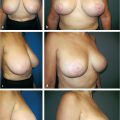
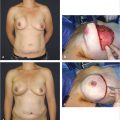
21 Decision Making in Mastopexy
Summary
This chapter revisits the key elements in assessing a patient for mastopexy. The factors affecting outcomes are discussed together with solutions to many of the problems accompanying the ptotic patient.
Key Topics
Ptosis classification.
Surgical options for ptosis correction.
Augmentation mammaplasty.
Periareolar scar technique.
Circumareolar scar technique with periareolar purse-string closure.
Vertical mastopexy without augmentation.
Vertical scar technique with lower parenchymal flap for upper breast fullness.
Vertical mastopexy augmentation.
Vertical scar technique with short horizontal incision.
Wise’s technique with implant placement.
Key Teaching Points
Ptosis is often accompanied by involutional atrophy.
Skin tightening alone will rarely achieve a satisfactory long-term outcome.
Breast augmentation is often required to produce a pleasing aesthetic result.
Wise’s pattern excisions are frequently required to restore breast balance and shorten the vertical limb of a mastopexy.
21.1 Observations
21.1.1 Definition
Mastopexy is an operation of temporal value meant to restore a youthful, uplifted appearance to aging breasts that have sagged and lost their shape.
Technical Pearl
The improvement effected is usually not a lasting one, given that it relies on tightening the cutaneous and parenchymal structures that failed initially, creating the need for the procedure in the first place. Time and gravitational forces eventually reverse some of the tightening and elevation produced by surgery.
The benefits of mastopexy come at the expense of breast scarring, which may be significant in severe cases. Vertical and periareolar purse-string mastopexy techniques have reduced but not eliminated the length of these scars. When the breasts once again begin to sag, as they usually do, negating the effects of early surgery, the scars will be a permanent reminder of the surgical intervention.
Mastopexy is one of the more problematic aesthetic breast procedures; it is fraught with trade-offs and none of the solutions are permanent or trouble free.
Mastopexy alone can leave significant visible scars, particularly in patients with major ptosis and minimal skin elasticity. Patients are not always clear about the breast alteration they seek, and they may not understand the limitations of the procedure, especially when upper breast fullness must be addressed. They know that their breasts hang lower than they did previously and are flattened above, producing an aged appearance. Patients are often unhappy not only with the lower breast position but also with the loss of upper pole fullness. The altered breast shape that has lost much of its upper breast fullness may be the real source of discontent. In many patients, mastopexy alone improves the shape of the breast but does not necessarily achieve the degree of upper breast fill the patient desires. I often suggest a breast implant to improve the shape of the ptotic breast, provide more youthful upper pole fullness, and add an element of permanence to the correction while minimizing the length of the mastopexy scars. This solution, however, introduces the possible concerns, objections, and complications associated with breast implants.
My primary concern, then, is to determine whether this patient should have an operation to correct ptosis or whether her expectations are too vague or unattainable. Many women have confused expectations of this operation, desiring youthful, uplifted breasts with little or no visible scarring. If a patient has a paucity of breast tissue, a pleasing result will be unattainable without the use of an implant. Frequently, this type of result is just not possible, and it is important to explain this to the patient before a decision is made to perform mastopexy. The use of breast implants alone may provide upper pole fullness and enlarge some breasts exhibiting minimal early ptosis, without adjunctive skin tightening. The risk/benefit ratio of this procedure must be carefully discussed with the patient. Several basic questions must be addressed: Does the breast lift justify the resulting scars? Would placement of an implant be the best strategy? Will insertion of an implant provide additional breast fullness and permit shortening of the scars sufficiently to justify the increased concern associated with these devices?
21.2 Patient Assessment and Selection
Women with breast ptosis have an excess of breast skin compared with the amount of underlying mobile breast tissue. This skin is usually lax, has poor elasticity, and does not support and shape the breast. Furthermore, the skin is often thin, with reduced strength, and striae reflect tears and weakness in the deep dermis. The striae are covered with epidermis but retain little, if any, underlying dermis to contribute strength and elastic support. The volume of breast parenchyma is highly variable. The glandular tissue is quite mobile over the chest wall because of attenuation of the fascial supports and Cooper’s ligaments. When a woman with ptosis stands, her breasts assume a lower than normal position, and a varying percentage of breast tissue rotates or droops over a fixed inframammary crease. The nipples and areolae are also low relative to a normal breast position, located at or below the inframammary crease. Upper pole flattening occurs because of the descent of the breast parenchyma and deficiency or atrophy of upper breast parenchyma.
Many women with ptosis recall when their breasts (either during puberty or pregnancy and lactation) were full, youthful, and uplifted. Others mention that their breasts were always poorly shaped and ptotic, even when they were teenagers; they say their breasts never had an attractive, full, youthful appearance. Ptosis is disturbing—drooping breasts are seen as symbolic of the aging process.
21.2.1 Patient Profiles
Women with Ptosis Associated with Obesity, Pregnancy, or Lactation
The breasts of most obese women have a large percentage of fatty tissue. Their heavy breasts are stretched and may rotate over the inframammary crease, resulting in nipples that point inferiorly, or even toward the abdominal wall in severe cases. Significant weight loss may result in a dramatic loss of breast volume, creating additional ptosis associated with inadequate skin retraction.
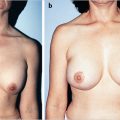
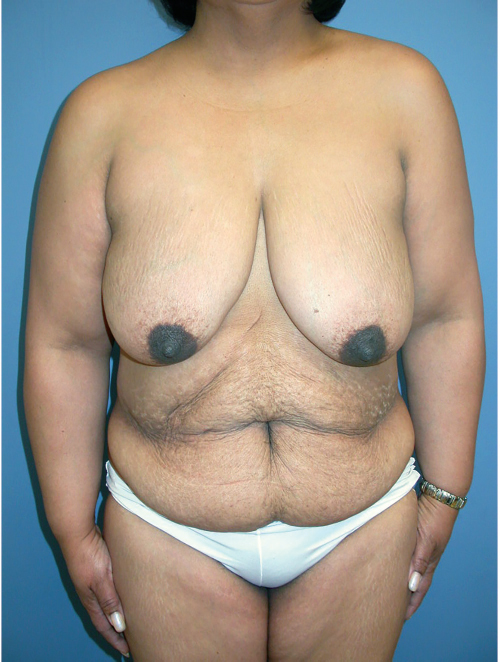
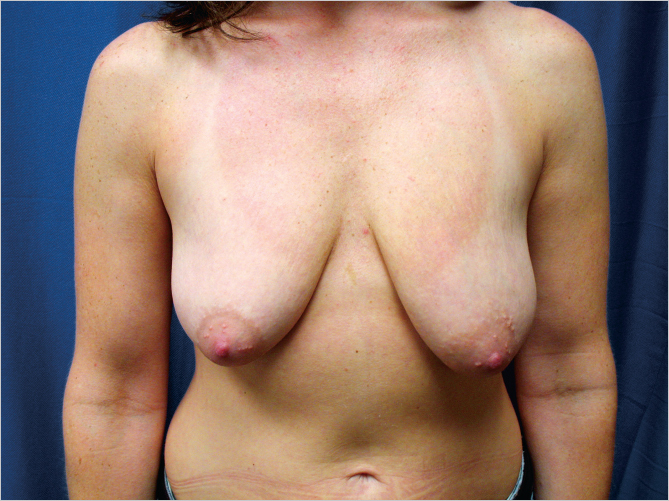
Breast ptosis often develops after pregnancy and lactation. After the skin has stretched, tears occur in the thinned dermis, and striae develop. Breasts with striae are less likely to tighten and firm up to their former shape after lactation. The ptosis seems to increase with every pregnancy and is not entirely related to the increase in breast size or the duration of lactation. After lactation, the breasts can develop involutional hypoplasia, and in patients with more inelastic skin, ptosis or pseudoptosis develops (▶Fig. 21.1).
Young Women with Large, Full Breasts and Thin Skin
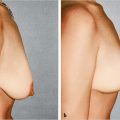
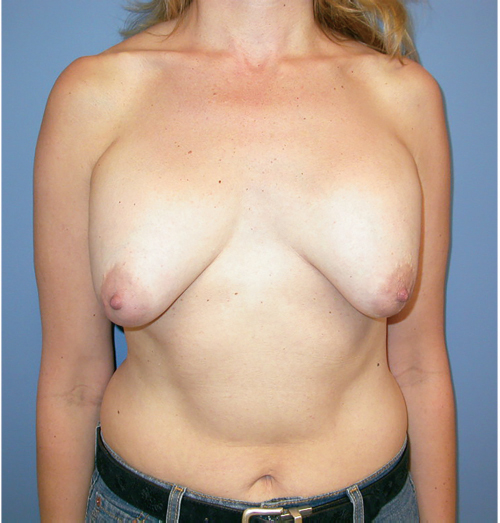
Ptosis develops relatively early in some women, during puberty or the late teens. These women tend to have somewhat larger breasts with thinner, inelastic skin and increased breast mobility over the musculofascial layer of the chest wall. The inframammary fold may be higher or constricted. Frequently they have had previous episodes of weight gain and loss, and their breasts have not returned to their condition before the weight variation (▶Fig. 21.2).
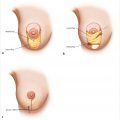
Their breasts are characteristically soft and loosely attached to the fascia, with attenuation of the internal support and laxity of Cooper’s ligaments. The nipple–areola complex is positioned low on the gland (▶Fig. 21.3).
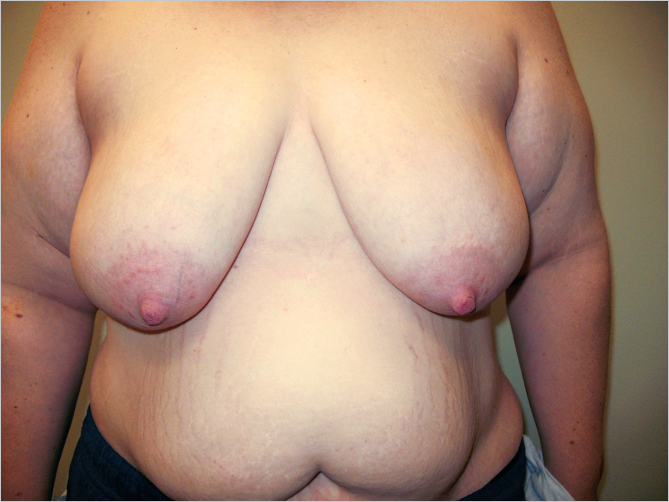
Women after Menopause
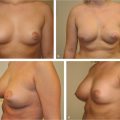
Postmenopausal women usually have breast ptosis as a result of involution that occurred after pregnancy and lactation; this condition is further exacerbated by the loss of skin elasticity and breast volume after menopause (▶Fig. 21.4). Menopause results in diminished blood flow to the breast skin and parenchyma.
Technical Pearl
In thin patients with mobile breast parenchyma, skin flaps should be minimally undermined to reduce the risks of skin necrosis caused by damage to the subdermal plexus.
Hypertrophic scarring is rare in this patient population. Because women in this age group are at higher risk for breast cancer, preoperative mammography and pathologic evaluation of removed glandular tissue are recommended. Internal flaps of breast parenchyma can become devascularized and develop fat necrosis or calcifications that will later be seen on mammograms. These changes can mimic breast cancer and confound future breast surveillance.
21.3 Concerns of the Patient and Surgeon
Scars.
Breast size.
Breast position and contour.
Implants.
Permanence.
Symmetry.
Oncologic concerns with breast screening.
21.3.1 Scars
It is relatively easy to lift the breasts to a new position before the operation; manual repositioning does not produce scars. Mastopexy, however, is not so innocuous. Many women are alarmed when the surgeon describes the scars that will be created from a procedure to produce a more youthful breast appearance. Although the vertical mastopexy and periareolar purse-string mastopexy reduce the length of the scars, they are still located centrally and are quite visible. The patient must determine whether the improved shape and position justify the scars. If she decides to proceed, she will want the scars to be minimal, inconspicuous, and thin.
21.3.2 Breast Size
Most patients who request a mastopexy do not want their breasts to look smaller after their breast lift. Many patients prefer an enlargement, especially one that creates fullness of the upper pole. Simply tightening the lax skin can make their breasts appear even smaller despite retention of all parenchymal tissue during the mastopexy. From the patient’s view looking downward, the loose, ptotic breast appears to flow and project outward before mastopexy. This gives the pseudo-appearance of breast projection.
Technical Pearl
During the preoperative evaluation, it is important to tighten the breast skin while the patient is looking down at her breasts and while she is looking in a mirror to provide a preview of her appearance after mastopexy without using an implant.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree