1 Anatomy of the Breast
Summary
Surgery of the breast requires a detailed understanding of the anatomy and embryology of the breast. A knowledge of the anatomy and development of the breast is important in understanding many of the conditions that plastic and reconstructive surgeons treat. This chapter will focus on the anatomy of the breast and conditions that may arise with aberrant development of the breast.
1.1 Introduction
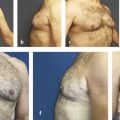
The appearance and function of the breast are important to both men and women. Female breasts appear in adolescence, are typically larger than male ones, and serve an important role in child-rearing (lactation), distinguishing feminine body image, clothing wear, and courting a mate. Male breasts, on the other hand, lack glandular tissue, are smaller, and help to maintain a masculine body image.
In addition, breast appearance and shape are of chief importance to plastic and reconstructive surgeons, as they are routinely asked to restore or augment the normal shape and function of breasts. In fact, it is no surprise that the breast is one of the most common areas operated on by plastic surgeons. In this chapter, we will review normal breast development and anatomy and highlight the contrast with abnormal breast conditions that surgeons commonly encounter.
1.2 Embryology
The first sign of breast development in mammals occurs with the appearance of the milk lines (mammary ridges, mammary crests), which are a pair of ventral ectodermal ridges that initially extend from the axilla to the inguinal region at 4 to 6 weeks gestation. 1 The ectoderm gives rise to the ventral breast skin and the lactiferous ducts, while the mesenchyme gives rise to the fascia, or connective tissue stroma, and vascularity. By the fifth or sixth week, the ectodermal skin layer penetrates into the mesodermal layer to form the ducts. At 10 weeks the milk line normally atrophies proximally and distally to the pectoral region, leaving a pair of mammary glands. The areola is often visible by 5 months gestation.
Mammary gland formation and hypertrophy are driven by maternal hormones, specifically prolactin. The nipple is typically everted at birth due to local relative abundance of mesenchymal tissue. 2 Neonatal breast buds at birth may secrete small amounts of cloudy fluid similar to milk due to maternal hormonal exposure in utero, which normally wanes in the first weeks after birth. Any deviation in or persistence of early embryologic stages of development will result in congenital breast malformations and abnormalities, which will be described later in further detail. It is important to note that male and female breast development in utero and up to the point of puberty are essentially identical.
1.3 Development
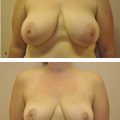
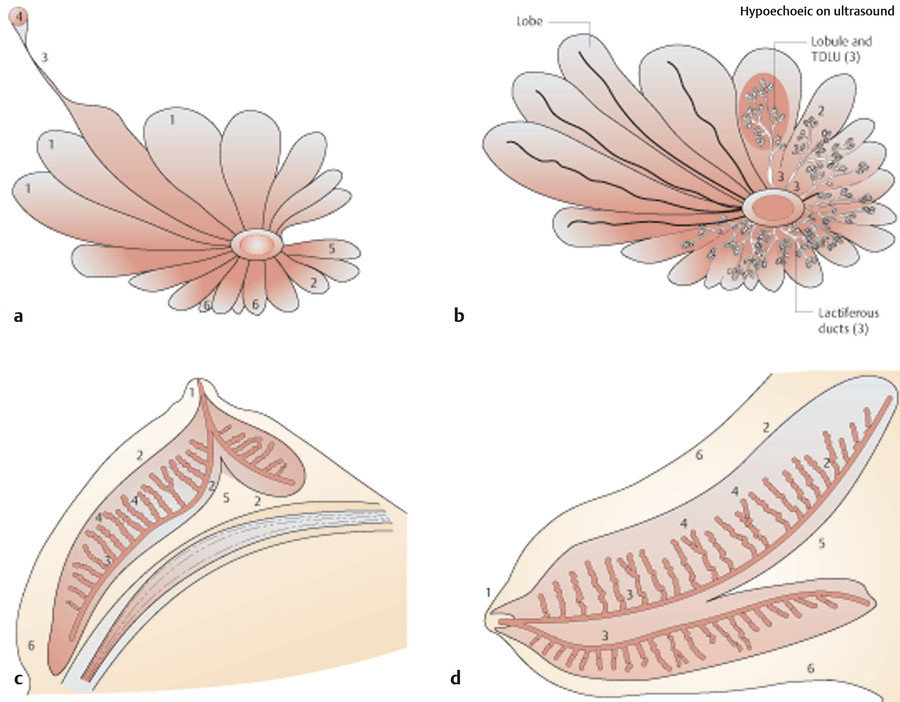
With the onset of puberty, sex hormones drive secondary development of distinguishing breast characteristics. In males, testosterone and relative lack of estrogen increases androgen-responsive traits, including increased muscle mass and hair growth with decreases in body fat, including, but not limited to the breast. Male breast ductal tissue remains hypoplastic and incapable of lactation under these hormonal conditions. In females, estrogen and relative lack of testosterone drive lobular hypertrophy as well as ductal extension into the submammary fat pad. Specifically, this lobular hypertrophy results in lactiferous ducts increasing their branching and acini at the proximal duct. The final result of this hypertrophy is the development of 16–24 terminal duct lobular units, which are arranged radially from the nipple areolar complex (NAC; Fig. 1‑1 3 ). Each lobular unit is organized along a main lactiferous duct, which is fed by hundreds of acini and terminates in the nipple. The developing female nipple and areolar skin are secondarily enlarged by parenchymal hypertrophy.
In puberty, mammary gland, nipple, and areola development follows stages first described by British pediatrician James Tanner. Tanner staging describes genital, breast, and pubic hair changes in both male and female adolescents. Except for female breast development, most of the Tanner staging is beyond the scope of the plastic surgeon.
Up to typically 10 years of age, girls are at Tanner stage I, with no mammary glandular development and the areola slightly elevated. The presence of a breast bud with areolar widening heralds Tanner stage II, which typically occurs by age 11 years. Tanner stage III, characterized by the breast bud widening beyond the borders of the areola, usually occurs by age 13. By age 15 years, most girls enter Tanner stage IV, marked by a secondary mound of the NAC projecting from the breast mound. Breast development continues until adult size is attained, with elimination of this secondary NAC projection (Tanner stage V).
Multiple factors can impact the timing of each Tanner stage, including end-organ responsiveness to sex hormones, familial early onset of puberty, ethnicity, and body fat percentage, all of which can globally impact estrogen production in the peripheral tissues. Dysregulation of adolescent breast development requires a multidisciplinary team approach and will be discussed further in more detail. Breast aging and senescence will also be described later.
1.4 Pregnancy and Lactation
During pregnancy, breast parenchyma growth occurs under the influence of progesterone, estrogen, prolactin, placental lactogen, and chorionic gonadotropin. During the postpartum period, elevated prolactin promotes milk secretion, while oxytocin promotes milk letdown and ejection. These hormones are often persistently elevated through breastfeeding. Once the stimulation for prolactin and oxytocin is eliminated, the levels fall, milk production ceases, and the gland atrophies.
1.5 Landmarks
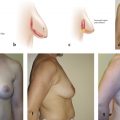
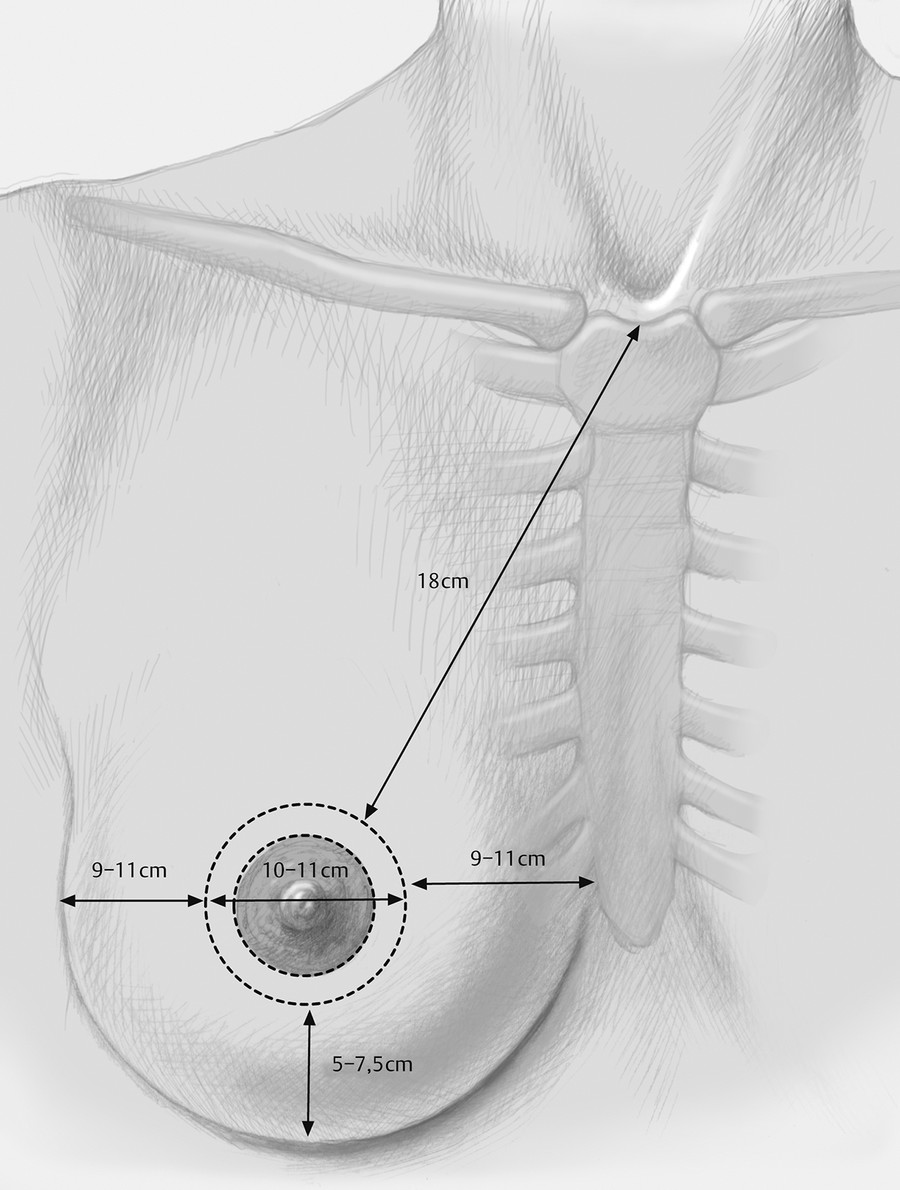
There are numerous anatomic landmarks of the breast that are critical to the plastic surgeon for preoperative evaluation and operative planning (Fig. 1‑2). 3 The midline is often marked from the sternal notch to the umbilicus. With the patient standing, the nipple-to-midline and nipple-to-nipple distances are often measured. The breast meridian, a line from the midclavicle through the NAC, is also marked bilaterally. The sternal notch–to-nipple distance is measured bilaterally, and differences are noted. The inframammary fold (IMF) is marked bilaterally, and the distance from the nipple to the IMF is measured and recorded. The upper breast border is often marked at the edge of the breast parenchyma superiorly (Fig. 1‑3a), along with the anterior axillary fold and lateral breast border. Each breast base width is measured from medial to lateral parenchyma and recorded.
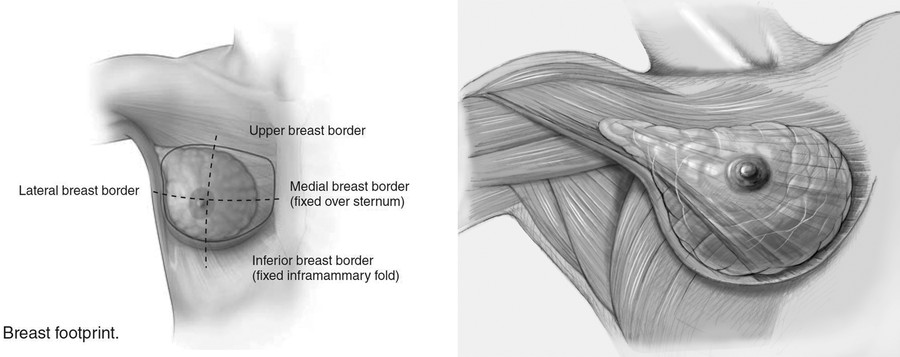
1.6 Basic Breast Anatomy
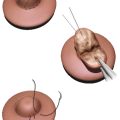
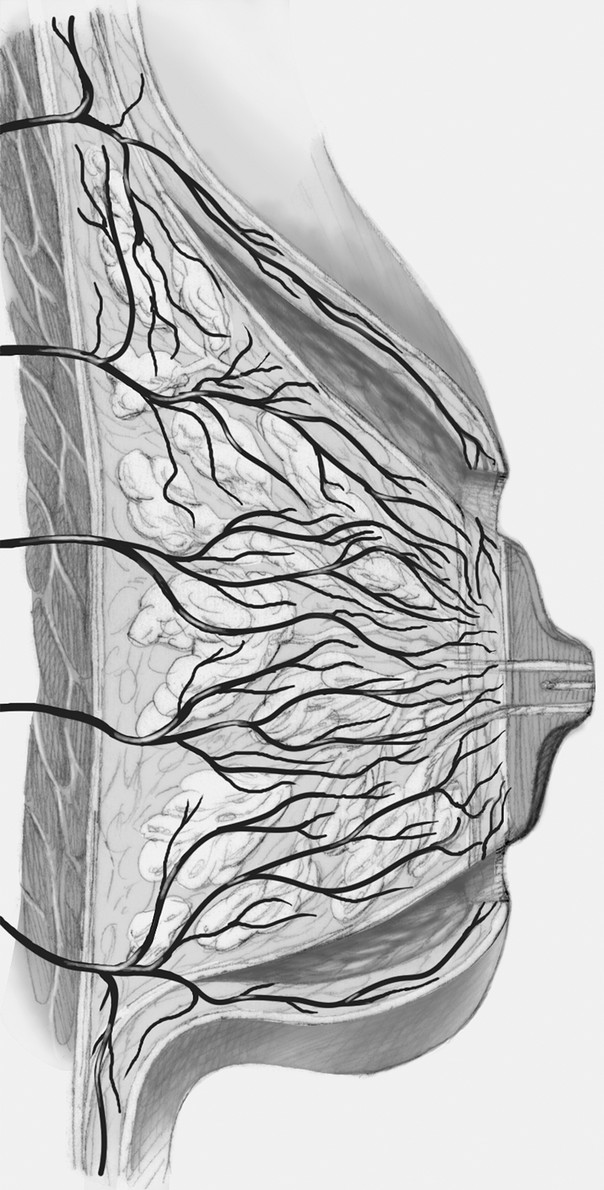
Surgical techniques around the breast are grounded in a foundation of basic breast anatomy and physiology. The majority of the mammary gland lies directly superficial to the pectoralis major muscle (Fig. 1‑3b). 4 Breast parenchyma, which is predominantly made up of glandular tissue and fat, may extend to the sternum medially, the clavicle superiorly, the IMF inferiorly, and the lateral border of the pectoralis major laterally. The parenchyma is suspended by Cooper’s ligaments (pectineal ligaments), connective tissue in the breast that maintains structural integrity and extends from the clavicle and deep fascia of the upper chest to the dermis. Perforating branches of the internal mammary arteries and vein are the major blood supply medially (Fig. 1‑4). Additionally, a rich collateral vascular supply is available from the intercostal, lateral thoracic, and thoracoacromial perforators. Most lymphatic drainage is via level 1 axillary lymph nodes. Most of the breast sensory fibers are derived from medial and lateral intercostals. Greater breast anatomic detail will be described in the following paragraphs.
1.6.1 Aesthetic Subunits of the Female Breast
The aesthetic breast maintains natural size and shape with ideal NAC position (Fig. 1‑2). The ideal NAC is positioned naturally on the most projecting aspect of the breast mound, centered over the parenchyma halfway between the sternum and anterior axillary line and above the IMF. 5 The ideal breast parenchyma has less upper pole fullness, an upper pole–to–lower pole ratio of approximately 45 to 55%, a full lower pole, with upward nipple angulation of approximately 20° (Fig. 1‑3b). Approximate ideal dimensions are sternal notch–to-nipple distance of 18–21 cm, internipple distance of 18–21 cm, and nipple-to-IMF distance of 5–8 cm (Fig. 1‑2). Breast symmetry is ideal but uncommon in the general population. The aging process and its effect on breast shape will be described in greater detail in a subsequent section of this chapter.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree