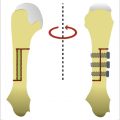
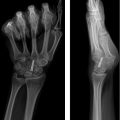
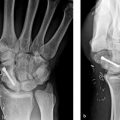
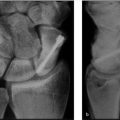
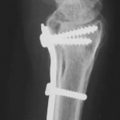
47 Phalangeal Osteotomies
Abstract
This chapter is a review of phalangeal malunion and the methods for correction including malunion evaluation, treatment options, and tips regarding phalangeal osteotomies. Given the variety of surgical options, surgeons must preoperatively plan in advance regarding the location, type, and fixation of osteotomies. While there are a variety of methods for surgical correction, operative procedures do not always achieve desired outcomes. Therefore, preoperative discussion must include current hand function difficulties and expected outcomes. Nonetheless, well-planned phalangeal osteotomies when indicated can achieve appropriate correction and improve overall hand function.
47.1 Description
Malunion is the result of a fracture healed with deformity. The bone is stable, but the functional impact is determined by the location, type, and severity of the deformity. Osteotomy allows for deformity correction to achieve acceptable alignment with internal fixation. 1
47.2 Key Principles
In assessing a malunion, multiple factors must be evaluated.
Malunion site, including extra-articular or intra-articular, combined, proximal, or distal metaphyseal, or diaphyseal
Deformity type: radial or ulnar deviation, flexion or extension, pronation or supination, shortening, or combination
Degree of healing, including immature versus mature callus
Soft tissue involvement, including integrity/adhesions of the flexor and extensor tendons and condition/contracture of joint capsules 2
Furthermore, it is important to assess the patient’s overall hand function, treatment goals and expectations, and specific functional limitations with daily activities. This information is vital in determining course of action to maximize that patient’s outcome.
47.3 Expectations
Benefits of corrective osteotomy include improved function and dexterity of the affected and adjacent digits and the hand as a functional unit. When phalangeal malunions persist, long-term complications include flexor tendon adhesions, extensor lags, flexor and extensor imbalance, and adjacent joint contractures. 1
47.4 Indications
Malunion management is variable and is up to individual surgeon and patient preference, as patients will have different functional requirements and personal desires. 1 While most malunions involve a combination of deformities, usually there is one major component causing functional change and causing surgical consideration. 3 Phalangeal malunions greater than 15 degrees in the sagittal plane or 10 degrees of malrotation that are symptomatic or functionally obstructive may benefit from osteotomy. 1 , 3 Other indications include pain or decreased grip strength. 4
47.5 Contraindications
Acceptance of mild or sometimes greater deformity with a healed and asymptomatic malunion may be preferred when there is uncertain prospect for functional improvement. Physicians should have particular restraint in late presenting (> 10 weeks) patients and those with clinically stable malunions as near-perfect results are not typical and therapy focused on improved motion and strengthening may be an acceptable alternative to surgery. Furthermore, correction for cosmesis alone without functional restrictions should be discouraged. 1
47.6 Special Considerations
A detailed preoperative evaluation is important. This should include deformity and functional limitation assessment, including investigation of the bone and soft tissues. X-rays of the malunion site will help to determine potential correction sites and need for possible bone graft. 5
Surgical timing is important as osteotomies performed earlier will allow for easier soft tissue rebalancing and deformity correction prior to the onset of tendon adhesions and joint contractures. If an osteotomy cannot be attempted prior to 10 weeks, consider starting a therapy program to maximize digital motion, and delay surgery until the 3-month mark. 1
When surgery is necessary, the physician must choose among approaches, osteotomy site, operative techniques, fixation devices, and rehabilitation regimens. 1
Preoperative discussion and patient selection are vital as both surgeon and patient should comprehend the potential benefits and realistic expected outcomes. Furthermore, both parties should be aware of the potential need to change surgical plans in the case of intraoperative complications such as intraarticular fragmentation or fixation failure requiring joint reconstruction or fusion. In this case, the surgeon may need other implants or methods of fixation available.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree