23 Vertical Mastopexy
Summary
This chapter reviews vertical mastopexy as a procedure suited to correction of mild-to-moderate ptosis. It can be combined with augmentation for a more significant nipple elevation. The procedure reduces scarring but excessive vertical length can be problematic. The nuances of the procedure are discussed as are the outcomes.
Key Teaching Points
Vertical mastopexy alone is an effective technique for mild-to-moderate degrees of ptosis but functions best when combined with subpectoral implant placement.
Vertical mastopexy alone is a moderately powerful tool for breast elevation. It should be used with caution in patients with very long inframammary fold to nipple distances.
Imbrication of the lower pole or the use of lower breast flaps is essential to achieve adequate upper pole fullness.
23.1 Vertical Mastopexy without Augmentation
Vertical mastopexy resolves many of the issues that plague periareolar techniques. While the periareolar approach causes widening of the transverse diameter and flattening of the front of the breast with a marked tendency for areolar dilation in the long term, the addition of a vertical skin excision helps to narrow the breast diameter transversely and increases conical projection of the breast mound. Imbrication of the lower pole of the breast pushes breast tissue into the center of the breast mound creating central and upper pole fullness, which can be useful in those patients not desiring breast augmentation.
In my experience, the greatest single disadvantage of the vertical technique is excessive elongation of the vertical limb of the lower pole scar resulting in an appearance of pseudoptosis. This can be readily corrected by performing a short inframammary transverse wedge resection of skin to shorten the vertical limb to acceptable levels.
People often object to this concept of incorporating a short inframammary incision, suggesting that the standard Wise pattern technique would be more appropriate in the first place. This argument entirely misses the point that the standard Wise pattern approach creates a very long inframammary incision, which is prone to hypertrophy and visibility both medially and laterally. The longer the medial and lateral scar lengths, the greater the tendency for poor scarring. Additionally, because of the diverging nature of the vertical limbs of the Wise mastopexy, tension progressively increases toward the base of the breast resulting in potential problems with delayed healing and skin necrosis at the T junction. Based on the shape of the ideal breast, the base of the lower pole is exactly the point at which one requires the least tension in order to mimic the soft, natural fullness of a beautiful breast. Furthermore, the use of minimally undermined medial and lateral skin-parenchymal flaps enhances breast blood supply while allowing ample opportunity to decrease transverse breast diameter and shape the breast appropriately. The incorporation of a periareolar cartwheel Gore-Tex suture helps to reduce the tendency for spreading of the areola diameter over time.
Surgical Plan
Preoperative markings to designate a new nipple position and areolar circumference.
Displacement of the breast medially and laterally to mark the vertical incision lines from below the new areola to a point 1 to 2 cm above the inframammary fold.
Deepithelialization of the upper and lower skin excisions.
Conservative elevation of the medial and lateral breast flaps and preparation of the central-inferior breast tissue for imbrication.
Central breast imbrication and upward transposition of breast tissue.
Vertical limb closure.
Periareolar inset.
Short inframammary transverse skin wedge resection if required to adjust vertical limb length.
23.1.1 Markings
Skin Marking
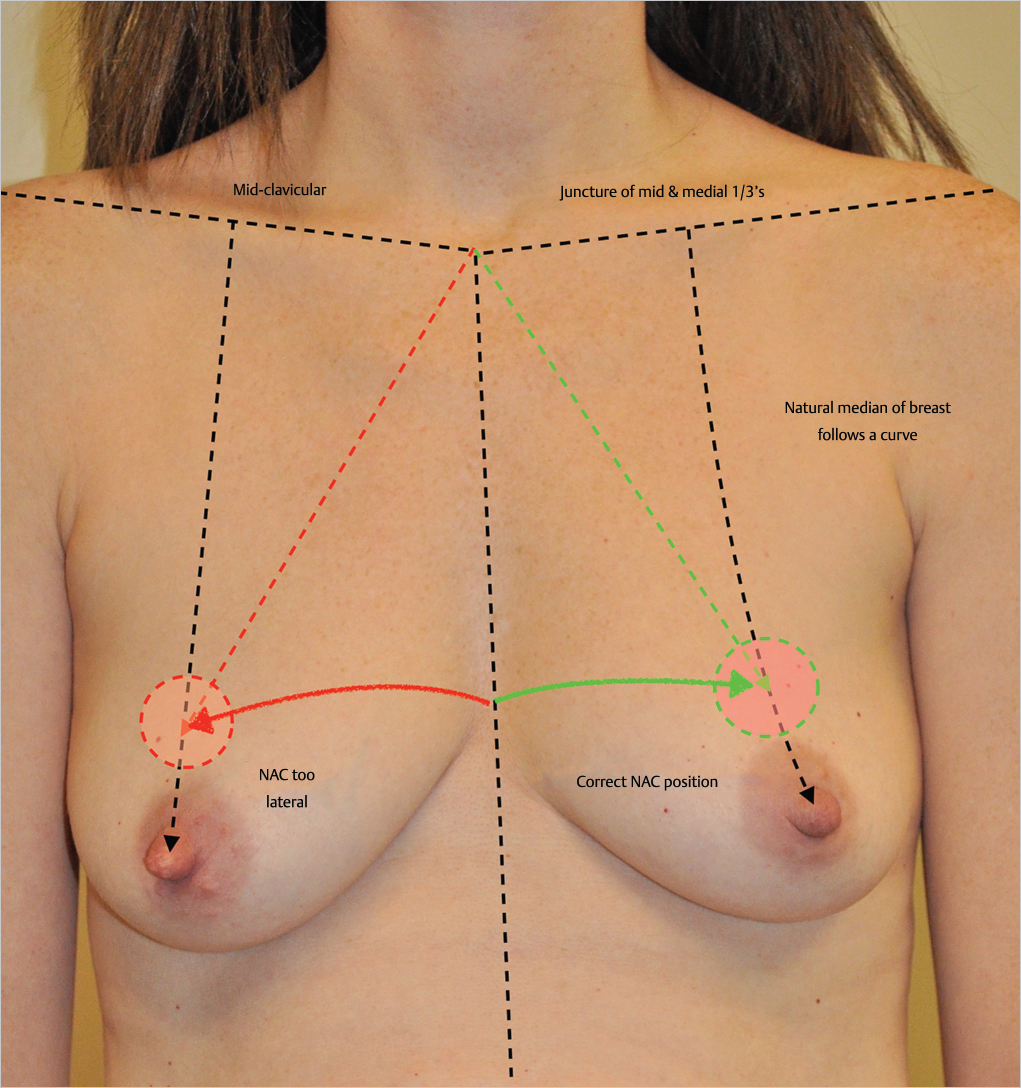
The final position of the nipple–areola complex (NAC) marking is critical in both mastopexy and breast reduction. Too medial placement causes the impression of “squinting nipples” which is almost impossible to correct satisfactorily. Too lateral a position causes unattractive divergence of the nipple position. Pitanguy’s point can be used to determine this position fairly well but may result in inadequate elevation over time. Slight overcorrection can be helpful when mastopexy alone is being performed, as these patients have already demonstrated a significant tendency to stretch out in the past. When marking patient, many surgeons drop a perpendicular from the midclavicular point to the nipple. They then use a line from the suprasternal notch to the intersection with the midclavicular line to determine the level of the new NAC position. While this can be fairly accurate, there is a tendency for the nipple to be placed slightly too lateral when using this technique, particularly in very ptotic women requiring significant cephalad movement of the NAC or in women with broad breasts (▶Fig. 23.1 ).
Clinical Pearl
My preference is to drop a slightly curved line from the junction of the medial and central thirds of the clavicle to the nipple, allowing the nipple position to migrate upward in a more natural curved progression along the true median of the breast.
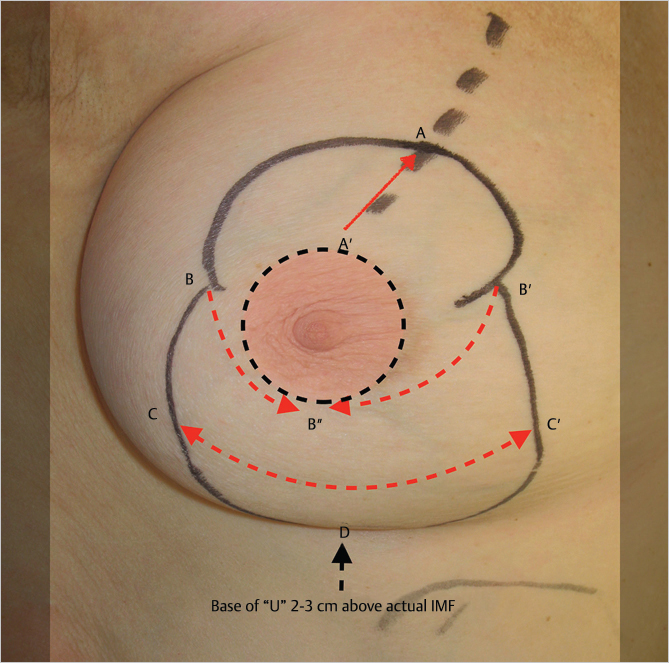
The nipple is marked 1 to 2 cm above the existing inframammary crease (i.e., slightly above Pitanguy’s point), along the median of the breast. The upper point of the new areolar location (point A in ▶Fig. 23.2) is typically marked at 18 to 20 cm from the nipple to the notch, depending on the patient’s height and chest wall length. This places the nipple itself at 20 to 21 cm from the sternal notch. An inverted C-shaped dome incision is marked, with the lower limbs of the inverted C ending at or just below the lower border of the preexisting areolar position (points B and B’ in ▶Fig. 23.2). The medial and lateral portions of the dome should not be too wide as this places excessive lateral tension across the freshly sutured NAC. The breast is displaced medially, and a perpendicular line is dropped along the median of the breast to within 2 cm of the inframammary crease. The breast is displaced laterally, and the medial vertical incision is marked in a similar fashion. The two vertical incisions are joined by a gentle U-shaped incision with its base 1 to 2 cm above the inframammary crease (point D in ▶Fig. 23.2).
23.1.2 Operative Technique
Nipple–Areola Incision and Breast Deepithelialization
The nipple–areolar diameter is marked with an imprint from a “cookie cutter” marker, typically at 42 mm. This imprint is incised into, but not through the deep dermis (▶Fig. 23.3).
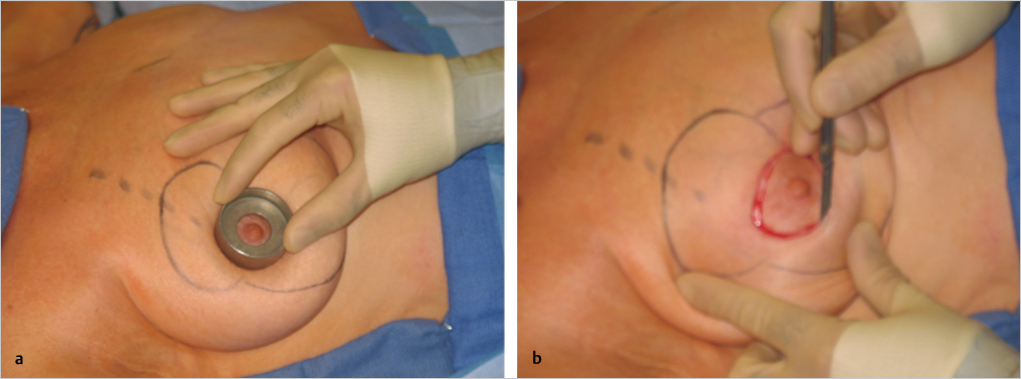
The outermost skin incision is made into dermis, and intervening skin to be resected is deepithelialized (▶Fig. 23.4).
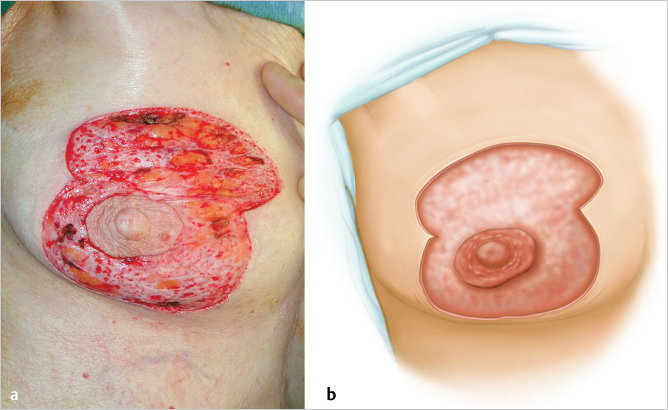
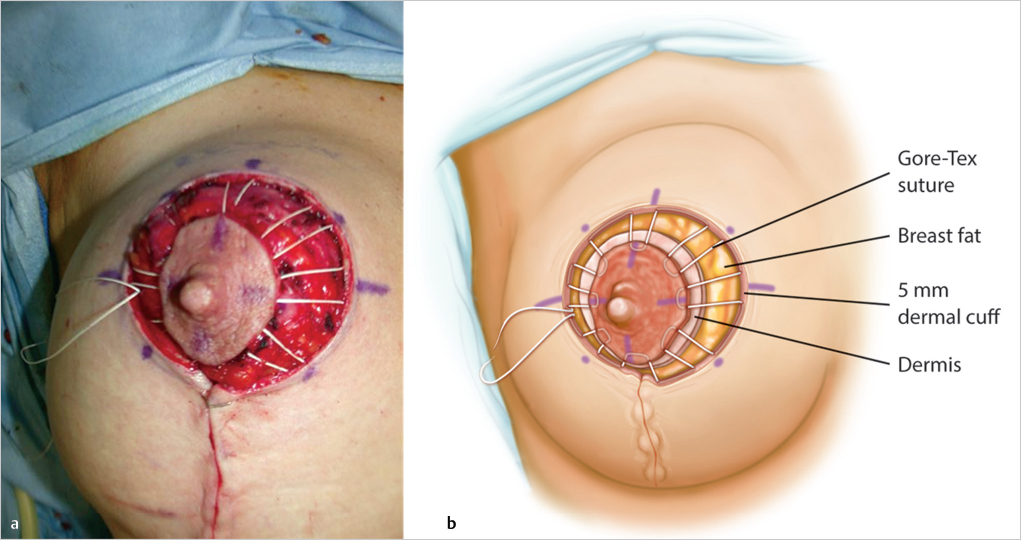
Dermal Cuff Creation
The dermis of the periareolar inset is incised full thickness down to the parenchyma, 3 to 5 mm within the outermost circumference of the areolar skin inset. This provides a 3- to 5-mm dermal cuff in preparation for the periareolar Gore-Tex suture insertion (▶Fig. 23.5).
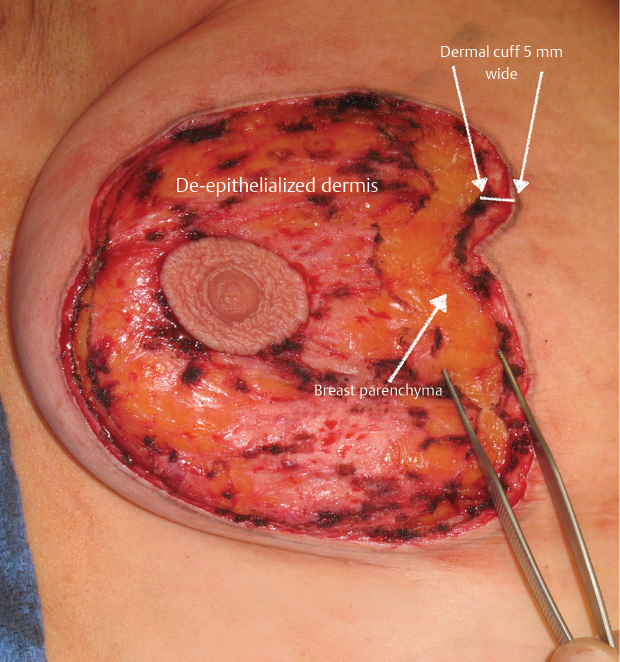
Preparation of the Inferior Dermal Triangle for Imbrication
The dermal triangle below the inferior border of the areola is incised into the parenchyma transversely, allowing the areola to ride upward more easily and to facilitate easier vertical plication of the lower pole for autoaugmentation of the central breast (▶Fig. 23.6).
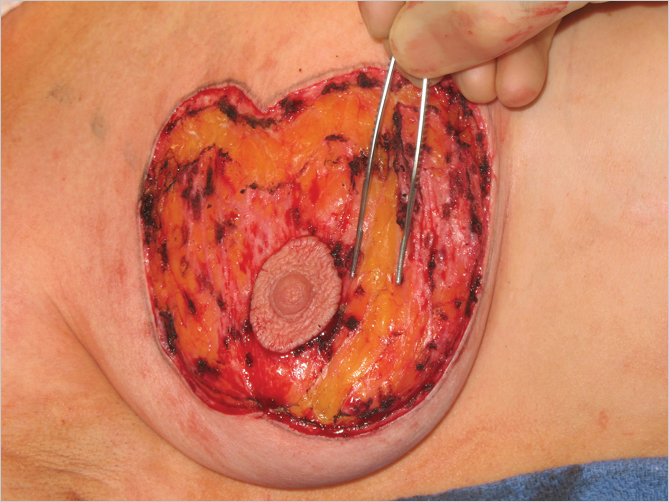
Vertical Lower Pole Imbrication for Autoaugmentation
The deepithelialized lower pole is imbricated using a running 3–0 Vicryl suture on a taper pointed needle. This maneuver infolds the lower central breast parenchyma into the center of the breast mound to some degree, creating autoaugmentation. Leaving a layer of deepithelialized dermis on the lower glandular triangle is critical to allow the sutures to hold well enough without tearing through breast fat (▶Fig. 23.7).
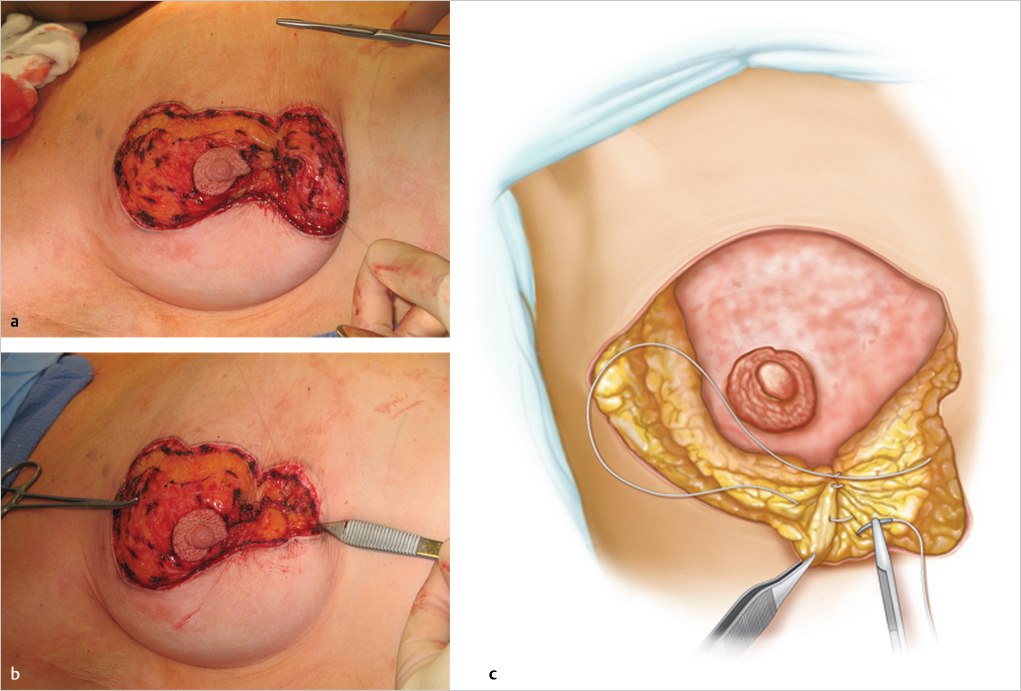
Elevating Lateral and Medial Skin Flaps
Thick skin flaps are raised for 2 to 3 cm laterally and medially along the vertical limbs of the mastopexy after imbrication of the central gland has been performed to achieve projection. The flaps are approximately 1-cm thick leaving a robust blood supply to the overlying skin (▶Fig. 23.8). This maneuver allows for easy approximation of the medial and lateral skin pillars over the central imbricated glandular tissue. Inferiorly, the gland can be elevated off the underlying pectoralis major muscle and sutured down again 1 to 2 cm higher if the inframammary fold (IMF) needs adjustment. This can also improve lower pole shape at the IMF for a more rounded profile if there is any tendency for dog-ear formation to occur (▶Fig. 23.9).
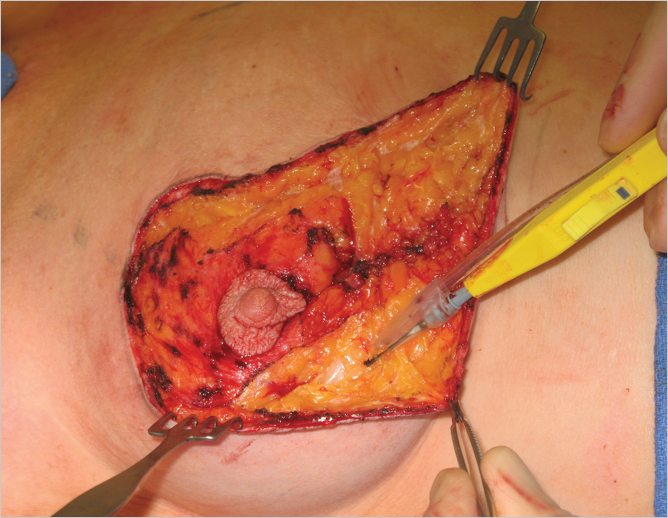
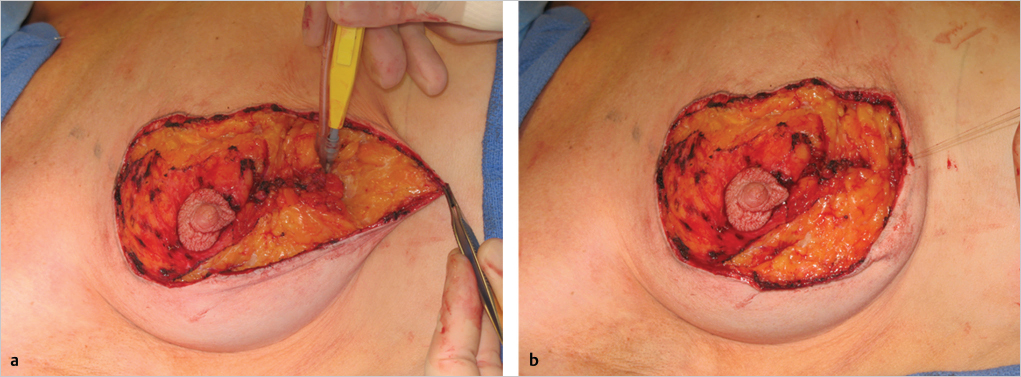
Vertical Pillar Closure and Dog-Ear Management
At this juncture, the medial and lateral skin pillars can be tailor-tacked with staples prior to subcuticular closure. Any gross dog-ear formation or adjustment to excess vertical scar length can be made at this time with excision of the dog-ear or removal of a horizontal wedge resection of skin at the IMF (▶Fig. 23.10).
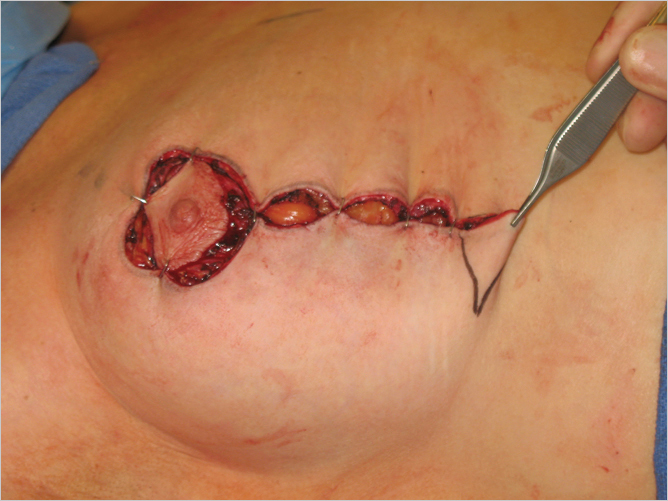
Insertion of the Gore-Tex Periareolar Cartwheel Suture
The insertion of the Gore-Tex periareolar suture is a key step toward achieving a stable nipple–areolar diameter in the long term. The use of absorbable sutures tends to permit late stretching of both the areola diameter and the periareolar scar. The areolar inset is first divided into four major and then an additional four minor quadrants with a marking pen. Reciprocal markings are performed on the NAC itself to match the inset markings.
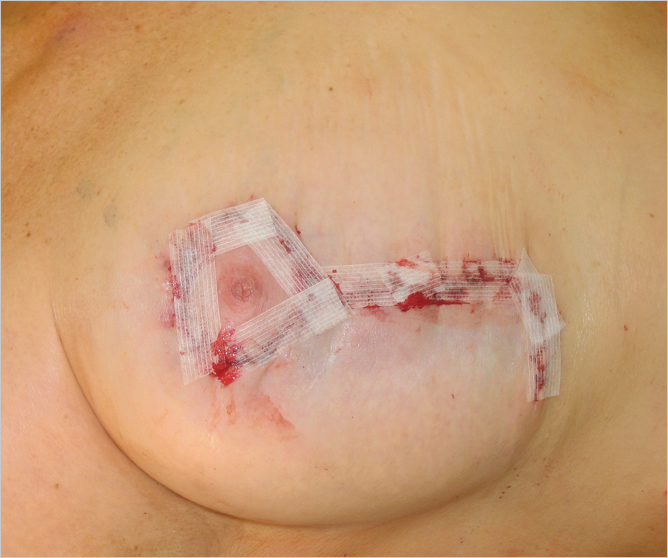
These orientation marks are important for maintaining even tension and placement along the suture line before final tightening takes place. A 2–0 Gore-Tex equivalent polytetrafluoroethylene suture on a Keith needle is used (Surgiform, Lugoff, SC). The suture is started within the edge of the 3- to 5-mm dermal cuff; I usually begin at the 7 o’clock position. Larger bites are taken on the outermost area of the periareolar inset, and smaller bites taken on the areola (▶Fig. 23.11). Once a 360-degree inset has been placed, traction is applied to both ends of the Gore-Tex suture, and the purse-string is closed down to a diameter of 42 mm on average. The knot is tied with 8 to 10 throws on the suture. The knots should be pulled down into the breast parenchyma, inserting the suture deep into the subcutaneous tissues and bringing it out laterally through the skin. It is cut flush with the skin surface. A running 4–0 Monocryl suture is used to close. The vertical closure is completed with interrupted sutures, followed by running 3–0 or 4–0 Monocryl sutures. Steri-Strips are applied (▶Fig. 23.12).
23.1.3 Results
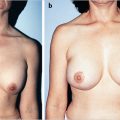
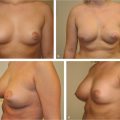
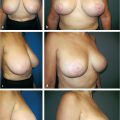
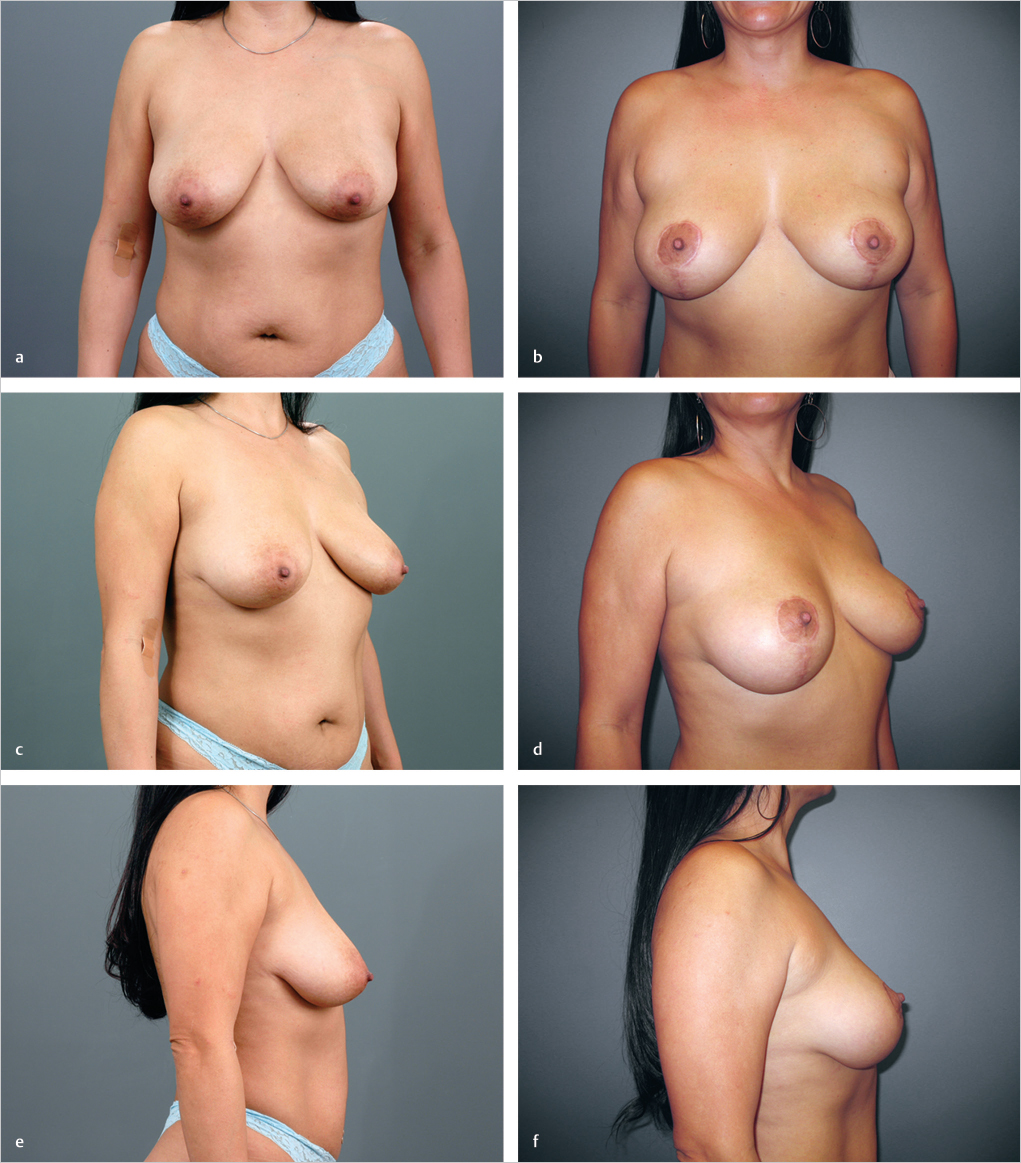
This 39-year-old woman of mixed Filipino and Spanish heritage presented for correction of postpartum breast ptosis. She was comfortable with her breast volume but had noticed progressive sagging of her breasts and areolar dilation after lactation. A vertical mastopexy was planned. Central imbrication of the breast mound was planned to augment the center of the breast mound. A vertical technique was selected over a conventional Wise pattern approach in order to reduce the possibility of poor IMF scarring, given her mixed Asian origins and tendency toward hypertrophic scar formation. She is shown 18 months after a vertical mastopexy. She has a pleasing improvement in breast shape and very acceptable scarring, despite her potential for keloid formation (▶Fig. 23.13).
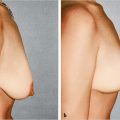
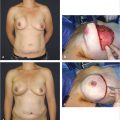
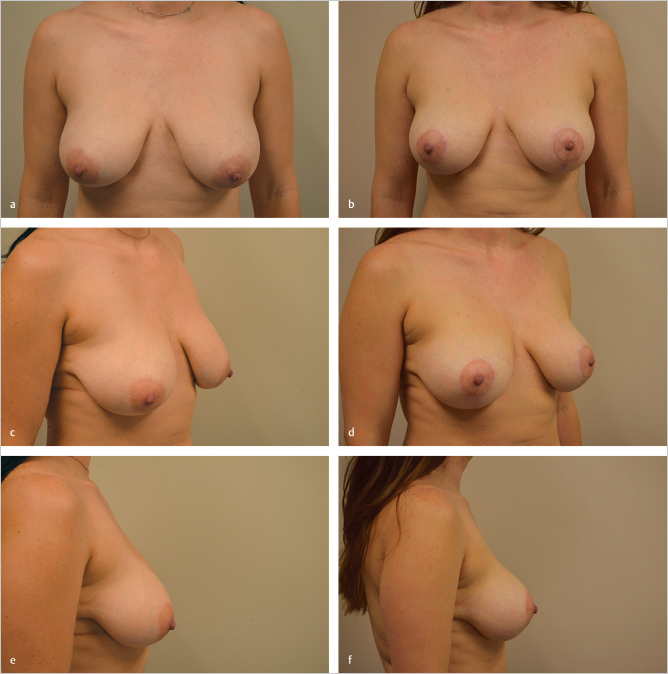
This 35-year-old woman had breast-fed three children and developed postlactational involution and grade 3 ptosis. She requested correction of the ptosis but was concerned about breast scarring. A small augmentation with a vertical mastopexy was advised because of the profound loss of upper pole breast volume. She was strongly opposed to any form of implanted material and was willing to accept the upper pole volume loss if satisfactory nipple elevation and breast reshaping could be achieved without augmentation. A vertical mastopexy with central lower pole imbrication and elevation was planned with suture suspension to the chest wall. She is shown 16 months after this procedure and has a pleasing shape to her breasts, even though the upper pole volume loss is not fully corrected. She was very pleased with the outcome. Nipple sensation had normalized by 6 months postoperatively (▶Fig. 23.14).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree