51 Capitate Shortening Osteotomy
Abstract
Capitate shortening osteotomy is a procedure used to mechanically unload the lunate in patients with early stage Kienbock disease. This procedure has traditionally been utilized for patients with neutral or positive ulnar variance where radial shortening osteotomy is contraindicated. The goal of the procedure is to decrease the load on the lunate, allowing revascularization and preventing articular collapse. Capitate shortening osteotomy is a technically straightforward procedure that entails excising a 2-mm wafer of bone from the capitate waist. Reported outcomes are in-line with other unloading procedures for early stage Kienbock disease.
51.1 Introduction
Capitate shortening osteotomy was introduced by Almquist 1 in 1986 as a procedure to mechanically unload the lunate in early stage Kienbock disease. It was originally described as a treatment option for those patients with ulnar neutral or positive variance when joint leveling procedures, such as radial shortening osteotomy or ulnar lengthening, are contraindicated. However, capitate shortening osteotomy can be utilized independent of the length relationship between the radius and the ulna and does not affect the kinematics of the distal radioulnar joint. The goals of capitate shortening osteotomy are decreasing the mechanical load on the lunate, promoting revascularization, and halting the progression of disease. Various adjunct procedures have been described with capitate shortening osteotomy including capitohamate arthrodesis 1 and vascularized bone grafting of the lunate. 2
51.2 Indications
Capitate shortening osteotomy can be used as a lunate unloading procedure in Kienbock disease in patients that have failed conservative treatment as well as primary treatment in Lichtman stages II (X-ray positive but without articular surface collapse) and IIIa (articular surface collapse but without carpal collapse). Traditionally, it has been used in ulnar neutral and ulnar positive variance, when joint leveling procedures are contraindicated; however, it can be utilized regardless of variance.
51.3 Contraindications
Lunate fragmentation
Advanced arthritic changes of the radiolunate articular surface
Advanced arthritic changes of the midcarpal articular surfaces
51.4 Operative Technique
A dorsal longitudinal incision is utilized in-line with the middle finger ray, beginning at the base of the middle finger metacarpal and extending proximally to the radiocarpal articulation. The distal aspect of the extensor retinaculum may need to be incised to allow for appropriate retraction of the fourth extensor compartment. A posterior interosseous neurectomy may be performed at this time as a wrist capsule denervation procedure. A longitudinal dorsal capsulotomy is performed exposing the capitate and lunate. Direct observation of the lunate is undertaken with specific attention toward any fragmentation. Gentle traction is applied along the middle finger and the proximal and distal lunate articular surfaces are inspected. The surgery proceeds if no contraindications are met.
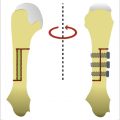
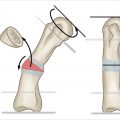
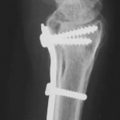
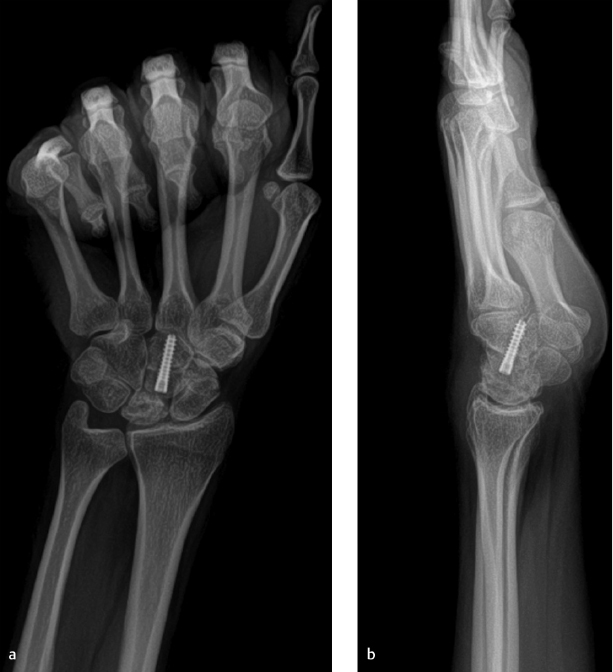
Parallel cuts are then created at the capitate waist with a fine oscillating saw so as to remove a 2-mm wafer of bone. The kerf of the blade should be taken into account when planning the cuts in order to remove the appropriate thickness of bone. The cut surfaces are manually compressed using a blunt instrument inserted into the capitolunate articulation. Fixation of the osteotomy can occur using various methods including K-wires, headless compression screw, or staple. It is the author’s preference to use a headless compression screw placed antegrade (► Fig. 51.1). Wrist flexion aids in presenting the capitate head for placement of the screw, taking care not to distract the osteotomy site with the maneuver. The wound is closed in layers and a short-arm splint is applied which is maintained until the first postoperative visit. At that time, a short-arm cast is applied and is continued until union is confirmed on radiographs, typically in 6 to 8 weeks. Gentle range-of-motion exercises are initiated at that time; however, the wrist remains protected by a removable splint until there is evidence of revascularization of the lunate.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree