%), and resulted in decreased discharge to independent living (68.0% vs. 70.1%).
Burns have an outsized impact on patients, families, and communities. For example, the healthcare costs of burns are prodigious. The average charges for hospital care of a burned patient range from $48,000 to $1.2 million (average $92,000), with much higher costs incurred by those with extensive burns. The length of hospital stay ranges from 1 day to hundreds of days (mean 9.7), and, for patients 80 years and older, is more than twice that for children under 5.
In this chapter we review the epidemiology of burn injury in the United States and globally. We provide an example of mortality analysis after burn from a single burn center (the US Army Institute of Surgical Research) for the years 1957–2022. Finally, we discuss long-term outcome measures for burn survivors. The main theme of the chapter is that although burn incidence, burn size, and mortality have decreased in the United States, several problems remain. In the United States, burns disproportionately afflict persons from lower socioeconomic communities and those whose age, other comorbidities, or high-risk occupations predispose to injury. Globally, low-income countries experience much higher mortality and disability rates after burn than those in higher-income countries. Striking improvements in mortality in higher-income countries yielded to the problems of long-term survivorship and highlight the value of outcomes other than mortality in assessing the quality of care.
Epidemiology in the United States
Several sources of data are available concerning burn epidemiology in the United States. We reviewed data from the CDC and the American Burn Association (ABA).
United States: CDC data
The current edition of the Web-based Injury Statistics Query and Reporting System (WISQARS) produced by the CDC provides nonfatal and fatal injury and cost-of-care data for the years 2001–21. We found 8,539,700 nonfatal burns in this database (an average of 426,985 per year). Most were classified as unintentional (includes undetermined); 0.5% were caused by self-harm; 1.8% were caused by assault; and 0.7% occurred in the course of legal intervention. Fig. 3.1 provides the nonfatal crude injury rate per 100,000 persons secondary to unintentional burns for 2001–21. The overall rate for the 2-decade period was 127, with a decrease in this rate from 175 in 2001 to 82 in 2021. Most of these patients were treated and released (92.2%), 3.2% were transferred, 3.1% were hospitalized, and 1.6% were observed, left against medical advice, or had an unknown disposition. Thus the great majority of unintentional burns were treated on an outpatient basis in the United States during this time frame.
United States, 2001–21: Crude Injury Rate per 100,000, Nonfatal Unintentional Burns, by Year of Injury.
Fig. 3.2 shows the age and sex distribution of nonfatal unintentional burns over the 2 decades. We found a clear predominance of males in the data, most evidently in the youngest age group (0–4 years) and in adults of working age (20–64 years old). Two peaks are evident in age distribution, one in the youngest group, and the other in the 20- to 24-year-old group. More detailed examination of the data for each year of life shows the peak year for burn risk is actually the second; for 2002–21, the number of nonfatal unintentional burns increased by a factor of 2.33 from the first to the second year of life (data not shown).
United States, 2002–2021: Crude Injury Rate per 100,000, Nonfatal Unintentional Burns, by Age Group and Sex.
Black bars , Males; gray bars , females.
The decrease in the injury rate observed over the 2-decade period has been unequally distributed among age groups, as shown in Fig. 3.3 . The most dramatic decreases in the rate occurred in the pediatric and young adult groups. Meanwhile, the substantial increase in the total number of persons age 65 and older (from 95 million in 2001 to 135 million in 2021) shows the total number of burns in the elderly actually trended upward during this time frame (data not shown). As a consequence of the changing rates for different age groups, the percentage of elderly with burns has steadily increased from 15.8% in 2001 to 24.6% in 2021, a 55.7% increase. The elderly now account for one-quarter of burns in the United States, pointing to the growing importance of geriatric burn care.
United States, 2001–21: Crude Injury Rate per 100,000, Nonfatal Unintentional Burns, by Age Group and Year.
Solid line , Age 0–17 years; Big dashed line , age 18–45 years; Small dashed line , age 46–65 years; Dotted line , age 66 years and up.
Turning our attention to fatal burns, during 2001–21, the total number of deaths was 63,683 and the crude death rate per 100,000 was 1.1. Of these, 87.7% were unintentional, 3.4% homicides, 5.0% suicides, and 3.9% undetermined. Yearly crude death rate data are presented in Fig. 3.4 , demonstrating a slight decrease over the 2-decade period.
United States, 2001–21: Crude Death Rate per 100,000, Fatal Unintentional Burns, by Year of Injury
.
Injuries exact an enormous economic cost, and burns are no exception. For 2021 and considering fatal burns only, the cost of medical care for burn patients was $64.8 million, and the value of statistical life lost was $36.2 billion. This amounts to $36.3 billion in combined costs, or $41.4 million per fatality. For ED treat-and-release cases, the medical costs were $1.2 billion, with an average per patient cost of $10,078. Work-loss costs were $384 million, and quality-of-life costs were $2.7 billion. This sums to $4.3 billion overall or $33,605 per patient. Nonfatal hospitalized patients constitute, as expected, the highest expenditure for medical costs at $2.3 billion, or $142,115 per patient. Work-loss costs were $324 million, and quality-of-life costs were $2.8 billion. This sums to $5.5 billion overall or $344,476 per patient. These data underscore the societal cost of thermal injury, as well as to individual patients and their families, and should energize burn-prevention efforts.
United States: ABA data
The National Burn Repository (NBR) annual report is available from the ABA. The 2022 report contains data for 177,307 patients admitted during the years 2016–21 from 103 of the 143 self-designated burn centers in the United States. Thus it only represents patients who receive inpatient care at those centers. Most cases (41.9%) were contributed by burn centers in the extensive Southern region of the country. Males predominated in the data at 66.1% versus females at 33.9%. Indeed, more males than females were entered across all age groups, except that the sexes were equally represented at the extremes of age (<1 year and >80 years). The leading etiologies for males were flame (31.6%) and scald (24.8%); for females they were scald (31.9%) and flame (22.8%). The age groups most frequently represented in the NBR data are infants (<1 year old) at 3208 cases; toddlers (1–2 years old) at 11,587; and young children (2–5 years old) at 3475 cases (normalized to year of life). Interestingly, older children and adolescents (ages 5–20) are underrepresented.
The overall mortality in the NBR data was 3.2%. As expected, mortality increases with age and with burn size. The combination of burns and inhalation injury yielded a mortality of 26.2%. The mean hospital length of stay was about 8.6 days. Length of stay was a function of Baux score (age plus total body surface area [TBSA]), up to a score of 100 to 109; above that it dropped precipitously, reflecting the effect of mortality.
Most burns occurred as a result of incidents not involving employment (71.8%), followed by employment (9.9%). Most occurred in a private residence (55.3%). The leading mechanism of injury in the NBR report was flame or flash at 36.9%. Flame injuries were associated with a TBSA greater than 20% in 13.5% of cases, occurred along with inhalation injury in 16.5% of cases, and had a 7.1% mortality. Flash burns, by contrast, represented a milder form of injury with a mortality of 2.4%. Contact with a hot object was responsible for 9.8% of admissions. Chemical injury caused 3.1% of injuries. Many chemical injuries (41%) occurred in the workplace and most (68.5%) were less than 10% TBSA. Electric injury caused 2.6% of cases and was even more commonly workplace-related (55%); 89% of these patients were men. Scald burns constituted 29.6% of cases. Children (≤16 years old) represented 41% of scalds, and 14.9% of scalds occurred in children 1 to 2 years old. 95.5% of scalds were accidental. Most (about 75%) were less than 10% TBSA; only a fraction (2.6%) were greater than 20%.
Most patients in the NBR report (75.1%) were discharged home. An additional 7.4% went home with home healthcare services, and 8.7% were discharged to other healthcare facilities such as a skilled nursing facility or an acute rehabilitation unit.
Most burns were below 10% TBSA, which included 68.0% of the cases. Another 11.4% measured 10% to 19.9% TBSA. (Note: These TBSA percentages were calculated from individual burn etiology charts, as overall TBSA ranges were not reported in the 2022 report.) These numbers are all from burn centers, and it is likely that many other burns below 10% TBSA were treated in nonburn hospitals. With this in mind, it is likely that most burns over 10% were treated at burn centers; thus, the distribution in the NBR data is biased toward larger burns.
United States: Epidemiology studies
Regional, socioeconomic, and racial differences impact burn risk (and outcomes) in the United States and point to opportunities for prevention. For example, geographic and housing tract location significantly influences the rate of house fires and the subsequent death rates from associated burns. Age of the home, economic status, number of vacant houses, and immigration status affect the house-fire rate. , House-fire death rates are higher in the Eastern region of the United States, particularly the Southeast, compared with the Western region. Cooking is the leading cause of house fires in the United States, accounting for 49% of house fires and 41% of fire-related injuries. Another leading cause of house fires is heating equipment, accounting for 12% of injuries. Other causes include electrical systems (9%), arson (9%), and tobacco smoking (5%). The cause of house fires with the highest mortality is cigarette smoking, accounting for 24% of residential fire-related deaths. The number of residential fires decreased during 2012–21 by 5% and the number of associated injuries decreased by 7%, but the number of residential fire deaths increased by 8%.
A review of articles on racial and ethnic disparities in the United States showed that minorities often had poorer inpatient and outpatient burn outcomes. Examples included worse psychosocial, pain, and healing outcomes. These studies focused mainly on Black and Hispanic patients, whereas Asian and Native American patients were underrepresented. The review suggests areas for improvement in prevention efforts targeted at burn etiologies experienced by specific communities. For example, Hispanic children were more likely to get injured by a pull-down scald. Understanding the cultural factors, such as how burn scars are interpreted or how the healthcare system is viewed, is likely key to providing optimal care to members of different communities.
In an analysis of the relationship between fire-related injury rates and socioeconomic indicators by census tract in Baltimore for 2005–09, correlates of injury were percentage of vacant homes and percentage of homes built in 1939 or earlier, whereas the percentage of persons over 25 years old with a college degree was protective. In the 59 community districts in New York City, a study found an association between frequency of heating complaints and that of structural fires. Furthermore, fires were more common in Black/non-Hispanic neighborhoods. The authors surmised that heating problems contribute to unsafe home-heating practices and thus to increased fire risk.
Fires detected by smoke alarms have a lower death rate. A Cochrane review of smoke-alarm promotion programs found that (1) promotion programs modestly increase alarm ownership and function but do not affect fire or injury rates; (2) counseling (of parents/guardians) as part of child healthcare may increase ownership and use of alarms; (3) free alarm distribution programs are not effective; and (4) alarm installation programs may increase ownership and function and reduce injuries.
The high quality of care achieved via development of specialized burn centers in developed countries does come with hidden trade-offs for some patients. A geospatial analysis of burn-center location in the United States examined the distance between US counties (in the 48 contiguous states and the District of Columbia) and the nearest ABA-verified adult or pediatric burn center. Rural patients travel twice as far to get to a burn center and incur twice the transport costs as urban patients. Adults have poor access to care in the mountain West, similar to pediatric care in the mountain West and Southeast. No adult burn center is available within 100 miles for 57.5% of US counties, and no pediatric burn center is available within 100 miles of 64.4% of US counties.
Climate change
Increased wildfire activity secondary to climate change is a newly identified risk factor for burns. One study estimated that human-caused climate change nearly doubled the forest-fire area during 1984–2015 in the western United States. These and similar findings predict continued high wildfire risk, but the potential impact in terms of burn injuries and deaths is unknown. The burn center at University of California, Davis, admitted 16 patients from the 2017 Tubbs and the 2018 Camp wildfires. These patients had increased mortality, hospital length of stay, wound infections, and readmission rates.
Global epidemiology
Global: WHO data
We reviewed the WHO’s Global Health Estimates 2019 dataset, which estimates disease burden by cause, age, sex, country, and region for the years 2000, 2010, 2015, and 2019. The crude death rate per 100,000 persons is presented in Fig. 3.5 . It is evident that death rate differs greatly by country income level, from 0.8 for high-income countries to 2.9 for low-income countries in 2019. We calculated a “disparity index,” the ratio of the crude death rate for low-income countries to that for high-income countries, and found it was fairly constant at 3.6 for 2000 and 3.5 for 2019. In other words, the death rate for burns is more than three times greater in low- than in high-income countries. The global crude death rate has decreased from 2.0 to 1.5 over the 19-year period. Numerically, the biggest difference occurred in low-income countries with a delta of 1.1, but the biggest percentage decrease was seen in upper-middle-income countries at 39%. These data indicate that improvements have occurred worldwide, but substantial disparities persist in this injury sector. The data do not, however, distinguish between increased mortality secondary to increased burn incidence, and that secondary to decreased access to or quality of care for those who do get burned.
WHO, 2000–2019: Crude Death Rate by Country Income Level.
Triangles , Low income; diamonds , low-middle income; black circles/solid line , global average; squares , upper-middle income; open circles , high income.
From WHO mortality data, 2019.xlsx. Injury from fire, heat, and hot substances. Global Health Estimates 2019: Deaths by Cause, Age, Sex, by Country and by Region, 2000-2019. Geneva, World Health Organization; 2020.
Disability-adjusted life years (DALYs) are the number of years lost due to ill health, disability, or early death per 100,000 people. DALY by country income group from the WHO Global Health Estimates 2019 are shown in Fig. 3.6 and are similar to those for crude death rates mentioned previously.
WHO, 2000–19: DALY by Country Income Level.
Triangles , Low income; diamonds , low-middle income; black circles/solid line , global average; squares , upper-middle income; open circles , high income. From WHO burn DALY data, 2019.xlsx. Injury from fire, heat, and hot substances.
Source: Global Health Estimates 2019: Disease burden by Cause, Age, Sex, by Country and by Region, 2000-2019. Geneva: World Health Organization; 2020. available at https://www.who.int/data/gho/data/themes/mortality-and-global-health-estimates/global-health-estimates-leading-causes-of-dalys .
Global: Epidemiology studies
Other studies confirmed differences in burn incidence and outcomes across the globe. In one analysis of the Global Burden of Disease Survey 2017, burn-related DALY decreased worldwide by 43.7% from 1990 to 2017. But improvement has lagged in low-middle and low sociodemographic index regions. Africa had the highest age-adjusted DALY rates and the slowest improvement. Similarly, the global age-adjusted death rate decreased from 1990 to 2017. Some areas showed an increase in mortality (e.g., southern Latin America). Mortality is concentrated in mid- and lower-income areas. Three of 21 regions showed a substantial increase in incidence; China increased by more than 30%.
A review of articles on burn epidemiology trends since 2001 compared findings by Human Development Index (HDI) quartiles (very high, high, medium, and low HDI levels). Overall, they identified a downward trend in burn incidence, severity, length of stay, and mortality. However, these trends were most pronounced in very high HDI countries and heterogeneous in high and medium HDI countries. There were no publications from low HDI countries.
Another study examined the relationship between pediatric burn mortality (Global Burden of Disease Study of 2013) and economic indices. Lower gross domestic product (GDP) per capita (from World Bank data) and increased income inequality by country (Gini index) were associated with increased mortality. Food insecurity is also associated with pediatric burn outcomes. A report based on the WHO Global Burn Registry (GBR) and the Economist Intelligence Unit’s Global Food Security Index evaluated death rates among burned children in nine lower- and middle-income countries. Death rates were increased for countries with lower food security. Of note, most of the pediatric deaths in the study were from a single country.
Cooking is a common cause of injury worldwide. Twenty-five percent of burns in one report based on the GBR were cooking related. Of these, 22% were cookstove-related burns. The latter group had higher TBSA and mortality. Most were related to equipment or structural problems (e.g., explosions) rather than to human behavior or movement. Equipment available for cooking varies by country income level; for example, kerosene use is more common and electricity less common in lower- and middle-income countries versus high-income countries. Indeed, kerosene use is more frequently associated with cookstove-related burns than are other fuels.
Global: Country and regional studies
Currently, 200 million to 1 billion people live in informal settlements worldwide; this number is projected to increase to 3 billion by 2030. In South Africa, 18% to 33% of the total population lives in informal settlements. Fire risk is high in these communities. Reported fires in South African settlements increased from 3200 in 2004 to 5544 in 2019. Causes included open flames (40%) and electrical issues. The closeness of dwellings increases the speed of fire spread, as does the use of non–fire-retardant building materials. Fire extinguishment is delayed by long fire-department response times and by unreliable water supplies.
In 2021, an online survey of healthcare workers involved in burn care in Africa was conducted. A separate burn ward was available in 34.7% of centers. Regular skin grafting was done in 39.1% of centers. A significant relationship was found between HDI and mortality. Most respondents (78.2%) attributed poor outcomes to late presentation.
In a review of papers from sub-Saharan Africa, 80% of patients were under 10 years old, the leading cause of injury was scalds, and there was a 17% death rate. Burn care in the region is hampered by a lack of resources, skilled personnel, and appropriate healthcare policies. Competing healthcare issues include the need to address malaria, tuberculosis, and HIV/AIDS.
A survey of 357 households in rural Ghana found, remarkably, that 6.4% of children were burned per year. The most common etiology was flame; 85.8% used open fire for cooking and biomass for fuel; stove height was within reach of children under 5 years in 96% of households.
Face-to-face interviews of over 800,000 households in Bangladesh showed that burns were the fifth overall cause of illness or injury in children ages 1 to 17, and the third cause in children ages 1 to 4. Most burns occurred in the kitchen, and flame burns caused by cooking fires or kerosene-lamp fires were the leading causes. Burns were four times more common in rural than in urban areas.
Studies of burn epidemiology in Nepal identified that females had higher mortality than males, reflecting at least in part a higher rate of flame burns of higher TBSA incurred in the home. Open fires, clothing choices (sarees), and unregulated use of liquefied petroleum gas (LPG) increase risk of such injuries. Because Nepal is mountainous and many people live in remote areas without ready access to transportation, delayed presentation is common; in one study, 31.8% presented more than 1 week postburn. Burns in excess of 40% TBSA are uniformly lethal in this region.
A review of children under the age of 5 years from Mexico treated at the Shriners Institute in Galveston, Texas, all with greater than 20% TBSA, revealed that the leading causes of injury were flame and scald. Flame burns were most commonly caused by explosion of a propane tank or gas line, and scalds by falling into a container of hot fluid.
High-risk populations
Children
In 2020, 228 children died from fires or burns in the United States, with the highest death rate per capita in those under 5 years of age. The number of pediatric burn patients admitted to hospitals is influenced by cultural differences, resource availability, and medical practice. Consequently, it varies by geographic area from a low rate of 1.4/100,000 population in North America to a high of 10.8/100,000 population in Africa.
As noted earlier, children are at high risk of scald injury, representing 41% of such injuries in the NBR. In a report on more than 1000 pediatric scalds in England and Wales, pulling down a hot beverage was involved in a third of cases, whereas nonintentional immersion injuries in baths or showers accounted for only 1.4%. Risk factors for pediatric scald injury have been identified and include male sex, age 1 to 2 years, large sibling group, young mother, single-adult household, living in an area of increased maternal deprivation, immigration from a less-developed country, and less-developed fine motor skills or hyperactive behavior in the child. A recent study conducted in Florida identified an increased risk of pediatric scalds in Black populations with low access to food; children with scalds also had a higher social vulnerability index.
Powered home equipment (e.g., treadmills, vacuum cleaners) can cause friction burns in children. Treadmill burns more commonly affect the volar rather than the dorsal surface of the hand, and often involve skin grafting.
Elderly
An increasing number of elderly persons present with burns, both because they represent an increasing portion of the population in many countries and because of increased risk of thermal injury. Whereas males predominate in younger cohorts of burn patients, the rates of burn by sex are almost even in the elderly. The authors of a paper published in 2000 noted that 77% of elderly patients had one or more preexisting medical conditions. Examination of predictors of mortality revealed that the usual signals such as increasing age, burn size, and inhalation injury remain the most useful in this age group. Several authors reported lower mortality rates in the elderly than expected from standard prediction models, suggesting that we are improving care in this age group as well.
A recently identified factor in burns in the elderly is dementia. Harvey and others identified a 1.6 odds ratio of burn risk in the aged with dementia versus those without. In addition, the burns were more likely to be larger and were more likely associated with ignition of clothing or with scalds; hospital length of stay was twice as long.
Elder abuse can also take the form of severe burn. A congressional report published in 1991 indicated that 2 million older Americans are abused each year. A retrospective review of 28 patients 60 years and older admitted to a single burn center over 1 year identified self-neglect in 7, neglect by others in 3, and abuse by others in 1. Notification of adult protective services was required in 2 cases. The authors concluded that abuse was likely to be underreported because of a low index of suspicion on the part of healthcare personnel.
Disabled
Patients with disabilities are a group considered to be burn-prone and are often injured in the home by scalding. From a 1993 report, the effects of disability and preexisting disease were evident in the hospital length of stay (27.6 days on average) and in the death rate (22.2%) associated with a modest average burn size (10% TBSA).
Healthcare-related risk
Lewis et al. examined healthcare use rates in the United States from 2008–17 by burn patients, both before and after burn injury, and compared them to unburned controls. This included ED visits, outpatient visits, inpatient hospital stays, psychiatric care, and nutrition support. They found increased use before injury for all variables except skilled nursing facility use. Use after injury was increased for all variables and persisted for at least 25 months. Thus people with increased healthcare needs are also at increased risk of burn injury.
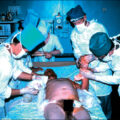
Patients may sustain burns while hospitalized for nonburn reasons. Approximately 2% of surgical anesthesia malpractice claims involved fire in the operating theater, and 85% of these involved head and neck surgery. These were most commonly associated with the use of electrocautery around oxygen sources. Application of excessively hot soaks or towels or inappropriate use of heat lamps or a heating blanket are other causes of injury.
Intoxication
Intoxication increases the risk of thermal injury. An analysis of the 2014 Nationwide Emergency Department Sample database looked at more than 20,000 ED visits by young burn patients (ages 13–25 years) in the United States. They determined burn mechanism and intoxication status (alcohol and/or drugs) using International Classification of Diseases, Ninth Edition (ICD-9) codes and used transfer or admission as indices of more severe injury. The frequency of intoxication increased with age (5.8% for 13–17 years, 25% for 18–20 years, and 69% for 21–25 years). Intoxicated burn patients had a higher likelihood of a flame mechanism of injury. The combination of flame burn and intoxication was associated with increased likelihood of hospital admission or transfer. Thus intoxication is common in burn patients in the United States in this age range, and increases risk of a flame mechanism and of a more severe injury. The Ross Tilley Burn Centre in Toronto, Canada, conducted a retrospective study of 1199 patients admitted during 2006–14. They found a 34% rate of alcohol or drug misuse, which was associated with increased length of stay, bacteremia, and sepsis.
Work-related burns
Work-related burns account for 20% to 25% of all serious burns and also account for about 2% of all workplace injuries. The US Bureau of Labor Statistics (BLS) reported 1,176,340 nonfatal injuries and illnesses in the workplace for 2020; of these, 11,840 (1.0%) were thermal injuries and 3540 (0.3%) were chemical injuries. The leading sectors experiencing thermal injuries were accommodation and food services (5350 injuries), manufacturing (1950), trade transportation and utilities (1330), and healthcare and social assistance (1190). Restaurant-related burns, particularly those due to deep fryers, represent a major and preventable source of occupational burn morbidity. The BLS reported that in 2017 workers in restaurants had a burn injury rate of 9.1 per 10,000 full-time workers, compared with 1.4 for all private industries. The risk of burns due to hot tar (bitumen) is greatest for roofers and paving workers. In one 1982 report, 16% of all accidents involving roofers and sheet-metal workers were burns caused by hot bitumen, and 17% of those injuries were of sufficient severity to prevent work for a variable period of time.
Military personnel
In wartime, military personnel are at high risk for burns, related both to combat and to nonintentional causes. The incidence of burns is associated with the types of weapons employed and has ranged from 2.3% to as high as 85% over the past 8 decades. The detonation of a nuclear weapon at Hiroshima in 1945 instantaneously generated an estimated 57,700 burned patients and destroyed many treatment facilities, which thereby compromised their care. In the Vietnam conflict, as a consequence of the total air superiority achieved by the US Air Force and the relative lack of armored fighting vehicle activity, those with burns constituted only 4.6% of all patients admitted to Army medical treatment facilities from 1963 to 1975. During 1965–70, Neel reported that “over half” of the burns in Vietnam were nonintentional in nature.
Burns during conflicts have not always been this low, as exemplified by the Israeli conflicts of 1973 and 1982, and the British Army of the Rhine experience in World War II. Both of these conflicts were dense, with personnel in armored fighting vehicles who had a relatively high incidence of burns. , The increased incidence of burns, 10.5% and 8.6% in the Israeli conflicts of 1973 and 1982, respectively, as compared with the 4.6% incidence in the 1967 Israeli conflict, was considered to reflect what has been termed battlefield saturation with tanks and antitank weaponry. Decreasing incidence of burns in armored vehicle combat has been attributed to enforced use of flame-retardant garments and the effectiveness of an automatic fire-extinguishing system within tanks. These factors have also been credited with reducing the extent of the burns that did occur. For example, in the 1973 Israeli conflict 29% of burned patients had injuries of more than 40% TBSA, and only 21% had burns of less than 10% TBSA. After institution of garment and fire-extinguisher policies, in the 1982 Israeli conflict those same categories of burns represented 18% and 51%, respectively, of all burn injuries. Thirty-six burns (7.8% of the total 458 casualties) were sustained among the US forces during Operation Desert Shield/Desert Storm in 1990–91, in which there was extensive involvement of armored fighting vehicles.
Burns have also been common during war at sea, as recently reviewed by Tadlock and colleagues. During the Falkland Islands campaign of 1982, 112 (21.7%) of the 516 battle casualties received on the British hospital ship SS Uganda had burns. A single event, an Exocet missile attack on the HMS Sir Galahad, generated 179 casualties for the SS Uganda, of which 83 had burns (46.3%). Of these, 75 were evacuated to the United Kingdom; upon arrival, 48 were admitted to a single burn center. Hand injuries were present in all of those admitted for inpatient hospitalization. Smoke-inhalation injury caused by shipboard fires was also common, with 80 patients admitted to the SS Uganda. Finally, cold injury, specifically trench foot, occurred in 70 (13.6%) of SS Uganda patients.
During recent combat in Iraq, Afghanistan, and surrounding regions (Operations Enduring Freedom, Iraqi Freedom, New Dawn, Freedom Sentinel, and Inherent Resolve), the US Army Burn Center (US Army Institute of Surgical Research [USAISR]) at Fort Sam Houston, Texas, provided care for all US military patients who sustained significant burns. During these conflicts (September 2001–August 2021), 1008 patients were admitted to that burn center from the combat zone. The mean burn size was 16.0% and the mortality rate was 5.5% (Luckado T, personal communication, January 22, 2024).
Furthermore, the US Department of Defense Trauma Registry (DoDTR) aims to collect data on all battlefield casualties treated at US medical treatment facilities, to include host-nation soldiers and civilians. As of November 2019, data from 86,857 patients were available in the DoDTR; burns were present in 6369 (7.3%) of these patients. The leading mechanism of injury for all casualties in the DoDTR (42.6%) was explosives. Furthermore, explosions caused by improvised explosive devices (IEDs) constituted 31.9% of all patients in the DoDTR. IEDs were even more common among those with burns, representing 3302 of 6369 burn patients (51.8%) (Graham BA, personal communication, November 15, 2019). The prevalence of IED burns was first described by Kauvar et al. In addition, nonintentional burns were particularly common during the early phases of these conflicts because of practices such as burning human waste and other refuse with accelerants. ,
Of the 830 US battlefield burn patients discharged from the US Army Burn Center during the peak war years of 2003–13, 11 (1.3%) died after discharge and within 10 years of injury. The causes included drug overdose (5 patients), another war-related injury (3), motor vehicle crash (2), or a nonintentional explosion (1). There was no indication of suicide. The drug overdose deaths featured opioids, a benzodiazepine, a mixture of drugs, or in one case a mixture of drugs and alcohol; these findings point to the risks associated with symptomatic treatment of postburn pain and anxiety and the need for mitigation strategies.
Intentional burns
Burns can be intentional, either self-inflicted or done purposefully by another. The average burn size in intentional burns is larger than other causes, at approximately 20% TBSA. The reasons for intentional burns, specifically assaults, are reported to be conflict between persons including spouses, elderly abuse, and economic transactions. For self-inflicted injuries, these are related to domestic discord, difficulty between family members, and social distress from unemployment. Mortality rates worldwide for intentional burns are reported at 65%.
Self-inflicted burns
It is estimated that 4% of burns (published range 0.37%–10%) are self-inflicted. The psychopathology of self-immolation varies greatly by country and culture. A single-center review of self-immolation patients presenting to University of California, Davis, during 2012–21 revealed 111 patients (3% of total admissions). Risk factors included prior diagnosis of psychiatric illness (especially major depression, schizophrenia, or bipolar disorder), use of illicit substances or tobacco, housing insecurity, and male sex. These patients had larger burns but an increased likelihood of survival when controlling for age, burn size, and inhalation injury. Only 15.3% of survivors of suicide burns were discharged to an inpatient psychiatric facility. Thus the concept of futility for patients with this mechanism is not supported. Over a recent 14-year period, suicide attempts constituted 3.4% of admissions to the burn intensive care unit (ICU) in Hannover, Germany. Preexisting psychiatric diagnosis was present in 75.6% of suicide versus 14.5% of nonsuicide patients. The leading psychiatric diagnosis was a mood disorder in 44.4%. Suicide-attempt burns were larger (TBSA 30.7% vs. 12.3%), had higher mortality (24.4%), lower age, and higher likelihood of a flame mechanism.
Self-immolation as a cause of injury in the Arab world increased after the Arab Spring of 2011. Typical patients were young married women of lower socioeconomic status and educational level. Most often these injuries occurred at home and after marital conflict. Kerosene was the leading accelerant. Although depression was the most common comorbid condition, social issues rather than a previously diagnosed mental illness predominated. A review of 29 studies on self-immolation in Iran reported on 5717 patients. Self-immolation constitutes 25% of suicide cases in Iran and is the most common form of suicide in some parts of the country. Average age was 27 years, most patients were married, few (19%) had a known mental illness, and 70% were female. Lower socioeconomic class predominated: 27% were illiterate and 51% lived in rural areas. This mechanism carried a 61% mortality.
Assault by burning
Assault by burning is most often caused by throwing liquid chemicals at the face of the intended victim or by the ignition of a flammable liquid with which the victim has been doused. These types of injuries are generally rare in the developed world but are quite common in low- and middle-income countries. In one study of such injuries in the United States, risk factors included African-American, female, unemployed, and premorbid substance abuse. Occasionally, injuries will be induced by spouses characteristically dousing the face or genitalia. In India, a common form of spouse abuse is burning by intentional ignition of clothing. When such burns are fatal, they have been called “dowry deaths” because they have been used to establish the widower’s eligibility for a new bride and her dowry.
Child abuse
Child abuse represents a form of burns perpetrated by parents, siblings, caregivers, or childcare personnel. Child abuse has been associated with teenage parents, mental deficits in either the child or the abuser, illegitimacy, a single-parent household, and low socioeconomic status, although child abuse can occur in all economic groups. Abuse is usually inflicted on children younger than 2 years of age who, in addition to burns, may exhibit signs of poor hygiene, psychological deprivation, and nutritional impairment.
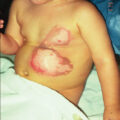
The most common form of child abuse involving burns is caused by hot water in bathing. In a recent report, it was noted that about 5% of pediatric burn admissions were associated with abuse, and most were due to scalds (90%). In a recent British study, those referred for child protection assessment were more likely to have been injured in baths, to have symmetrically located burns, or to have been unwitnessed injuries.
A systemic review of nonaccidental burns in children estimated the incidence at 9.7% of children seen in EDs for burns. Features associated with very high suspicion included burns of the posterior trunk, deep partial- and full-thickness burns, and burns caused by hot tap water. Burns with moderate to high suspicion included those located on the buttocks, genitalia, or legs; those associated with other injuries; and those in younger children. The importance of identifying child abuse in the case of a burn injury resides in the fact that if such abuse goes undetected and the child is returned to the abusive environment, there is a high risk of fatality due to repeated abuse.
Specific mechanisms of injury
Flame and flash
Residential structure fires are the leading cause of fire-related death and involve flame and smoke inhalation injury mechanisms. The National Fire Protection Association (NFPA) recorded that fire departments responded to 1.5 million fires in the United States in 2022. These fires caused 3790 civilian fire deaths and 13,250 injuries; most were in association with structural fires.
Misuse of fuels and other flammable liquids constitutes the majority of flame injuries. This etiology is particularly common in young men. Mortality rates and hospital lengths of stay are greater (up to twofold) than for other burn etiologies. This is probably related to full-thickness burns caused by high-temperature gasoline ignition. Because of these findings, any prevention program should include safe use of flammable liquids.
Another commonly encountered cause of flame burns is automobile crashes. A study conducted in Germany demonstrated that about 1% of car crashes had associated burns; these injuries were more common in frontal and high-energy collisions. In a review of 178 patients burned in an automobile crash, one-third had other injuries, most commonly involving the musculoskeletal system; approximately 1 in 6 had inhalation injury (1 in 3 of those who died). In one review, burns sustained while operating a vehicle involved an average of more than 30% TBSA. They were associated with mechanical injuries (predominantly fractures) much more frequently than burns incurred during vehicle maintenance. The latter involved an average of less than 30% TBSA.
The ignition of clothing is the second-leading cause of burn admissions for most ages. More than three-quarters of deaths due to the ignition of clothing occur in patients older than 64 years. The Flammable Fabrics Act was enacted in the United States in 1953. In 1975, the Consumer Protection Safety Commission codified the Standard for the Flammability of Clothing Textiles (16 CFR 1610). Clothing and textile fabrics are required to meet this standard. It provides a method for testing flammability, establishes three classes of flammability based on time of flame spread, and prohibits the most dangerous fabrics from being used for clothing. The standard was updated in 2023. Since 2000, the deaths per million population attributed to clothing ignition decreased from 0.44 to 0.28. There were 85.8 clothing-related fatalities per year during 2017–21, of which 2.6 per year were related to nightwear.
Scald
Scalds are generally partial thickness; however, full-thickness injury can occur. In particular, full-thickness burns have a much higher incidence with hot-oil burns. Young children are most commonly injured by pulling a container of hot liquid onto themselves, whereas older children and adults are most commonly injured by improper handling of hot-oil appliances. The case fatality rate of scald injury is low (presumably due to the usually modest extent and limited depth of the burn), but scalds are major causes of morbidity and associated healthcare costs, particularly in children younger than 5 years of age and in the elderly.
Tap water scalds can be prevented by adjusting the temperature settings on hot water heaters or by installing special faucet valves so that water does not leave the tap at temperatures above 48.8°C (120°F). In the United States, state and local plumbing codes typically address the temperature of the residential hot water supply.
Contact
Contact burns are the third-most encountered cause of injury and are most common in children and young adults. For children, the incidence is higher due to lack of safety awareness and grasping hot objects. Another cause recently identified was contact burns due to glass-fronted fireplaces. In this study, 402 children were identified with this injury in the United States in a 5-year period. This rate was 20 times higher than that estimated by the US Consumer Product Safety Commission.
Burns caused by prolonged contact with pavement increase during the summertime in hot areas of the United States, especially when the ambient temperature exceeds 35°C (95°F). A review from the Las Vegas, Nevada, burn center for 2014–18 yielded 195 patients with this mechanism, of whom half required excision. Common circumstances included being found down by emergency medical services (EMS) or walking barefoot on pavement. Concomitant hyperthermia was associated with increased TBSA, number of surgeries, ICU days, and mortality. It seems likely that increasing summertime temperatures will increase the incidence of these injuries.
Chemical burns
Chemicals are a well-known cause of burns, and these burns are generally caused by either acidic or alkali chemicals, although chemical burns can also occur with organic solvents. In a recent review of the literature for chemical burns, the reported percentage of burns related to chemical agents is between 2% and 10% of injuries. Most of those affected are men who were injured either in the workplace or domestic setting. Acids caused about 25% of the injuries and bases 55%.
The greatest risk of injury due to strong acids occurs in patients who are involved in plating processes and fertilizer manufacture, whereas the greatest risk from alkalis is associated with soap manufacturing and in the home with the use of oven cleaners. The greatest risk of organic solvent injuries is associated with the manufacture of dyes, fertilizers, plastics, and explosives, and that for hydrofluoric acid injury is associated with etching processes, petroleum refining, and air conditioner cleaning. Anhydrous ammonia injury is most common in agricultural workers, and cement injury (an alkali injury with associated thermal injury) is most common in construction workers.
Electric injury
Electrical current is another cause of injury seen in burn centers; such injuries imply the passage of current through the patient’s body. (By contrast, in other cases the patient sustains thermal injury while working in the vicinity of electrical wires and sustains what should be called a flash injury.) A low-voltage injury is usually defined as one involving less than 1000 V, whereas a high-voltage injury is one involving greater than 1000 V. Approximately one-third of electric injuries occur in the home, with another one-quarter occurring on farms or industrial sites and the rest occurring in the occupational setting. Children may be injured by inserting metallic objects into electrical receptacles or by biting or sucking on electrical cords, resulting in oral commissure burns. Low-voltage direct-current injury can be caused by contact with automobile battery terminals or by defective or inappropriately used medical equipment such as electrosurgical devices, external pacemakers, or defibrillators. , Although such injuries may involve the full thickness of the skin, they are characteristically of limited extent.
Employees of utility companies, electricians, construction workers (particularly those working with cranes), farm workers moving irrigation pipes, oil-field workers, truck drivers, and individuals installing antennas are at greatest risk of work-related high-voltage electric injury. The greatest incidence of electric injury occurs during the summer as a reflection of farm irrigation activity, construction work, and work on outdoor electrical systems and equipment.
During 1994–2008, 26 patients with high-voltage injury and 30 with low-voltage injury were treated at a regional burn center. Mortality was only 3.6%, which is likely biased in that those who died at the scene of injury were not included. Another study reported the outcome of 195 patients with high-voltage electric injury treated at a single burn center during a 19-year period. A total of 187 (95.9%) survived and were discharged. About one-half of patients with high-voltage injury underwent fasciotomy, and, even so, amputation was necessary in almost all of these. Of note, about 15% developed some long-term neurologic deficit, and 3% developed cataracts.
Lightning
Death due to lightning strikes has steadily decreased in the United States; 28 people died per year in the United States from this mechanism during 2006–21. In the United States, these are most common in Florida and the Southeast coast and occur most often in June, July, and August. The typical victim is a young person engaging in outdoor recreation on the weekend. Higher-risk occupations include roofing, farming, and construction. Most injuries in survivors are superficial, and deep injuries are rare. Males are five times more likely to be struck by lightning than are females. Approximately 30% of those struck by lightning die, with the greatest risk of death being in those patients with cranial or leg burns.
Fireworks
Fireworks are another seasonal cause of burns. Approximately 8% of patients with fireworks injuries undergo hospitalization for care, and approximately 60% of those injuries are for burns of specific areas, mostly those of the hands, head, and eyes. According to the US Consumer Products Safety Commission, 14,700 people were treated in emergency departments in the US for fireworks injuries in 2024; 37% of the injuries were burns. Sparklers, firecrackers, and bottle rockets caused the greatest number of burns. Of note, the incidence of such injuries has decreased by 30% over the past 25 years. Males aged 10 to 14 are at the highest risk for fireworks-related injuries, whereas younger males are at highest risk for injuries from sparklers. Proposed prevention measures include reducing the explosive units per package, package warnings, and limiting the sale of the devices to children.
Outcomes: Mortality
In many respects, mortality is the most straightforward quality metric. The earliest comprehensive statistical technique used for mortality assessment after burn was univariate probit analysis. , An early attempt at multivariate evaluation was made at the US Army Surgical Research Unit (USASRU) at Fort Sam Houston, Texas, using probit plane analysis to estimate the relative contributions of partial- and full-thickness burns to mortality. The advent of computers of suitable power and the further development of statistical techniques has reduced the difficulty of analyzing burn mortality and has made these techniques much more accessible.
One of the first comprehensive analyses of this sort was done on a population of 8448 patients admitted for burn care to the USAISR (the successor to the USASRU) between January 1, 1950, and December 31, 1991, and was reported in earlier editions of this book. The USAISR is the second-oldest continuously operating burn center in the United States. Thus data from this burn center provide an invaluable opportunity to understand long-term changes in patient care and their effects on outcome.
To further address the changes previously found up to 1991, we analyzed changes in mortality risk occurring over time from 1950 to 2022. In this analysis, only patients admitted to the burn center on the day of burn or 1 or 2 days after burn were included. This excluded data for 1950–56, years for which date of burn was not available. Furthermore, only patients with flame, flash, and scald injuries were included; those with electrical, chemical, or other thermal processes and exfoliative dermatitides were excluded. Patients of all ages and burn sizes were included. Mortality was assessed as death at any time during the index hospitalization at the burn center, regardless of cause. This dataset’s chief advantage is its longevity; its chief disadvantages are the absence of certain variables such as full-thickness burn size and inhalation injury from the earlier years (which are therefore not included here), and changes over time in certain variables as described later in this chapter.
A total of 12,341 patients met inclusion criteria and were analyzed. The mortality rate was 15.4%. The mean age was 35.0 ± 20.2 years. Mean TBSA was 20.8 ± 22.6%. Fig. 3.7 shows the number of patients admitted per year (and meeting inclusion criteria) and the percentage of those patients who were children (<18 years old). These data demonstrate an increase in the total number of patients over the period of analysis and a decrease in pediatric admissions around the year 2000, corresponding to a change in hospital admission policy. Fig. 3.8 shows the percentage of patients by age and TBSA groups over the entire analysis. Note that burn size is skewed toward small burns (<20% TBSA), a common finding. Fig. 3.9 displays the mean TBSA per year; we found a steady decline from about 40% in the mid-1970s to about 10% at the present time. Meanwhile, Fig. 3.10 shows the mean age of patients per year with a steady increase from the low 20s in the early 1960s, to the high 40s today; this increase in age is only partially explained by the aforementioned loss of pediatric admissions.
USAISR, 1957–2022: Total Number of Patients and Percentage of Pediatric Patients by Year.
Black line , Total number of patients per year; gray bars , percentage of pediatric patients (age <18 years) per year.
USAISR, 1957–2022: Percentage of Patients by Age and TBSA Groups.
Black bars , Age group; gray bars , TBSA group.
USAISR, 1957–2022: Mean TBSA by Year.
USAISR, 1957–2022: Mean Age by Year.
Observed mortality by TBSA group is shown in Fig. 3.11 . This graph demonstrates the sigmoid dose-response relationship between burn size and risk. In these data, small burns have little impact on mortality risk; there is an inflection point at about 20% TBSA burned, after which risk accelerates with increasing TBSA burned; finally, mortality rate levels off at higher TBSA burned. By contrast, observed mortality by age group is shown in Fig. 3.12 . Here, risk is lowest for the 20- to 39-year age group; it tends to plateau at advanced ages. This concept is further discussed later.
USAISR, 1957–2022: Observed Mortality by TBSA Group.
USAISR, 1957–2022: Observed Mortality by Age Group.
We then examined the relationship between mortality and the covariates age, TBSA, and year of injury using binomial logistic regression (backward likelihood-ratio method). In the analysis, age was represented as a cubic age function (age_fn), given by the equation:
This permits use of a single term that captures the observation that the relationship between age and outcome is not linear but rather “bathtub shaped,” with a nadir at about 20 years and a leveling off in advanced age; this relationship is suggested by Fig. 3.12 as mentioned earlier. Considering age function and TBSA as covariates, and using all the data from the 65-year dataset, the probability of mortality is given by the following equation:
Examples of solutions to this equation are as follows. The solution to the equation for various burn sizes, holding age constant at 20 years, is displayed in Fig. 3.13 . This graph can be compared with Fig. 3.11 and more clearly demonstrates the sigmoidal dose-response curve. Similarly, the solution to the equation for various ages, holding TBSA constant at 50%, is displayed in Fig. 3.14 . This graph can be compared with Fig. 3.12 and clearly demonstrates the cubic (bathtub-shaped) age relationship. It is important to remember that this equation was developed using data from the entire 65-year analysis, over which mortality changed significantly. Thus the predictions made by this equation overestimate mortality risk for patients receiving care in the current era.
USAISR, 1957–2022: Predicted Probability of Death as a Function of TBSA at Age 20 Years.
USAISR, 1957–2022: Predicted Probability of Death as a Function of Age at TBSA 50%.
To better demonstrate these changes in mortality, we then performed logistic regression analysis using cubic age function, TBSA, and year of admission as covariates. As expected, this demonstrated that, controlling for age and TBSA, mortality risk decreased over time (data not shown). Next, we performed the analysis again using year as a categorical variable, permitting calculation of odds ratios for mortality for each individual year from 1957–2022; see Fig. 3.15 . The graph is remarkable for two peaks in mortality risk, 1960–63 and 1969–73. The first peak represents a period of increased mortality associated with invasive gram-negative burn wound infections. This peak was followed by a striking decrease in mortality risk in 1964 with the introduction of topical mafenide acetate cream for antimicrobial chemoprophylaxis. The second peak, in 1969–73, reflects the emergence of other virulent gram-negative organisms less sensitive to mafenide acetate (e.g., Providencia spp.). With the introduction of silver sulfadiazine cream, first as a single agent and then as an alternating agent along with mafenide acetate, a subsequent decline in mortality risk occurred. Further decreases in mortality risk were observed with the introduction and then essentially standardized use of burn wound excision in the late 1970s, enhanced infection control in the early 1980s, and improvements in mechanical ventilation in the early 1990s. The reduction in mortality risk has been maintained over the subsequent decades.
USAISR, 1957–2022: Logit Mortality by Year.
Several authors developed easy-to-use mortality predictors based on the above concepts. The original Baux index (age plus burn size) was published in 1961. At that time, the Baux index was roughly equal to the predicted mortality for a group of patients; for example, a patient whose Baux index equaled 100 had a 100% predicted mortality. Since then, improvements in care in developed countries mandated a revision of the Baux score. The revised Baux score also takes into account the presence or absence of inhalation injury and can be implemented using a published nomogram.
Other predictors of mortality
In general, the effect of medical comorbidities on mortality is encompassed by age. In a single-center study, the presence of a comorbidity was an independent predictor of mortality risk along with age, TBSA, and inhalation injury. But the greatest impact of medical comorbidities occurred in the young in this study, which was attributed to the collinearity with age in older patients.
The greatest utility of mortality prediction models probably lies in assessing the effect of systems of care for groups of patients, rather than in predicting outcomes for individuals. For example, this approach was used to identify the patients who, based on burn size, benefitted most from the introduction of mafenide acetate as a topical antimicrobial in 1964. Shirani and colleagues demonstrated the independent and additive contributions of inhalation injury and pneumonia to postburn mortality. Several studies confirm the importance of timely resuscitation, transfer, and surgery on postburn mortality. In the study by Wolf et al. of 104 children with at least 80% TBSA burns, delayed intravenous (IV) access was an independent predictor of mortality. In an evaluation of nearly 2500 massive burns (mean TBSA 55.5%) from 106 burn centers in China in 2014, only 17% of patients arrived at a burn center within 6 hours of injury; predictors of death included burn index (= full + one-half partial TBSA), older age, admission later than 6 hours postburn, and inhalation injury. A recent study using the TriNetX database demonstrated that burn wound excision within 3 days of injury lowers the risk of mortality and infection compared with excision between 4 and 14 days after burn.
Other outcomes
Given the improvements in mortality after burn in developed countries since World War II, attention has recently turned to measurements of the quality of life of survivors as important indices of burn-care outcomes. The burn survivor experiences significant challenges in the physical, psychological, and functional domains, some of which last for years; indeed, severe thermal injury can be a lifelong problem. These changes in turn influence health-related quality of life (HRQoL).
Physical and physiologic outcomes
Physical consequences are often the most outwardly obvious effects of burn injury, and include scarring, amputation, pruritus, and neuropathy. Less obvious but equally impactful are the physiologic consequences. These include hypermetabolism and catabolism, and decreased pulmonary function, aerobic capacity, and heat tolerance. Wilmore and colleagues at the USAISR described the hypermetabolic, catabolic response to thermal injury, and nutritional and pharmacologic interventions to mitigate its effects. The group at Galveston, Texas provided definitive evidence for pharmacologic management of hypermetabolism after severe injury and demonstrated the persistence of this phenomenon for up to 36 months despite successful wound healing and discharge from the hospital. This chronic postburn syndrome features increased resting energy expenditure, decreased lean body mass, increased cardiac output, increased heart rate, increased catecholamine and cytokine levels, and so forth.
Furthermore, researchers in Dallas documented the effect of the chronic postburn syndrome on key physiologic functions. At 2 to 50 years after burn, survivors had reduced pulmonary function values (lower forced expiratory volume in 1 second [FEV 1 ] and maximal voluntary ventilation [MVV]; higher airway resistance) than uninjured normative values. The etiology of these changes is uncertain, but inhalation injury, burn size, or time after burn did not affect the results. On the other hand, Suman and colleagues have shown that exercise training improved pulmonary function after burn.
Greatly reduced maximal oxygen consumption (VO 2max ) was seen in 80% to 88% of survivors at 1 to 51 years after burn. This was not related to time after burn or TBSA burned. Again, the mechanism is uncertain. The authors speculate that physiologic (lean body mass loss), psychological, scar-related, and/or socioeconomic factors may contribute to reduced participation in exercise and thus to reduced aerobic capacity. Six months of progressive community-based exercise training improved VO 2max in patients with no burns, moderate TBSA burns, or high TBSA burns. Presence of burns and TBSA had no effect on the magnitude of the improvement. Muscle biopsies confirmed increased activity of citrate synthase and cytochrome C oxidase.
Grafted skin has impaired vasodilatory and sweating responses that do not improve over time. As a result, burn survivors are at increased risk of heat injury when exercising in the heat. However, survivors can exercise for up to 30 minutes at moderate intensity without risk of heat stress. Also, a 7-day heat acclimation program for burn survivors, consisting of 90 minutes of exercise a day at 40°C, attenuated the increase in core body temperature during exercise.
For some patients, thermal injury appears to be as much consequence of, as it is a cause of, a patient’s physical decline. For example, Singer evaluated mortality at 1 year after admission for 48 people who were burned while smoking on home oxygen therapy and who were admitted to a single burn center. The mean burn size was 2% and the average length of stay was 2 days. Despite this, 1-year mortality was very high at 54%, significantly higher than that predicted by standard variables at 23.5%.
Psychological outcomes
Psychological illness is a common consequence of thermal injury. Acute stress disorder occurs in about a quarter of burn survivors, posttraumatic stress disorder (PTSD) in a third, and major depressive disorder in a quarter. Body image dissatisfaction and insomnia are common. Analysis of data from the Burn Model System study (see later) identified significant psychological distress in 34% of inpatients that did not resolve at 6, 12, or 24 months after burn.
Burn survivors commonly receive narcotics for pain management. A query of the TriNetX database identified that survivors who developed an opioid-use disorder after burn had higher rates of new psychiatric disorders including major depression, generalized anxiety disorder, and PTSD. They also had more homicidal/suicidal ideation, more suicide attempts, and higher rates of polysubstance abuse. Thus burn survivors should be monitored for development of opioid addiction; evidence of addiction should prompt increased attention to mental health; multimodal pain management is essential; and opioid-prescribing practices should be carefully managed.
Families may be adversely affected when a child is burned. Patterson and colleagues administered the Short Post Traumatic Stress Rating Interview (SPRINT) to 159 caregivers of burned children, of whom 4.5% screened positive for possible PTSD. Others documented much higher rates of PTSD and depression in caregivers, likely reflecting the lower mean TBSA in this study of 2.7%.
Functional outcomes
Physical, physiologic, and psychological factors impact the ability of the burn survivor to return to basic and instrumental activities of daily living (ADLs) and work-related tasks. Measures of physical function assess a person’s functional status in self-care, functional mobility, and participation in daily life. Few patient-reported and physical-performance assessments have been validated for burn populations, let alone adopted for universal use. Table 3.1 describes assessments identified over the past 20 years. These assessments may be used to help prioritize and assess the effects of both reconstructive surgery and rehabilitation therapy.
Table 3.1
Functional Assessment Tools for Burn Patients
| Assessment | Activity Assessed | References |
|---|---|---|
| Patient-Rated Functional Assessments | ||
| BHOT | Hand function with daily tasks | , |
| COPM | Function during self-selected activities (up to 5) | , |
| DASH | Upper extremity and hand function during daily tasks | |
| LEFS | Lower extremity function during mobility tasks | , , |
| MHQ | Upper extremity and hand function with daily tasks | , |
| Quick DASH | Upper extremity and hand function with daily tasks | , , , |
| T-MAM for Burns | Ability to perform manual hand functions | |
| Physical Performance Functional Assessments | ||
| FAB | ADL performance in acute care setting | |
| FAB-CC | Bed mobility and transfers to determine ICU-AW | |
| FIM | Performance of upper- and lower-body ADLs | |
| JHFT | Upper extremity and hand function | , |
| PPT | Hand function/fine motor control | , |
| SHFT | Grip and pinch patterns used with various functional tasks | |
| TEMPA | Upper extremity activity with functional tasks | |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree