86 Felon
Abstract
A felon is a subcutaneous abscess of the tip of the finger involving the palmar pad. A felon left untreated can cause compartment syndrome of the distal phalangeal pulp. Staphylococcus aureus is the most common causative organism for a felon. Prompt incision and drainage is indicated to prevent pulp loss and neurologic damage at the tip of the finger. Prompt drainage can also prevent spread into the distal phalanx, distal interphalangeal joint, and flexor tendon sheath. Incisions that lower the chance of skin necrosis or neurological damage should be used.
86.1 Description
A felon is an abscess of the deep tissues of the palmar surface of the fingertip or thumb that is typically caused by a bacterial infection.
86.2 Anatomy
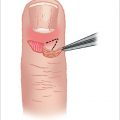
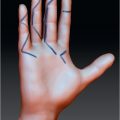
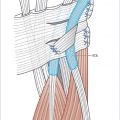
The anatomy of the distal pulp is different from the rest of the finger. Multiple vertical trabeculations divide the pulp space into distinct separate septal compartments. The trabeculae give the fingertip strength by running from the periosteum of the terminal phalanx to the skin. These septal compartments are filled with adipose tissue and eccrine sweat glands which exit into the glabrous skin. The digital arteries run along the volar radial and ulnar sides of the distal phalanx. Just volar to the arteries are the digital nerves. The nerves have extensive terminal branches on the volar aspect of the fingertip which provide for excellent tactile discrimination.
86.3 Pathophysiology
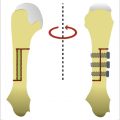
Bacteria can enter the distal pulp via a variety of ways. This can occur by direct inoculation with a needle stick or with a penetrating foreign body. Skin bacteria can also enter via the eccrine sweat glands which lead directly to the distal pulp and are contained in septal compartments. These compartments are unyielding to any increased pressure. The resultant inflammation and abscess formation leads to ischemic pain and continued vascular comprise. If not decompressed, the felon can progress to digital ischemia and skin slough. Additionally, due to the strength of the skin in this location, the infection continues deeper to cause damage to the bone and joint capsule as opposed to decompressing itself through the skin. 1
86.4 Pathogens
The most common causative organisms are Staphylococcus aureus followed by streptococcal species. Community-acquired methicillin-resistant Staphylococcal aureus (CA-MRSA) is so common that first-line antibiotic regimen should now include coverage for such. The incidence of MRSA ranges from 34 to 73% of all hand infections. 2 A felon infection is more likely to be MRSA when looking at all hand infections. 3 In this paper looking at all hand infections, felon was 1.9% of the total but 6.3% of the CA-MRSA infections. Intravenous drug use and a prior hand infection were additional risk factors for CA-MRSA infection. Cases of felons due to gram-negative bacteria have been reported. 4 Eikenella corrodens or Pasteurella multocida may be causative when the penetrating injury was a human or animal bite. Patients with diabetes or who are immunocompromised are more likely to have polymicrobial infections.
86.5 Risk Factors
Patients who are required to do fingerstick measurements for blood glucose are at risk for direct inoculation. Individuals in occupations where their hands are around dirty, sharp objects and those who are exposed to animals and potential animal bites are theoretically at risk. Immunocompromised individuals are also at risk.
86.6 Differential Diagnosis
Gout, pyogenic granuloma, and herpetic whitlow can mimic infection. Local trauma can present with pain, redness, and swelling. Localized cellulitis without abscess can have similar subjective complaints. Determining when a superficial infection becomes deep is difficult, and additional imaging may be needed.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree