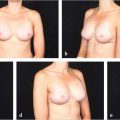
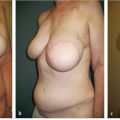
47 Latissimus Dorsi Flap Anatomy
Summary
The anatomy of the latissimus dorsi muscle is key to understanding and safely performing this flap for breast reconstruction. It has a track record of exceptional reliability, is easy to raise, and has a long and consistent large vascular pedicle with a long arc of rotation. It is useful for both primary and secondary salvage breast reconstruction.
Key Teaching Points
The flap carries a large, well-vascularized skin pedicle.
Fat necrosis is not a significant problem with this flap.
The vascular pedicle is large, consistent, and easily dissected.
The arc of rotation is extensive.
Donor site closure must be well performed with adequate long-term drainage to reduce seroma formation.
Use of the myocutaneous flap results in a 15% loss of humeral extension at the shoulder.
A perforator (thoracodorsal artery perforator) flap may be raised if muscle is not required.
The serratus fat pad is a consistently present anatomical landmark that is helpful in guiding dissection.
47.1 Latissimus Dorsi Morphology
47.1.1 Morphology
Extending over the lower half of the thorax and lumbar region, the latissimus dorsi muscle is a large triangular back muscle, thinner at its origin and becoming much thicker toward its insertion (▶Fig. 47.1).
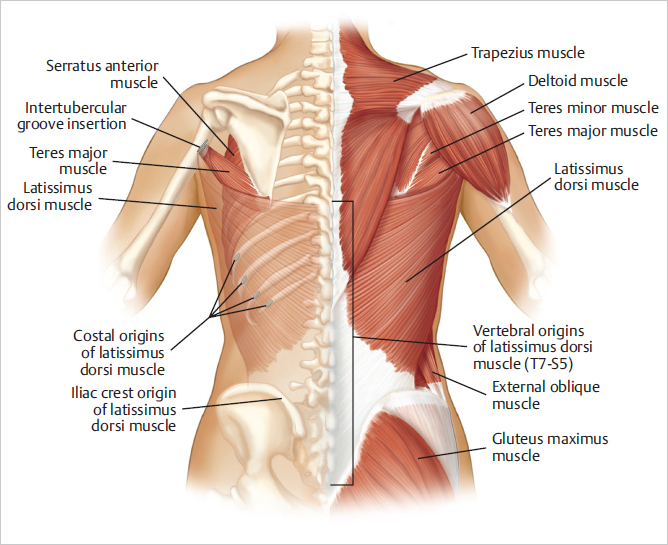
47.1.2 Origin
Spinous processes of T6 to T12, and the lower third to fourth ribs laterally, where it is closely associated with some origins of the external oblique muscle, the posterior layer of the thoracolumbar fascia, and the iliac crest. It is thinnest approximately 1 cm from its medial and lower fascial origins; it becomes thicker laterally, up to 2 to 2.5 cm, as the fibers converge toward the axilla from the inferior tip of the scapula toward the insertion onto the humerus.
47.1.3 Insertion
Medial lip of the intertubercular groove of the humerus.
47.1.4 Action
Internal rotation and extension of the humerus.
47.1.5 Arc of Rotation
The muscle can be transposed anteriorly to reach the sternal notch and even the cheek superiorly, while inferiorly it can reach the xiphisternum when the pedicle is skeletonized to its origin. Complete division of the insertion into the humerus can extend the arc of rotation to several centimeters.
Over the inferior tip of the scapula, the muscle fibers may have some adherence to the teres major muscle; the latissimus dorsi muscle spirals laterally and anteriorly around the teres major toward its insertion. The latissimus dorsi insertion is through a 3-cm broad tendon attached to the medial lip of the intertubercular groove of the humerus. The tendon and proximal latissimus dorsi muscle actually encircle the teres major, which is the muscle that primarily contributes to the form of the posterior axillary fold. This fold is unaffected by anterior transfer of the latissimus dorsi muscle and its insertion, because the teres major remains to give it a form (▶Fig. 47.2).
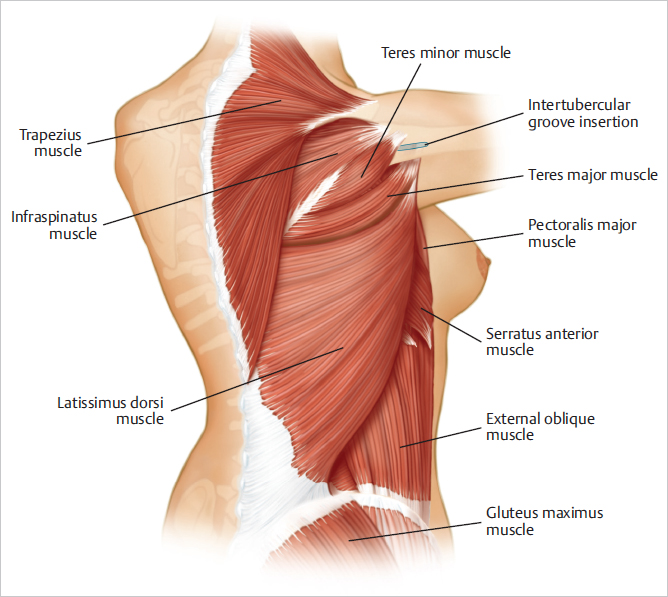
Except for its insertion and a small triangular segment covered by the trapezius muscle in its upper medial region, the outer surface of the latissimus dorsi muscle is entirely subcutaneous. It extends posteriorly nearly to the midline and approaches the posterior iliac crest, at which point it merges into tendon and thoracolumbar fascia.
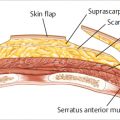
The deep surface of the latissimus dorsi muscle is positioned above the ribs and the medial and inferior aspect of the serratus posterior muscles. Its position is superficial to the serratus anterior muscle, which extends posterolaterally from a line drawn from the inferior tip of the scapula to the eighth rib. Fascia connects the latissimus dorsi and the medial free margin of the serratus anterior; these attachments must be divided during latissimus dorsi flap mobilization to prevent elevating the serratus anterior muscle along with the latissimus dorsi muscle.
Technical Pearl
A useful guide during dissection of the muscle is the fat pad overlying the serratus anterior muscle. Unless it is required for additional volume (which is rare), this fat pad can be followed along its superficial surface, leading the surgeon safely to the medial border of the latissimus dorsi without any risk of inadvertently elevating the serratus anterior muscle (▶Fig. 47.3).
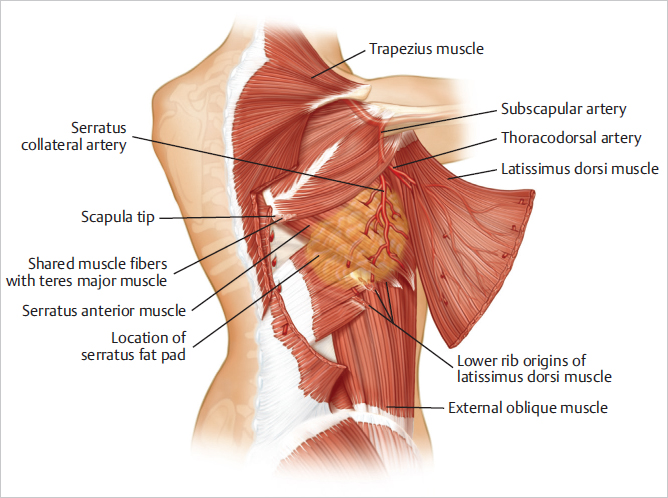
The latissimus dorsi, serratus anterior, and teres major muscles are in close association from the inferior tip of the scapula to its insertion, with the latissimus dorsi spiraling around the teres major when approaching the insertion and remaining superficial to the serratus anterior muscle. Across its superior margin the latissimus dorsi extends from the posterior axillary fold just above the inferior tip of the scapula to the spinous process of T6 posteriorly. Its lateral margin is located along the midaxillary line and also marks the lateral extent of breast parenchyma. It is the reference point for the lateral margin of a mastectomy dissection. Because the lateral latissimus dorsi margin is also the lateral extent of the mastectomy, some deep scar tissue is elevated with the flap for breast reconstruction.
Elevation of the latissimus dorsi muscle after a mastectomy should pose no threat to its vascularity, because the dissections are made anteromedially over the serratus anterior muscle, but not in contact with the flap’s major vascular pedicle.
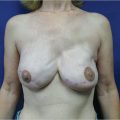
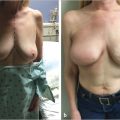
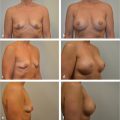
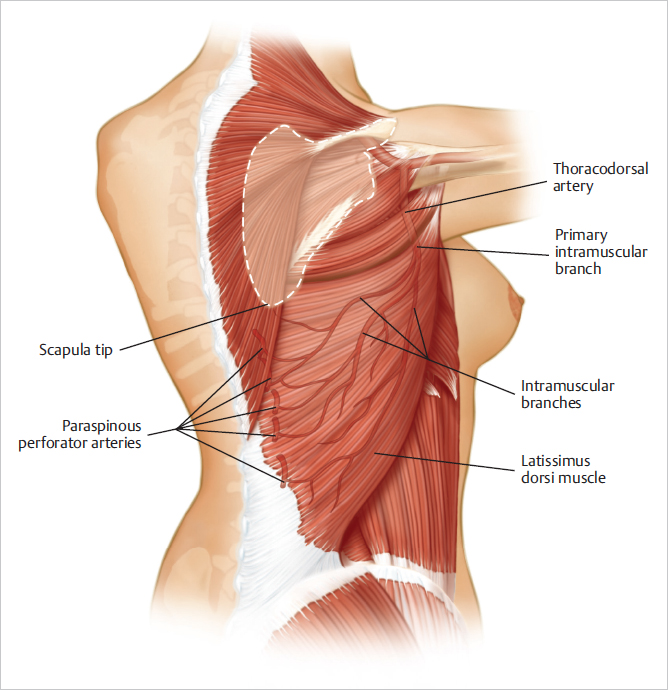
The skin and subcutaneous tissue superficial to the entire muscle and an area of skin approximately 3 cm beyond the muscle margin may be included in the cutaneous territory of the latissimus dorsi musculocutaneous unit. There is a more vigorous blood supply over the upper two-thirds of the latissimus dorsi muscle when the flap is based on the thoracodorsal pedicle. When requirements dictate a skin island of the distal third of the latissimus dorsi muscle, its viability is enhanced by constructing a longer skin island with the proximal portion based over the upper two-thirds of the latissimus dorsi muscle (▶Fig. 47.4).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree