4 Selection of the Surgical Approach
Summary
Breast augmentation with implants may be accomplished through various surgical incisions. These include the inframammary, periareolar, transaxillary, and transumbilical approaches. This chapter will discuss these various options and discuss technical considerations as well as advantages and disadvantages of the different techniques.
4.1 Introduction
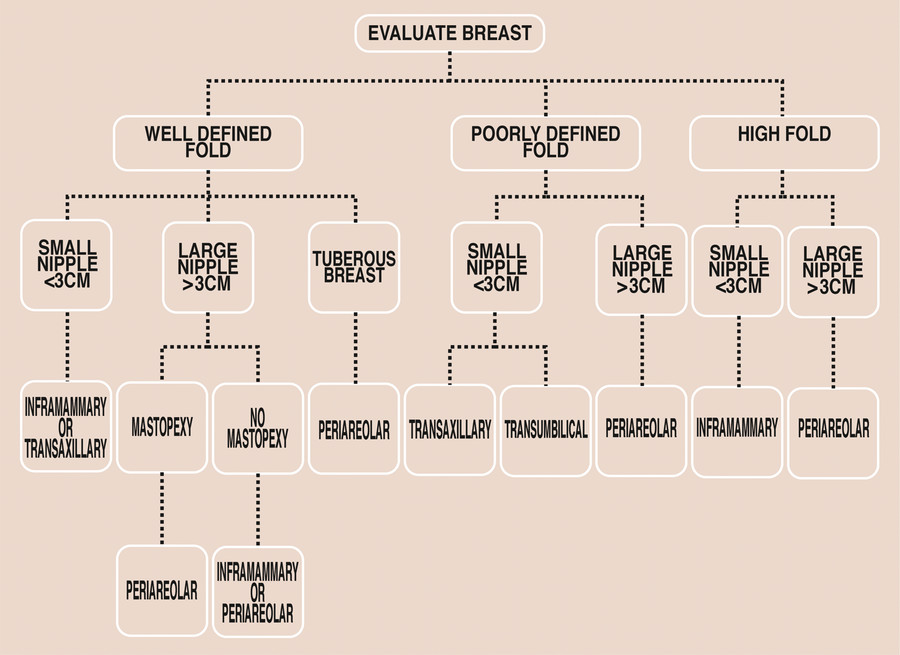
Selection of incision location is an important component of the breast augmentation consultation that must be discussed between the patient and the plastic surgeon. Available options include inframammary, periareolar, transaxillary, and transumbilical approaches. Each technique has its own advantages and disadvantages. The plastic surgeon should be well informed about each to select the approach that is best suited for each individual patient (Fig. 4‑1). For all incision types, the surgeon must balance the desire for an inconspicuous scar with the need for adequate exposure for dissection that will accommodate the implant and minimize the chance of complications. This chapter will focus on the technical aspects of each technique, favorable/unfavorable patient anatomy for each approach, effect on nipple sensation and breastfeeding, and rate of capsular contracture associated with each approach.
4.2 Approaches
4.2.1 Inframammary Fold Breast Augmentation
Most published literature regarding breast augmentation involves the use of the inframammary incision. Therefore, it is certainly the best-studied approach and is the incision of choice for most plastic surgeons. 1 A 4- to 5-cm transverse incision is made in the skin parallel to the inframammary fold (IMF) with a scalpel. For ideal aesthetics, the inframammary incision should be centered over a vertical line marking the meridian of the breast or shifted slightly laterally. A medially shifted incision tends to be more visible and thus less desirable. Electrocautery is used to dissect through the superficial fascia of the breast at a 45° angle until the pectoralis major muscle fascia is reached. The surgeon can then elect to develop either a subpectoral, a subglandular, or a subfascial pocket for implant insertion.
Special attention must be given to asymmetry of the native IMFs when planning the inframammary incision. In the majority of patients, the left IMF is located slightly more superiorly. 2 The difference in IMF position can be more easily visualized by drawing a horizontal tangent line from each IMF to the midline. Differences in IMF position can be managed by lowering the more superiorly positioned IMF to a more inferior level by placing the skin incision at the more inferior horizontal tangent level bilaterally. However, this will not correct asymmetry in craniocaudal position of the nipple areola complex (NAC). For instance, if both the IMF and NAC are positioned more superiorly in the left breast, lowering the left IMF to the same level as the right IMF will not change the more superior position of the left NAC compared to the right NAC. Therefore, the nipple-to-incision distance will not be the same bilaterally even though the new IMF and breast mound positions will appear more symmetric.
Compared with the other approaches, careful planning of the exact location for the inframammary incision is critical so that it lies precisely in the IMF at the end of the operation (Fig. 4‑2). Insertion of an implant stretches the breast skin to accommodate the increased volume, often recruiting abdominal skin onto the breast mound and thus lowering the IMF to a more inferior position. Therefore, in patients with relatively short nipple-to-IMF distances undergoing augmentation using an implant with a wide base width, the incision should be made inferior to the native IMF on the abdominal wall such that the incision will ultimately lie in the IMF after the implant is inserted and the IMF is lowered by the implant. Effective lowering of the IMF by an implant is a product of tissue shifting such that structural integrity of the lower border of the breast is maintained and should not be confused with iatrogenic violation of the IMF, as the latter can lead to a double-bubble deformity and inferior malposition of the implant.
Various calculations have been proposed for selecting the precise location of the inframammary incision based on implant dimensions and nipple-to-IMF distance. The Randquist formula is a simple approach that has been effective in the authors’ practice (Table 4‑1). 3 The Randquist 3 and High Five 4 systems are commonly used formulas but have been criticized as basing their calculations on inconsistent measurements such as skin stretch. 5 Recently, the ICE principle was introduced, which relates the implant dimensions (I), the capacity of the breast (C), and the excess tissue needed to accommodate the implant (E), equal to the difference between I and C. 6 The authors showed greater than 99% accuracy of scar placement in the IMF through calculations based on implant dimensions and nipple-to-IMF distance. 6
After placement of the implants, the inframammary incisions should be closed in three layers (superficial fascia, deep dermal, and subcuticular). Some authors have advocated the placement of three-point sutures between the superficial fascia of the breast, superficial fascia of the IMF, and deep fascia of the IMF in select patients to prevent inferior malposition over time. 7 When implants are placed in a subpectoral pocket, the IMF is subjected to repeated downward force by the implant from contraction of the overlying pectoralis major, with progressive instability of the IMF.
Advantages and Disadvantages
Advantages of the inframammary approach include an easier learning curve with direct visualization of the breast for precise pocket dissection and potentially less risk of contamination. In a thorough analysis of the literature, Namnoum et al found a lower relative risk of capsular contracture, moderate to severe malposition, and secondary procedures with the inframammary approach compared to the periareolar and transaxillary approaches. 8
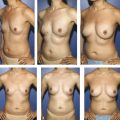
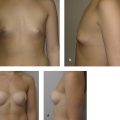
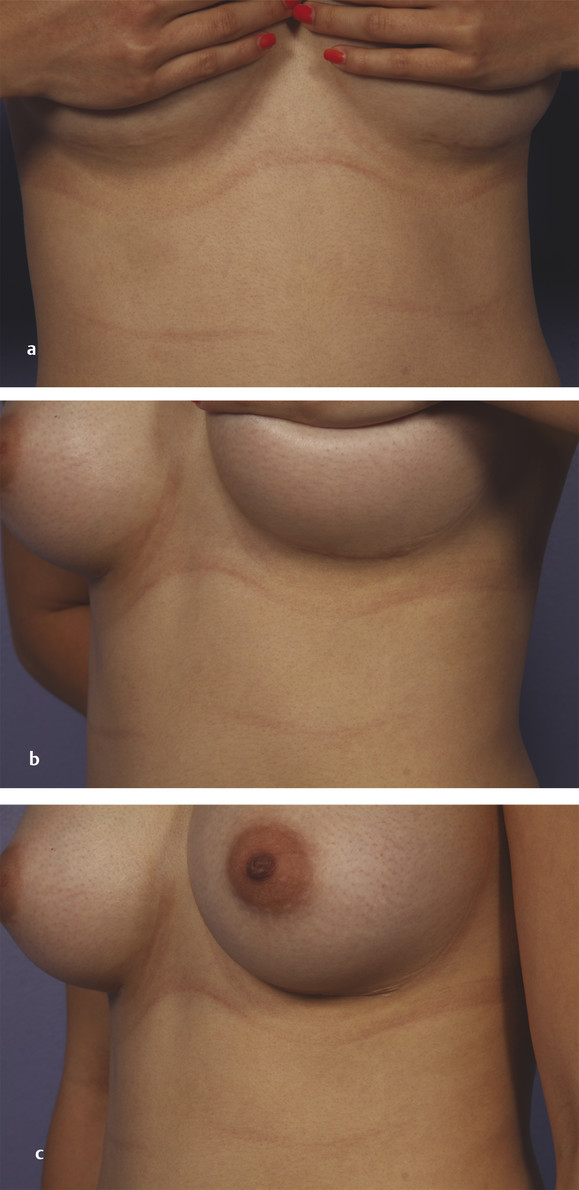
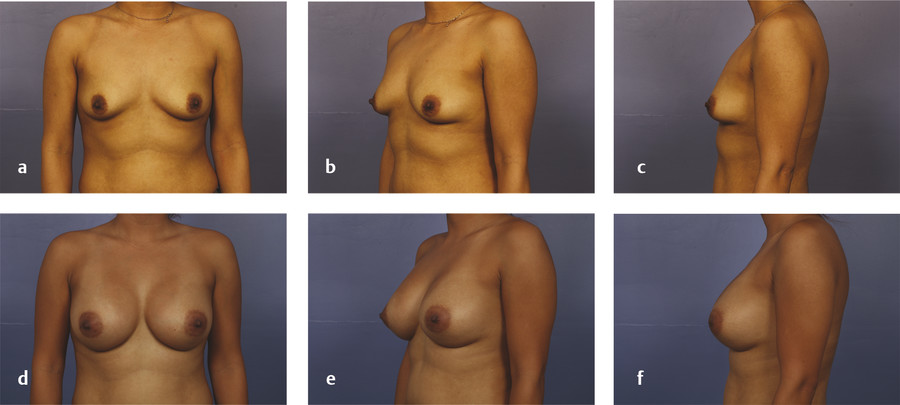
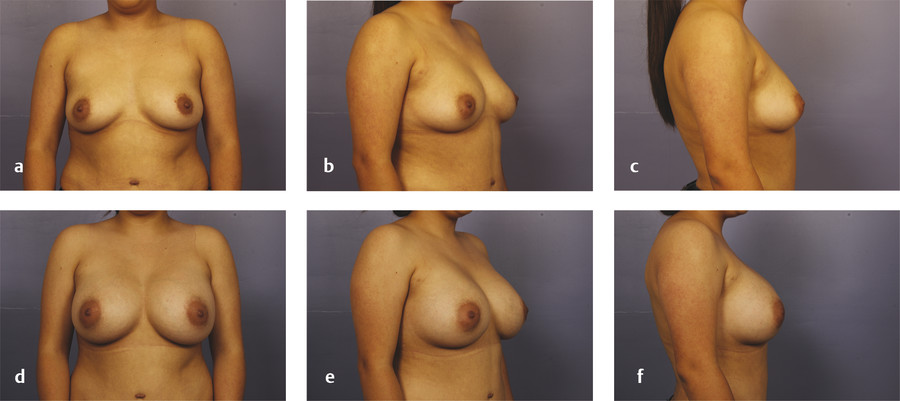
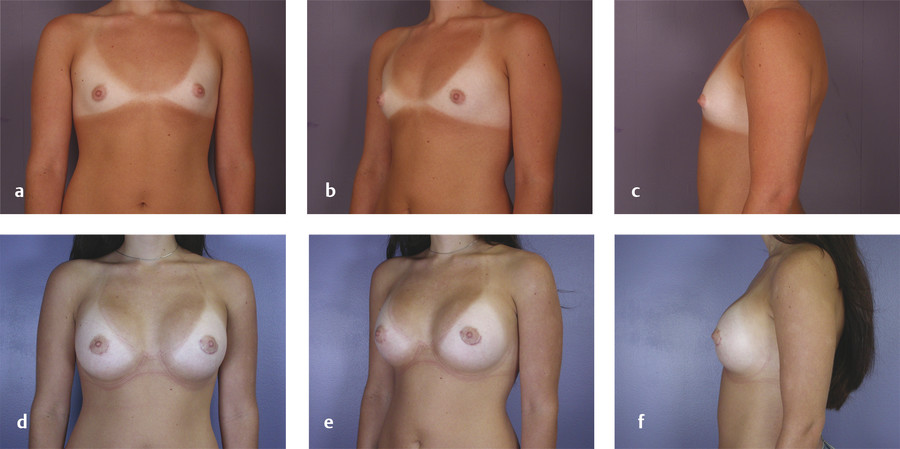
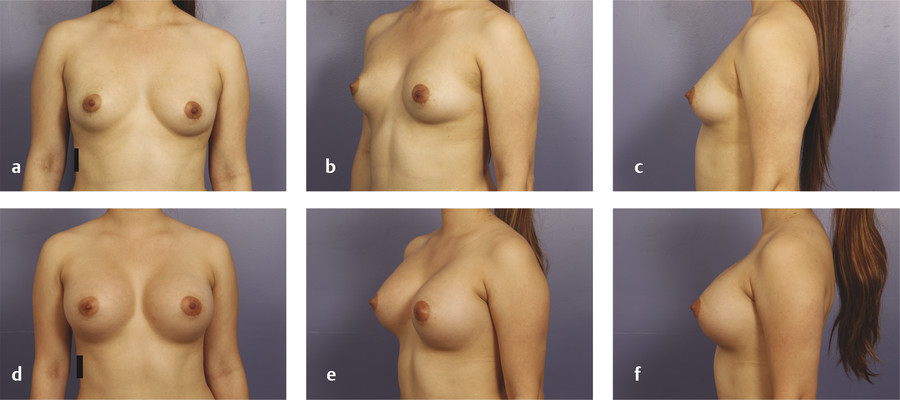
The primary disadvantage of the inframammary approach is a more visually noticeable scar from a basilar view of the breasts and in patients with a poorly defined IMF. A well-placed scar in the IMF should not be visible in an upright position. In patients who preoperatively have adequately sized breasts and a prominent IMF crease, the inframammary scar is well hidden as gravity allows the inferior pole of the augmented breast to descend over the fold. Pre- and postoperative photos of two patients who underwent breast augmentation via the IMF are shown in Fig. 4‑3 (anatomic implant) and Fig. 4‑4 (round implant).
4.2.2 Periareolar and Transareolar Breast Augmentation
Periareolar (PAr) Approach
Jones and Tauras first described the periareolar (PAr) approach to breast augmentation in 1973. 9 An advantage of the PAr approach is that it offers direct visualization of the IMF from a cephalad direction within the pocket. As opposed to the inframammary approach, the PAr approach allows for a more controlled manipulation of the IMF when desired; it also affords maintenance of the IMF via avoidance of dissection of the fold (when desired), which could lead to instability of the fold. It is considered by some to be the most versatile approach because it allows central access to the breast with the greatest ability to lower the IMF. 10 , 11 Easy access to all four quadrants of the breast offers the greatest ease in performing secondary procedures such as capsulectomy.
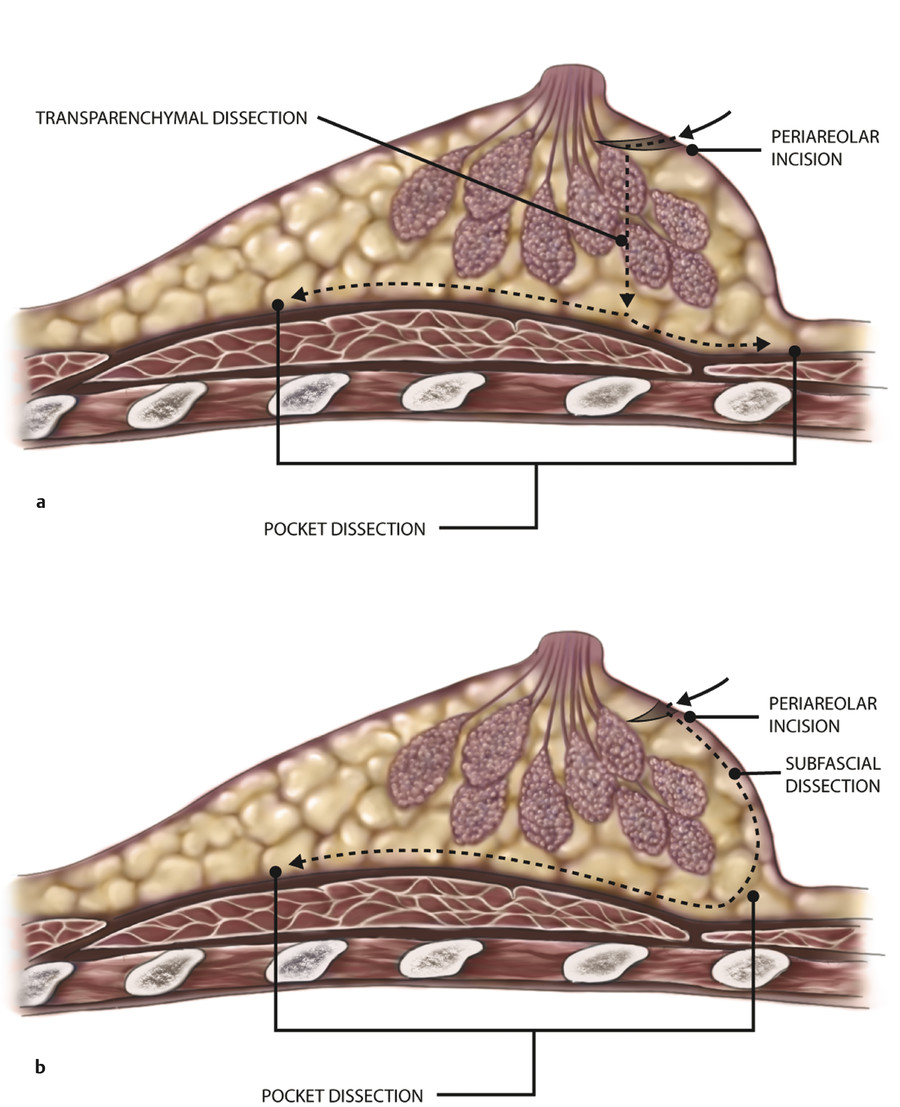
After the PAr skin is incised, there are two possible paths of dissection that can be used to reach the pectoralis major muscle (Fig. 4‑5). The first option is a transparenchymal dissection in which electrocautery is used to go directly straight down posteriorly through the breast parenchyma (transparenchymal approach). The second option is to leave the breast parenchyma undisturbed by first dissecting caudad toward the IMF, raising a flap of inferior pole skin at the level of the superficial fascia, and then dissecting cephalad along the chest wall toward the pectoralis major muscle (periparenchymal approach). 12 The advantage of raising a flap of inferior pole skin is that it allows for more effective release of superficial bands in the case of a constricted breast, but the disadvantage is thinness of the tissue, which can lead to a flattened lower pole contour in some patients after healing. The advantage of the transparenchymal route is an easier, more direct dissection with less chance of devascularizing the lower pole skin, but the disadvantage is a theoretically greater risk of bacterial release from division of breast ducts. 12
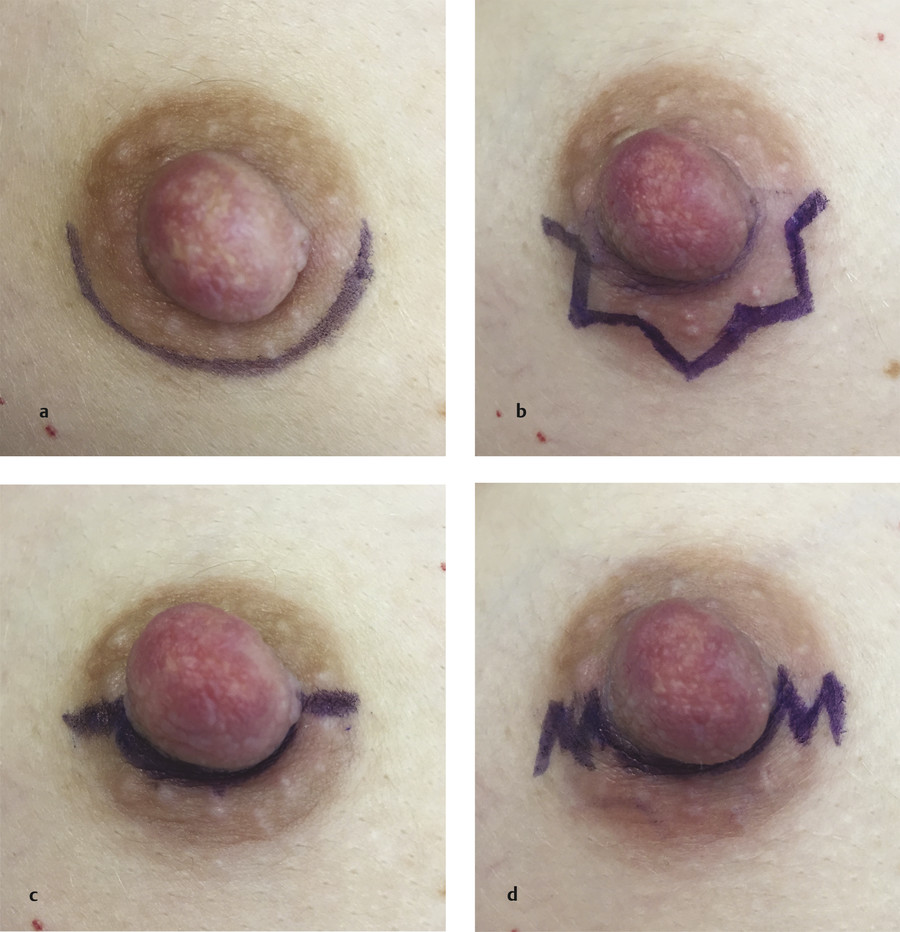
The size of the PAr incision is determined mainly by the size of the areola. The surgeon has little ability to increase incision length intraoperatively if exposure is inadequate and still stay within the confines of the areola. In patients with large areolas, the PAr technique can be advantageous. A large areola allows the surgeon to create a longer incision in the shape of a semicircle for better exposure during dissection while still maintaining a well-hidden scar at the inferior areolar border (Fig. 4‑6a). If areola reduction or circumareolar mastopexy is to be performed concomitantly, the PAr approach may be preferable to avoid an additional scar. As such, this approach is especially useful in patients with tuberous breasts who have large, herniating areolas and high (superiorly positioned) IMFs with short nipple-to-IMF distances. In patients with small areolas, use of the PAr approach limits exposure and thus makes dissection more difficult. The PAr approach can still be used in patients with small areolas with the addition of omega extensions beyond the pigmented border of the areola, but this produces a more visible scar. The PAr approach has been shown to have good outcomes in Asian women. 13 Asian patients often have small areolas, and thus the use of a zigzag incision that straddles the areolar border has been described. 14 The proposed advantages of the PAr zigzag include extension of the effective incision length and a multidirectional incision for less scar contracture (Fig. 4‑6b).
Transareolar (TAr) Approach
The transareolar (TAr) approach, also known as the perinipple approach, is a similar alternative to the PAr approach with a few small differences that make it better suited for certain patients who desire augmentation via the NAC. 15 , 16 , 17 TAr incisions are maintained within the body of the areola but can be less camouflaged because they are not at the natural breast skin–areola junction. The TAr incision is marked in a transverse direction from the 3 o’clock to 9 o’clock positions of the areola or angled slightly obliquely; the incision is continued along the inferior edge of the nipple in the central areola (Fig. 4‑6c). The medial and lateral extensions within the areola on each side of the nipple can also be performed in a zigzag pattern (Fig. 4‑6d); this zigzag pattern can be used to extend the length of the incision for greater access for dissection in the case of a small areola. 17 In patients with darkly pigmented areolas with distinct margins, a PAr scar may be preferable to a TAr scar because of the potential for hypopigmentation when the TAr scar matures within the dark skin of the areola. Conversely, in patients with lightly colored areolas with indistinct margins, a PAr scar may be more noticeable; therefore, a TAr approach may be preferable in patients with these physical characteristics. 10 , 11
Advantages and Disadvantages
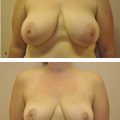
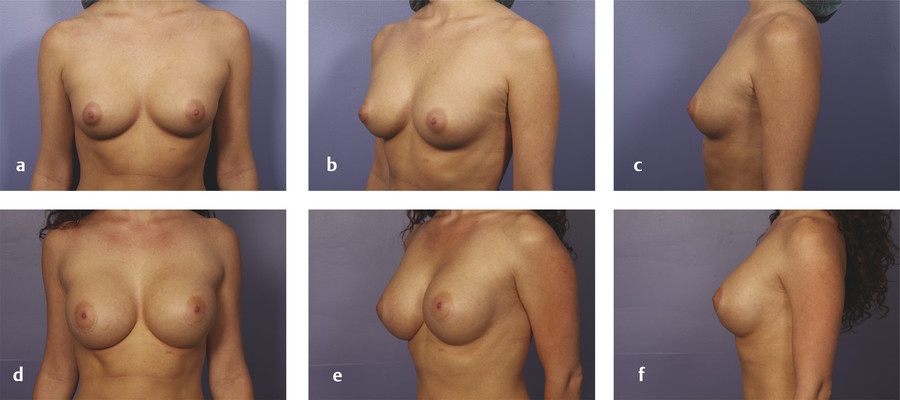
Disadvantages of the PAr and TAr approaches include a scar that is visible at the central focal point of the breast (the NAC) with violation of the lactiferous ducts and breast parenchyma during dissection. The PAr/TAr scar is best concealed in scant clothing or swimwear compared to the other approaches, but the scar is the most noticeable in the upright position in the absence of clothing. This can be an important consideration for models and actresses whose occupation requires nudity or in the setting of intimate relationships. The PAr scar is preferable to the TAr scar if a mastopexy is later performed for ptosis as the patient ages because the mastopexy incisions can be placed through the previous PAr scar. Microscopic analysis of samples obtained during TAr breast augmentations have shown the presence of skin flora. 18 This presence of bacteria in the region of the areola has been hypothesized to influence development of capsular contracture. However, Stoff-Khalili et al found that the rate of complications such as capsular contracture with the subglandular approach through a PAr incision are reduced by the subfascial approach to a rate similar to the subpectoral approach without the postoperative discomfort and muscle animation. 19 Fig. 4‑7 and Fig. 4‑8 demonstrate pre- and postoperative photos of two patients who underwent breast augmentation via the PAr approach.
4.2.3 Transaxillary (TAx) Breast Augmentation
Transaxillary (TAx) breast augmentation was first introduced in the early 1970s 20 , 21 , 22 , 23 and was advanced by the introduction of the endoscope in the early 1990s. 24 , 25 With both the endoscopic and nonendoscopic (blind) techniques, a 4- to 5-cm horizontal incision is made just lateral to the lateral border of the pectoralis major muscle through a crease as cephalad as possible in the axilla to allow it to be better concealed with the shoulder abducted to 90 degrees. Dissection is performed in a subcutaneous plane to avoid axillary lymphatics and intercostobrachial nerves until the pectoralis major fascia is reached. 26 , 27 , 28 Intercostobrachial nerve injury has been reported to be a common complication if dissection is performed deeper than in a subcutaneous plane prior to reaching the pectoralis major muscle. 29 The subglandular, subpectoral, or subfascial plane of dissection is then selected. The pectoralis major fascia is thicker on the cephalad portions of the muscle compared to at the IMF, making the subfascial plane of dissection a little easier to get started through this approach compared to the inframammary approach. Pereira reported similar satisfaction rates in a comparison of various planes of dissection with the transaxillary approach. 30 The transaxillary approach is a little more challenging in patients with a long torso and a low breast footprint, and thus patients with a short torso and high breast footprint are considered more favorable candidates. 10
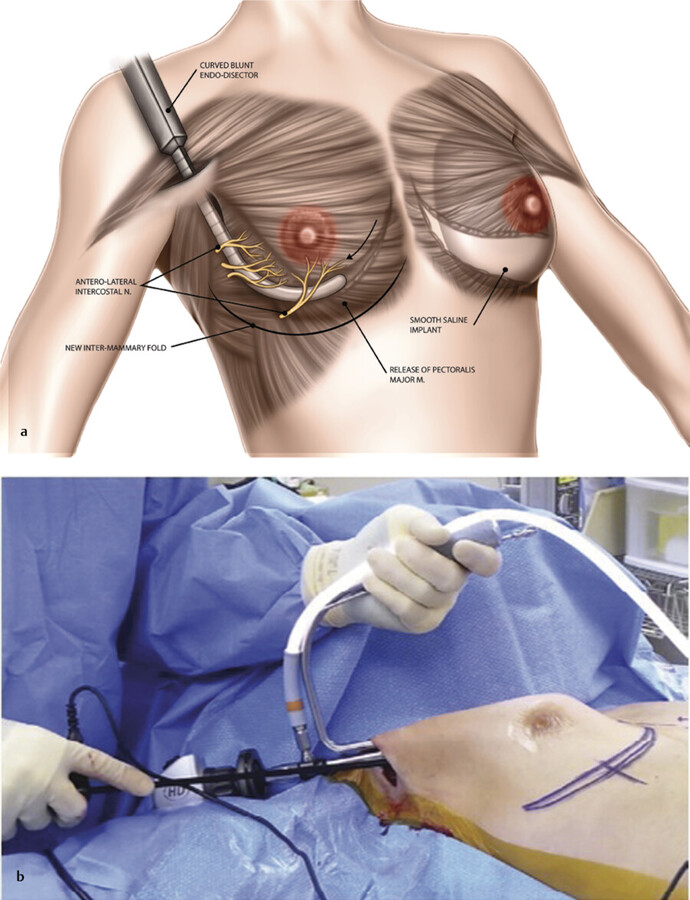
With the blind technique, an Agris-Dingman dissector 31 is passed bluntly in the selected plane to create the pocket. Blunt dissection via this technique works well in the subpectoral plane, with avulsion of the inferomedial attachments of the pectoralis major muscle to the chest wall (Fig. 4‑9a). A long, straight retractor and long electrocautery tip with sharp dissection are more effective than the Agris-Dingman dissector for the subfascial approach because the pectoralis major muscle fascia does not separate bluntly from the muscle very well. With the endoscopic technique, a 10-mm, 30° endoscope is inserted (Fig. 4‑9b). 32 , 33 In theory, use of an endoscope allows precise pocket dissection, especially at the IMF, and meticulous hemostasis compared to the blind approach. 34 However, debate exists about whether these assumptions are adequately supported by data or more theoretical in nature. Roxo et al have reported significantly longer operative times without improved safety or better outcomes with the endoscopic approach. 35 In a 20-year experience of 1,682 patients utilizing the blind approach, Huang et al reported the need for secondary procedures in 13% of patients with low rates of malposition (3.0%), hematoma (0.1%), and capsular contracture (1.9%). 36
Advantages and Disadvantages
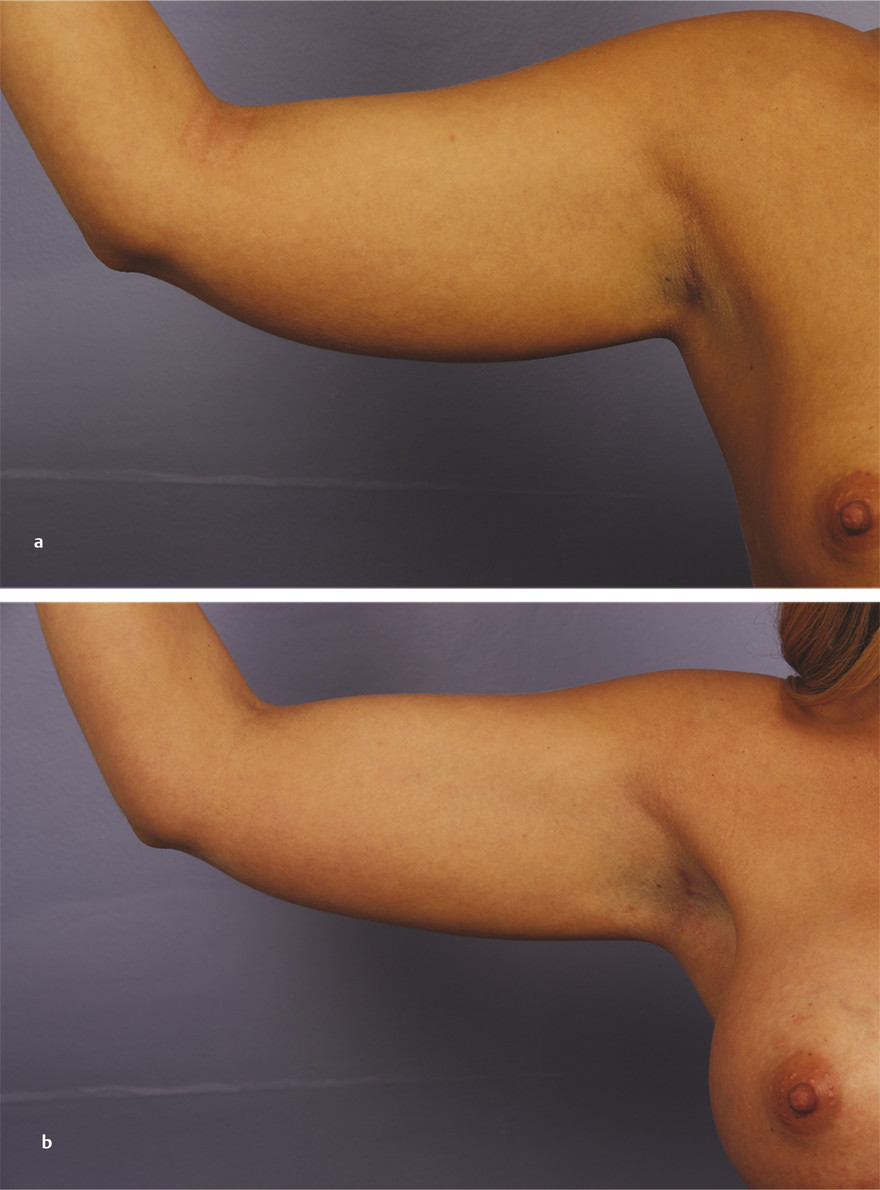
Advantages of transaxillary breast augmentation include no visible scars on the breast and excellent concealment of the scar in one of the natural creases of the axilla (Fig. 4‑10). Therefore, this technique is ideal in patients desiring silicone augmentation who scar poorly or are averse to scars. It is also a good option in patients with small breasts that do not descend over the IMF or have poorly defined IMFs that would make an inframammary scar more pronounced. For these reasons, it is often the preferred technique in patients of Asian descent. 37 Despite this preference in Asian patients, scar assessment of the transaxillary approach compared to the inframammary approach showed comparable cosmetic results. 38 Because of the difficulty of pocket dissection relative to the inframammary and periareolar approaches, the transaxillary approach is also a good option in patients who already have sizable breasts and want only a small augmentation. 10 Disadvantages of the transaxillary approach include a difficult learning curve, less precise pocket dissection that can lead to asymmetry, potential for superior or inferior implant malposition, and inability to perform all reoperations through the same axillary incision. Operatively raising the IMF, advanced capsular contractures, plane change, ptosis, and complicated pocket revision are difficult or impossible to correct through the same axillary incision. 36
Inferior implant malposition or “bottoming-out” of the implant due to excessive release of the IMF is a major concern with the transaxillary approach. Conversely, superior implant malposition is also a common occurrence resulting from inadequate release of the prepectoral fascia. Improvements in the blind technique to prevent malposition have been described, including disruption of the extended pectoral fascia. 39 To combat a bottomed-out implant, postoperative techniques have also been developed. 40 , 41 , 42 Mills et al developed the shoelace breast cast to reinforce the IMF until sealing of the pocket occurs and the capsule matures with the implants in the appropriate position. 42 With concerns about technical control, many surgeons prefer to use round implants with the transaxillary approach. 34 However, other authors have reported success with the use of anatomic implants. 43 , 44
The transaxillary approach has also met criticism regarding potential interference with sentinel lymph node biopsy (SLNB) later in life due to disruption of axillary lymphatics. 45 , 46 This is a legitimate concern, considering that augmentations are mainly performed in young women and breast cancer develops in 1 out of 8 women over their lifetime. Studies by Sado et al and Weck Roxo et al in which lymphoscintigraphy was performed preoperatively, within 1 month postoperatively, and 6 months postoperatively following transaxillary augmentation found that some patients may experience a transient reduction in lymphatic flow that later returns to normal. They suggested that there might be pressure on the lymphatics from edema or the implant in the early postoperative period, with normalization or adaptive/regenerative capacity of lymphatic pathways in the late postoperative period rather than permanent obstruction by cicatricial fibrosis of lymphatic vessels. 47 , 48
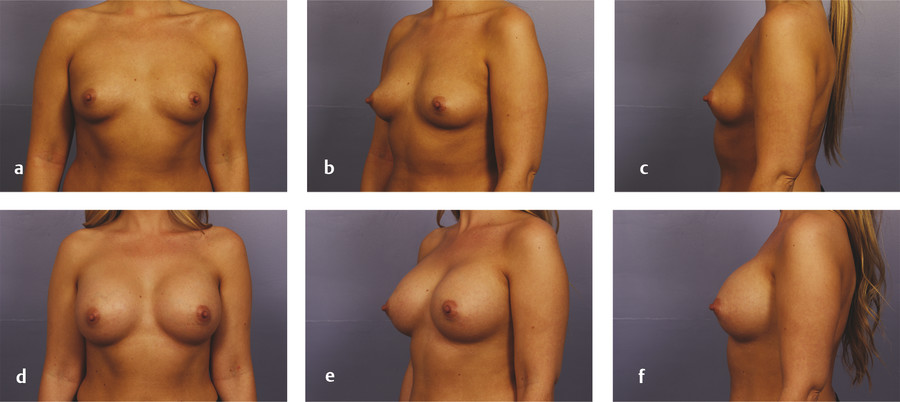
High satisfaction has been reported with the transaxillary approach. 49 , 50 Momeni et al reported higher satisfaction with the transaxillary approach compared to the inframammary approach. 49 Many of the available studies reporting complications are from authors who infrequently perform the transaxillary approach. Authors with greater experience report lower rates of complications. In over 2,500 transaxillary augmentations, Gelfant recalled only seven hematomas and one infection requiring explantation with a capsular contracture rate around 1%. 51 Fig. 4‑11 and Fig. 4‑12 demonstrate pre- and postoperative photos of two patients who underwent breast augmentation via the transaxillary approach.
4.2.4 Transumbilical Breast Augmentation (TUBA)
The TUBA technique was first introduced in 1993 by Johnson and Christ. 52 It takes advantage of the fact that inflatable saline implants can be inserted through small, remote incisions, which is not normally possible with prefilled silicone implants. The implants can be placed in either the subglandular or subpectoral planes. 53 , 54 , 55 , 56 , 57
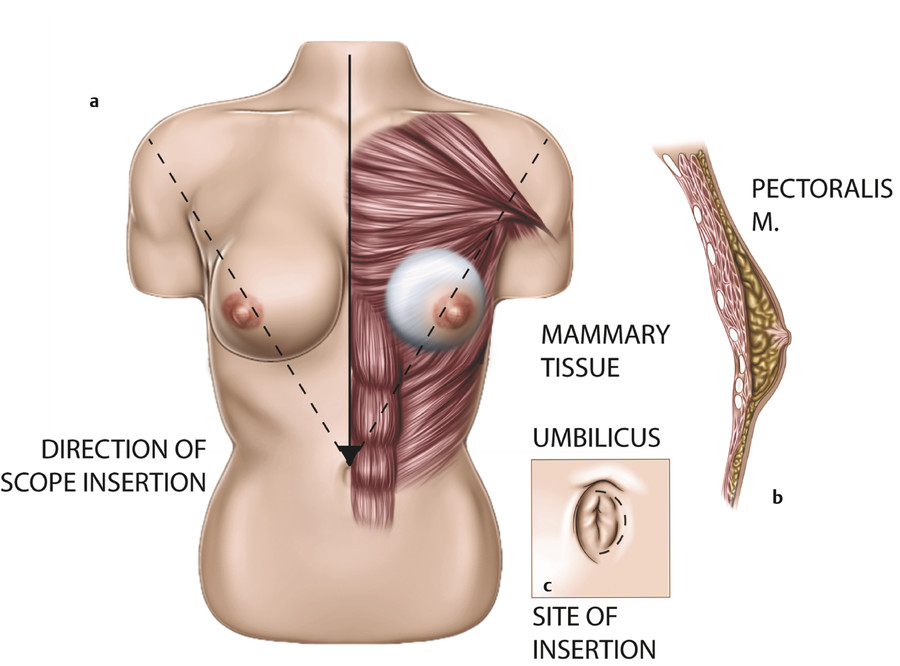
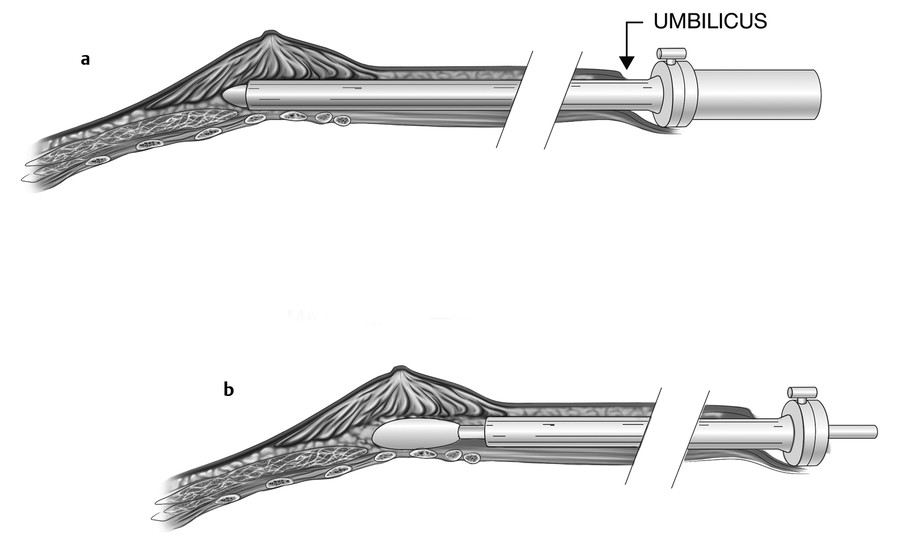
The procedure is performed using an instrument called a mammascope or endotube. The mammascope has the basic configuration of a sigmoidoscope (10 mm, 0° endoscope) but is longer (30 cm) and has an enlarged handle on the obturator for better control during passage through the tissue and ability to span the longer distance to the breast. The path of dissection is marked by drawing a line starting from the umbilicus that passes tangentially along the medial edge of the areola bilaterally (Fig. 4‑13). The lateral edge of the pectoralis major is lateral to this line. An incision is made around the rim of the umbilicus, and the mammascope with internal obturator is inserted through this incision. The mammascope with obturator is tunneled through the deep layer of the subcutaneous tissue just superficial to the abdominal wall fascia (in a manner analogous to a liposuction cannula) to just above the NAC (Fig. 4‑14a). The nondominant hand is used to lift the subcutaneous tissue and breast away from the abdominal wall and chest wall musculature, respectively, while passing the cannula. The obturator is then removed and the mammascope is used to inspect the plane of dissection to confirm a bloodless field (Fig. 4‑14b), followed by removal of the mammascope for implant loading. A subglandular plane is illustrated, as the technique was originally described.
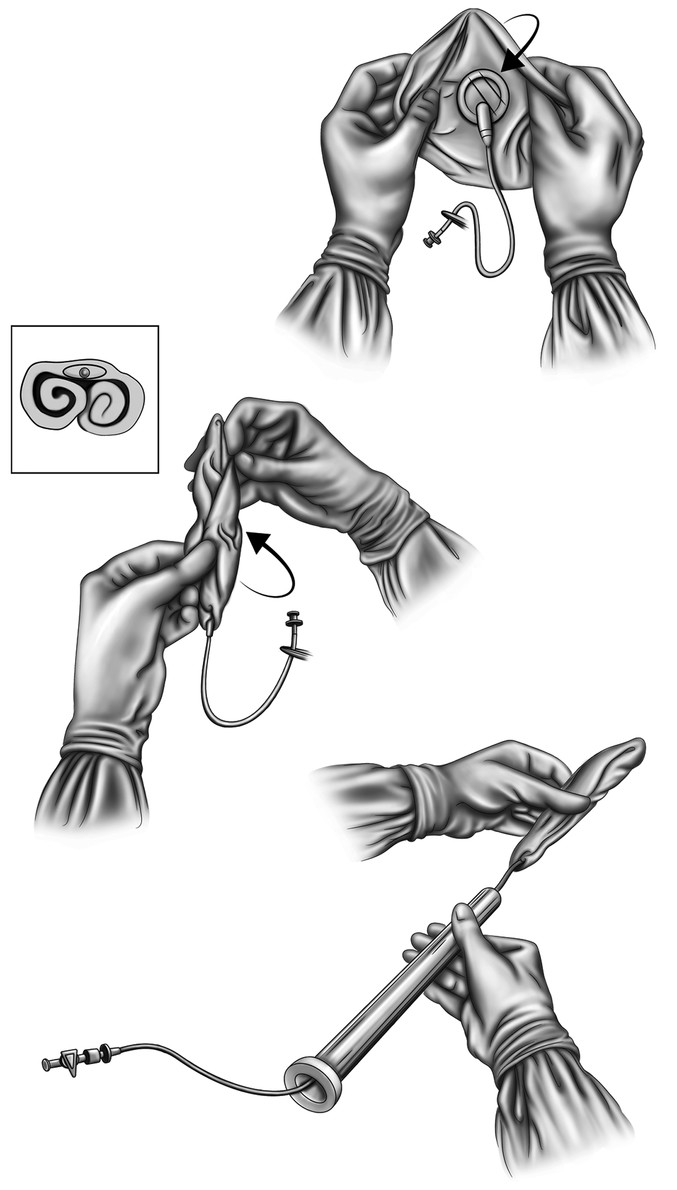
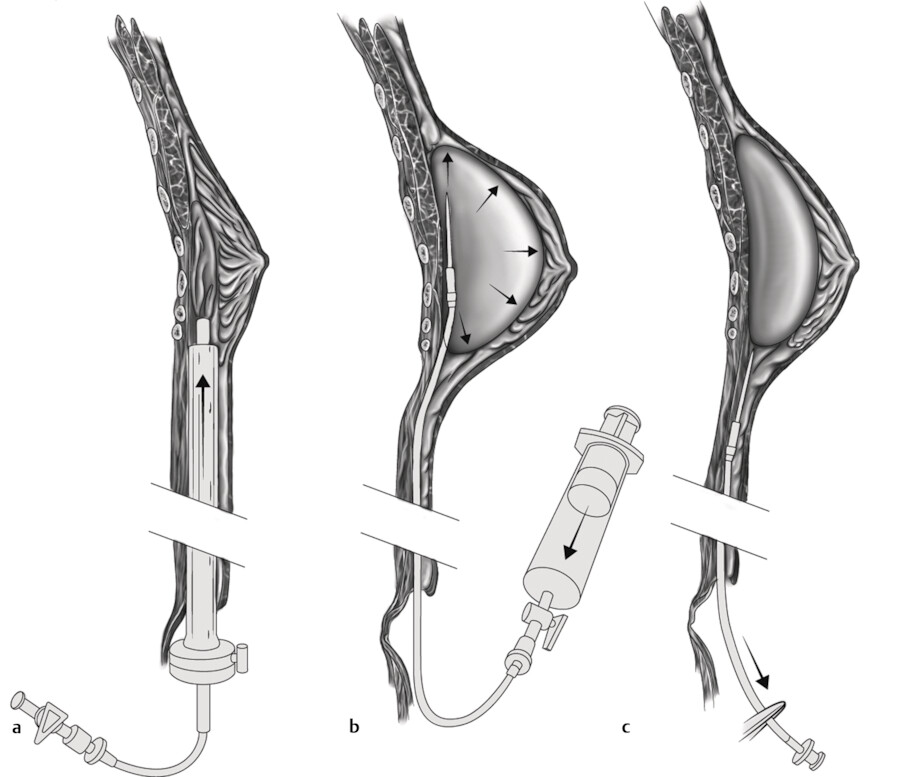
The saline implant is cigar-rolled around its fill tube, the fill tube is attached to an extension tube through the mammascope, and the implant is loaded into the mammascope (Fig. 4‑15). The implant-loaded mammascope is then pushed through the previously created tunnel into the breast, with the fill tube facing the underlying fascia. The deflated implant is then deployed by gently rocking the mammascope free and withdrawing the mammascope from the body, making sure not to dislodge the fill tube prematurely (Fig. 4‑16a). If the fill tube dislodges prematurely, the surgeon can milk the implant retrograde out the umbilical opening, reattach the implant to the fill tube, and reinsert it with the mammascope. The implant is overfilled with saline inside the pocket (Fig. 4‑16b), and the pocket dissection is adjusted by manually manipulating the implant extracorporally. The same procedure is repeated for the contralateral breast, and the fill tubes are removed by manual traction once the breast volumes are deemed symmetric (Fig. 4‑16c). If the fill tube is dislodged while the implant is only partially filled, the implant must be sacrificed by intentional deflation so that it can be removed and a new implant used.
Advantages and Disadvantages
TUBA does offer the least conspicuous scar that is farthest from the breast. However, the transumbilical approach has the distinct disadvantage of traditionally requiring saline implants. Like axillary augmentation, TUBA has the disadvantage of imprecise pocket creation due to the remote access to the breast and near impossibility of revision for complications through the umbilicus. A unique disadvantage of TUBA is development of contour deformities in the form of track marks; however, this is minimized in experienced hands. 58 , 59 The presence of an epigastric hernia is a relative contraindication due to the potential for bowel injury. Scars from previous surgery in the epigastric region also potentially make the dissection more difficult when performed through the umbilicus. Alternatively, these scars can be used for insertion.
TUBA was once a popular approach when saline implants were the predominant implant material used for primary augmentations. Following removal of the moratorium on silicone breast implants that lasted from 1992 to 2006, this technique has fallen out of favor by many surgeons. Therefore, TUBA is mainly considered to be of historical importance at this point because of the renewed popularity of silicone implants. However, a group in South Korea has recently described the placement of round silicone implants via the transumbilical approach. 60
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree