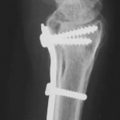
48 Corrective Osteotomy of Metacarpal Malunion
Abstract
Corrective osteotomy of malunited fractures of the metacarpals is a valuable technique for the hand-and-wrist surgeon. In addition to correcting deformity, restoration of normal metacarpal anatomy can relieve pain, improve grasp, correct scissoring of digits, and restore intrinsic tendon balance to correct pseudoclawing of the digits. A variety of osteotomy techniques allow the surgeon to selectively address symptomatic angular, rotational, and length deformities following suboptimal initial fracture healing. With clearly articulated goals, thoughtful preoperative planning, and meticulous operative technique, the surgeon and patient should expect predictable improvement in hand function and correction of deformity.
48.1 Description
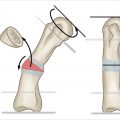
Corrective osteotomy techniques allow the hand surgeon to address symptomatic rotational, angular, and length deformities that occur following malunion of metacarpal fractures. A number of techniques including closing wedge osteotomy, opening wedge osteotomy, and derotation osteotomy are available to address the specific three-dimensional pathoanatomy of the malunion.
48.2 Key Principles
48.2.1 Treat the Patient, Not the Radiograph
Identify the patient’s symptoms and concerns:
Patients may complain of pain, weakness, lost range of motion, and deformity
Articulate the functional deficit to be addressed
Preoperative discussion of desired outcome is essential to a satisfactory result
Typical functional goals for surgery include correction of digital overlap during grasp, or “scissoring,” eliminating pseudo-claw deformity to restore motion, and reduction of metacarpal head prominence in the palm
48.2.2 Diagnose Before Initiating Treatment
Imaging
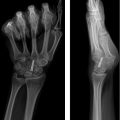
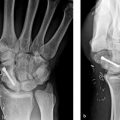
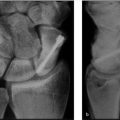
Obtain high-quality radiographs of hand: three views (Postero-anterior, lateral, oblique)
Obtain films of contralateral hand to serve as a template for baseline normal anatomy
Obtain films of initial injury whenever possible
Pathoanatomy of Malunion
Identify the site and direction (rotational, angular, shortening) of the malunion
Identify underlying deforming forces that contributed to metacarpal deformity, so that these may be corrected intraoperatively
48.2.3 Measure Twice, Cut Once
Carefully plan the location, angle, and direction of osteotomy to achieve desired correction
Achieve rigid stable fixation of osteosynthesis site, to prevent recurrence of deformity
Anticipate need for bone graft to augment stability and/or cellularity of osteosynthesis site
Perform frequent re-assessment of correction intraoperatively to ensure patient’s goals are achieved
48.3 Expectations
Following corrective osteotomy of metacarpals, predictable and uneventful bony union should be expected. The surgeon should expect objective improvement in the patient’s functional deficit. The patient should expect resolution of the chief concern and subjective improvement of preoperative symptoms.
48.4 Indications
Symptomatic angular deformities of the metacarpal
Rotational deformity of the metacarpal 1
Less than 20 degrees—metacarpal base osteotomy
More than 20 degrees—osteotomy at malunion site, or step-cut derotation osteotomy
Length discrepancy of the metacarpal
Rotational deformity of the proximal phalanx (up to 20 degrees)
48.5 Contraindications
Active nicotine use
Unresolved infection
Insufficient soft tissue coverage
48.6 Special Considerations
48.6.1 Hardware Selection
Rigid stable fixation of the osteotomy site is essential for predictable union, early postoperative mobilization, and optimal outcomes
2.0/2.4 mm metal plates and screws are typically used to achieve stable fixation of metacarpal osteotomy sites
Many plating systems include purpose-made corrective osteotomy plates with oblong holes that facilitate angular stability, while permitting rotational adjustment, which allows the surgeon to “dial in” the degree of correction desired
The use of locking screws minimizes undesired deformation of osteosynthesis site during fixation
48.6.2 Bone Graft Selection
>For most cases with less than 1 cm of anticipated bone deficit, compressed cancellous autograft (from iliac crest, or distal radius) provides satisfactory material to fill the defect.
For defects larger than 1cm, structural corticocancellous iliac crest autograft may be useful, and additional lag screw fixation of the bone graft to the plate can enhance stability.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree