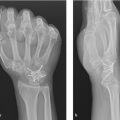
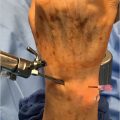
79 Needle Aponeurotomy for Dupuytren’s Disease
Abstract
There are several techniques used to treat Dupuytren’s disease surgically. Needle aponeurotomy (NA) has become more popular after its introduction into United States in 2003 and has gained popularity over the past decade. Its advantage is that it is a simple procedure with a fairly quick return to function, while its disadvantages are that it has a quicker recurrence rate and the potential for nerve or tendon injuries. It is ideally suited for metacarpophalangeal (MP) or mild proximal interphalangeal (PIP) contractures in individuals who want a quicker return to function and are not as concerned with the potential for a sooner recurrence.
79.1 Key Principles
Dupuytren’s disease is prevalent and estimated to affect about 3% to 6% among adult Caucasians or approximately 13.5 to 27 million people in the United States or Europe. It is present in people of all races and peaks in their 40 s and 50 s, with men at 50 years of age and women slightly older at 60 to 70 years of age. The incidence rises with increasing age.
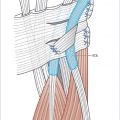
The most common fingers affected in Dupuytren’s tend to be the ring finger followed by the small, middle, and thumb, with the index finger being least affected. There also can be seen web involvement as the proliferative phase develops with the random accumulation of myofibroblast which form palmar nodules. Fibroblast can align along tension lines and form ropelike structures named cords. These collagen cords are relatively acellular and avascular. Often times, there is an early phase skin pitting and/or dimpling. This can be due to the pretendinous bands that connect the dermis to the palmar fascia.
Metacarpophalangeal (MPJ) and proximal interphalangeal (PIPJ) contractures can occur together. The metacarpophalangeal (MP) contractures also can produce natatory bands, which involve the web space between adjacent fingers.
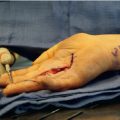
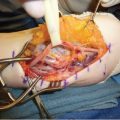
Needle aponeurotomy (NA) was reintroduced in the modern era by Lermusiaux in the 1980s, who used a needle instead of a knife and brought to the United States by Dr. Eaton in the early 2000s. NA has gained popularity significantly in the past several years as an alternative to an open fasciectomy. NA is based on the principles of using a needle to cut the cord versus an open surgical procedure. It is designed to provide a quicker return to function yet also provide a reasonable degree of contracture correction. It requires an understanding of the anatomy and the location to place and cut the cord to provide the maximum correction with minimal complications.
79.2 Indications
NA can be used for either MPJ or PIPJ joint contractures or a combination of both. It, however, has its best and longer lasting results when MPJ contractures are the ones that are corrected, whereas PIPJ contractures have less reliable results. It does require a skill set of having done this previously and usually the patient is kept awake to avoid significant complications.
It is ideally suited for a large cord producing an MPJ or PIPJ contracture with minimally large nodularity. A positive tabletop test is required or an MPJ contracture of at least 30 degree or similar PIP contracture.
Recurrence is usually defined as a greater than 20 degrees contracture after treatment. Across all treatment techniques, the estimated rates of recurrence are almost 65% at 10 years, 30% usually seen in the first and second postoperative years with the additional 15% during the third to fifth, and 10% between the 5th and 10th year. NA is considered for any patient who has a large palpable cord. The larger the cord and the larger the contracture especially at the MPJ, the easier it is to treat.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree