88 Septic Joint
Abstract
Septic arthritis of the hand warrants urgent surgical attention. Delay in surgical treatment can result in rapid articular cartilage degradation from the bacterial toxins, with the inflammatory response and volume overload causing pressure necrosis. Infections of the hand joint can be caused by adjacent spread of an existing infection and less commonly by a hematogenous route. However, the most common mechanism for joint contamination in the hand is penetrating trauma. Direct inoculation through a laceration or puncture is of particular concern when metacarpophalangeal (MCP) joints are involved in clenched fist injuries. Not only is the history of infection source important to the treatment and selection of antibiotics, but also the location of the septic joint in the hand. The distal interphalangeal (DIP) joint, proximal interphalangeal (PIP) joint, MCP joint, and wrist joint all have special considerations when managing pyogenic infections in these spaces.
88.1 Introduction
The management of joint infections in the hand and wrist shares the same principles with treating infections in larger joints. In the closed confines of the relatively smaller space, the bacterial toxins along with immunogenic response both begin to erode the surface within hours after inoculation. 1 Therefore, prompt surgical irrigation of the joint and debridement of necrotic tissue are of paramount importance. Intraoperative cultures should be taken both for aerobic and anaerobic organisms. In clinical settings, where the patient is immunocompromised or has a history of marine water exposure, it is recommended to also include fungal and mycobacterial cultures. Recent studies have had some impact on the antibiotic choice and duration when dealing with small joint infections and will be discussed further in this chapter. 2 , 3 , 4 , 5
88.2 Clinical Presentation
Penetrating injury with a foreign object or a bite is the more common history preceding a joint infection in the finger. An untreated paronychia or felon prior to presentation is also relevant as it can seed the DIP joint. 6 Another source of infection can be a flexor sheath infection, which is known to contaminate the PIP joint if this is left unchecked or undertreated. Systemic signs are less reliable in the diagnosis of the isolated septic finger joint; however, the presence of such signs, such as fever, chills, and abnormal vital signs, should warrant specific attention to a distant source of infection via hematogenous spread.
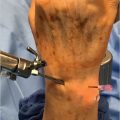
The septic wrist joint has a different presentation from that of the infections of the small finger joints. Usually, it presents as an atraumatic painful wrist that is accompanied by warmth and pain with motion. 7 While important with any infection, a thorough review of the medical history with particular attention to inflammatory and immunological comorbidities is essential when evaluating the likelihood of a septic wrist. 8
88.3 Diagnosis
The diagnosis of septic finger joints has more obvious clinical signs with many times an antecedent trauma involving a human or animal bite, puncture from a thorn or needle, cut with a knife, and many other mechanisms of traumatic seeding of the joint. The septic wrist joint presents differently and warrants more attention to medical history and relies more on diagnostic testing to rule out other causes such as inflammatory arthropathies that may represent an infection.
88.3.1 Physical Examination
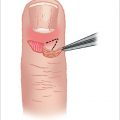
A patient with a septic finger joint usually presents with a readily recognizable fusiform swelling of the involved joint along with erythema, warmth, and pain with any kind of motion. In this setting, the finger is fluctuant and motion may not be possible due to the volume overload in the joint capsule. The site of injury along the involved digit also gives clues as to mechanism of inoculation and will help determine the operative plan. During the examination, the clinician should appreciate even the smallest of wounds over joints as a source of the contamination. However, exam findings of the septic wrist can also be found in painful wrists in many of the inflammatory and other immune system conditions. These signs include warmth, pain with active and passive range of motion, redness, and edema. 7
88.3.2 Differential Diagnosis
The more common conditions in the differential diagnosis for septic arthritis are listed in ► Table 88.1. In the setting of direct trauma, prior surgery, and recent infection, the diagnosis of joint infection can be made readily with correlating exam. Without such predisposing factors and when the exam alone is not enough to establish a diagnosis, a more complete clinical evaluation can be made with proper radiographic and laboratory testing.
88.3.3 Laboratory and Diagnostic Testing
Laboratory testing in any instance where septic joint is in the differential should entail a white cell count (WBC), C-reactive protein (CRP) level, and an erythrocyte sedimentation rate (ESR). When clinically appropriate, uric acid level, Lyme disease titer, and serum inflammatory disease markers should also be obtained. Elevated acute phase inflammatory markers, along with physical exam findings of a painful warm joint, typically put a septic joint diagnosis high on the differential. 9 Despite this, the presence of elevated serum inflammatory markers is nonspecific as examined in many previous studies and can be found in many noninfectious conditions. 10 , 11 , 12
Radiographs can add further evidence in helping to rule or rule out joint infections. In one study looking at wrist inflammation, findings of chondrocalcinosis on radiographs suggest in most cases a noninfectious process. 13 Other radiograph findings particular to different inflammatory arthropathies in the differential are listed in ► Table 88.1.
Given the lack of key pathognomonic imaging or laboratory criteria to establish joint infection, joint fluid analysis re-mains the best option for a definitive diagnosis. 8 Joint aspiration of small joints in itself can be difficult to perform and attempts that yield no fluid doesn’t necessarily rule out joint infection. 10 When a successful arthrocentesis is performed, preference of the synovial fluid analysis should go to gram stain, cultures, and crystalline analysis. 14 A variety of conditions can be identified with synovial fluid testing as detailed in ► Table 88.1. Joint fluid WBC can be obtained if enough volume is available; however, the unpredictability in using this to diagnose septic joint makes this a second-tier option. 14 , 15 , 16 Systematic work-up of suspected joint infections in the hand and wrist involves several elements of clinical evaluation, imaging, and serum analysis. The arrival to a final diagnosis is made with a combination of these findings, rather than any one in particular.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree