Summary
Patient selection is critical in enhancing the safety profile of chemical peeling. Proper intraoperative technique and tailored treatment plans to each individual patient is necessary in order to achieve desirable results. Early detection of complications can minimize the chances of scarring and long-term sequela.
10 Chemical Peels
10.1 Background
As life expectancy and life qualities have progressed over the past century, there has been a proportionate increase in public demand for rejuvenating skin treatments. Expectedly, this has led to a surge in the options from practitioners, aestheticians, and pharmaceutical companies for skin resurfacing. The most commonly used facial resurfacing modalities currently are chemical peeling, laser resurfacing, and dermabrasion. These different variations of skin resurfacing options have been used for rhytids, actinic damage, lentigines, and dyschromias. The goal of this chapter is to describe the most commonly encountered complications of the various skin resurfacing modalities, and how to manage them. Advanced skin resurfacing, when practiced with knowledge and good technique, can yield excellent results in skin rejuvenation with a high safety profile.
10.2 Patient Selection
The first step in enhancing the safety profile of facial resurfacing is identifying both the optimal and suboptimal patient. The ideal patient must both be a physical candidate for a skin resurfacing, and also have appropriate expectations for their postoperative results. The most common complication experienced after facial resurfacing is unmet patient expectations, due to poor preprocedural discussion. Skin-specific changes, such as photodamage, lentigines, and rhytids, must be distinguished from other changes like jowling or volume loss. The ideal facial resurfacing patient will have blond hair, blue eyes, fair skin, and fine wrinkles. Of course, the vast majority of facial resurfacing patients do not fit into exact ideal criteria. Therefore, tools such as the Fitzpatrick skin type scale are used to characterize a patient’s suitability (see Table 10.1). Additionally, patients can be rated by their skin type, complexion, texture, and photoaging, using categorizing schemes such as the one by Glogau (see Table 10.2).
10.3 Preoperative Guidelines
A detailed review of any patient medical conditions must be reviewed before facial resurfacing. The relative contraindications for any resurfacing procedure include diabetes, smokers, active or frequent herpes simplex virus (HSV) infections, cutaneous radiation history, hypertrophic scarring, or keloid history. Photosensitizing drugs, birth control pills, and exogenous estrogen should be avoided due to the increased risk of hyperpigmentation. With women of child-bearing age, they should also be warned not to have plans to become pregnant within 6 months after facial resurfacing, due to elevated estrogen levels of pregnancy. 1
Isotretinoin (Accutane) is an absolute contraindication to any facial resurfacing. Skin resurfacing relies on reepithelialization from hair follicles and sebaceous glands for healing, and isotretinoin prevents this from happening. It is widely recommended for all patients to stop isotretinoin for 12 to 24 months before facial resurfacing.
It is paramount to address sun exposure and smoking during the planning stages. Skin resurfacing in the faces of chronic smokers can lead to poor tissue healing, because of the microvascular damage from smoking. All current smokers should cease smoking 1 month beforehand and continue to avoid smoking for at least 6 months after the procedure. In addition, patients should be advised to avoid excessive and direct sun exposure for 6 weeks after skin resurfacing. If this is unacceptable to the patient, other options besides deep skin resurfacing should be explored.
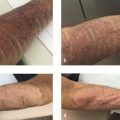
Finally, as mentioned beforehand, the largest risk in facial resurfacing is unmet expectations by the patient. The patient and the practitioner must have agreed upon the realistic expectations of the procedure. The patient’s axillary skin can represent the final result of the skin resurfacing, as long as this region has not previously received excessive sun damage. 2
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree