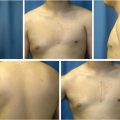
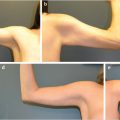
Abstract
Cleft lip deformity not only involves physical distortion, but even more, it commonly carries with it emotional, psychological, and social scarring. For these reasons, surgical intervention is critical, and the author covers every consideration involved in the proper treatment of cleft lip deformity. In preparing for surgery, any comorbities, such as cardiac and pulmonary anomalies, should be identified and addressed, and a presurgical molding technique adopted. Various operative techniques are discussed, and postoperative complications are identified.
12 Cleft Lip Deformity
12.1 Goals and Objectives
Learn the nomenclature and challenges for patients with cleft lip deformity.
Understand the types of presurgical molding and their benefit.
Recognize the different types of cleft repair.
Know the principles for cleft lip repair as well as the indications and timing for additional surgery.
12.2 Patient Presentation
Patients born with cleft lip have a facial deformity that can lead to emotional and physical distortion if unrepaired. These children can suffer from societal exclusion, profound psychological effects, as well as functional compromise. 1 Cleft patients need surgical intervention to help avoid these poor outcomes. In addition, their parents require substantial time investment for education, encouragement, and emotional support. The care of the cleft patient requires a multidisciplinary approach in an effort to provide the necessary resources to optimize the long-term emotional and physical outcome.
Many patients with cleft lip are born into varying levels of socioeconomic class and educational achievement. 2 Therefore, it is important to establish the financial ability and the resources that each family has in order to care for their child. Those with fewer resources and lesser education are more likely to struggle to “make ends meet” while trying to attend the multiple appointments that are needed for their child. A social worker plays a major role in targeting the families that will require more assistance. A unified craniofacial team can lessen the stress on these families and provide an opportunity to see multiple practitioners in one single visit to the center. 3 Additionally, this single visit provides the practitioners an opportunity to meet together and establish a unified and comprehensive plan for each patient.
In addition to a cleft surgeon, a comprehensive craniofacial team offers an evaluation from otolaryngology, oral surgery, psychology, social work, audiology, speech therapy, orthodontics, pediatric dentistry, pediatrics, and genetics. Each specialist plays a significant role in the care of these patients throughout the life of a cleft patient. It is ideal to meet patients within the first couple of weeks of birth. Not only does early involvement help the parents to better cope with the emotional strain, but it also helps parents to better care for their infant. Nutritional support and education for methods of feeding can help ensure that the baby will consume enough nutrition in order to grow and thrive. Finally, this early visit establishes an opportunity for the cleft surgeon to evaluate the severity of the cleft and determine the best approach in preparation for surgical intervention.
12.3 Preparation for Surgery
Patients born with cleft lip may have additional comorbidities that should be addressed prior to surgery. They may have cardiac and pulmonary anomalies that require repair or close monitoring prior to cleft repair. It is also important to assess their growth and weight gain on the pediatric growth chart in order to limit complications with general anesthesia and surgery. Age old recommendations have stated that babies should weigh a minimum of 10 pounds prior to surgery.
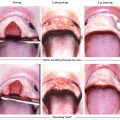
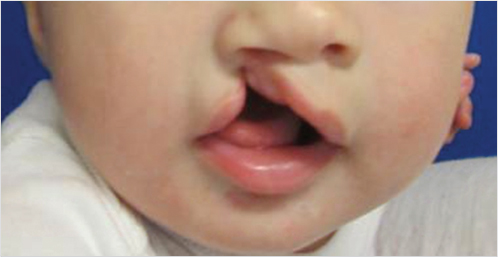
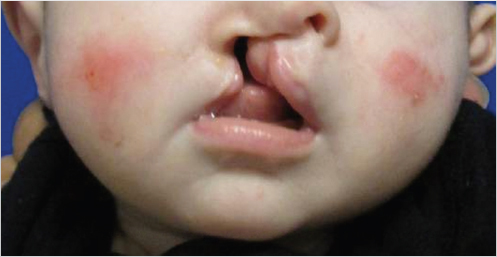
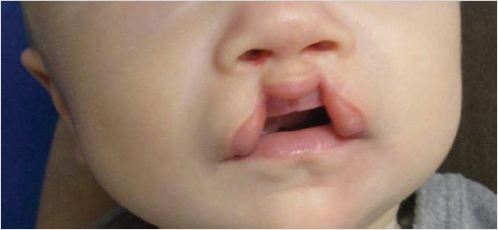
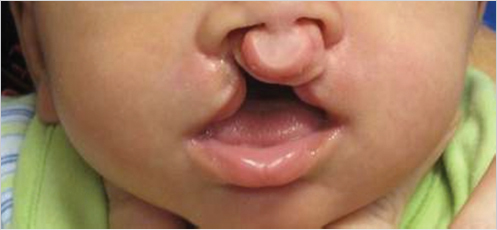
There are differing levels of cleft severity, including incomplete clefts all the way to very wide complete clefts. They may be unilateral or bilateral. Larger width clefts will have a greater impact on the nasal and alveolar deformity. Fig. 12‑1 is an example of an incomplete unilateral cleft lip, while Fig. 12‑2 shows a unilateral complete cleft lip. Fig. 12‑3 and Fig. 12‑4 are examples of an incomplete bilateral and complete bilateral cleft lip, respectively. Assessment of the cleft width is necessary in order to determine the need and type of presurgical molding. It is imperative to determine the ability and means for each parent to follow through on presurgical treatment. Time and financial constraints will prevent good outcomes due to patient inability to attend clinic to monitor the success of the treatment.
There are three types of presurgical techniques, which include taping, nasoalveolar molding, and Latham appliance. 4 , 5 The simplest technique is the act of taping. The infant care provider gently pinches the cleft lip together and applies tape over the gap. This must be performed several times per day, as the tape is likely to fall off when it gets wet during feedings. Taping is very inexpensive and it is very simple to train care providers on the technique. Unfortunately, taping does not address the nasal deformity and it can irritate infant’s skin. Nasoalveolar molding requires an intraoral impression to design an acrylic orthopaedic appliance that is placed into the infant’s mouth. This device enables the cleft gap to narrow while expanding the tissue to help improve the shape of the nose while preventing palatal collapse. It requires multiple and consistent trips to the pediatric dentist for monitoring of the appliance fit and progression of the molding. This can be difficult for some families. Some infants do not tolerate the appliance and constantly push it out, thereby limiting the potential for benefit.
The Latham appliance is surgically inserted into the infant’s mouth early in infancy. The parents are trained to turn the screws daily in order to bring the cleft together. 6 , 7 There is an adjustment period for the infant, as the permanent appliance can affect feeding in the early stages. This also requires an additional exposure to anesthesia during the placement of the device. However, this technique limits the number of clinic visits as compared to nasoalveolar molding (Fig. 12‑1; Fig. 12‑2; Fig. 12‑3; Fig. 12‑4; Table 12‑1).
12.4 Treatment
The face is one of the single most important tools we use to communicate with other individuals in society. We smile, frown, and use other facial expressions to convey our thoughts and feelings. When the face is scarred in some way or not perceived as acceptable by society, individuals suffer emotional consequences and social ostracizing. This also has a long-term negative impact on the patient with a cleft lip and their family. 8 Surgical repair of a cleft lip allows patients to remain an acceptable member of society. In addition, surgery allows the patient to have better oral hygiene while consuming food and beverage.
The overall goal of lip repair is to create a result that addresses many anatomic features. The surgeon must create muscle continuity. The lip height on the cleft side should be equal to the noncleft side. The cupid’s bow should be in continuity with the peaks at the same horizontal level. The vermillion cutaneous junction should be contiguous without step-off deformities. The red lip should be full and symmetric between the cleft and noncleft side, while the wet lip and dry lip junction needs to match at the point of intersection. Finally, the surgeon must spend adequate time addressing the nasal deformity. The flattened ala needs to be contoured at the time of lip repair. The nasal bases should sit at the same horizontal plane and the tip of the nose should be addressed to create better nasal tip projection. Finally, the nares should be equal in diameter and the surgeon needs to try and avoid creating a web in the nasal vestibule of the cleft side (Table 12‑2).
The standard time for lip repair is approximately at 3 months. Most surgeons want the infants to be healthy and thriving with a weight equal to or greater than 10 pounds. If an infant undergoes presurgical techniques, they may not undergo surgery until the desired presurgical outcomes are achieved. Additionally, if the infant has any other underlying medical comorbidities, these too should be addressed prior to surgery. Cleft lip repair is the first surgery in a series of surgeries that the patient will have throughout his or her. Additional surgeries will be needed if the patient has a cleft palate and alveolar cleft (Table 12‑3).
Age | Treatment |
3 mo | Cleft lip repair |
9 mo | Cleft palate repair |
7–9 y | Alveolar bone grafting |
16–17 y | Orthognathic surgery |
16–18 y | Rhinoplasty and lip revision |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree